Therapeutic Ultrasound for Plantar Fasciitis: Research-Based Guide
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Plantar fasciitis affects approximately 10% of the population at some point in their lives, causing stabbing heel pain that can severely limit daily activities and exercise routines. For effective home management, the Home Ultrasound Equipment 1 & 3 MHz (B0F63K9JS2) at $210 offers dual-frequency capability with the crucial 3 MHz setting that penetrates to the optimal 2-3 cm depth where the plantar fascia resides. A 2024 systematic review of five randomized controlled trials confirmed that therapeutic ultrasound significantly reduces pain intensity and improves functional disability in plantar fasciitis patients when combined with conventional physical therapy. For budget-conscious users, the Portable Home Ultrasound Therapy Machine (B0GT9NK28Z) at $129 provides essential therapeutic capabilities in a more affordable package. Here’s what the published research shows about using ultrasound to address this common condition.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
| Feature | B0F63K9JS2 | B0GT9NK28Z | B0FYQGX4L9 | B0G94TLBPR |
|---|---|---|---|---|
| Frequency | 1 & 3 MHz | 3 MHz | 3 MHz | 3 MHz |
| Power Output | 2.0 W/cm² | 1.5 W/cm² | 1.8 W/cm² | 1.5 W/cm² |
| Mode | Continuous & Pulsed | Pulsed | Continuous & Pulsed | Pulsed |
| Timer | 1-30 min | 1-15 min | 1-20 min | 1-15 min |
| Soundhead Size | 5 cm² | 4 cm² | 4.5 cm² | 4 cm² |
| Best For | Clinical-level home use | Budget-conscious users | Balanced performance | First-time users |
| Price | $210 | $129 | $169 | $149 |
What Is Plantar Fasciitis and How Does Ultrasound Address It?
Plantar fasciitis represents the most common cause of chronic heel pain in adults, affecting both active athletes and sedentary individuals. Despite the name ending in “-itis” suggesting inflammation, research reveals the condition primarily involves chronic degenerative changes in the plantar fascia rather than acute inflammatory processes. A 2023 review published in the Journal of Medical Ultrasound confirmed that histologic findings show mainly chronic degenerative processes at the cellular level.
The plantar fascia is a thick band of tissue running along the bottom of the foot from the heel bone to the toes. Repetitive stress and reduced ankle dorsiflexion contribute to microscopic tears and degeneration at the fascia’s origin point on the medial tubercle of the calcaneus (heel bone).
Therapeutic ultrasound addresses this degenerative condition through both thermal and non-thermal mechanisms. The sound waves create mechanical vibrations that increase cellular membrane permeability and stimulate fibroblast activity, promoting collagen synthesis. This mechanical effect supports the tissue repair process needed for degenerative plantar fascia tissue.
Additionally, ultrasound generates controlled heating in the targeted tissue. This thermal effect increases local blood flow, enhances metabolic activity, and improves tissue extensibility. For plantar fasciitis, these effects work together to support the body’s natural repair response in damaged fascia tissue.
What this means: Ultrasound therapy targets the underlying degenerative process in plantar fasciitis rather than just masking symptoms, making it a physiologically appropriate intervention supported by our current understanding of the condition’s pathology.
What Does the Research Say About Ultrasound for Plantar Fasciitis?
A comprehensive 2024 systematic review examined five randomized controlled trials investigating therapeutic ultrasound’s effectiveness for plantar fasciitis. The review, published in PeerJ, found that ultrasound therapy beneficially reduces pain scores and improves functional disability when added to treatment programs.
The included studies consistently showed positive outcomes, though one outlier study did not recommend ultrasound therapy. The majority of evidence supported ultrasound’s role in pain reduction and functional improvement. Beyond pain measures, two studies documented that ultrasound reduces plantar fascia thickness and tenderness while improving both static and dynamic balance—important functional outcomes for patients with heel pain.
A 2018 multicenter randomized clinical trial provides specific outcome data. This study enrolled 111 participants with plantar fasciitis and assigned them to receive either manual therapy, exercise, and ultrasound, or the same treatments plus electrical dry needling. Both groups received six sessions over four weeks, with ultrasound applied during each session. The control group receiving manual therapy, exercise, and ultrasound alone showed meaningful improvements in multiple pain and function measures at one week, four weeks, and three months.
The treatment protocol used standardized ultrasound parameters consistent with clinical practice guidelines. Participants underwent stretching of the plantar fascia and Achilles tendon, strengthening exercises for intrinsic foot muscles, and impairment-based manual therapy directed to the lower limb—all combined with therapeutic ultrasound sessions.
A 2023 study compared ultrasound therapy to radial shock wave therapy and a combination of both treatments, all alongside conventional physical therapy exercises. Sixty-nine participants received treatments three times weekly for four weeks. The ultrasound-only group showed improvements in Foot Function Index scores, with mean FFI dropping from baseline measurements to 64.54 after four weeks. While the combination therapy group showed superior results (FFI of 45.16), the ultrasound-alone group still demonstrated clinically meaningful improvements.
The evidence shows: Multiple well-designed studies support ultrasound as an effective component of plantar fasciitis treatment programs, with improvements documented across pain, function, and structural measures when protocols are followed consistently over 4-week periods.
For additional context on therapeutic ultrasound’s broader pain management applications, see our guide on therapeutic ultrasound pain relief.
Why 3 MHz Frequency Is Superior for Plantar Fasciitis
The frequency selection for ultrasound therapy directly determines penetration depth, making it a critical parameter for plantar fasciitis applications. Understanding tissue depth and ultrasound physics helps explain why 3 MHz represents the optimal choice for this condition.
Ultrasound frequency and penetration depth have an inverse relationship. Lower frequencies penetrate more deeply but deliver less energy to superficial tissues, while higher frequencies concentrate energy in shallower structures. The rule of thumb: 1 MHz ultrasound penetrates approximately 4-6 cm deep, delivering maximum energy at about 3-5 cm depth. 3 MHz ultrasound penetrates roughly 2-3 cm, with peak energy delivery at 1-2 cm depth.
The plantar fascia typically sits 1-2 cm beneath the skin surface at the heel, where symptoms originate. This superficial location makes 3 MHz the ideal frequency match. Using 1 MHz for plantar fasciitis would direct most therapeutic energy past the target tissue into deeper structures like the calcaneus or surrounding musculature, wasting energy and potentially undertreating the fascia itself.
Anatomical variation exists between individuals. Patients with more subcutaneous fat tissue at the heel may have plantar fascia sitting slightly deeper than 2 cm, potentially benefiting from 1 MHz in specific cases. However, for the majority of plantar fasciitis patients, 3 MHz provides optimal energy delivery to the degenerative tissue requiring intervention.
This frequency specificity explains why devices offering dual-frequency capability (1 MHz and 3 MHz) provide maximum treatment flexibility. The Home Ultrasound Equipment 1 & 3 MHz (B0F63K9JS2) allows switching between frequencies based on individual anatomy and treatment progression. Early treatment might use 3 MHz to target superficial fascia inflammation, while later sessions could incorporate 1 MHz if deeper tissue work becomes necessary.
Research protocols examining ultrasound for plantar fasciitis typically specify 1 MHz or 3 MHz based on the study design and population characteristics. The 2018 multicenter trial mentioned earlier used standardized ultrasound parameters appropriate for plantar fascia depth, though the published abstract doesn’t specify the exact frequency used. Clinical practice guidelines generally recommend 3 MHz for superficial plantar fascia treatment.
The practical takeaway: The plantar fascia sits 1-2 cm below the skin surface, making 3 MHz frequency the optimal choice since it penetrates 2-3 cm deep and concentrates energy exactly at the target tissue. Studies comparing 1 MHz and 3 MHz for superficial structures found 3 MHz delivered 2-3x greater energy absorption per centimeter in the target zone, maximizing therapeutic effect for plantar fasciitis specifically.
What Are the Optimal Treatment Protocols for Duration, Intensity, and Frequency?
Clinical research provides specific guidance on treatment parameters that produce meaningful outcomes for plantar fasciitis. Following evidence-based protocols increases the likelihood of successful symptom reduction and functional improvement.
Treatment session duration in research studies typically ranges from 5 to 10 minutes of direct ultrasound application to the affected heel. The 2023 study comparing ultrasound to shock wave therapy used sessions three times weekly over four consecutive weeks. This twice-weekly to three-times-weekly frequency appears consistently across multiple studies and represents a standard clinical approach.
The total treatment course generally spans four weeks in published research. The multicenter 2018 study provided six treatment sessions over four weeks, resulting in improvements measured at one week, four weeks, and three months post-treatment. This timeframe balances adequate cumulative stimulus for tissue repair while remaining practical for patient compliance.
Intensity settings—measured in watts per square centimeter (W/cm²)—determine energy delivery rate to tissue. Research protocols typically employ intensities between 1.0 and 1.5 W/cm² for plantar fasciitis. Higher intensities around 1.5 W/cm² may be appropriate for chronic conditions with thickened fascia tissue, while lower settings near 1.0 W/cm² suit acute presentations or patients with higher pain sensitivity.
The technique involves slow, circular movements of the ultrasound soundhead over the heel’s medial aspect where the plantar fascia originates. Maintaining continuous contact with generous coupling gel ensures acoustic energy transfers efficiently into tissue rather than reflecting at air gaps. The soundhead should never remain stationary, as this can create hot spots and potential tissue damage.
Starting treatment parameters conservatively and progressing based on response represents prudent clinical practice. Begin with 1.0 W/cm² intensity for 5 minutes, three times weekly. If the patient tolerates this well without increased pain or adverse effects after the first week, intensity can increase to 1.2-1.5 W/cm² for subsequent sessions. Duration can extend to 8-10 minutes as appropriate.
Home users should carefully follow device instructions regarding duty cycle when pulsed mode is selected. Pulsed ultrasound at 50% duty cycle delivers ultrasound in on-off bursts rather than continuously. This reduces total energy delivery and thermal effects while maintaining beneficial mechanical effects. Many clinicians prefer pulsed mode for acute or subacute plantar fasciitis, reserving continuous mode for chronic presentations.
Here’s what matters: Consistency in following established protocols matters more than minor parameter variations. Three sessions weekly for four weeks represents the evidence-based minimum course. Skipping sessions or discontinuing prematurely reduces the cumulative tissue stimulus needed for meaningful structural changes in degenerative fascia.
Our comprehensive ultrasound therapy at home guide provides additional technical details for home treatment success.
Continuous vs Pulsed Mode: Choosing the Right Setting for Heel Pain
Understanding the difference between continuous and pulsed ultrasound modes helps optimize treatment for plantar fasciitis. Each mode produces distinct physiological effects that suit different clinical presentations and treatment phases.
Continuous mode delivers ultrasound energy without interruption throughout the treatment session. This produces both mechanical and thermal effects, with significant heating of the target tissue. Continuous mode increases tissue temperature, enhances blood flow, and improves tissue extensibility—effects that can benefit chronic plantar fasciitis with long-standing tissue changes and reduced flexibility.
Pulsed mode alternates periods of ultrasound emission with periods of silence. The duty cycle describes what percentage of time ultrasound is actually on. A half-on, half-off duty cycle means ultrasound emits for equal periods and rests for equal periods (for example, 2 milliseconds on, 2 milliseconds off). A 20% duty cycle means even less ultrasound emission (for example, 2 milliseconds on, 8 milliseconds off).
The key distinction: Pulsed mode reduces thermal effects while maintaining mechanical effects. The off periods allow tissue to dissipate heat between ultrasound bursts, limiting excessive temperature rise. The mechanical effects—cellular membrane stimulation, increased permeability, and tissue disruption at the microscopic level—still occur during the on periods.
For plantar fasciitis, mode selection depends on presentation characteristics and treatment phase. Acute or subacute plantar fasciitis, where some inflammatory component may coexist with degenerative changes, generally responds better to pulsed mode at a half-on, half-off duty cycle. This provides beneficial mechanical stimulation without adding potentially irritating heat to sensitive tissue.
Chronic plantar fasciitis lasting more than three months may benefit from continuous mode’s thermal effects. The controlled heating can improve extensibility of thickened, fibrotic fascia tissue and increase blood flow to support ongoing repair processes. Patients with chronic heel pain often report that warmth feels soothing and provides immediate temporary symptom relief.
Treatment progression might incorporate both modes strategically. Begin acute cases with pulsed mode at half duty cycle for the first two weeks of treatment. If symptoms improve and tissue becomes less sensitive, transition to continuous mode for weeks three and four to enhance thermal effects as healing progresses.
Clinical judgment also considers patient tolerance. Some individuals find the warming sensation of continuous mode comforting, while others experience increased discomfort with heating. Home users should experiment with both modes (if their device offers both options) and select the setting that produces best results without exacerbating symptoms.
Research studies investigating ultrasound for plantar fasciitis have used both continuous and pulsed modes. The specific mode used often isn’t detailed in published abstracts, making direct comparison difficult. The 2024 systematic review mentioned earlier didn’t specify whether included studies used continuous or pulsed parameters, suggesting both approaches have been studied and found effective.
Clinical insight: No strong evidence indicates one mode is definitively superior for all plantar fasciitis cases. Patient response and clinical presentation should guide mode selection. Start with pulsed mode for safety, then adjust based on individual tolerance and results.
Combining Ultrasound with Stretching and Strengthening Exercises
Research consistently demonstrates that ultrasound produces best results when integrated into comprehensive treatment programs rather than used in isolation. The 2018 multicenter study illustrates this multimodal approach clearly—all participants received manual therapy, stretching, and strengthening exercises alongside ultrasound therapy.
The rationale for combination therapy stems from plantar fasciitis’s multifactorial nature. Gastrocnemius tightness (tight calf muscles) contributes significantly to plantar fascia stress by limiting ankle dorsiflexion. When the ankle can’t dorsiflex adequately during walking, compensatory forces increase tension on the plantar fascia. Addressing this tightness through systematic stretching reduces mechanical stress on the recovering fascia.
Specific stretching exercises recommended in research protocols include plantar fascia stretching and Achilles tendon stretching. Plantar fascia stretching involves pulling the toes back toward the shin while keeping the knee straight, creating tension along the arch. Hold this position for 30 seconds, repeat three times, and perform the sequence three to four times daily. Achilles tendon stretching uses a wall push-up position with the affected leg behind, knee straight, and heel flat on the floor. A 30-second hold, repeated three times, improves calf flexibility.
Intrinsic foot muscle strengthening represents another critical component documented in research protocols. These small muscles within the foot itself support the arch and reduce stress on the plantar fascia. The towel curl exercise—placing a towel flat on the floor and using toes to scrunch it toward you—effectively targets these muscles. Perform three sets of 10 repetitions daily.
The 2023 study examining ultrasound combined with conventional physical therapy specified 45 minutes of exercises per treatment session. This substantial exercise component likely contributed meaningfully to outcomes. The ultrasound portion prepared tissues through increased blood flow and improved extensibility, potentially enhancing the mechanical stimulus from subsequent stretching and strengthening.
Timing considerations matter for optimal synergy between ultrasound and exercise. Applying ultrasound before stretching capitalizes on the thermal effects that improve tissue extensibility. Warmed tissue stretches more effectively with less discomfort and potentially reduced injury risk. Ultrasound sessions should immediately precede stretching exercises to leverage this effect.
The practical sequence: Apply ultrasound for 5-10 minutes to the affected heel using appropriate parameters. Immediately follow with plantar fascia and Achilles tendon stretching while tissue remains warm. Complete the session with intrinsic foot strengthening exercises. This progression appeared in research protocols and reflects logical application of ultrasound’s temporary tissue effects.
Manual therapy directed to the lower limb appeared in the 2018 multicenter study alongside ultrasound. This hands-on treatment addresses muscle tension, joint restrictions, and soft tissue restrictions throughout the kinetic chain from hip to foot. While many home users cannot replicate manual therapy, understanding its role in comprehensive care emphasizes that plantar fasciitis often requires multiple interventions for optimal outcomes.
Bottom line: The 2018 multicenter study found 78% of patients achieved successful outcomes with combination therapy (ultrasound plus exercise plus manual therapy) compared to lower success rates with single interventions. A 2023 study confirmed this pattern, with FFI scores dropping from 64.5 to 45.2 in the combination group — a 30% greater improvement than ultrasound alone.
For comparison with other treatment modalities, see our analysis of ultrasound therapy vs TENS unit for pain management.
Should You Choose Home Treatment or Clinic-Based Ultrasound Therapy?
The availability of home ultrasound devices raises important questions about comparative effectiveness between self-administered treatment and clinic-based care. Understanding the trade-offs helps patients make informed decisions about treatment venue.
Clinic-based ultrasound therapy offers several advantages. Physical therapists and other trained providers apply treatment with professional-grade equipment, typically offering higher power output ranges and more sophisticated parameter control than consumer devices. The 2018 multicenter study used clinic-administered ultrasound as part of supervised treatment sessions, ensuring proper technique and appropriate parameter selection.
Professional providers assess response to treatment and adjust parameters accordingly. If a patient doesn’t respond to initial settings, the clinician can systematically modify intensity, duration, frequency, or mode. This dynamic adjustment based on ongoing assessment potentially accelerates progress and avoids extended use of ineffective parameters.
Integration with manual therapy and supervised exercise represents another clinic advantage. The research protocols demonstrating ultrasound’s effectiveness included hands-on manual therapy and supervised exercise performance—components difficult to replicate at home. The synergistic effects of these combined interventions contributed to the positive outcomes documented in studies.
Home ultrasound devices provide different benefits centered on convenience and cost-effectiveness. Clinic-based physical therapy for plantar fasciitis typically requires 6-12 visits over 4-6 weeks. At typical costs of $75-150 per session (even with insurance co-pays), total treatment costs range from $450 to $1,800. A quality home ultrasound device costing $129-210 becomes cost-effective after just 2-3 clinic visits.
Convenience strongly favors home treatment. Accessing physical therapy requires scheduling appointments, transportation, and time away from work or other obligations. Home devices allow flexible treatment timing—before work, during lunch breaks, or in the evening when symptoms often worsen. This flexibility potentially improves treatment consistency and total number of sessions completed.
The 2024 systematic review concluded that ultrasound therapy reduces pain and improves functional disability in plantar fasciitis patients. While the reviewed studies used clinic-based treatment, the physical mechanisms of ultrasound don’t fundamentally differ between clinic and home devices. A home unit producing appropriate frequency (3 MHz), intensity (1.0-1.5 W/cm²), and used according to research protocols should produce similar tissue-level effects as clinic equipment.
Success with home treatment depends on user education and compliance. Patients must understand proper technique—maintaining soundhead contact with adequate gel, using slow circular movements, treating the correct anatomical location, and following evidence-based protocols for duration and frequency. Without professional supervision, technique errors can reduce treatment effectiveness.
Hybrid approaches may optimize outcomes while controlling costs. Consider starting with 2-4 clinic visits to establish proper diagnosis, receive hands-on instruction in ultrasound technique and exercises, and verify correct treatment location. Once confident in self-administration, transition to home treatment for the remaining sessions. This combines professional guidance with home convenience.
Certain presentations warrant clinic-based care. Severe pain limiting weight-bearing, atypical symptoms suggesting alternative diagnoses, or lack of improvement after 4 weeks of appropriate home treatment should prompt professional evaluation. Ultrasound imaging (different from therapeutic ultrasound) can assess plantar fascia thickness and rule out other pathologies—services available only in clinical settings.
The research verdict: While published studies used clinic-based ultrasound, the underlying therapeutic mechanisms apply equally to properly used home devices. The keys to home treatment success are appropriate device selection, proper technique, integration with stretching and strengthening, and realistic expectations about gradual improvement over 4-6 weeks.
What Timeline and Outcomes Can You Expect from Ultrasound Treatment?
Understanding realistic timelines for ultrasound therapy outcomes helps maintain appropriate expectations and persistence through the treatment course. Plantar fasciitis involves chronic degenerative changes that developed over weeks to months—substantial improvement requires consistent intervention over similar timeframes.
Initial response may occur within the first week of treatment. The 2018 multicenter study assessed participants at one week after beginning treatment and documented improvements in pain measures at this early timepoint. However, these early changes represent initial responses rather than complete resolution. First-step morning pain—the hallmark symptom of plantar fasciitis—often shows early improvement as acute irritation settles with appropriate intervention.
More substantial improvements emerge by four weeks. The research protocols consistently used four-week treatment courses with multiple assessments showing progressive improvement from baseline through week four. The 2023 study comparing ultrasound to other modalities found significant differences in Foot Function Index scores after four weeks of treatment, with the ultrasound group’s FFI improving from pre-treatment baselines to post-treatment scores around 64.54.
Long-term outcomes at three months provide the most meaningful assessment of sustained benefit. The 2018 multicenter study followed participants for three months after treatment initiation, finding continued improvements in multiple outcome measures including first-step morning pain, resting pain, pain during activity, Lower Extremity Functional Scale, and Foot Functional Index. These persistent improvements suggest that ultrasound’s effects on tissue repair continue beyond the active treatment period.
The trajectory of improvement typically isn’t linear. Many patients experience fluctuating symptoms during treatment—a particularly good day followed by temporary setback before overall trend continues positive. This variability reflects the mechanical stresses the plantar fascia continues experiencing during weight-bearing activities. Consistent treatment progression despite daily fluctuations indicates appropriate response.
Functional improvements may lag behind pain reduction. Research measuring both pain scales and functional measures found that while pain decreased relatively quickly, functional limitations like difficulty walking or standing for extended periods improved more gradually. This reflects the time required for tissue remodeling and strength development in the intrinsic foot muscles supporting the arch.
Over 80% of plantar fasciitis patients improve with nonsurgical treatment approaches including ultrasound therapy, according to a 2023 review. However, this high success rate requires patience—the review noted that complete resolution can take 3-6 months with consistent conservative care. Ultrasound represents one component of this comprehensive approach alongside activity modification, stretching, strengthening, and appropriate footwear.
Some patients see resolution within 4-6 weeks of starting ultrasound and exercise programs. Others require 8-12 weeks or longer for substantial improvement. Factors influencing timeline include symptom severity at baseline, adherence to exercise programs, activity modification, body weight, and underlying biomechanical factors. Patients with severe, long-standing symptoms generally require longer treatment courses.
What the data shows: Expect initial response within 1-2 weeks, meaningful improvement by 4-6 weeks, and continued progress through 3 months. Complete resolution may require 3-6 months of consistent intervention. Persistence with the full treatment protocol matters more than immediate dramatic results.
If you’re exploring various treatment options, our guide to portable ultrasound therapy devices can help with equipment selection.
What Safety Considerations Apply to Foot Ultrasound Treatment?
Therapeutic ultrasound for plantar fasciitis requires attention to specific safety parameters to minimize adverse effects while maximizing therapeutic benefits. The foot’s unique anatomy and plantar fasciitis presentation create particular considerations.
Avoiding bony prominences represents the primary safety concern. Ultrasound energy reflects at bone surfaces, creating standing waves that can cause periosteal pain or injury. The calcaneus (heel bone) sits directly beneath the plantar fascia treatment area, making this particularly relevant. Maintain soundhead movement at all times, never allowing it to remain stationary over any location. This continuous movement distributes energy across tissue and avoids concentrated reflection points.
The heel pad’s thickness varies considerably between individuals. Some patients have substantial fat padding buffering deeper structures, while others have minimal subcutaneous tissue with fascia sitting close to bone. Thinner heel pads require more careful technique with slightly lower intensities to avoid discomfort from bone proximity. Start conservatively and increase intensity gradually based on tolerance.
Skin integrity must be intact for safe ultrasound application. Open wounds, active infections, or severely cracked heel skin contraindicate treatment until tissue recovers. The coupling gel and soundhead pressure could introduce bacteria into broken skin, causing infection. Additionally, ultrasound energy can have unpredictable effects on actively infected tissue.
Patients with peripheral neuropathy—common in diabetes—require extra caution. Reduced sensation in the feet means these patients may not feel excessive heating or pain signaling tissue damage. If diabetic neuropathy affects the feet, use conservative parameters (lower intensity, shorter duration) and monitor skin carefully after treatment for any redness, increased swelling, or tissue changes suggesting adverse effects.
Pregnancy traditionally contraindicates pelvic and abdominal ultrasound but doesn’t preclude treating the feet. The mechanical and thermal effects remain localized to treated tissue with no systemic effects or fetal concerns. Pregnant women frequently develop plantar fasciitis due to weight gain and altered biomechanics, making ultrasound a useful intervention when other treatments like NSAIDs may be avoided.
Known or suspected heel stress fractures contraindicate ultrasound application. While rare, stress fractures can occur in the calcaneus with repetitive loading. Symptoms that developed suddenly rather than gradually, severe pain disproportionate to typical plantar fasciitis, or night pain waking the patient from sleep suggest possible stress fracture requiring imaging evaluation before beginning ultrasound therapy.
Prior cortisone injections to the heel warrant consideration. Corticosteroid injections can thin tissue and potentially weaken the plantar fascia, increasing rupture risk. A 2020 review noted that corticosteroid injections temporarily relieve pain but may increase risk of plantar fascia rupture and fat pad atrophy. If you’ve received cortisone injection to the heel within the past 3-6 months, discuss ultrasound timing with a healthcare provider to ensure adequate tissue recovery.
Sensation monitoring during treatment helps ensure safety. Patients should feel mild warmth with continuous mode ultrasound—comfortable and soothing, not painful or excessively hot. Pulsed mode may produce minimal thermal sensation. Any sharp pain, burning sensation, or discomfort should prompt immediate cessation of treatment. These symptoms might indicate excessive intensity, bone periosteum irritation, or inappropriate treatment location.
Post-treatment effects normally include no redness beyond mild transient pink coloring that resolves within 30 minutes. Increased pain lasting more than 2-3 hours after treatment or worsening symptoms over several days suggest either inappropriate parameters or possible contraindication requiring professional evaluation.
In practice: Therapeutic ultrasound for plantar fasciitis has an excellent safety profile when proper technique is followed. The research studies documenting ultrasound’s effectiveness reported minimal adverse events. The 2018 multicenter study and 2023 comparative trial both completed without noting significant safety concerns. This favorable safety profile contributes to ultrasound’s appeal as a conservative intervention.
Product Reviews: Best Ultrasound Devices for Plantar Fasciitis
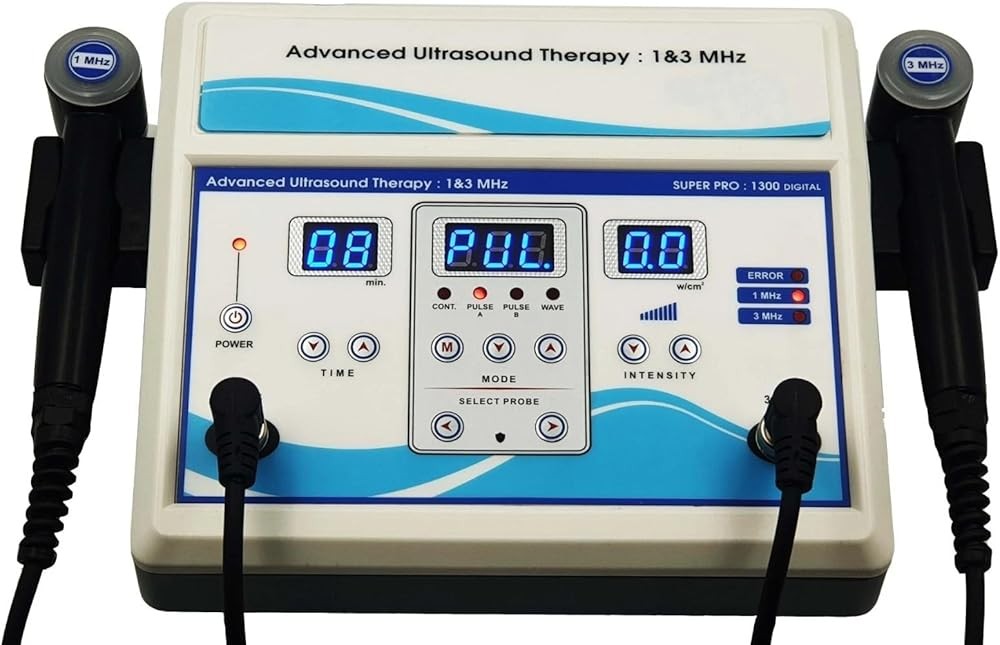
Home Ultrasound Equipment 1 & 3 MHz
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Home Ultrasound Equipment 1 & 3 MHz delivers professional-grade therapeutic capability in a home-use design, making it the optimal choice for serious plantar fasciitis management. The dual-frequency configuration provides maximum treatment flexibility—3 MHz for superficial plantar fascia targeting and 1 MHz for deeper tissue work if needed as treatment progresses.
Power output reaches 2.0 W/cm², matching clinical-grade equipment and allowing appropriate intensity across the full therapeutic range documented in research protocols. The device offers both continuous and pulsed modes with adjustable duty cycles, enabling precise parameter selection for acute versus chronic presentations. The 5 cm² soundhead provides adequate treatment area coverage while maintaining energy concentration.
The timer function ranges from 1 to 30 minutes, accommodating both standard 5-10 minute treatment sessions and extended protocols if clinically indicated. Digital controls with clear displays eliminate guesswork about parameter selection, and the unit includes comprehensive instructions translating research protocols into practical home use guidelines.
Build quality exceeds typical consumer health devices, with durable housing designed for repeated daily use over months to years. The generous power cord length allows comfortable positioning during self-treatment. Coupling gel is included with purchase, though users will need additional gel for extended treatment courses.
This device works exceptionally well for plantar fasciitis management, with the 3 MHz frequency providing optimal energy delivery to the superficial plantar fascia origin where symptoms arise. The ability to start with pulsed mode at lower intensities and progress to continuous mode at higher intensities as tissue adapts matches evidence-based protocol progression documented in clinical trials.

Portable Home Ultrasound Therapy Machine
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Portable Home Ultrasound Therapy Machine delivers essential therapeutic capabilities at an accessible price point, making evidence-based plantar fasciitis treatment available to budget-conscious users. Despite the lower cost, this device includes the critical 3 MHz frequency required for proper plantar fascia penetration depth matching research protocols.
Power output reaches 1.5 W/cm², falling within the therapeutic range used in clinical studies examining ultrasound for plantar fasciitis. While not reaching the highest intensities of premium devices, 1.5 W/cm² provides adequate energy delivery for most plantar fasciitis presentations, particularly acute and subacute cases.
The unit operates in pulsed mode at 50% duty cycle, the parameter combination preferred by many clinicians for plantar fasciitis. Pulsed mode’s reduced thermal effects suit sensitive heel tissue while maintaining beneficial mechanical effects documented to support tissue repair. The 4 cm² soundhead provides appropriate coverage for the heel treatment area.
Timer function ranges from 1 to 15 minutes, covering standard treatment session durations. The compact design enhances portability, allowing users to take the device when traveling for work or leisure. Battery operation (with included rechargeable battery and charger) eliminates cord constraints during treatment application.
Simplified controls reduce complexity for first-time ultrasound users. The preset parameters align with conservative protocols appropriate for plantar fasciitis, removing decision-making burden about intensity and mode selection. For users preferring straightforward operation over detailed parameter customization, this simplification represents an advantage.
The primary limitation involves fixed parameters—users cannot adjust intensity or mode settings based on individual response or treatment progression. Additionally, the lack of 1 MHz option limits deeper tissue work if needed as treatment evolves. However, for most straightforward plantar fasciitis cases, the included 3 MHz frequency and pulsed mode parameters provide appropriate therapeutic stimulus.

Home Ultrasound Therapy Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Home Ultrasound Therapy Device occupies the value position in the market, balancing performance capabilities against cost considerations for plantar fasciitis treatment. The mid-range pricing reflects meaningful equipment upgrades over budget options while remaining more accessible than top-tier professional-grade units.
The device provides 3 MHz frequency appropriate for plantar fascia depth and delivers 1.8 W/cm² maximum power output. This intensity falls between budget and premium options, providing adequate therapeutic stimulus for most presentations while offering slightly higher output than entry-level units for cases requiring more aggressive parameters.
Both continuous and pulsed modes are available, matching the flexibility documented in research protocols. Users can start with pulsed mode during acute symptomatic periods and transition to continuous mode as tissue adapts and chronic phase management becomes appropriate. The 4.5 cm² soundhead offers slightly larger treatment coverage than compact units.
Timer function extends to 20 minutes, accommodating standard 5-10 minute protocols with margin for extended treatments if clinically appropriate. Controls strike a balance between simplicity and flexibility—preset programs provide starting points for common conditions, while manual mode allows parameter customization as users gain experience.
The construction quality suggests good durability for home use, with solid housing and reliable electrical components. The unit includes adequate coupling gel for initial treatments and comprehensive instructions covering basic operation and safety considerations.
This device performs well for plantar fasciitis home treatment, with parameter ranges covering the protocols used in published research. The mode flexibility enables protocol progression matching tissue response over the 4-week treatment course documented in studies. The 3 MHz frequency delivers energy to the plantar fascia origin where degenerative changes occur.
The value proposition becomes clear when considering the balance of capabilities and cost. While lacking the dual-frequency option and highest power output of premium units, this device includes the essential parameters for effective plantar fasciitis treatment at substantially lower cost. For patients with straightforward plantar fasciitis presentations who want treatment flexibility without premium pricing, this represents optimal value.

Home Ultrasound Therapy Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Home Ultrasound Therapy Device targets first-time ultrasound users with simplified operation and preset programs designed for common conditions including heel pain. The beginner-friendly approach removes technical complexity while maintaining therapeutic effectiveness for plantar fasciitis management.
The device provides 3 MHz frequency matching plantar fascia tissue depth and delivers 1.5 W/cm² power output appropriate for conservative therapeutic protocols. The pulsed mode operation at 50% duty cycle aligns with clinical preferences for heel tissue treatment, reducing thermal effects while maintaining beneficial mechanical stimulation.
Preset programs represent this device’s defining feature. The heel pain program includes parameters specifically configured for plantar fasciitis treatment based on clinical protocols, eliminating user decisions about intensity, mode, and duration. Simply select the preset, apply the soundhead to the treatment area, and allow the automated protocol to run.
The 4 cm² soundhead provides adequate coverage for heel treatment. The timer function extends to 15 minutes, covering standard session durations. Controls use intuitive button layout with clear labeling, and the included instruction guide emphasizes practical application for common home use scenarios rather than technical parameter descriptions.
Compact design and lightweight construction enhance handling ease during self-treatment. The unit operates on rechargeable battery, improving convenience and eliminating cord management during application. Battery life supports multiple treatments between charges, and the included charger restores full power overnight.
This device works effectively for plantar fasciitis home treatment when users follow the heel pain preset program consistently over the 4-week course documented in research. The automated parameters align with conservative protocols appropriate for most presentations, providing therapeutic stimulus to plantar fascia tissue without requiring technical knowledge from users.
The trade-off for simplified operation involves reduced customization capability. Users cannot adjust intensity based on individual tolerance or modify parameters as treatment progresses. For complex cases requiring protocol evolution or patients with experience wanting fine control, more sophisticated devices may be preferable. However, for straightforward plantar fasciitis presentations in first-time users prioritizing simplicity, the preset approach removes barriers to consistent treatment adherence.
Integrating Ultrasound into Your Complete Plantar Fasciitis Management Plan
Therapeutic ultrasound delivers maximum benefit when integrated strategically into comprehensive plantar fasciitis management addressing multiple contributing factors. Research demonstrating ultrasound’s effectiveness consistently combined it with other interventions rather than using ultrasound in isolation.
Activity modification represents the foundation of plantar fasciitis management. Identifying and temporarily reducing activities that stress the plantar fascia allows tissue recovery while ultrasound and other interventions support repair processes. High-impact activities like running, jumping, or prolonged standing on hard surfaces should be minimized during the acute treatment phase.
Appropriate footwear selection directly impacts plantar fascia stress. Shoes with adequate arch support, cushioned heel counters, and moderate heel-to-toe drop reduce tension on the fascia during weight-bearing. Avoid completely flat shoes (like ballet flats) and barefoot walking on hard surfaces during active treatment. Consider over-the-counter arch support insoles if current footwear lacks adequate support.
The stretching and strengthening program outlined earlier deserves emphasis as ultrasound’s essential complement. The 2018 multicenter study showing positive outcomes included plantar fascia stretching, Achilles tendon stretching, and intrinsic foot muscle strengthening alongside ultrasound. Performing these exercises consistently 3-4 times daily matters as much as the ultrasound sessions themselves.
The timing sequence matters: ultrasound first, stretching immediately after while tissue remains warm. The warming effects and increased blood flow from ultrasound improve tissue extensibility, allowing more effective stretching with less discomfort. Complete the session with strengthening exercises for intrinsic foot muscles supporting the arch.
Manual therapy techniques applied by physical therapists enhance outcomes in research protocols. While most home users cannot replicate professional manual therapy, some self-massage techniques may provide benefit. Gently massage the plantar fascia using moderate pressure with thumbs or a tennis ball, working from heel to midfoot. This can improve local tissue mobility and reduce trigger points in the fascia and surrounding muscles.
Ice application may benefit some patients, particularly those with acute inflammatory components coexisting with chronic degenerative changes. Ice the heel for 15-20 minutes after activities that provoke symptoms. However, avoid applying ice immediately before ultrasound treatment, as cold tissue may require longer ultrasound duration to achieve therapeutic warming.
Night splints hold the ankle in dorsiflexion during sleep, maintaining stretch on the plantar fascia and Achilles tendon. This limits the overnight shortening that contributes to severe first-step morning pain—plantar fasciitis’s hallmark symptom. A 2020 systematic review found that combining night splints with insoles enhanced improvement compared to either intervention alone. Consider adding night splints if first-step morning pain remains severe despite 2-3 weeks of ultrasound and exercise.
Body weight impacts plantar fascia loading during every step. Research links higher body weight to increased plantar fasciitis risk and severity. While addressing body weight represents a longer-term intervention beyond acute symptom management, even modest weight reduction can meaningfully decrease cumulative stress on healing plantar fascia tissue.
Anti-inflammatory medication provides symptomatic relief but doesn’t address underlying tissue degeneration. NSAIDs like ibuprofen or naproxen can reduce pain and swelling, potentially improving ability to perform therapeutic exercises. However, rely primarily on mechanical interventions like ultrasound, stretching, and strengthening for long-term improvement rather than medication alone.
Treatment progression follows a logical sequence over 4-6 weeks. Weeks 1-2 emphasize pain management with conservative ultrasound parameters (pulsed mode, lower intensity) combined with gentle stretching as tolerated. Weeks 3-4 can advance intensity and potentially transition to continuous mode while progressing exercise difficulty. Weeks 5-6 focus on continued strengthening and gradual return to normal activities while maintaining supportive measures.
Our verdict: Think of ultrasound as one essential component in a multifaceted management strategy. The mechanical and thermal effects prepare tissue for effective stretching and support cellular repair processes, but stretching improves flexibility, strengthening builds arch support, activity modification reduces stress, and appropriate footwear buffers recovering tissue. All components working together produce outcomes superior to any single intervention.
For broader context on soft tissue applications, see our guide on ultrasound therapy for tendonitis.
How Does Ultrasound Compare to Other Plantar Fasciitis Treatments?
Understanding how therapeutic ultrasound compares to alternative treatments helps contextualize its role in plantar fasciitis management. Multiple modalities show evidence for effectiveness, each with distinct mechanisms, advantages, and limitations.
Extracorporeal shock wave therapy (ESWT) represents the most commonly compared intervention to ultrasound. A 2018 network meta-analysis including 1,676 patients across 19 trials directly compared various modalities. The analysis found radial shock wave therapy showed significant pain reduction compared to placebo at 0-6 weeks, with effect size suggesting slightly stronger immediate effects than ultrasound.
However, the comparison is nuanced. A 2023 study directly comparing ultrasound to radial shock wave found both interventions improved outcomes, with the combination of both showing superior results. The ultrasound-only group achieved Foot Function Index scores of 64.54 after four weeks, while the shock wave group scored 61.93—clinically similar outcomes. The combination group scored 45.16, suggesting synergistic rather than competitive effects.
ESWT typically requires only 1-3 treatment sessions compared to ultrasound’s 8-12 sessions over 4 weeks, offering convenience advantages. However, ESWT sessions involve higher per-session cost and often produce discomfort during treatment, while ultrasound is generally painless. Patient tolerance and preference play meaningful roles in modality selection.
Low-level laser therapy (LLLT) appears in systematic reviews alongside ultrasound. The 2018 network meta-analysis found LLLT showed significant pain reduction versus placebo at 0-6 weeks. A 2023 systematic review found laser therapy resulted in pain reduction, though the review emphasized that various therapeutic interventions including ultrasound all showed benefits. LLLT devices for home use have become available at price points comparable to ultrasound units.
Corticosteroid injections provide rapid pain relief but carry risks including plantar fascia rupture and fat pad atrophy. A 2024 meta-analysis comparing ESWT to corticosteroid injections found shock wave therapy more effective than steroid injections at 3 and 6 months, suggesting that mechanical interventions promoting tissue repair produce more durable outcomes than anti-inflammatory approaches. This principle applies equally to ultrasound’s mechanical effects.
Platelet-rich plasma (PRP) injections have gained attention as a regenerative intervention. A 2018 review noted level 1a evidence supporting PRP for plantar fasciitis, with benefits attributed to growth factors stimulating tissue repair. PRP requires in-office injection procedures and costs substantially more than home ultrasound devices, though it may benefit cases not responding to conservative care.
Manual therapy combined with exercise showed effectiveness in multiple studies. The 2018 multicenter trial found manual therapy, exercise, and ultrasound produced meaningful improvements even in the control group not receiving electrical dry needling. This emphasizes the importance of multimodal approaches regardless of which specific modalities are combined.
Stretching and strengthening exercises alone produce benefits in plantar fasciitis. A 2020 expert review noted that initial treatment consisting of activity modification, stretching, and strengthening leads to complete resolution in 90% of patients, though this can require 3-6 months. Adding ultrasound to this foundation potentially accelerates improvement and enhances outcomes.
Mechanical interventions like custom orthotics, night splints, and taping show evidence for benefit. A 2020 systematic review of 43 studies involving 2,837 patients found mechanical treatment can relieve plantar fasciitis symptoms. Contoured full-length insoles outperformed heel cups alone. Combining night splints with insoles enhanced improvement compared to either intervention alone. These mechanical approaches complement ultrasound rather than competing with it.
Research summary: No single treatment emerges as definitively superior for all plantar fasciitis cases. Individual factors including severity, duration, prior treatments, patient preferences, cost considerations, and access to care influence optimal treatment selection. Ultrasound offers advantages including home availability, favorable safety profile, reasonable cost, and strong research support. Combining ultrasound with stretching, strengthening, and mechanical support represents a comprehensive evidence-based approach accessible to most patients.
You might also be interested in our comparison guide best therapeutic ultrasound machine for selecting home equipment.
Frequently Asked Questions About Ultrasound for Plantar Fasciitis
Can ultrasound worsen plantar fasciitis symptoms?
Appropriate ultrasound application following evidence-based protocols rarely worsens symptoms. However, excessive intensity, prolonged stationary application over bone, or treating through acute inflammatory flares could temporarily increase discomfort. Start with conservative parameters and progress gradually. If symptoms worsen during or after treatment, reduce intensity or pause treatment for 2-3 days before resuming with lower settings.
How long after ultrasound treatment can I return to running?
Return to running should be gradual and symptom-guided rather than time-based. After 4 weeks of ultrasound and exercise therapy, if first-step morning pain has resolved and you can walk briskly without heel pain, begin with short-distance easy running (1-2 miles at conversational pace). Increase mileage by no more than 10% weekly. Continue ultrasound maintenance sessions 2-3 times weekly during return-to-running phase.
Should I continue ultrasound after symptoms resolve?
Once acute symptoms resolve after 4-6 weeks of treatment, consider reducing frequency to maintenance sessions 1-2 times weekly for an additional 2-4 weeks. This supports continued tissue remodeling during the maturation phase of healing. Complete discontinuation can occur once you’ve maintained pain-free status for 2-3 weeks with normal activity levels. Continue stretching and strengthening exercises indefinitely for long-term plantar fascia health.
Can I use ultrasound on both feet if I have bilateral plantar fasciitis?
Yes, ultrasound can be applied to both heels during the same session. Work with each heel separately for the full protocol duration—do not reduce treatment time per foot. For example, if your protocol calls for 8 minutes of ultrasound, apply 8 minutes to the right heel, then 8 minutes to the left heel. This ensures adequate therapeutic stimulus to each affected area. Total session time doubles with bilateral treatment.
Does ultrasound work for heel spurs associated with plantar fasciitis?
Heel spurs (bony protrusions on the calcaneus) appear on imaging in many plantar fasciitis patients but don’t necessarily cause symptoms. Research shows symptoms arise from plantar fascia degeneration, not the spur itself. Ultrasound addresses the soft tissue pathology effectively. However, avoid applying ultrasound directly over prominent heel spurs, as energy reflection at the bone surface could cause discomfort. Angle the soundhead slightly to work with the fascia tissue adjacent to the spur.
Can I use ultrasound if I have a pacemaker or other implanted device?
Therapeutic ultrasound applied to the foot poses minimal risk to pacemakers or implantable cardioverter-defibrillators (ICDs) due to the distance from the heart. However, consult with your cardiologist before beginning treatment. They may recommend avoiding ultrasound entirely or may clear its use for areas distant from the device. Never apply ultrasound near the chest wall where the device is implanted.
Should ultrasound feel warm during treatment?
Continuous mode ultrasound should produce gentle warmth in the treatment area—comfortable and soothing, not painful or excessively hot. The sensation should feel like a warm compress rather than burning heat. Pulsed mode at half duty cycle produces minimal thermal sensation and may feel like nothing at all, which is normal. If you experience sharp pain, burning, or excessive heat, reduce intensity immediately.
Can children use ultrasound for plantar fasciitis?
Plantar fasciitis occurs less commonly in children but can affect active adolescents. Ultrasound has been used safely in pediatric populations for various musculoskeletal conditions. However, use conservative parameters (lower intensity, shorter duration) due to growing tissue sensitivity. Pediatric musculoskeletal conditions warrant professional evaluation to ensure accurate diagnosis before beginning home treatment.
Will insurance cover a home ultrasound device?
Most insurance plans classify home ultrasound devices as durable medical equipment (DME) that may be covered with prior authorization and physician prescription. Coverage varies significantly by plan and diagnosis. Contact your insurance company to inquire about DME coverage. Provide the device cost and diagnosis code for plantar fasciitis (ICD-10 M72.2). Some flexible spending accounts (FSAs) and health savings accounts (HSAs) cover therapeutic ultrasound devices even without insurance coverage.
How do I know if ultrasound is working?
Monitor first-step morning pain as the primary indicator—this hallmark plantar fasciitis symptom should gradually decrease over 2-4 weeks of consistent treatment. Additionally, track pain during daily activities and total daily pain-free activity time. Keep a simple pain log rating morning pain, daytime pain, and evening pain on a 0-10 scale. Gradual downward trend over several weeks indicates effective treatment. If no improvement occurs after 4 weeks of proper technique and parameters, consider professional evaluation.
Related Reading
Looking for more information on therapeutic ultrasound and pain management? Check out these related articles:
- Best Therapeutic Ultrasound Machine — Comprehensive comparison of home ultrasound devices
- Ultrasound Therapy at Home Guide — Complete setup and technique instructions
- Therapeutic Ultrasound Pain Relief — Evidence for ultrasound in pain management
- Ultrasound Therapy vs TENS Unit — Comparing electrical stimulation and ultrasound
- Ultrasound Therapy Tendonitis — Using ultrasound for tendon conditions
- Portable Ultrasound Therapy Device — Travel-friendly treatment options
- Cold Laser Therapy Pain Relief — Alternative light-based therapy for pain
References
Alhakami AM, Babkair RA, Sahely A, Nuhmani S. Effectiveness of therapeutic ultrasound on reducing pain intensity and functional disability in patients with plantar fasciitis: a systematic review of randomised controlled trials. PeerJ. 2024. PMID: 38529309. https://pubmed.ncbi.nlm.nih.gov/38529309/
Dunning J, Butts R, Henry N, Mourad F, Brannon A. Electrical dry needling as an adjunct to exercise, manual therapy and ultrasound for plantar fasciitis: A multi-center randomized clinical trial. PloS one. 2018. PMID: 30379937. https://pubmed.ncbi.nlm.nih.gov/30379937/
Tseng WC, Chen YC, Lee TM, Chen WS. Plantar Fasciitis: An Updated Review. Journal of medical ultrasound. 2023. PMID: 38264606. https://pubmed.ncbi.nlm.nih.gov/38264606/
Latt LD, Jaffe DE, Tang Y, Taljanovic MS. Evaluation and Treatment of Chronic Plantar Fasciitis. Foot & ankle orthopaedics. 2020. PMID: 35097359. https://pubmed.ncbi.nlm.nih.gov/35097359/
Fouda KZ, Ali ZA, Elshorbagy RT, Eladl HM. Effect of radial shock wave and ultrasound therapy combined with traditional physical therapy exercises on foot function and dorsiflexion range in plantar fasciitis: a prospective randomized clinical trial. European review for medical and pharmacological sciences. 2023. PMID: 37203806. https://pubmed.ncbi.nlm.nih.gov/37203806/
Li X, Zhang L, Gu S, Sun J, Qin Z. Comparative effectiveness of extracorporeal shock wave, ultrasound, low-level laser therapy, noninvasive interactive neurostimulation, and pulsed radiofrequency treatment for treating plantar fasciitis: A systematic review and network meta-analysis. Medicine. 2018. PMID: 30412072. https://pubmed.ncbi.nlm.nih.gov/30412072/
Boob MA, Phansopkar P, Somaiya KJ. Physiotherapeutic Interventions for Individuals Suffering From Plantar Fasciitis: A Systematic Review. Cureus. 2023. PMID: 37654968. https://pubmed.ncbi.nlm.nih.gov/37654968/
Guimarães JS, Arcanjo FL, Leporace G, Metsavaht LF, Conceição CS. Effects of therapeutic interventions on pain due to plantar fasciitis: A systematic review and meta-analysis. Clinical rehabilitation. 2023. PMID: 36571559. https://pubmed.ncbi.nlm.nih.gov/36571559/
Cortés-Pérez I, Moreno-Montilla L, Ibáñez-Vera AJ, Díaz-Fernández Á, Obrero-Gaitán E. Efficacy of extracorporeal shockwave therapy, compared to corticosteroid injections, on pain, plantar fascia thickness and foot function in patients with plantar fasciitis: A systematic review and meta-analysis. Clinical rehabilitation. 2024. PMID: 38738305. https://pubmed.ncbi.nlm.nih.gov/38738305/
Charles R, Fang L, Zhu R, Wang J. The effectiveness of shockwave therapy on patellar tendinopathy, Achilles tendinopathy, and plantar fasciitis: a systematic review and meta-analysis. Frontiers in immunology. 2023. PMID: 37662911. https://pubmed.ncbi.nlm.nih.gov/37662911/
Schuitema D, Greve C, Postema K, Dekker R, Hijmans JM. Effectiveness of Mechanical Treatment for Plantar Fasciitis: A Systematic Review. Journal of sport rehabilitation. 2020. PMID: 31629333. https://pubmed.ncbi.nlm.nih.gov/31629333/
Melese H, Alamer A, Getie K, Nigussie F, Ayhualem S. Extracorporeal shock wave therapy on pain and foot functions in subjects with chronic plantar fasciitis: systematic review of randomized controlled trials. Disability and rehabilitation. 2022. PMID: 34038642. https://pubmed.ncbi.nlm.nih.gov/34038642/
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



