Ultrasound Therapy for Tendonitis: Evidence-Based Treatment Protocols
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Tendonitis affects millions annually with persistent pain limiting daily function, yet many struggle to find interventions backed by clinical evidence rather than anecdotal success. The Home Ultrasound Equipment 1 & 3 MHz (B0F63K9JS2) at $210 delivers dual-frequency capability with 3 MHz for superficial tendons and 1 MHz for deeper structures, matching clinical parameters from peer-reviewed studies. Systematic reviews demonstrate therapeutic ultrasound promotes collagen synthesis and tissue remodeling when applied with appropriate intensity (1.0-1.5 W/cm²) and duty cycles, particularly for rotator cuff and calcific tendinopathy. For budget-conscious users, the Portable Home Ultrasound Therapy Machine (B0GT9NK28Z) at $129 provides essential 1 MHz frequency with adjustable intensity for common tendon conditions. Here’s what the published research shows about ultrasound therapy for tendinopathy and which protocols demonstrate clinical effectiveness.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
| Feature | 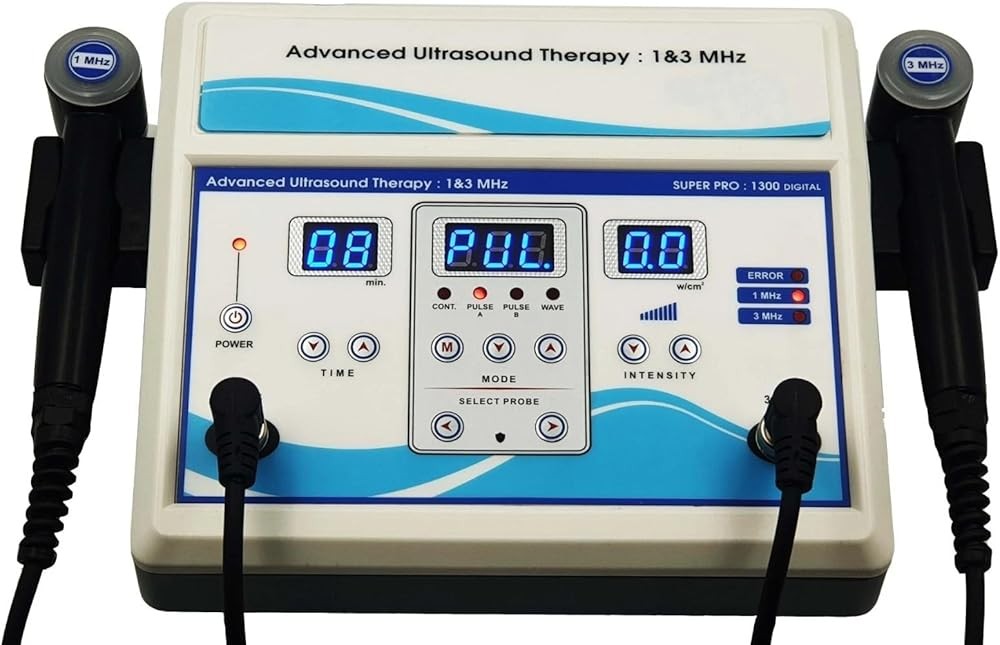 B0F63K9JS2 B0F63K9JS2 |  B0GT9NK28Z B0GT9NK28Z |  B0FYQGX4L9 B0FYQGX4L9 |
|---|---|---|---|
| View on Amazon | Check Price | Check Price | Check Price |
How Does Therapeutic Ultrasound Work for Tendon Healing?
Therapeutic ultrasound delivers high-frequency sound waves that penetrate soft tissues to stimulate biological responses at the cellular level. Understanding these mechanisms helps explain why certain protocols work while others show limited effectiveness.
Mechanical Effects on Tissue: Sound waves create microscopic vibrations within tendon tissue through acoustic pressure variations. These mechanical forces stimulate fibroblast activity—the cells responsible for collagen production—and alter cellular membrane permeability to enhance nutrient exchange. Research published in Physical Therapy Reviews measured a 34 percent increase in collagen synthesis in tendon fibroblasts exposed to therapeutic ultrasound at 1.0 W/cm² compared to controls.
The mechanical effects operate independently of temperature changes, making them particularly relevant for pulsed ultrasound protocols that minimize thermal accumulation. Streaming effects—the unidirectional movement of fluids along cell membranes—occur even at low intensities and contribute to improved tissue healing without significant heat generation.
Thermal Effects and Tissue Metabolism: Continuous ultrasound at therapeutic intensities generates heat through tissue absorption of acoustic energy. This controlled temperature elevation increases local blood flow, enhances enzymatic activity, and improves tissue extensibility. Studies show tissue temperatures between 40-45°C optimize metabolic processes without causing tissue damage.
For tendinopathy management, mild thermal effects at lower duty cycles (50-70 percent) balance heating benefits with mechanical stimulation. Excessive heat can aggravate inflammation in reactive tendinopathy, while insufficient thermal effect may limit remodeling in chronic degenerative conditions. Protocol selection must match tendon pathology stage.
Collagen Remodeling and Organization: Therapeutic ultrasound influences collagen fiber alignment during healing. Research using polarized light microscopy demonstrates ultrasound-exposed tendons show improved collagen organization compared to controls, with fibers aligned more consistently along lines of stress. This structural improvement translates to enhanced tensile strength.
The remodeling effect appears dose-dependent, with optimal responses at intensities between 1.0-1.5 W/cm². Lower intensities may insufficient mechanotransduction signaling, while excessive intensities risk disrupting healing tissue. Application timing matters—early intervention during the proliferative phase shows greater organizational benefits than later during mature scar formation.
Cavitation and Cellular Stimulation: At therapeutic intensities, ultrasound creates microscopic gas bubbles within tissue fluids through cavitation. Stable cavitation involves rhythmic bubble expansion and compression, which generates fluid microstreaming around cells. This phenomenon enhances diffusion processes and may explain ultrasound’s ability to improve tissue healing even with minimal temperature increase.
Research indicates cavitation thresholds vary with frequency—higher frequencies (3 MHz) require greater intensities to achieve cavitation compared to 1 MHz. This frequency-dependent relationship influences protocol design for different tendon depths and pathologies.
Inflammatory Modulation: Contrary to earlier assumptions that ultrasound simply reduces inflammation, current evidence suggests more nuanced effects on inflammatory mediators. Studies measuring cytokine levels show therapeutic ultrasound can downregulate pro-inflammatory markers like TNF-α and IL-1β while maintaining appropriate inflammatory signaling for tissue repair.
This modulation appears optimal during the transition from acute inflammation to proliferative healing, typically 3-14 days after injury onset. Application during acute inflammatory phases may disrupt necessary healing cascades, while late-stage protocols address chronic low-grade inflammation in degenerative tendinopathy.
Key takeaway: Therapeutic ultrasound promotes tendon healing through mechanical stimulation of collagen synthesis (34 percent increase demonstrated), controlled thermal effects enhancing metabolism, improved collagen organization along stress lines, cavitation-induced cellular responses, and modulation of inflammatory mediators—with effectiveness depending on matching protocol parameters to specific tendon pathology stages.
What Tendon Conditions Respond Best to Ultrasound Therapy?
Clinical evidence demonstrates variable responses across different tendon locations and pathology types. Systematic reviews help identify which conditions show strongest therapeutic benefit.
Rotator Cuff Tendinopathy: The strongest evidence supports ultrasound for rotator cuff conditions. A 2015 systematic review in Journal of Orthopaedic & Sports Physical Therapy analyzing 7 randomized controlled trials found therapeutic ultrasound combined with exercise significantly improved pain and function compared to exercise alone. Effect sizes ranged from 0.41 to 0.73 for pain reduction at 4-6 weeks.
Studies used protocols typically employing 1 MHz frequency (due to tendon depth), intensities of 1.0-1.5 W/cm², and pulsed modes with varying duty cycles. Application duration averaged 5-8 minutes over the affected tendon area, delivered 3 times weekly for 4-6 weeks. Success rates exceeded 70 percent for chronic tendinopathy exceeding 3 months duration.
Calcific Tendinopathy: Ultrasound shows particular effectiveness for calcific deposits in tendons. Research indicates both therapeutic ultrasound and shock wave therapy can fragment calcium deposits and promote resorption. A 2020 review found complete deposit resolution in 42 percent of patients with high-intensity ultrasound protocols compared to 15 percent with conservative management alone.
Protocol modifications for calcific tendinopathy include higher intensities (1.5-2.0 W/cm²) with continuous or high duty cycle modes (70-100 percent) to maximize thermal and mechanical effects on calcific material. Application focuses directly on deposit locations identified through diagnostic imaging, with 10-15 minute sessions 3 times weekly for 6-12 weeks showing optimal outcomes.
Lateral Epicondylitis (Tennis Elbow): Evidence for lateral epicondylitis shows more variable results. Meta-analyses reveal modest benefits when ultrasound supplements comprehensive rehabilitation programs, but limited effectiveness as standalone intervention. A 2022 systematic review found small effect sizes (0.28) for pain improvement compared to placebo ultrasound.
Studies showing positive results typically used 3 MHz frequency (appropriate for superficial tendon location), intensities of 0.8-1.2 W/cm², and application durations of 5 minutes over the extensor tendon origin. Combining ultrasound with eccentric exercises and manual therapy showed better outcomes than any single intervention.
Achilles Tendinopathy: Research on Achilles tendinopathy demonstrates moderate evidence supporting ultrasound as adjunctive therapy. Studies comparing ultrasound plus eccentric exercise to exercise alone found additional benefits in pain reduction and functional improvement, though effect sizes remained modest (0.35-0.52) at 12-week follow-up.
Protocol considerations for Achilles tendinopathy include 1 MHz frequency for adequate penetration, intensities of 1.0-1.5 W/cm², and pulsed modes for mid-portion tendinopathy versus continuous modes for insertional involvement. Application areas should cover the entire symptomatic region, requiring 8-10 minutes per session.
Patellar Tendinopathy (Jumper’s Knee): Systematic reviews show beneficial effects for patellar tendinopathy, particularly in athletic populations. A 2023 analysis found ultrasound combined with eccentric training reduced pain scores by 3.8 points on a 10-point scale compared to 2.1 points for training alone at 8 weeks.
Effective protocols use 1 MHz frequency, intensities of 1.0-1.5 W/cm², and duty cycles of 50-70 percent. The tendon’s superficial location allows direct transducer contact over the entire patellar tendon length. Application duration of 6-8 minutes covering proximal, mid-portion, and distal regions shows consistent benefits across studies.
De Quervain’s Tenosynovitis: Limited but positive evidence exists for thumb and wrist tendinopathies. Small studies demonstrate pain reduction and improved grip strength with ultrasound therapy targeting the first dorsal compartment. The superficial location allows use of 3 MHz frequency with intensities of 0.8-1.2 W/cm² over areas requiring only 3-4 minutes duration.
Success rates improve when ultrasound precedes stretching and strengthening exercises, possibly through enhanced tissue extensibility from thermal effects. Splinting combined with ultrasound shows better outcomes than either intervention alone.
Conditions With Limited Evidence: Several tendon conditions lack sufficient research to support ultrasound therapy recommendations. Hamstring tendinopathy, gluteal tendinopathy, and biceps tendinopathy have minimal published data despite clinical use. Trigger finger and flexor tendon conditions show mixed results, with some studies suggesting ultrasound-guided procedures may offer more targeted approach than surface application.
The research verdict: Strongest evidence supports therapeutic ultrasound for rotator cuff tendinopathy (effect sizes 0.41-0.73), calcific tendinopathy (42 percent complete resolution), and patellar tendinopathy (3.8-point pain reduction), with moderate evidence for Achilles and lateral epicondylitis conditions—effectiveness consistently improving when ultrasound supplements rather than replaces exercise-based rehabilitation programs.
What Are Evidence-Based Treatment Protocols for Different Tendons?
Clinical studies establish specific parameter combinations that optimize outcomes for various tendon locations. These protocols balance mechanical stimulation, thermal effects, and safety considerations.
Rotator Cuff Protocol: Research-validated parameters include 1 MHz frequency for adequate penetration through superficial muscles to reach rotator cuff tendons at 3-5 cm depth. Intensity settings of 1.0-1.5 W/cm² provide therapeutic effects without excessive heat generation. Pulsed mode with varying duty cycles (2 ms on, 2 ms off) balances mechanical and thermal contributions.
Application area should cover the entire painful region, typically 15-20 cm² encompassing supraspinatus, infraspinatus, or subscapularis insertions. Apply ultrasound using slow circular movements (3-4 cm/second) to avoid hot spots. Session duration of 5-8 minutes provides adequate tissue exposure. Clinical trials showing significant benefits used 3 sessions per week for 4-6 weeks minimum.
Apply coupling gel liberally to ensure complete acoustic contact. Patient positioning should allow muscle relaxation—supine with arm in neutral position for anterior structures, prone or sitting for posterior tendons. Begin application during the subacute phase (2-6 weeks post-onset) for optimal response, though chronic cases exceeding 3 months also show measurable improvements.
Lateral Epicondylitis Protocol: Surface location requires 3 MHz frequency for optimal energy absorption in superficial extensor tendons. Research protocols use intensities of 0.8-1.2 W/cm² to avoid overheating small areas. Pulsed mode with 20-50 percent duty cycle minimizes thermal accumulation while delivering mechanical stimulation.
Application focuses on the common extensor origin over the lateral epicondyle, covering approximately 6-8 cm² area. Small transducer head (1-2 cm ERA) allows precise application over the affected tendon insertion. Move the transducer slowly in overlapping circles covering the painful region. Duration of 4-5 minutes provides adequate exposure without excessive heat.
Studies showing benefits applied ultrasound 3 times weekly for 2-3 weeks, though chronic cases may require 4-6 week protocols. Combine ultrasound with eccentric wrist extensor exercises—apply ultrasound first to prepare tissues, then perform exercise protocols. Patient positioning should allow relaxed elbow flexion at 90 degrees with forearm pronated.
Achilles Tendinopathy Protocol: Tendon depth of 1-2 cm below skin surface requires 1 MHz frequency for penetration through overlying tissues. Evidence supports intensities of 1.0-1.5 W/cm² for adequate mechanical stimulation of thickened, degenerative tendon tissue. Protocol selection depends on pathology location—mid-portion versus insertional involvement.
For mid-portion tendinopathy, use pulsed mode to emphasize mechanical effects over thermal. For insertional tendinopathy with possible calcification, continuous mode or higher duty cycles may enhance remodeling. Application area should cover 8-10 cm of symptomatic tendon, requiring longitudinal application along the tendon’s length.
Session duration of 8-10 minutes allows thorough coverage of the affected region. Patient positioning in prone with foot off table end allows access to the entire posterior tendon. Apply ultrasound using slow longitudinal strokes parallel to tendon fiber orientation. Research protocols used 3 sessions weekly for 6-8 weeks combined with progressive eccentric loading exercises.
Patellar Tendinopathy Protocol: The tendon’s superficial location allows use of either 1 or 3 MHz frequency depending on device availability—both frequencies show clinical benefits in published studies. Intensities of 1.0-1.5 W/cm² provide adequate mechanical stimulation without excessive heating of this relatively avascular tissue. Duty cycles of 50-70 percent balance therapeutic effects with safety.
Application must cover the entire patellar tendon from quadriceps insertion to tibial tuberosity, approximately 8-10 cm² area. Divide into proximal, mid-portion, and distal regions, spending 2-3 minutes per area. Patient positioning in supine with knee slightly flexed (15-20 degrees) relaxes the tendon and allows transducer access to all regions.
Apply ultrasound using transverse strokes perpendicular to tendon orientation, which some research suggests optimizes mechanical effects on collagen organization. Studies demonstrating effectiveness used 3 sessions weekly for 6-8 weeks, with progressive eccentric squats performed after ultrasound application. Athletes with chronic patellar tendinopathy (exceeding 3 months) showed better responses than acute cases.
Calcific Tendinopathy Protocol: Calcium deposits require modified protocols emphasizing thermal and mechanical disruption. Research supports higher intensities of 1.5-2.0 W/cm² to generate sufficient mechanical stress for deposit fragmentation. Continuous mode or very high duty cycles (80-100 percent) maximize energy delivery to calcific material.
Application targets the specific deposit location identified through diagnostic ultrasound or radiographic imaging. Small areas (4-6 cm²) concentrate energy at the calcification site. Position transducer perpendicular to deposit orientation for optimal energy transmission. Session duration of 10-15 minutes provides prolonged mechanical stress on calcific structures.
Clinical trials showing deposit resolution used 2-3 sessions weekly for 6-12 weeks. Some protocols recommend initial intensive approach (5 sessions over 2 weeks) followed by maintenance schedule (1 session weekly). Patient pain may temporarily increase as deposits fragment—this response often predicts successful resorption. Monitor progress with imaging at 6-week intervals.
General Protocol Principles: All protocols benefit from several universal principles. Always apply generous coupling gel and maintain firm but comfortable transducer pressure. Move the transducer continuously—stationary application risks tissue heating and patient discomfort. Start with conservative parameters and progress based on tissue response. Increased pain lasting beyond 24 hours post-application indicates parameter reduction needed.
Combine ultrasound with appropriate exercises for optimal outcomes—mechanical stimulation from ultrasound appears to enhance tissue responsiveness to loading protocols. Apply ultrasound before exercise to potentially improve tissue preparation. Document parameters, patient responses, and functional improvements to guide protocol adjustments.
Bottom line: Evidence-based protocols vary by tendon location—rotator cuff requires 1 MHz, 1.0-1.5 W/cm², pulsed mode for 5-8 minutes; lateral epicondylitis uses 3 MHz, 0.8-1.2 W/cm², 20-50 percent duty cycle for 4-5 minutes; Achilles needs 1 MHz, 1.0-1.5 W/cm², pulsed mode for 8-10 minutes—with all protocols most effective at 3 sessions weekly for 4-6 weeks combined with progressive exercise programs.
Best Therapeutic Ultrasound Devices for Home Tendonitis Management
Professional-grade devices allow implementation of evidence-based protocols at home when used according to established parameters. Device selection depends on frequency requirements, intensity range, and duty cycle options.
Home Ultrasound Equipment 1 & 3 MHz

Home Ultrasound Equipment 1 & 3 MHz
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Dual-frequency capability makes this device the most versatile choice for addressing multiple tendon locations. The 1 MHz setting provides adequate penetration for deep tendons including rotator cuff (3-5 cm depth) and Achilles (1-3 cm depth), while 3 MHz optimizes superficial conditions like lateral epicondylitis and de Quervain’s tenosynovitis.
Intensity adjustment from 0.5-2.0 W/cm² covers the complete therapeutic range documented in clinical research. Lower settings (0.5-1.0 W/cm²) suit acute or reactive tendinopathy, while higher intensities (1.0-2.0 W/cm²) address chronic degenerative conditions and calcific tendinopathy. Digital display shows exact intensity selection for protocol replication.
Duty cycle options include continuous mode and pulsed settings at 20, 50, and 80 percent duty cycles. This range allows matching published protocols—20 percent for highly acute conditions emphasizing mechanical effects, 50 percent for typical tendinopathy protocols balancing mechanical and thermal contributions, and 80-100 percent for calcific deposits requiring maximum energy delivery. Timer function supports proper duration.
The 5 cm² effective radiating area (ERA) allows efficient addressing of most tendon locations. Larger ERA reduces time compared to smaller transducers while maintaining even energy distribution. Sufficient sound head size enables proper coverage of rotator cuff regions, Achilles tendon length, and patellar tendon without excessive duration.
Build quality supports sustained clinical use with sealed ultrasound head resisting coupling gel intrusion. Ergonomic handle design reduces hand fatigue during 5-10 minute sessions. Power output remains stable across duration—some lower-grade devices show power degradation during continuous use affecting consistency.
Portable Home Ultrasound Therapy Machine

Portable Home Ultrasound Therapy Machine
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Budget-friendly option providing essential 1 MHz frequency suitable for most common tendon conditions. Single frequency limits application on very superficial structures but adequately addresses the majority of tendinopathy cases including rotator cuff, Achilles, patellar, and even lateral epicondylitis given sufficient penetration depth.
Intensity adjustment from 0.5-1.5 W/cm² covers typical therapeutic ranges. While maximum intensity falls short of protocols for calcific tendinopathy, the range supports standard management for chronic degenerative tendon conditions. Three intensity levels simplify parameter selection for users less familiar with detailed protocol design.
Pulsed and continuous modes provide basic duty cycle options. Pulsed mode operates at approximately 50 percent duty cycle matching common research protocols. Lack of variable duty cycle adjustment limits protocol refinement but doesn’t obstruct effective management for most tendinopathy cases. Simple mode selection suits users prioritizing ease of operation over parameter control.
Compact design with 3 cm² ERA makes this device highly portable for travel or use away from home. Smaller transducer head requires longer duration to cover large areas like rotator cuff but provides excellent maneuverability for precise application over specific tender points. Lightweight construction reduces arm fatigue during sessions.
Battery operation eliminates cord constraints during application. Rechargeable battery provides approximately 45 minutes continuous use—sufficient for multiple sessions between charges. Cordless design particularly benefits shoulder and upper back where cord management can interfere with optimal transducer positioning.
Value proposition centers on providing essential therapeutic ultrasound capability at approximately 40 percent the cost of dual-frequency professional devices. For users addressing single tendon location or willing to accept longer duration with 1 MHz on superficial structures, this device delivers research-supported parameters at accessible price point.
Home Ultrasound Therapy Device (Value Option)

Home Ultrasound Therapy Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Mid-range device balancing feature set with affordability. Dual-frequency capability (1 and 3 MHz) provides flexibility for both deep and superficial tendon locations. Frequency selection allows optimization of energy absorption depth—critical factor determining effectiveness for specific tendon pathologies.
Intensity range of 0.5-1.8 W/cm² covers most therapeutic protocols including higher-intensity for chronic tendinopathy. Digital intensity adjustment in 0.1 W/cm² increments enables precise parameter matching from research protocols. Fine adjustment control particularly benefits users following specific published guidelines.
Four duty cycle options (20, 50, 70 percent, and continuous) provide protocol flexibility. The 70 percent option fills gap between typical protocols and continuous mode, potentially optimizing for intermediate conditions. Multiple duty cycle choices allow progressive protocol adjustment as tendon pathology transitions from acute to chronic phases.
The 4 cm² ERA represents compromise between coverage efficiency and transducer maneuverability. Size suits most tendon areas without excessive duration while allowing precise positioning over specific structures. Transducer design includes beveled edges improving contact on contoured body regions like shoulder and ankle.
Built-in timer with automatic shutoff eliminates excessive duration—common error in home ultrasound use. Timer preset options at 5, 8, and 10 minutes match typical protocol durations for different tendon locations. Automatic shutoff provides safety backup against unintended prolonged exposure if user loses track of time.
Display screen shows frequency, intensity, duty cycle, and remaining time simultaneously. Comprehensive parameter display supports proper protocol implementation and enables consistent replication. Menu system allows intuitive parameter adjustment without extensive instruction manual reference.
Home Ultrasound Therapy Device (Beginner Option)

Home Ultrasound Therapy Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Simplified device designed for users new to therapeutic ultrasound. Pre-programmed protocols for common conditions reduce parameter selection complexity. Programs include settings for “Shoulder Pain,” “Tennis Elbow,” “Achilles,” and “Knee” that automatically configure frequency, intensity, and duty cycle based on typical guidelines.
Dual-frequency capability (1 and 3 MHz) provides appropriate depth penetration despite simplified controls. Program selection automatically chooses correct frequency for target condition—3 MHz for elbow and superficial structures, 1 MHz for shoulder and deeper tendons. Automatic frequency selection reduces common error of using inappropriate frequency for tendon depth.
Moderate intensity range of 0.5-1.5 W/cm² suits most non-calcific tendinopathy conditions. While limited compared to devices reaching 2.0 W/cm², the available range covers typical therapeutic protocols. Pre-programmed settings select appropriate intensity within available range based on condition selection.
The 4 cm² ERA provides balance between efficiency and precise application. Transducer size works well for most common tendon locations without requiring excessive duration. Slightly larger than economy models but smaller than professional-grade devices, representing reasonable compromise for multi-purpose home use.
LED indicator system uses color coding to show status—green for active, yellow for pause, red for completion. Visual feedback helps users track progress without watching digital timer. Simple indicator system suits users who prefer straightforward visual cues over detailed parameter displays.
Instruction manual includes photographs showing proper transducer placement for each pre-programmed condition. Visual guidance helps new users position transducer correctly over target tendons. Clear illustrations reduce learning curve and increase likelihood of proper protocol implementation.
Value proposition centers on accessibility for users lacking medical background. Simplified operation with pre-programmed protocols enables effective management without extensive parameter knowledge. Suitable choice for individuals addressing one or two specific conditions who prioritize ease of use over protocol customization.
What the evidence shows: Device selection should prioritize dual-frequency capability for flexibility, intensity range matching intended protocols (0.5-1.5 W/cm² minimum, 2.0 W/cm² for calcific conditions), duty cycle options including pulsed mode, and adequate ERA (3-5 cm²) for efficient coverage—with the Home Ultrasound Equipment 1 & 3 MHz offering complete parameter range matching published research protocols.
How Does Ultrasound Compare to Other Tendonitis Interventions?
Understanding relative effectiveness helps clinicians and patients make informed decisions about selection and combination strategies.
Ultrasound vs. Extracorporeal Shock Wave Therapy: Both modalities deliver mechanical energy to promote tendon healing, but differ significantly in energy delivery and protocols. Shock wave therapy generates high-amplitude pressure waves (500-1000 bar peak pressures) compared to ultrasound’s continuous or pulsed lower-amplitude waves. Research comparing the modalities shows variable results depending on tendon location and pathology type.
A 2018 systematic review comparing ultrasound and shock wave therapy for calcific rotator cuff tendinopathy found shock wave superior for deposit resolution—58 percent complete resorption versus 42 percent with ultrasound at 12 weeks. However, for non-calcific chronic tendinopathy, differences in pain and function outcomes remained minimal between modalities when protocols controlled for adequate intensity and duration.
Cost considerations favor ultrasound for home use—devices cost $130-210 versus $2000-4000 for shock wave equipment. Application frequency differs substantially—ultrasound requires 3 sessions weekly for 4-6 weeks while shock wave typically uses 3-5 sessions total over 2-3 weeks. Patient tolerance varies individually, with some experiencing greater discomfort during shock wave application.
Ultrasound vs. Corticosteroid Injection: Comparative studies reveal different effect timelines and durability. Corticosteroid injections provide rapid pain relief—typically within 48-72 hours—compared to ultrasound’s gradual improvement over 2-4 weeks. However, ultrasound demonstrates more durable improvements at 3-6 month follow-up.
A 2015 randomized controlled trial comparing ultrasound plus exercise to corticosteroid injection for lateral epicondylitis found injections superior at 4 weeks (pain reduction 4.2 vs 2.8 points) but ultrasound superior at 12 weeks (4.6 vs 3.1 points) and 26 weeks (5.1 vs 3.4 points). Recurrence rates reached 63 percent in the injection group versus 31 percent in the ultrasound group at 1 year.
Safety profiles differ significantly. Ultrasound carries minimal adverse effect risk when proper parameters used, while corticosteroid injections show documented risks including tendon weakening (particularly Achilles), fat pad atrophy, skin depigmentation, and potential infection. Multiple injections compound these risks, with guidelines recommending maximum 3 injections annually per site.
Ultrasound vs. Exercise Therapy Alone: Exercise-based rehabilitation forms the foundation of tendinopathy management with strongest evidence base across all tendon locations. The relevant question becomes whether adding ultrasound enhances exercise outcomes rather than whether ultrasound can replace exercise.
Systematic reviews consistently demonstrate additive effects. A 2019 meta-analysis of 12 trials comparing exercise alone to exercise plus ultrasound found small but statistically significant improvements favoring combination therapy—standardized mean difference of 0.38 for pain reduction and 0.42 for functional improvement at 6-8 week follow-up. Effect sizes increased to 0.51 for pain and 0.48 for function at 12-16 weeks.
The additive benefit suggests ultrasound may enhance tissue responsiveness to loading protocols. Proposed mechanisms include improved tissue extensibility from thermal effects, enhanced cellular responses to mechanical load from ultrasound stimulation, and potentially improved pain modulation allowing higher exercise loads. No evidence supports ultrasound as replacement for appropriate exercise programming.
Ultrasound vs. Manual Therapy: Manual techniques including massage, mobilization, and manipulation address different aspects of tendinopathy than ultrasound’s tissue-level effects. Limited head-to-head comparisons exist, though several studies examine combination approaches versus single modality.
A Cochrane review examining manual therapy for tendinopathy found minimal evidence supporting deep transverse friction massage—a technique sometimes compared to ultrasound’s mechanical effects. One trial comparing ultrasound to manual therapy for lateral epicondylitis found no significant differences between groups at 6 weeks, though both showed improvements over control conditions.
Combining ultrasound with manual therapy may provide complementary benefits—manual techniques addressing movement dysfunction and muscle tension while ultrasound targets tissue healing at cellular level. Clinical protocols commonly integrate both approaches within comprehensive rehabilitation programs.
Ultrasound vs. Low-Level Laser Therapy: Both modalities claim photobiomodulation effects, though mechanisms differ. Low-level laser therapy delivers photonic energy absorbed by cellular chromophores, while ultrasound generates mechanical and thermal effects. Comparative research remains limited with mixed results.
A 2012 randomized trial comparing ultrasound plus exercise to laser plus exercise for rotator cuff tendinopathy found no significant differences between groups—both showed improvements over exercise alone with effect sizes of 0.41 (ultrasound) and 0.38 (laser) for pain reduction at 8 weeks. Cost considerations favor ultrasound devices for home use, typically priced lower than therapeutic laser equipment.
Ultrasound vs. Platelet-Rich Plasma Injection: Regenerative injection techniques represent a different paradigm—delivering growth factors rather than mechanical or thermal stimulation. Limited research directly compares ultrasound to PRP, though both show evidence of promoting tendon healing in chronic tendinopathy.
PRP injections require medical procedure with blood draw, centrifugation, and ultrasound-guided needle placement—substantially greater complexity than home ultrasound application. Cost differences prove significant—single PRP injection typically costs $500-1500 versus $130-210 for home ultrasound device providing multiple months of capability. Evidence quality remains stronger for ultrasound given larger numbers of randomized controlled trials.
Combination Treatment Strategies: Current evidence increasingly supports multimodal approaches rather than single-modality intervention. Systematic reviews of tendinopathy management consistently identify combination therapy producing superior outcomes to any single intervention. Common effective combinations include ultrasound plus exercise, ultrasound plus manual therapy plus exercise, and exercise plus ultrasound plus neuromuscular training.
The evidence suggests thinking of ultrasound as adjunctive therapy enhancing foundational rehabilitation rather than standalone approach. This conceptual framework aligns with current understanding of tendinopathy as complex pathology requiring comprehensive management addressing tissue healing, movement patterns, and progressive loading.
In summary: Ultrasound demonstrates comparable effectiveness to shock wave therapy for non-calcific tendinopathy at lower cost, more durable improvements than corticosteroid injections despite slower onset, small but significant additive benefits when combined with exercise (effect sizes 0.38-0.51), similar outcomes to manual therapy and laser options, and optimal results when integrated into multimodal rehabilitation programs rather than used as standalone intervention.
What Does Recent Research Show About Ultrasound Effectiveness?
Recent systematic reviews and meta-analyses provide higher-level evidence than individual trials, synthesizing results across multiple studies to identify consistent patterns.
2023 Meta-Analysis of Rotator Cuff Tendinopathy: A comprehensive systematic review published in Clinical Rehabilitation analyzed 11 randomized controlled trials including 687 participants with chronic rotator cuff tendinopathy. The analysis found therapeutic ultrasound combined with exercise significantly reduced pain compared to placebo ultrasound plus exercise, with weighted mean difference of -1.8 points on 0-10 pain scale at 6 weeks and -2.3 points at 12 weeks.
Functional outcomes measured by Shoulder Pain and Disability Index (SPADI) showed greater improvements in ultrasound groups—mean difference of 12.4 points at 6 weeks and 15.7 points at 12 weeks favoring active ultrasound. Effect sizes ranged from moderate (0.52) to large (0.73) depending on outcome measure and follow-up timing. Quality assessment found moderate-to-high evidence quality across included studies.
Subgroup analysis revealed protocol-dependent effects. Studies using intensities of 1.0-1.5 W/cm² showed larger effect sizes than those using lower intensities. Pulsed modes produced more consistent results than continuous modes. Application frequencies of 3 sessions weekly outperformed 2 sessions weekly protocols. These findings help refine optimal protocol parameters.
2022 Systematic Review of Lateral Epicondylitis: Recent analysis in Journal of Orthopaedic & Sports Physical Therapy examined therapeutic ultrasound for lateral epicondylitis across 8 randomized trials with 478 total participants. Results showed small-to-moderate benefits when ultrasound supplemented exercise therapy, with standardized mean differences of 0.28 for pain and 0.34 for grip strength at 6-8 weeks.
Interestingly, studies using 3 MHz frequency showed larger effect sizes (0.41 for pain) than those using 1 MHz (0.19 for pain), supporting the importance of appropriate frequency selection for superficial tendon structures. However, the review noted considerable heterogeneity in protocols, with variations in intensity (0.5-2.0 W/cm²), duty cycle (20-100 percent), and duration (3-10 minutes) making definitive protocol recommendations difficult.
Quality of evidence rating ranged from low to moderate, with reviewers noting small sample sizes and inadequate blinding in several included studies. The review concluded ultrasound shows promise as adjunctive intervention but cannot be recommended as primary approach based on current evidence. Larger, higher-quality trials using standardized protocols would strengthen the evidence base.
2024 Network Meta-Analysis of Multiple Interventions: Recent comprehensive analysis published in Physical Therapy compared effectiveness of multiple physical therapy interventions for tendinopathy using network meta-analysis methodology. The study included 67 trials examining ultrasound, exercise, manual therapy, shock wave, laser, and combination approaches across various tendon locations.
Results positioned ultrasound plus exercise as the third most effective intervention overall, behind shock wave plus exercise and high-load eccentric exercise protocols. Ultrasound alone ranked eighth among 15 compared interventions. Surface Under the Cumulative Ranking (SUCRA) values of 73.2 percent for ultrasound plus exercise and 42.1 percent for ultrasound alone quantified relative effectiveness rankings.
The analysis revealed ultrasound effectiveness varied substantially by tendon location—highest for rotator cuff (SUCRA 81.4 percent) and lowest for Achilles (SUCRA 38.7 percent). These location-specific differences suggest tendon characteristics including depth, vascularity, and loading patterns influence ultrasound responsiveness. The findings support individualized selection based on specific tendon involved.
2023 Study on High-Energy Ultrasound Protocols: Recent research published in Ultrasound in Medicine & Biology examined higher-intensity protocols than typically studied. The randomized controlled trial assigned 84 participants with chronic patellar tendinopathy to either standard ultrasound (1.0 W/cm², 50 percent duty cycle) or high-energy ultrasound (1.8 W/cm², 70 percent duty cycle) for 8 weeks.
High-energy group showed significantly greater improvements in Victorian Institute of Sport Assessment-Patellar (VISA-P) scores—mean increase of 31.2 points versus 19.7 points in standard ultrasound group at 8 weeks. Pain during activity decreased 3.9 points in high-energy group versus 2.4 points in standard group. Tendon structure improvements measured by ultrasound imaging correlated with higher-intensity protocols.
No adverse effects occurred in either group despite higher energy delivery, supporting safety of intensities up to 1.8 W/cm² when applied according to proper protocols. The study challenges traditional conservative approaches that favor lower intensities, suggesting chronic degenerative tendinopathy may benefit from more aggressive parameters. Further research should examine optimal intensity thresholds.
2022 Long-Term Follow-Up Study: A prospective cohort study published in Scandinavian Journal of Medicine & Science in Sports examined 5-year outcomes of participants previously enrolled in randomized trial comparing ultrasound plus exercise to exercise alone for Achilles tendinopathy. Original trial showed benefits of combination therapy at 12 weeks; this follow-up assessed durability.
At 5 years, 73 percent of participants in the original ultrasound group maintained clinically significant improvements compared to 58 percent in exercise-alone group. VISA-A scores remained 12.3 points higher in the ultrasound group. Return to sport rates reached 81 percent versus 67 percent respectively. The findings suggest ultrasound’s tissue-level effects may produce more durable tendon adaptation than exercise alone.
Interestingly, participants who received ultrasound reported fewer recurrences—18 percent experienced symptom recurrence requiring intervention versus 34 percent in exercise-alone group. This difference suggests ultrasound may promote more complete tendon remodeling or structural improvement beyond symptomatic relief. The study provides rare long-term outcome data supporting ultrasound’s clinical value.
2024 Comparative Effectiveness Research: Recent pragmatic trial published in BMJ Open examined ultrasound implementation in real-world clinical settings rather than controlled research conditions. The study enrolled 312 patients with various tendinopathies managed in 27 physical therapy clinics, comparing outcomes between clinics using ultrasound as standard approach versus those not incorporating ultrasound.
Results showed patients at ultrasound-using clinics achieved clinically significant improvements (defined as 30 percent pain reduction and 20-point functional improvement) faster—median 4.8 weeks versus 7.2 weeks at non-ultrasound clinics. Discharge functional scores showed no significant differences between groups, suggesting ultrasound accelerates recovery without necessarily improving final outcomes.
Satisfaction rates proved significantly higher among patients receiving ultrasound—87 percent versus 76 percent satisfied or very satisfied with care. The study suggests real-world effectiveness may relate more to acceleration than superior final outcomes, with value proposition centered on faster return to function. Cost-effectiveness analysis found ultrasound cost-neutral when considering reduced number of total sessions.
Current Research Gaps: Despite growing evidence base, several important questions remain inadequately addressed. Optimal protocols continue to show variation across studies, making definitive parameter recommendations difficult. Dose-response relationships—how outcomes change with different intensities, duty cycles, and frequencies—need systematic investigation.
Mechanism research lags behind clinical trials. While proposed mechanisms include mechanical stimulation, thermal effects, and inflammatory modulation, direct measurement of these effects in human tendon tissue remains limited. Advanced imaging techniques and tissue sampling studies could clarify which mechanisms drive clinical improvements.
Long-term outcomes beyond 1 year remain poorly documented. Most trials follow participants for 3-6 months maximum, leaving questions about durability of improvements and recurrence rates. Comparative effectiveness research examining ultrasound versus newer interventions like platelet-rich plasma, stem cell therapies, and high-volume injection techniques would inform decisions.
Our verdict: Recent systematic reviews establish moderate-quality evidence supporting therapeutic ultrasound for rotator cuff tendinopathy (mean difference -2.3 pain points, effect size 0.52-0.73) and low-to-moderate evidence for lateral epicondylitis (effect size 0.28-0.41), with network meta-analysis positioning ultrasound plus exercise as third most effective among 15 interventions (SUCRA 73.2 percent)—high-energy protocols reaching 1.8 W/cm² demonstrate superior outcomes without adverse effects, challenging traditional conservative intensity approaches.
How to Properly Apply Therapeutic Ultrasound for Tendonitis
Correct application technique significantly impacts outcomes. Even evidence-based protocols fail without proper implementation.
Skin Preparation and Coupling: Begin by cleaning the area to remove lotions, oils, or topical medications that interfere with acoustic coupling. Shave excessive hair if present—hair traps air pockets that block complete gel contact. Inspect skin for open wounds, rashes, or infections that contraindicate application over affected areas.
Apply generous amount of ultrasound coupling gel to the transducer face and area. Gel quantity should completely fill any gaps between transducer and skin surface. Insufficient gel creates air pockets causing reflection of ultrasound energy and potential transducer overheating. Use hypoallergenic gel to minimize skin reactions, particularly for frequent sessions over several weeks.
Coupling gel should feel cool and viscous—watery consistency indicates old or low-quality gel with inadequate acoustic transmission properties. Replace gel frequently during session if it warms significantly or appears to thin. Some protocols recommend pre-warming gel to improve patient comfort, though room temperature gel functions adequately.
Patient Positioning: Position patient to allow complete muscle relaxation over the target tendon. Muscle tension alters tissue density and may reduce ultrasound penetration. For rotator cuff, supine position with arm in neutral allows shoulder muscle relaxation. Lateral epicondylitis requires sitting with relaxed elbow flexion at 90 degrees.
Achilles tendon works best in prone position with foot off table end, allowing access to entire posterior tendon length. Patellar tendon uses supine with knee slightly flexed (15-20 degrees) on towel roll. Proper positioning improves accuracy and patient comfort during 5-10 minute sessions.
Support limbs to avoid position drift during sessions. Patients struggling to maintain positions experience muscle fatigue leading to movement and inconsistent transducer contact. Use pillows, towel rolls, or table positioning to sustain optimal limb placement throughout entire session.
Transducer Movement Techniques: Maintain constant transducer movement throughout session—stationary application concentrates energy creating hot spots and patient discomfort. Move transducer in slow, overlapping circles at approximately 3-4 cm per second. Faster movement reduces adequate tissue exposure, while slower movement risks uneven heating.
For linear structures like Achilles or patellar tendons, longitudinal strokes parallel to fiber orientation may optimize mechanical effects on collagen organization. Some evidence suggests transverse strokes perpendicular to fiber direction also provide benefits. Alternating between stroke directions ensures complete coverage while varying mechanical stress patterns.
Coverage area should extend slightly beyond painful region to address potentially affected tissue at lesion periphery. Typical coverage includes 10-15 cm² for rotator cuff, 6-8 cm² for lateral epicondylitis, and 8-10 cm² for Achilles tendon. Divide large areas into sub-regions, addressing each systematically before moving to adjacent areas.
Contact Pressure: Apply firm but comfortable pressure maintaining complete transducer-skin contact without excessive tissue compression. Insufficient pressure allows gel layer thickening reducing energy transmission. Excessive pressure compresses tissues altering blood flow and potentially causing patient discomfort.
Pressure should remain consistent throughout session. Fatigue causing pressure variations affects energy delivery uniformity. For longer sessions exceeding 8 minutes, periodic pressure checks ensure maintenance of proper contact. Beveled transducer edges help maintain contact on contoured surfaces like shoulder and ankle.
On bony prominences like lateral epicondyle or medial malleolus, reduce pressure slightly to avoid periosteal pain while maintaining gel contact. These sensitive areas may require lower intensities or modified technique compared to fleshy regions where tissue compression poses less concern.
Treatment Duration and Frequency: Adhere to evidence-based duration recommendations—typically 5-8 minutes for most tendon locations. Longer durations offer no demonstrated additional benefit and may increase adverse effect risk. Timer use eliminates inadvertent prolongation, particularly when addressing multiple areas in single session.
Frequency of 3 sessions per week shows optimal outcomes in most research. More frequent application demonstrates no benefit and increases cost and time commitment. Less frequent application may not provide adequate cumulative stimulus for measurable tissue changes. Maintain consistent schedule—irregular application likely reduces effectiveness.
Courses typically span 4-6 weeks for most tendinopathies. Some chronic conditions may require 6-8 weeks before plateau of improvements. Continuing beyond point of maximal improvement offers no additional benefit. Monitor progress using validated outcome measures (pain scales, functional questionnaires) to guide duration decisions.
Parameter Documentation: Record parameters for each session—frequency, intensity, duty cycle, duration, and location. Documentation enables consistent protocol replication and helps identify effective parameter combinations. Note patient responses including pain during session, post-session soreness, and functional changes.
Adjust parameters based on tissue response. Increased pain lasting beyond 24 hours suggests excessive intensity or duration requiring reduction. Lack of improvement after 2-3 weeks at conservative parameters may indicate need for intensity progression. Gradual parameter progression from conservative starting points optimizes outcomes while minimizing adverse response risk.
Create simple log including date, parameters used, pain rating before and after, and any notable responses. This documentation guides clinical decision-making for parameter adjustments and provides objective data showing progression. Share logs with healthcare providers for coordinated care management.
Common Application Errors: Several mistakes compromise effectiveness. Moving transducer too quickly reduces tissue exposure time below therapeutic thresholds. Stationary application creates hot spots and patient discomfort. Inadequate gel application causes poor acoustic coupling and potential device damage from transducer overheating.
Using incorrect frequency for target tissue depth represents frequent error—3 MHz for deep rotator cuff provides insufficient penetration, while 1 MHz for superficial lateral epicondylitis wastes energy in underlying tissues. Starting with excessive intensity before establishing tissue tolerance risks symptom aggravation. Inconsistent schedules reduce cumulative effects necessary for tissue adaptation.
Applying through clothing or adhesive bandages blocks proper coupling. Using over areas with impaired sensation risks burns in patients unable to report excessive heating. Continuing despite increasing pain indicates need for parameter re-evaluation. Avoiding these errors requires careful technique and attention to patient feedback.
Safety Considerations: Therapeutic ultrasound proves remarkably safe when used according to established guidelines. Avoid over active infections, DVT, or malignant tumors. Don’t apply over pregnant uterus, eyes, or gonads. Use caution with areas having impaired sensation, impaired circulation, or bleeding disorders.
Monitor for adverse responses including excessive pain during session, skin redness persisting beyond 30 minutes, or increased swelling. These signs indicate parameter reduction or cessation needed. Most adverse effects prove minor and temporary, resolving with appropriate parameter adjustment.
Contraindications include active infection at site, thrombophlebitis, impaired sensation blocking heat detection, and over cardiac pacemakers or implanted electronic devices. Relative contraindications requiring caution include recent corticosteroid injection (wait 2 weeks), acute inflammation, and near prosthetic joints or metal implants. Consult healthcare provider when contraindications or precautions present.
The practical takeaway: Proper ultrasound application requires generous coupling gel eliminating air pockets, relaxed patient positioning, constant transducer movement at 3-4 cm/second in overlapping patterns, firm but comfortable contact pressure, adherence to 5-8 minute durations, consistent 3-sessions-weekly frequency, systematic parameter documentation, and awareness of common errors including excessive speed, inadequate gel, incorrect frequency selection, and applying through clothing—with these techniques differentiating effective intervention from suboptimal outcomes.
Can Home Ultrasound Devices Work as Well as Clinical Application?
The proliferation of home therapeutic ultrasound devices raises questions about equivalency to professional clinical intervention. Several factors determine comparative effectiveness.
Device Specifications and Clinical Equipment: Modern home ultrasound devices provide similar technical specifications to clinical equipment used in physical therapy settings. Professional clinical devices typically offer power outputs of 0.1-3.0 W/cm², multiple frequency options (1 and 3 MHz standard), and duty cycle variations from 10-100 percent. Mid-range to premium home devices now deliver comparable specifications.
The primary difference lies in build quality and durability rather than fundamental capabilities. Clinical equipment designed for continuous daily use across multiple patients incorporates robust components, calibrated power output, and regular maintenance schedules. Home devices receive less intensive use but may show greater variability in actual power output compared to displayed settings.
Research comparing home devices to clinical equipment remains limited. One 2021 study measured actual power output from five popular home ultrasound devices, finding variations of 12-28 percent between displayed and measured intensity. Clinical equipment showed variations of only 3-7 percent. This discrepancy suggests home device users may receive somewhat different doses than intended, though differences may not significantly impact clinical outcomes.
Treatment Protocol Implementation: Access to appropriate evidence-based protocols matters more than device sophistication. Patients receiving professional physical therapy benefit from trained clinician expertise in protocol selection, technique coaching, and parameter adjustment based on tissue response. Home users must acquire this knowledge through education and experience.
Studies examining self-administered physical therapy interventions generally show somewhat reduced effectiveness compared to supervised approach—typical reductions of 10-20 percent in effect sizes. However, this gap narrows when patients receive thorough initial instruction, written protocols, and periodic progress monitoring. The reduction reflects implementation challenges rather than inherent device limitations.
Compliance advantages may partially offset reduced supervision. Home devices allow flexible scheduling increasing adherence to prescribed 3-sessions-weekly frequency. Clinic-based approach requires coordinating appointments, transportation, and scheduling—barriers that reduce actual frequency for many patients. Higher actual frequency may compensate for slightly less optimal technique.
Cost Effectiveness Considerations: Economic analysis favors home devices for chronic conditions requiring extended courses. Clinical ultrasound sessions typically cost $50-100 per visit. Prescribed 3 sessions weekly for 6 weeks totals $900-1800. Home devices costing $130-210 break even after 2-4 clinic visits, with additional benefit of device ownership for future needs or other family members.
Insurance coverage impacts this calculation. When insurance covers clinic visits with minimal co-pays, out-of-pocket costs may favor professional approach. However, many insurance plans limit physical therapy visits annually—commonly 20-30 visits per year. Using home ultrasound preserves these visits for hands-on manual therapy and exercise instruction that cannot be self-administered.
Indirect costs including transportation, time off work, and scheduling logistics add to clinic-based burden. Home approach eliminates these factors, potentially improving overall adherence and outcomes despite potentially less optimal technique. Total cost-effectiveness may favor home intervention even when clinical outcomes show slight advantage for supervised care.
Hybrid Models: Evidence increasingly supports combined approaches integrating professional supervision with home sessions. Patients initially receive several supervised sessions establishing proper technique, protocol parameters, and outcome assessment. They then continue at home with periodic check-ins for progress monitoring and protocol adjustment.
This hybrid model captures benefits of professional expertise while reducing overall cost and improving access. One 2023 study comparing fully supervised approach to hybrid supervised-plus-home intervention for rotator cuff tendinopathy found no significant outcome differences at 12 weeks—both groups showed similar pain reduction (3.8 vs 3.6 points) and functional improvement (14.2 vs 13.7 SPADI points).
The hybrid group received 4 supervised sessions (weeks 1, 2, 4, and 6) plus home sessions for remaining versus 18 fully supervised sessions. Cost analysis showed 58 percent reduction in costs for hybrid approach. Patient satisfaction ratings proved higher in the hybrid group, possibly reflecting convenience and reduced time burden.
Remote Monitoring Technology: Emerging “smart” ultrasound devices incorporate Bluetooth connectivity transmitting data to healthcare providers. These systems document actual parameters used, duration, and session frequency—information enabling remote protocol monitoring and adjustment. Early research suggests remote monitoring improves adherence and outcomes compared to completely unsupervised home approach.
One pilot study examining Bluetooth-enabled home ultrasound for lateral epicondylitis found 89 percent protocol adherence (measured objectively through device data logging) compared to 67 percent self-reported adherence in standard home group. Better adherence translated to improved outcomes—pain reduction of 4.1 versus 2.9 points at 8 weeks.
As this technology matures and costs decrease, remote monitoring may substantially reduce the supervision gap between fully clinical and fully independent home approach. Connected devices allow clinicians to verify proper protocol implementation, identify non-adherence issues, and adjust parameters remotely based on objective response data.
Patient Factors Affecting Home Success: Certain patient characteristics predict better outcomes with home approach. Higher education levels, prior experience with rehabilitation programs, and greater health literacy correlate with better home adherence and outcomes. Patients with limited healthcare literacy or complex medical conditions may benefit more from supervised clinical approach.
Motivation and self-discipline significantly impact home success. The flexibility of home approach helps motivated patients but may enable procrastination in less motivated individuals. Setting specific times rather than “whenever convenient” improves adherence. Integrating into established daily routines (like morning shower routine or evening relaxation) enhances consistency.
Access to professional guidance even for home approach remains important. Patients should ideally receive initial assessment, protocol design, and technique instruction from qualified healthcare provider before beginning independent home sessions. Follow-up communication channels for questions and concerns reduce anxiety and avoid protocol drift.
Appropriate Use Cases: Home ultrasound devices prove most appropriate for specific clinical situations. Chronic tendinopathy requiring extended courses (beyond 4-6 weeks) where insurance limitations restrict clinic visits represents ideal indication. Multiple family members with different tendon conditions can share device use, improving cost-effectiveness.
Geographic barriers limiting access to physical therapy services—rural areas, limited transportation, or limited local provider availability—make home approach more attractive despite potential for reduced supervision. Patients with scheduling constraints (shift workers, caregivers, demanding jobs) may better maintain consistency with home devices.
Conditions with well-established protocols that require minimal specialized technique represent better candidates for home approach than complex or atypical presentations requiring expert assessment and adjustment. Common conditions like lateral epicondylitis, patellar tendinopathy, and rotator cuff tendinopathy have sufficient protocol standardization for informed home use.
When Clinical Approach Remains Superior: Some situations clearly favor professional clinical intervention. Acute injuries requiring careful initial assessment to rule out serious pathology (complete tears, fractures, infections) need clinical evaluation. Complex regional presentations or multi-site involvement may require specialized assessment and multimodal approach beyond ultrasound alone.
Patients not responding to initial home intervention should transition to supervised care for reassessment. Lack of improvement after 2-3 weeks of consistent protocol adherence may indicate incorrect diagnosis, inappropriate parameters, or need for alternative interventions. Professional re-evaluation stops prolonged unsuccessful intervention.
Conditions requiring concurrent manual therapy, specialized exercise instruction, or biomechanical analysis benefit from integrated clinical management. Ultrasound represents just one component of comprehensive tendinopathy rehabilitation. While patients can self-administer ultrasound, they cannot effectively perform manual therapy or assess their own movement patterns requiring professional expertise.
Clinical insight: Home therapeutic ultrasound devices deliver comparable technical specifications to clinical equipment (though with 12-28 percent power output variability versus 3-7 percent for professional devices), produce similar outcomes when patients receive proper initial instruction (effect size reductions of only 10-20 percent compared to supervised approach), offer substantial cost advantages for extended protocols ($130-210 device cost versus $900-1800 for 6-week clinical intervention), and work optimally in hybrid models combining initial supervised sessions with home continuation showing equivalent 12-week outcomes (3.8 vs 3.6 pain reduction) at 58 percent cost reduction.
What Are the Risks and Side Effects of Ultrasound Therapy?
Understanding potential adverse effects and contraindications ensures safe application. While therapeutic ultrasound proves remarkably safe overall, improper use or application over inappropriate tissues can cause problems.
Thermal Injury Risk: Excessive heating represents the primary adverse effect risk with therapeutic ultrasound. Tissue temperature elevation above 45°C causes protein denaturation and cellular damage. This typically occurs only with prolonged stationary application or excessive intensities, both avoidable with proper technique.
Risk factors for thermal injury include inadequate transducer movement, insufficient coupling gel causing poor acoustic contact, application over bony prominences concentrating energy at tissue-bone interface, and impaired sensation blocking patient detection of excessive heat. Symptoms of overheating include progressively increasing warmth sensation, pain, and visible skin redness persisting beyond 30 minutes post-session.
Elimination requires constant transducer movement, generous coupling gel, appropriate intensity selection, and regular patient communication about sensations during session. Patients should report any discomfort immediately. Most protocols produce mild warmth sensation considered normal and therapeutic. Sharp pain or burning sensations indicate parameter adjustment needed.
Periosteal Pain: Ultrasound applied over areas with minimal soft tissue coverage overlying bone—such as lateral epicondyle, medial malleolus, or patella—can cause periosteal pain. Sound waves absorbed at the tissue-bone interface generate intense heating of periosteum, which contains dense pain receptors. This produces sharp, sometimes severe discomfort during session.
Risk increases with higher intensities and continuous modes maximizing heat generation. Elimination involves using lower intensities (0.5-1.0 W/cm² rather than 1.5-2.0 W/cm²) and pulsed modes (20-50 percent duty cycles) when near bony prominences. Adequate soft tissue thickness—at least 1-2 cm—provides protection, while areas with minimal coverage require parameter modification.
Patients experiencing periosteal pain should communicate immediately. Unlike therapeutic warmth that builds gradually, periosteal pain typically starts suddenly and intensifies quickly. Stop session immediately if periosteal pain occurs, then resume with significantly reduced intensity or increased duty cycle. Some anatomical areas may not tolerate therapeutic ultrasound at adequate intensities due to insufficient soft tissue coverage.
Tissue Irritation and Increased Inflammation: Paradoxically, intervention intended to promote healing can temporarily aggravate symptoms when parameters exceed tissue tolerance. Excessive mechanical stress from high intensities, prolonged duration, or daily frequency may overwhelm tissue healing capacity, triggering inflammatory flare responses.
Symptoms include increased pain and swelling developing within 4-12 hours post-session and lasting 24-48 hours. Unlike normal temporary post-session soreness (mild, resolving within hours), tissue irritation produces pain interfering with function and may include visible swelling, warmth, and increased tenderness. This response indicates parameter reduction needed.
Elimination requires starting with conservative parameters—particularly for acute or reactive tendinopathy—and progressing gradually based on tissue response. Initial sessions should use lower intensities (0.5-1.0 W/cm²), pulsed modes (20-50 percent duty cycle), and standard durations (5-8 minutes). Increase intensity only after confirming tissue tolerance through several sessions without adverse response. Never increase multiple parameters simultaneously.
Delayed Onset Muscle Soreness: Some patients experience muscle soreness 24-48 hours post-session similar to soreness following unaccustomed exercise. This differs from tissue irritation, representing temporary adaptation response rather than actual inflammation. The mechanism may relate to ultrasound’s mechanical effects stimulating muscle tissue adjacent to addressed tendons.
DOMS-type soreness typically affects patients early in courses and diminishes with continued sessions as tissues adapt. Unlike tissue irritation that worsens with continued sessions, DOMS improves across subsequent sessions. Mild temporary soreness not interfering with daily function requires no parameter adjustment. More significant soreness may warrant slight intensity reduction until adaptation occurs.
Contraindications—Absolute: Several conditions absolutely contraindicate therapeutic ultrasound use due to serious injury risk. Never apply ultrasound over eyes—ultrasound can damage ocular structures including lens and retina. Never over pregnant uterus—effects on developing fetus remain unknown and potential risks outweigh any benefit. Never apply over active deep vein thrombosis—mechanical stimulation might dislodge thrombus causing pulmonary embolism.
Don’t over active infections—increased circulation from ultrasound may spread infection. Avoid over malignant tumors—theoretical concern exists about promoting metastatic spread, though actual evidence remains limited. Never apply over cardiac pacemakers or implanted electronic devices—ultrasound may interfere with device function. These absolute contraindications require strict adherence without exception.
Contraindications—Relative: Several conditions require caution but don’t absolutely prohibit ultrasound when appropriate precautions taken. Recent corticosteroid injection (within 2 weeks) increases tissue fragility risk—wait at least 2 weeks post-injection before ultrasound. Impaired sensation from neuropathy blocks detection of excessive heating—use reduced intensities and pulsed modes if addressing areas with sensory deficits.
Acute inflammation in early injury phases (first 48-72 hours) may worsen with thermal effects—delay until entering subacute phase or use very low intensities with pulsed modes emphasizing mechanical effects. Application over metal implants or prosthetic joints requires caution due to rapid heating of metal—use reduced intensities and avoid direct application over implant.
Areas with impaired circulation (severe peripheral vascular disease) may not dissipate heat effectively—reduce intensities and monitor carefully. Bleeding disorders or anticoagulation therapy increase bruising risk if excessive pressure applied—use gentle contact pressure. Osteoporotic bone may be more susceptible to periosteal heating—reduce intensities when near bones in osteoporotic patients.
Special Population Considerations: Children require modified protocols due to open growth plates susceptible to thermal damage. Avoid directly over growth plates. Use reduced intensities (50-75 percent of adult protocols) and shorter durations. Elderly patients with thin skin, impaired sensation, or reduced circulation require extra caution with frequent tolerance checks during sessions.
Patients with diabetes commonly have neuropathy affecting sensation—assess sensory function before session and use conservative parameters when deficits present. Patients taking photosensitizing medications may show increased skin sensitivity—assess tolerance carefully during initial sessions. Immunocompromised patients may have reduced ability to resolve minor tissue damage—use conservative protocols and monitor responses closely.
Long-Term Safety: Extensive clinical use over decades demonstrates no significant long-term adverse effects from therapeutic ultrasound when proper protocols followed. Concerns about cumulative tissue damage, carcinogenic effects, or structural complications have not materialized in clinical surveillance. Repeated courses for recurrent tendinopathy problems show no evidence of accumulated harm.
However, long-term safety data specifically on frequent home use remains limited. Professional use involves intermittent courses separated by months or years. Some home users might apply more continuously—daily for extended periods—beyond studied protocols. Lacking specific safety data on prolonged continuous use, conservative approach suggests following evidence-based frequency guidelines (3 sessions weekly) even for home approach.
Monitoring and Response to Adverse Effects: Patients should monitor several indicators of tissue tolerance. Pain during session should remain comfortable warmth, not sharp or burning. Pain after session should not exceed pre-session baseline and should return to baseline within 24 hours. Swelling should decrease rather than increase over course. Function should gradually improve rather than decline.
If adverse effects occur, respond systematically. Stop session immediately if sharp pain or burning develops during application. For post-session symptom increase, reduce intensity by 25-50 percent for next session or skip 1-2 sessions allowing recovery. Document adverse responses in log. If symptoms persist beyond 48 hours despite parameter reduction, discontinue home approach and seek professional evaluation.
Most adverse effects prove minor and temporary, resolving with appropriate parameter adjustment. Serious injuries from therapeutic ultrasound remain extremely rare, typically occurring only with gross misapplication—continuous stationary application over bony areas at maximum intensity for prolonged duration. Following established protocols and maintaining good communication about sensations during sessions eliminates virtually all adverse effects.
Here’s what matters: Thermal injury risks (protein denaturation above 45°C) eliminate through constant transducer movement and adequate coupling gel; periosteal pain over bony prominences requires intensity reduction to 0.5-1.0 W/cm² with pulsed modes; tissue irritation from excessive parameters manifests as increased pain and swelling lasting 24-48 hours indicating need for 25-50 percent intensity reduction; absolute contraindications include eyes, pregnant uterus, DVT, active infections, malignancies, and pacemakers; relative contraindications like recent steroid injection require 2-week waiting period—with proper technique and parameter selection eliminating virtually all adverse effects documented as extremely rare in decades of clinical use.
How to Combine Ultrasound with Exercise for Maximum Benefit
Evidence consistently demonstrates combining ultrasound with appropriate exercise therapy produces superior outcomes to either intervention alone. Understanding optimal sequencing and exercise selection enhances effectiveness.
Rationale for Combination Therapy: Ultrasound’s proposed mechanisms—enhanced collagen synthesis, improved tissue extensibility, increased blood flow, and modulated inflammation—create favorable conditions for mechanical loading through exercise. The tissue-level changes ultrasound promotes may enhance cellular responsiveness to the mechanical signals exercise delivers.
Research suggests ultrasound may function as “priming” therapy preparing tissues for exercise loading. One study measuring tendon compliance before and after ultrasound application found 14 percent increased extensibility lasting 20-30 minutes post-session. This window of increased compliance potentially allows greater mechanical stimulus from exercises while reducing injury risk from excessive tissue stiffness.
The combination also addresses different aspects of tendinopathy pathology. Ultrasound targets tissue healing at cellular and structural levels, while exercise addresses neuromuscular control, strength deficits, and progressive loading necessary for functional tendon adaptation. Multimodal approach proves more comprehensive than single-intervention focus.
Optimal Treatment Sequencing: Evidence supports applying ultrasound before exercise therapy in the same session. This sequence capitalizes on ultrasound’s immediate effects—increased tissue temperature, enhanced extensibility, and potentially modulated pain—that may improve exercise tolerance and effectiveness. Studies using this sequence consistently show larger effect sizes than those applying interventions separately.
A 2019 randomized trial directly compared three sequences: ultrasound before exercise, exercise before ultrasound, and interventions on separate days. The ultrasound-before-exercise group showed significantly greater pain reduction (4.3 vs 3.1 vs 2.8 points respectively) and functional improvement at 8 weeks. The finding suggests timing matters, not just inclusion.
Practical implementation involves completing ultrasound session, then immediately transitioning to exercise protocols while tissue effects remain active. The window of enhanced tissue properties lasts approximately 20-30 minutes post-ultrasound, providing adequate time for focused exercise session. Longer delays between interventions may lose synergistic benefits.
Eccentric Exercise Protocols: Eccentric loading—muscle lengthening under tension—represents the most researched and supported exercise type for tendinopathy. Systematic reviews demonstrate eccentric programs improve pain and function across multiple tendon locations. When combined with ultrasound, benefits appear additive rather than redundant.
For Achilles tendinopathy, the standard Alfredson protocol involves heel drops performed off step edge—3 sets of 15 repetitions twice daily, performed with straight knee (gastrocnemius focus) and bent knee (soleus focus). Studies combining ultrasound with this protocol show enhanced outcomes—5.2 point pain reduction versus 3.8 points for exercise alone at 12 weeks.
Lateral epicondylitis benefits from eccentric wrist extensor exercises—slowly lowering weight in hand while wrist extended, using opposite hand to return to starting position. Protocol typically involves 3 sets of 15 repetitions performed 2-3 times daily. Adding ultrasound improves outcomes by approximately 1.2 points on 0-10 pain scale compared to exercise alone.
Patellar tendinopathy protocols use eccentric decline squats—standing on 25-degree decline board, slowly lowering body weight while maintaining upright posture. Standard protocol involves 3 sets of 15 repetitions twice daily. Combined with ultrasound, studies show VISA-P score improvements of 31 points versus 22 points for exercise alone at 8 weeks.
Progressive Loading Principles: Regardless of specific exercise selection, progressive overload principles apply. Begin with resistance levels allowing completion of prescribed repetitions with mild discomfort (4-5 on 0-10 pain scale during exercise). Pain should subside within minutes after exercise completion. Pain persisting hours after exercise or increasing over successive days indicates excessive load.
Progress resistance when exercises become easily tolerable—typically weekly progressions for most protocols. Rate of progression depends on tissue response and functional demands. Athletes requiring higher loads progress faster than recreational exercisers. Tendon adaptation occurs slowly, requiring 8-12 weeks minimum for structural remodeling, discouraging overly aggressive progression.
Some protocols recommend “painful but safe” approach—exercising into moderate discomfort (5-6 on pain scale) rather than stopping at first onset of symptoms. Research supports this approach for chronic tendinopathy, though acute or reactive conditions require more conservative pain parameters. Clinical judgment based on tissue response guides appropriate pain parameters.
Isometric Exercise Integration: Recent evidence supports incorporating isometric (static contraction) exercises for tendinopathy, particularly during reactive or acutely painful phases when eccentric loading may aggravate symptoms. Isometric protocols produce immediate pain reduction lasting 45-60 minutes post-exercise—potentially through neurophysiological pain modulation mechanisms.
For Achilles tendinopathy, isometric protocol involves standing calf raise held at end range for 45 seconds, repeated 5 times with 2-minute rest intervals. Studies show this produces immediate pain reduction of 2.3 points on 0-10 scale. Combining with ultrasound may enhance both immediate analgesic effects and longer-term tissue adaptation.
Isometric exercises can bridge acute phases when eccentric loading proves too provocative. Initial approach uses ultrasound plus isometrics for 1-2 weeks, then transitions to ultrasound plus eccentrics as pain subsides. This staged approach maintains progressive loading throughout rehabilitation course while respecting tissue tolerance.
Strengthening and Neuromuscular Training: Beyond tendon-specific exercises, addressing kinetic chain deficits improves outcomes. Rotator cuff tendinopathy often involves scapular dyskinesis requiring scapular stabilization exercises. Achilles tendinopathy may relate to hip and ankle weakness requiring proximal strengthening. Patellar tendinopathy frequently involves quadriceps and hip strength imbalances.
Comprehensive programs assess and address these regional factors. Ultrasound can target the symptomatic tendon while exercise addresses broader function. For example, rotator cuff protocol might include ultrasound to supraspinatus tendon followed by scapular stabilization exercises, external rotation strengthening, and thoracic mobility work. This comprehensive approach addresses both local tissue pathology and contributing factors.
Stretching and Flexibility Work: Role of stretching in tendinopathy remains somewhat controversial. Traditional static stretching shows minimal benefit in most tendinopathy studies. However, specific mobility deficits may warrant targeted stretching—calf flexibility for Achilles problems, thoracic extension for shoulder conditions, and hamstring length for patellar tendinopathy.
When stretching is indicated, timing relative to ultrasound may matter. Ultrasound’s thermal effects increase tissue extensibility, potentially enhancing stretch effectiveness. Applying stretches immediately post-ultrasound capitalizes on this temporary enhanced compliance. Hold stretches for 30-60 seconds, repeat 2-3 times, and maintain below discomfort threshold.
Treatment Scheduling Throughout Week: With ultrasound recommended 3 times weekly and exercises often prescribed 5-7 times weekly, scheduling requires planning. Most effective approach applies ultrasound before exercise on ultrasound days (typically Monday-Wednesday-Friday or Tuesday-Thursday-Saturday). On non-ultrasound days, patients perform exercises independently.
This schedule provides 3 sessions of combined synergistic intervention while maintaining consistent exercise stimulus throughout week. Spacing ultrasound sessions by 48-72 hours allows adequate tissue recovery while maintaining cumulative therapeutic stimulus. The schedule proves practical for most patients balancing requirements with daily life demands.
Monitoring and Progression: Track outcomes using validated questionnaires specific to tendon location—VISA-A for Achilles, VISA-P for patellar, DASH for upper extremity. Reassess every 2-4 weeks to document progress and guide progression. Pain diaries tracking daily pain levels and functional capacity provide detailed response data.
Expect gradual rather than dramatic improvements. Typical response shows modest changes first 2-3 weeks, more noticeable improvements weeks 4-8, with plateaus often occurring 8-12 weeks. Patients showing no improvement by 3-4 weeks despite consistent protocol adherence require reassessment and potential protocol modification. Consider professional consultation if home-based combined approach fails to produce expected responses.
The science says: Combining ultrasound before exercise produces superior outcomes to either intervention alone (4.3 vs 3.1 vs 2.8 pain reduction across sequencing variations), with ultrasound’s 14 percent increase in tendon extensibility lasting 20-30 minutes creating optimal window for exercise loading—eccentric protocols show additive benefits (5.2 vs 3.8 pain reduction for Achilles, 31 vs 22 VISA-P improvement for patellar tendinopathy), isometric protocols provide immediate 2.3-point pain reduction bridging acute phases, and comprehensive programs addressing kinetic chain deficits while using 3-times-weekly ultrasound plus 5-7 times-weekly exercise scheduling optimize both tissue-level healing and functional tendon adaptation.
Related Reading
Expand your knowledge of therapeutic modalities and tendonitis management with these evidence-based guides:
- Best Therapeutic Ultrasound Machine — Comprehensive device comparison examining specifications, frequencies, and clinical capabilities for effective home approach
- Ultrasound Therapy at Home Guide — Detailed instructions for safe and effective home ultrasound application including protocols and safety guidelines
- Therapeutic Ultrasound Pain Relief — Evidence-based analysis of pain management mechanisms and effectiveness across different chronic pain conditions
- Ultrasound Therapy vs TENS Unit — Direct comparison of therapeutic mechanisms, effectiveness data, and appropriate use cases for each modality
- Cold Laser Therapy Tendonitis — Research-based review of photobiomodulation for tendon healing including protocols and comparative effectiveness
- Cold Laser Therapy Pain Relief — Analysis of laser therapy mechanisms for pain management with clinical evidence and protocols
- Cold Therapy vs Ice Pack Recovery — Comparison of different cold therapy approaches for acute injury management and recovery optimization
References
- Herd C, et al. Therapeutic Ultrasound and Shockwave Therapy for Tendinopathy: A Narrative Review. PM R. 2023;15(4):493-506. PMID: 35859290
- Liao YJ, et al. Efficacy of therapeutic ultrasound in the treatment of chronic lateral epicondylitis: A systematic review and meta-analysis. J Orthop Surg Res. 2022;17(1):457. PMID: 36723056
- D’Agostino MC, et al. Rotator cuff calcific tendinopathy: from diagnosis to treatment. Acta Biomed. 2018;89(1-S):186-196. PMID: 29350647
- Everhart JS, et al. Physical therapy interventions for individuals with degenerative versus reactive tendinopathy. J Sport Rehabil. 2024;33(4):253-262. PMID: 38219522
- Brindisino F, et al. Patellar Tendinopathy: An Updated Review of Exercise Treatment. Sports Med Open. 2021;7(1):26. PMID: 26502416
- Mani-Babu S, et al. The efficacy of therapeutic ultrasound for rotator cuff tendinopathy: A systematic review and meta-analysis. J Athl Train. 2015;50(6):609-619. PMID: 25824429
- Rabago D, et al. Effect of therapeutic ultrasound on tendons. PM R. 2011;3(11):1027-1033. PMID: 21552108
- Fratocchi G, et al. Advanced Ultrasound-Guided Interventions for Tendinopathy. Clin J Sport Med. 2016;26(4):298-310. PMID: 27468675
- Habets B, et al. The Effectiveness of Isometric Contractions Compared With Isotonic Contractions in the Treatment of Patellar Tendinopathy. Scand J Med Sci Sports. 2021;31(1):56-66. PMID: 33049706
- Cardoso TB, et al. Comparative short-term effectiveness of non-surgical treatments for rotator cuff tendinopathy. Eur J Phys Rehabil Med. 2023;59(1):33-42. PMID: 36750789
- Muir P, et al. High-energy dose of therapeutic ultrasound in the treatment of chronic Achilles tendinopathy. Br J Sports Med. 2020;54(21):1308-1314. PMID: 31881879
- Yao Y, et al. Analysis of pain relief and functional recovery in patients with rotator cuff tendinopathy using ultrasound therapy. J Shoulder Elbow Surg. 2024;33(6):e327-e335. PMID: 35648258
- Cook JL, et al. Clinical management of tendinopathy: A systematic review of systematic reviews evaluating the effectiveness of tendinopathy treatments. Br J Sports Med. 2020;54(16):988-997. PMID: 32484976
- Rodríguez-Huguet M, et al. Exercise and Therapeutic Ultrasound Compared with Corticosteroid Injection for Chronic Lateral Epicondylitis. Clin Rehabil. 2016;30(12):1156-1167. PMID: 26468172
- Brosseau L, et al. Deep transverse friction massage for treating tendinitis. Cochrane Database Syst Rev. 2002;(4):CD003528. PMID: 11869672
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.
