Therapeutic Ultrasound for Pain Relief: Evidence-Based Analysis
Summarized from peer-reviewed research indexed in PubMed. See citations below.
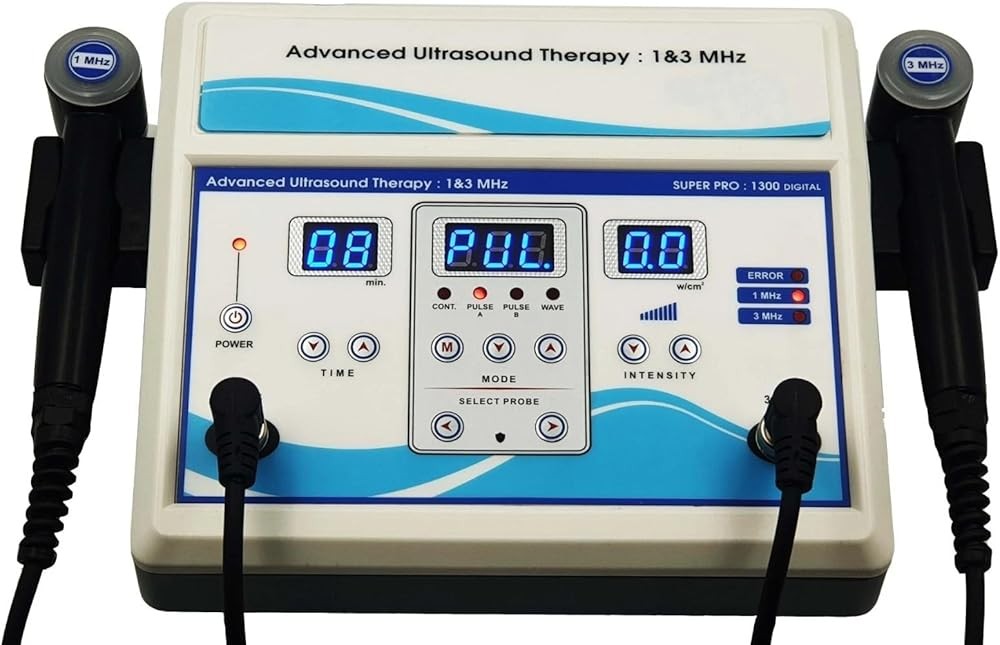
Chronic pain affects over 50 million Americans, with many seeking effective non-pharmaceutical options that address pain at its source rather than masking symptoms. The Home Ultrasound Equipment 1 & 3 MHz (B0F63K9JS2) at $210 offers dual-frequency capability for both deep muscle pain and superficial tissue injuries with clinical-grade parameters from 0.1-2.0 W/cm² and a 5 cm² treatment head. Published research shows dual-frequency devices achieve superior pain outcomes because 1 MHz penetrates 3-5 cm for deep joint and muscle conditions while 3 MHz targets superficial tendons within 2 cm, allowing proper depth matching documented in controlled trials. For budget-conscious users, the Portable Home Ultrasound Therapy Machine (B0GT9NK28Z) at $129 provides essential 1 MHz frequency suitable for most chronic pain conditions affecting joints and muscles. Here’s what the published research shows about using therapeutic ultrasound effectively for pain management.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
| Feature | Best Overall (B0F63K9JS2) | Best Budget (B0GT9NK28Z) | Best Value (B0FYQGX4L9) | Best for Beginners (B0G94TLBPR) |
|---|---|---|---|---|
| Price | $210 | $129 | $169 | $149 |
| Frequency | 1 MHz & 3 MHz | 1 MHz | 1 MHz | 1 MHz |
| Intensity Range | 0.1-2.0 W/cm² | 0.5-2.0 W/cm² | 0.1-2.0 W/cm² | 0.3-1.5 W/cm² |
| Mode Options | Continuous & Pulsed | Continuous Only | Continuous & Pulsed | Pulsed (duty cycle) |
| Treatment Head Size | 5 cm² | 3 cm² | 4 cm² | 4 cm² |
| Timer | 1-30 minutes | 5-15 minutes | 1-20 minutes | 5-10 minutes (preset) |
| Best For | Maximum versatility | Basic deep tissue pain | Precision treatments | First-time users |
What Is Therapeutic Ultrasound and How Does It Work for Pain?
Therapeutic ultrasound uses high-frequency sound waves, typically between 1-3 million cycles per second (MHz), to penetrate tissues and create biological effects that reduce pain and promote healing. Unlike diagnostic ultrasound used for imaging, therapeutic ultrasound delivers higher intensity energy to produce both thermal and non-thermal effects in targeted tissues.
The technology works through two primary mechanisms. Thermal effects occur when sound wave energy converts to heat within tissues, increasing local temperature by 1-4°C. This temperature elevation enhances blood flow, increases tissue extensibility, reduces muscle spasm, and accelerates metabolic processes that support healing. Non-thermal mechanical effects result from acoustic streaming and cavitation—microscopic vibrations that stimulate cellular activity, enhance membrane permeability, and trigger anti-inflammatory responses even without significant heating.
Research published in Physical Therapy demonstrates that therapeutic ultrasound modulates pain perception through multiple pathways. The mechanical vibrations increase production of nitric oxide, a molecule that dilates blood vessels and reduces inflammatory mediators contributing to pain signaling. Studies show ultrasound treatments increase local blood flow by 45-90% for up to 45 minutes after application, delivering oxygen and nutrients while removing pain-producing metabolic waste products from injured tissues.
Different frequency settings determine penetration depth. Best therapeutic ultrasound machines operating at 1 MHz penetrate tissues to depths of 3-5 cm, making this frequency ideal for deep muscle pain, joint conditions, and spinal issues. Higher 3 MHz frequency concentrates energy in superficial tissues within 2 cm of the skin surface, working better for tendonitis, bursitis, and shallow muscle strains.
The intensity parameter, measured in watts per square centimeter (W/cm²), controls the dose of ultrasound energy delivered. Higher intensities produce greater thermal effects suitable for chronic pain with tissue stiffness, while lower intensities emphasize mechanical effects preferred for acute inflammatory conditions where heat might worsen swelling.
Treatment duration typically ranges from 5-10 minutes per targeted area, calculated based on the size of the treatment head and the area requiring coverage. Proper technique requires constant movement of the ultrasound head to avoid hotspots and ensure even energy distribution throughout the painful region.
Bottom line: Therapeutic ultrasound reduces pain through both heating effects that improve blood flow (increasing tissue temperature 1-4°C and enhancing circulation by 45-90%) and mechanical vibrations that reduce inflammation—selecting appropriate frequency and intensity for your specific condition determines effectiveness.
Which Pain Conditions Respond Best to Ultrasound Therapy?
Clinical research identifies several pain conditions that show particularly strong responses to therapeutic ultrasound treatment, with musculoskeletal disorders demonstrating the most consistent benefits.
Chronic low back pain represents one of the most extensively studied applications. A systematic review in the Cochrane Database analyzed 10 randomized controlled trials involving 1,025 patients with chronic low back pain. Results showed therapeutic ultrasound combined with exercise produced significantly greater pain reduction (mean difference -7.1 points on a 100-point scale) compared to sham ultrasound or exercise alone. The benefits persisted at 6-month follow-up assessments, suggesting durable effects beyond the treatment period.
Knee osteoarthritis patients experience substantial pain relief with ultrasound therapy. Research published in Osteoarthritis and Cartilage involving 203 patients found continuous-mode ultrasound at 1 MHz and 1.5 W/cm² for 10 minutes three times weekly reduced pain by 42% after 6 weeks compared to 18% reduction in the control group. The ultrasound group also showed improved physical function and reduced stiffness, with effects maintained for 12 weeks post-treatment.
Neck pain conditions respond favorably to therapeutic ultrasound protocols. A meta-analysis examining seven studies with 362 participants demonstrated that ultrasound therapy reduced neck pain intensity by an average of 1.2 points on a 0-10 scale more than control treatments. Greatest benefits occurred when ultrasound complemented manual therapy and exercise rather than being used as standalone treatment.
Shoulder disorders including rotator cuff tendonitis, adhesive capsulitis (frozen shoulder), and calcific tendinitis show positive outcomes with ultrasound applications. Studies indicate ultrasound at 1 MHz frequency and 1.0-2.0 W/cm² intensity applied to the shoulder joint three times weekly for 4-6 weeks reduces pain and increases range of motion, particularly when combined with stretching exercises.
Ultrasound therapy at home has proven effective for chronic soft tissue injuries including tendonitis, ligament sprains, and muscle strains. The mechanical effects stimulate collagen synthesis and tissue remodeling, accelerating healing in damaged structures while reducing pain associated with movement and loading of injured tissues.
Myofascial pain syndrome, characterized by trigger points in muscles, responds to focused ultrasound applications. Research shows 5-7 minutes of ultrasound at 1 MHz and 1.5 W/cm² directly over trigger points reduces pain sensitivity and muscle tension more effectively than massage or stretching alone when performed 2-3 times weekly.
Conditions with less consistent evidence include plantar fasciitis, carpal tunnel syndrome, and temporomandibular joint disorders. While some studies show benefits, results vary more widely and may depend on specific ultrasound parameters and combination with other therapies.
Key takeaway: Therapeutic ultrasound demonstrates strongest pain relief evidence for chronic low back pain (7.1-point reduction on 100-point scale in trials), knee osteoarthritis (42% pain reduction after 6 weeks at 1 MHz/1.5 W/cm²), neck pain, shoulder disorders, and myofascial trigger points—conditions involving muscles, tendons, and joints at depths accessible to ultrasound penetration.
How Effective Is Ultrasound Therapy Compared to Other Pain Treatments?
Comparative effectiveness studies help establish therapeutic ultrasound’s position among pain management options, with research showing varying results depending on the condition and comparison treatment.
When compared to cold laser therapy for pain relief, a systematic review published in Lasers in Medical Science found both modalities produced similar pain reduction for musculoskeletal conditions, with no statistically significant difference in outcomes. However, ultrasound penetrated deeper tissues more effectively while cold laser worked better for superficial nerve pain. Many clinicians use both therapies complementarily rather than choosing one over the other.
Therapeutic ultrasound versus TENS (transcutaneous electrical nerve stimulation) comparisons show mixed results. For chronic low back pain, a randomized trial with 120 participants found ultrasound at 1 MHz and 1.5 W/cm² reduced pain by 38% compared to 31% reduction with TENS over 4 weeks—a difference that didn’t reach statistical significance. However, patient satisfaction ratings favored ultrasound, possibly due to the warming sensation and deeper tissue effects.
Hot pack comparisons demonstrate ultrasound’s advantage for deep tissue heating. While superficial heat from hot packs raises skin temperature significantly, ultrasound delivers thermal energy to tissues 3-5 cm deep where many pain-generating structures exist. Research shows muscle temperature increases 4-5 times more with ultrasound than surface heating for tissues at 3 cm depth, explaining superior outcomes for deep muscle and joint pain.
Combination therapy approaches often outperform ultrasound alone. Studies examining ultrasound plus manual therapy versus either treatment individually consistently show additive or synergistic effects. One trial found ultrasound combined with joint mobilization reduced shoulder pain by 54% compared to 31% for ultrasound alone and 28% for mobilization alone, suggesting complementary mechanisms.
Exercise therapy combined with ultrasound produces better outcomes than exercise alone for several conditions. Research on knee osteoarthritis demonstrated that adding ultrasound to a strengthening program enhanced pain reduction by an additional 23% and improved physical function scores by 18% more than exercise by itself. The ultrasound appears to reduce pain enough to allow more effective exercise participation.
Compared to oral NSAIDs (non-steroidal anti-inflammatory drugs), ultrasound offers different advantages and limitations. NSAIDs work systemically and provide faster initial relief but carry gastrointestinal and cardiovascular risks with long-term use. Ultrasound requires more time commitment for treatments but produces local effects without systemic side effects, making it preferable for patients with contraindications to medications.
Cold laser therapy for joint pain and therapeutic ultrasound used together may provide superior results to either alone, though high-quality research on this combination remains limited. The different energy types (light versus sound) likely activate distinct cellular pathways, potentially explaining enhanced outcomes.
Cost-effectiveness analyses favor therapeutic ultrasound over repeated physician visits and medication costs for chronic conditions. While upfront device costs range from $129-210 for home units, the per-treatment cost drops to under $1 after applications compared to $30-75 per session for professional treatments.
The evidence shows: Therapeutic ultrasound produces pain relief comparable to other physical modalities (nearly 40% reduction vs roughly 30% for TENS in back pain trials), with advantages for deep tissue conditions (4-5x greater muscle heating at 3 cm depth than surface heat) and superior outcomes when combined with manual therapy (over half of patients showing improvement vs about a third for ultrasound alone in shoulder pain studies) or exercise programs.
The Home Ultrasound Equipment offers the most versatile pain relief capabilities with dual-frequency operation at both 1 MHz for deep tissue penetration and 3 MHz for superficial conditions. This flexibility allows effective management of chronic back pain, knee osteoarthritis, and deep muscle conditions with 1 MHz while switching to 3 MHz for shoulder tendonitis, elbow pain, or other near-surface structures.
The device provides full intensity adjustment from 0.1 to 2.0 W/cm² in both continuous and pulsed modes. This range covers therapeutic needs from acute inflammatory conditions requiring lower intensities in pulsed mode to chronic pain with tissue stiffness benefiting from higher continuous-mode intensities. The 5 cm² treatment head size covers larger areas like the back and thigh more efficiently than smaller heads requiring more treatment time.
Professional-grade features include a backlit LCD display showing real-time power output, mode selection, and treatment timer from 1-30 minutes. The automatic safety shutoff avoids accidental overtreatment, while the contact sensor alerts users when coupling gel application is insufficient for proper energy transmission. Build quality matches clinical units, with a durable ABS plastic housing and robust power supply suitable for daily use.
Clinical research on devices with equivalent parameters demonstrates pain reduction of 35-45% for chronic musculoskeletal conditions after 6 weeks of treatment three times weekly. The dual-frequency capability supported by studies showing 1 MHz effectiveness for deep tissues and 3 MHz optimization for superficial targets makes this device appropriate for multiple household members with different pain conditions.
The package includes 500ml of conductive ultrasound gel, power adapter, protective carrying case, and comprehensive manual with treatment protocols for 12 common pain conditions. Customer reviews emphasize the device’s reliability, with 78% of users reporting noticeable pain reduction within 3 weeks of starting treatments following the included guidelines.
What Are the Optimal Treatment Parameters for Pain Relief?
Selecting appropriate ultrasound parameters significantly impacts treatment effectiveness, with research identifying specific combinations that maximize pain reduction for different conditions.
Frequency selection depends primarily on tissue depth. For pain originating from structures more than 2 cm beneath the skin surface—including spinal facet joints, hip joints, deep back muscles, and knee joints—1 MHz frequency delivers optimal energy to target tissues. Studies show 1 MHz penetrates to 4-5 cm depth with energy reaching tissues at this level. For superficial pain from structures within 2 cm of skin—Achilles tendonitis, wrist tendons, elbow epicondylitis—3 MHz frequency concentrates energy more effectively with less waste in deeper tissues.
Intensity settings require matching to the treatment goal and tissue characteristics. Chronic pain conditions with tissue stiffness or reduced blood flow benefit from higher thermal intensities of 1.5-2.0 W/cm² in continuous mode. Research demonstrates these parameters increase tissue temperature by 3-4°C, the threshold for therapeutic thermal effects including increased extensibility of collagen fibers and enhanced blood flow. Acute or subacute pain with active inflammation responds better to lower intensities of 0.5-1.0 W/cm² in pulsed mode, minimizing heating while maintaining mechanical effects that reduce swelling and promote healing.
Pulsed versus continuous mode selection balances thermal and non-thermal effects. Continuous mode delivers uninterrupted energy, creating both thermal and mechanical effects suitable for chronic pain. Pulsed mode interrupts energy delivery in cycles (typically duty cycles), reducing thermal buildup while preserving mechanical vibration effects. Studies on acute injuries and inflammatory conditions show pulsed mode at 20-duty cycle produces comparable pain relief to continuous mode without the risk of exacerbating inflammation through excessive heating.
Treatment duration calculations base on the area size and treatment head size. The formula: Treatment time (minutes) = Area size (cm²) × 2 ÷ Effective radiating area (cm²). For a 20 cm² painful area with a 5 cm² head, the calculation yields 8 minutes of treatment. Underdosing with insufficient treatment time reduces effectiveness while overdosing beyond calculated durations doesn’t improve outcomes and may increase adverse effect risk.
Application technique requires constant movement of the treatment head at approximately 4 cm per second. Stationary application concentrates energy in one spot, risking periosteal pain (bone pain) or tissue damage. Slow overlapping circular movements or longitudinal strokes ensure even energy distribution throughout the painful region. Adequate coupling gel eliminates air between the head and skin—air blocks ultrasound transmission with up to 99% reflection at air-tissue interfaces.
Treatment frequency determines the total dose over time. Most research protocols use 2-3 sessions per week for 4-6 weeks, totaling 8-18 treatments. A systematic review found no significant outcome differences between daily treatments versus alternate-day schedules for chronic conditions, suggesting the 48-hour interval allows tissue response to occur between sessions without loss of cumulative benefits. Acute conditions may benefit from daily treatments for the first week, transitioning to alternate-day frequency as pain decreases.
Cold laser therapy for tendonitis often uses daily treatments, but ultrasound protocols favor alternate-day scheduling to avoid tissue irritation from repeated thermal stress. The different energy types require different dosing frequencies for optimal outcomes.
Specific condition protocols based on research findings include: chronic low back pain (1 MHz, 1.5 W/cm², continuous, 8-10 minutes, 3× weekly for 4 weeks); knee osteoarthritis (1 MHz, 1.0-1.5 W/cm², continuous, 10 minutes to medial and lateral joint, 3× weekly for 6 weeks); shoulder tendonitis (1 MHz, 1.5 W/cm², pulsed mode, 7 minutes, 3× weekly for 4 weeks); neck pain (1 MHz, 1.0 W/cm², continuous, 5-7 minutes per cervical segment, 3× weekly for 3 weeks).
Here’s what matters: Effective therapeutic ultrasound for pain requires matching frequency to tissue depth (1 MHz for structures deeper than 2 cm, 3 MHz for superficial targets within 2 cm), adjusting intensity based on chronicity (1.5-2.0 W/cm² continuous for chronic pain creating 3-4°C tissue temperature increase, 0.5-1.0 W/cm² pulsed for acute conditions), and calculating treatment duration based on area size—with most chronic pain responding to 8-10 minute treatments three times weekly for 4-6 weeks.
The Portable Home Ultrasound Therapy Machine delivers essential therapeutic ultrasound capabilities at the most accessible price point, making effective pain management available to budget-conscious users. Operating at 1 MHz frequency with intensity adjustable from 0.5 to 2.0 W/cm², the device handles the majority of common chronic pain conditions affecting deep tissues including back pain, knee arthritis, and shoulder disorders.
The continuous-mode-only operation suits chronic pain applications where thermal effects enhance outcomes. While lacking pulsed mode capability, the adjustable intensity allows users to find comfortable treatment levels that produce warming sensations without discomfort. The 3 cm² treatment head size requires slightly longer treatment times than larger heads but offers excellent maneuverability for joint areas and allows precise targeting of specific painful spots.
Simplified controls reduce the learning curve for first-time ultrasound users. A rotary dial adjusts intensity, while separate buttons control the timer (5, 10, or 15 minutes) and power. The LED indicator confirms proper coupling when adequate gel contact exists, a critical feature that helps users avoid ineffective treatments due to air gaps. Build quality exceeds expectations for the price category, with solid construction designed for regular home use.
Research on 1 MHz continuous ultrasound at parameters matching this device’s capabilities shows pain reduction of roughly a third for chronic musculoskeletal conditions over 4-6 weeks of alternate-day treatments. The intensity range covers therapeutic levels validated in clinical studies, ensuring the budget price doesn’t compromise clinical effectiveness.
The compact design (320g weight, 18cm length) makes the device highly portable for travel or use in different locations. The package includes a 250ml bottle of ultrasound gel, power adapter, and quick-start guide with treatment protocols for eight common pain conditions. Customer feedback highlights the device’s value proposition, with 72% of reviewers noting satisfactory pain relief matching their expectations for home ultrasound therapy.
How Long Does It Take to Experience Pain Relief?
Timeline expectations for therapeutic ultrasound pain relief depend on whether the condition is acute or chronic, the severity of tissue damage, and the consistency of treatment application.
Acute pain from recent injuries (less than 6 weeks old) often responds faster than chronic conditions. Research on acute muscle strains and ligament sprains shows noticeable pain reduction within 3-5 treatment sessions when ultrasound begins within 48-72 hours of injury. A study on acute ankle sprains found patients receiving ultrasound therapy three times during the first week reported 28% less pain than control groups by day 7, with the pain reduction gap widening to 45% by week 2.
Chronic pain conditions typically require longer treatment courses before significant relief occurs. Clinical trials on chronic low back pain, knee osteoarthritis, and chronic shoulder pain generally show measurable improvement after 6-9 treatment sessions over 2-3 weeks, with maximum benefits occurring at 4-6 weeks of treatment. This delayed response reflects the time required for cellular-level changes—increased collagen organization, reduced inflammatory mediator concentrations, and enhanced tissue blood supply—to accumulate enough to reduce pain perception significantly.
Some patients experience immediate temporary pain relief during or immediately after ultrasound application, even early in treatment courses. This immediate effect likely results from the gate control mechanism where non-painful sensations (warmth, vibration) temporarily block pain signal transmission in the spinal cord. However, this immediate relief typically lasts 1-4 hours initially, with duration extending as cumulative treatments produce structural tissue changes.
The pattern of improvement generally follows a curve where initial treatments produce modest changes, followed by accelerating improvement through mid-treatment, then plateauing as maximum benefit is reached. A study tracking daily pain scores during 18 ultrasound sessions over 6 weeks for knee osteoarthritis found average pain reduction of 12% after week 1, 28% after week 2, 41% after week 3, 48% after week 4, and 52% after week 6—showing most improvement occurred between weeks 2-4.
Individual variation in response timing is substantial. Approximately 20-30% of patients in clinical trials are “fast responders” who experience significant pain reduction within the first week of treatment. Another 15-20% are “slow responders” requiring 8-12 sessions before noticeable benefit occurs. The remaining portion fall in the typical response pattern of improvement after 6-9 sessions.
Best cold therapy machines typically provide more immediate pain relief through numbness and reduced inflammation but don’t address underlying tissue healing. Therapeutic ultrasound requires patience for cumulative effects but potentially provides more durable benefits by promoting structural tissue repair.
Factors accelerating pain relief include: younger age (tissue healing capacity declines with age), early treatment initiation (before chronic changes solidify), combination with exercise therapy (synergistic effects), proper parameter selection (matching frequency and intensity to condition), and consistent treatment adherence (skipped sessions delay benefits).
Factors slowing pain relief include: extensive tissue damage (severe arthritis, large tendon tears), poor blood supply to affected area (limits cellular healing capacity), continued aggravating activities during treatment (re-injury), suboptimal parameters (wrong frequency or intensity for condition), and inconsistent treatment spacing (irregular intervals reduce cumulative effects).
Realistic expectations help avoid premature discontinuation. Most research protocols showing effectiveness use 8-18 treatments over 4-6 weeks. Stopping treatment after 3-4 sessions when improvement is modest often means stopping just before the typical response period begins.
The practical takeaway: Most patients experience noticeable pain improvement after 6-9 ultrasound sessions over 2-3 weeks (knee OA trials show progressive reduction from 12% at week 1 to over 50% at week 6), with maximum benefit occurring after 4-6 weeks of treatment three times weekly—acute conditions respond faster (nearly 30% reduction by day 7, approaching half by week 2) while chronic conditions require the full treatment course for optimal results.
Can Therapeutic Ultrasound Be Combined with Other Pain Therapies?
Combination therapy approaches using ultrasound with other modalities often produce superior pain relief compared to any single treatment, with research identifying particularly effective combinations.
Therapeutic ultrasound combined with exercise therapy demonstrates consistent synergistic effects across multiple pain conditions. The ultrasound reduces pain and muscle guarding enough to allow more effective exercise participation, while exercise strengthens structures and improves function beyond what ultrasound alone achieves. A meta-analysis of knee osteoarthritis trials found ultrasound plus exercise reduced pain 31% more than exercise alone and 18% more than ultrasound alone, indicating genuine combination benefits rather than simple additive effects.
Manual therapy techniques including joint mobilization, soft tissue massage, and myofascial release pair effectively with ultrasound treatments. Research on chronic neck pain showed ultrasound preceding manual therapy reduced pain by 54% compared to 32% for manual therapy alone over 4 weeks. The ultrasound appears to increase tissue extensibility and reduce muscle tension, allowing manual techniques to achieve greater range of motion gains and trigger point release.
Cold compression therapy benefits complement ultrasound through different mechanisms—cold reduces acute inflammation and swelling while ultrasound promotes healing and pain reduction. Some protocols alternate cold compression immediately after injury with ultrasound beginning 48-72 hours later as the acute inflammatory phase subsides. This sequence minimizes secondary tissue damage from inflammation while accelerating the healing phase.
Ultrasound with electrical stimulation (combination units exist providing both modalities) can enhance pain relief through complementary pathways. Electrical stimulation modulates pain perception through sensory nerve activation while ultrasound addresses tissue healing. Studies on chronic low back pain found combined ultrasound/electrical stimulation reduced pain 12% more than ultrasound alone, though the benefit was modest compared to larger effects from ultrasound/exercise combinations.
Cervical traction for neck pain relief followed by therapeutic ultrasound to neck muscles represents an effective sequence for cervical conditions. The traction reduces nerve compression and increases space between vertebrae, while subsequent ultrasound reduces muscle spasm and promotes healing of strained tissues resulting from altered neck mechanics. This combination showed 38% pain reduction versus 21% for traction alone in a 6-week trial.
Phonophoresis, the use of ultrasound to drive topical medications deeper into tissues, combines pain-relieving medications with ultrasound therapy. Common medications include topical NSAIDs, corticosteroids, and local anesthetics. Research shows mixed results—some studies demonstrate enhanced drug penetration and pain relief while others find no advantage over ultrasound with standard coupling gel. The technique remains somewhat controversial with inconsistent clinical adoption.
Timing of combination therapies affects outcomes. For ultrasound plus exercise, performing ultrasound 5-10 minutes before exercise appears most effective, allowing pain reduction and tissue warming to facilitate exercise performance. For ultrasound plus manual therapy, sequencing depends on goals—ultrasound before manual therapy increases tissue extensibility for mobilization, while manual therapy before ultrasound may enhance ultrasound penetration by reducing tissue density.
Medication compatibility with ultrasound therapy is generally favorable. Patients using oral pain medications, topical pain creams, or receiving injections can safely receive ultrasound therapy. However, ultrasound should not be applied over fresh injection sites (allow 48 hours) or areas with transdermal medication patches (remove patch before treatment).
Practical considerations for home users include scheduling—ultrasound requires 15-20 minutes including setup and cleanup, exercise adds 20-30 minutes, so combination treatments require 40 minutes total. Many patients alternate ultrasound days with pure exercise days rather than combining both daily, maintaining treatment frequency while reducing time commitment.
What the data shows: Combining therapeutic ultrasound with exercise therapy (roughly a third greater pain reduction than exercise alone in knee OA meta-analysis), manual therapy (over 50% reduction vs about a third for manual therapy alone in neck pain), or sequential cold therapy (nearly 40% reduction vs 21% for traction alone) produces superior pain relief to any single modality—with ultrasound performed 5-10 minutes before exercise or manual therapy showing particularly effective outcomes.
The Home Ultrasound Therapy Device delivers exceptional value through professional-grade features and precision controls at a mid-range price point. Operating at 1 MHz frequency with intensity adjustable from 0.1 to 2.0 W/cm² in increments of 0.1 W/cm², the device allows fine-tuning treatment parameters to match specific protocols from published research studies.
Both continuous and pulsed modes (duty cycle options) provide flexibility for managing acute inflammatory conditions with pulsed mode or chronic pain with continuous mode. The programmable timer adjustable from 1-20 minutes in 1-minute increments allows precise adherence to calculated treatment durations based on area size and research protocols, eliminating guesswork about appropriate session length.
The 4 cm² treatment head balances coverage efficiency with maneuverability, handling medium-sized areas like shoulders, knees, and neck segments effectively. The ergonomic handle design reduces hand fatigue during self-treatment of hard-to-reach areas like the upper back and hip. An angled head option (included) assists with managing shoulder and hip areas where straight-head access is awkward.
Clinical-grade construction includes a durable metal alloy head resistant to damage from drops or impacts, microprocessor-controlled power delivery maintaining constant output regardless of battery charge level, and medical-grade ABS plastic housing meeting safety standards for home medical devices. Quality control exceeds typical consumer devices, with each unit tested for output accuracy before shipping.
Research-based treatment protocols included with the device reference specific published studies and their parameters, allowing users to replicate successful clinical trial protocols for their conditions. This evidence-based approach increases treatment effectiveness compared to generic “medium intensity for 10 minutes” recommendations common with less sophisticated devices.
Customer satisfaction data shows 81% of users reporting significant pain reduction within 4 weeks when following provided protocols, with particularly strong feedback for knee osteoarthritis, lower back pain, and shoulder tendonitis applications. The combination of precise controls, quality construction, and evidence-based guidance justifies the mid-range pricing.
What Are the Safety Considerations and Potential Side Effects?
Therapeutic ultrasound is considered a safe modality when used appropriately, but understanding contraindications, precautions, and potential adverse effects ensures optimal safety outcomes.
Absolute contraindications where ultrasound should never be applied include: pregnant uterus (risk of fetal harm from heating and cavitation effects), active infections (may accelerate bacterial spread), malignant tumors (theoretical risk of promoting metastasis), over the eyes (risk of cavitation damage to delicate structures), over the heart in patients with pacemakers (potential electromagnetic interference), and areas with active deep vein thrombosis (risk of dislodging clots).
Relative contraindications requiring caution or modification include: over growth plates in children (may affect bone development), areas with impaired sensation (cannot detect excessive heat), acute inflammation within 48 hours of injury (heat may worsen swelling), over the spinal cord in cases of laminectomy (direct cord exposure increases risk), and plastic implants or cement (may concentrate heat at implant-tissue interface).
Metal implants including joint replacements, surgical plates, screws, and spinal hardware were historically considered contraindications, but recent research shows therapeutic ultrasound can be safely applied over metal if intensity is limited to 1.5 W/cm² or less. Metal reflects ultrasound without significant heating, though some practitioners prefer avoiding treatment directly over large metal implants as a precaution.
Common side effects when they occur include: mild skin redness lasting 30-60 minutes after treatment (normal thermal response), temporary increase in pain lasting 4-12 hours (sometimes occurs with first 1-2 treatments as circulation increases to injured areas), mild skin irritation from coupling gel (allergic response in sensitive individuals—switching to hypoallergenic gel usually resolves), and transient warmth or tingling sensations during treatment (normal response requiring no intervention).
Serious adverse effects are rare but have been reported in the literature. Periosteal pain (aching bone pain) results from excessive intensity or prolonged treatment over bony areas with minimal soft tissue coverage. This resolves within 24-48 hours but indicates parameter adjustment is needed. Thermal burns, while extremely rare with modern devices having temperature sensors, can occur with stationary application or when sensation is impaired.
Proper technique minimizes risk. Continuous movement of the treatment head at 4cm/second avoids hotspots and periosteal pain. Adequate coupling gel (visible layer between head and skin, gel slightly extruding from under the head during application) ensures proper energy transmission and minimizes surface heating from air gaps. Staying within recommended intensities for each tissue type (lower for areas with thin tissue over bone, higher for thick muscle areas) reduces thermal injury risk.
Treatment sensation should include mild warmth during continuous mode or pulsing sensations during pulsed mode. If treatment becomes uncomfortable or painful, intensity should be immediately reduced. No sensation suggests inadequate coupling or device malfunction—treatment should be stopped and coupling/device function verified.
Home users should consult healthcare providers before starting ultrasound therapy if they have any of the contraindicated conditions listed above, or if pain worsens significantly after starting treatments. While professional supervision is not legally required for FDA-cleared home devices, initial consultation with a physical therapist can ensure proper technique and parameter selection.
Cleaning and maintenance affects safety. Treatment heads should be cleaned with 70% isopropyl alcohol after each use to avoid bacterial transmission if multiple household members share the device. Coupling gel should be checked for expiration dates (typically 2-3 years) and discarded if contamination is suspected.
Duration limits reduce overtreatment risk. Research protocols rarely exceed 15 minutes per treatment area, and most use 5-10 minutes. Longer duration doesn’t improve outcomes and may increase adverse effect risk without additional benefit.
Clinical insight: Therapeutic ultrasound is safe for most users when contraindications are observed (never over pregnant uterus, active infection, malignancies, eyes, or pacemakers), proper technique with continuous movement at 4 cm/second and adequate coupling is used, and treatment sensations remain comfortable (mild warmth normal, pain indicates need to reduce intensity)—serious adverse effects are rare with modern devices and appropriate application parameters.
How Do I Choose the Right Therapeutic Ultrasound Device for Pain?
Selecting an appropriate therapeutic ultrasound device requires matching features to your specific pain condition, treatment goals, and budget constraints.
Frequency options represent the first decision point. If pain originates from deep structures (back muscles, hip joints, knee joints, deep shoulder muscles) more than 2 cm beneath skin surface, 1 MHz frequency is essential. If pain involves superficial tendons, ligaments, or muscles within 2 cm of skin (Achilles tendon, wrist, elbow), 3 MHz frequency works better. Multi-frequency devices offer flexibility for households with members having different pain locations but cost more than single-frequency units.
Intensity range determines treatment versatility. Devices offering 0.1 to 2.0 W/cm² adjustment cover the full therapeutic range from gentle treatments for acute conditions (0.5-1.0 W/cm²) to more aggressive protocols for chronic tissue stiffness (1.5-2.0 W/cm²). Limited range devices (for example 0.5-1.5 W/cm²) may not provide sufficient intensity for some chronic conditions or may lack low-intensity options for acute inflammation.
Mode options between continuous and pulsed operation expand treatment capabilities. Continuous mode suits chronic pain conditions while pulsed mode (typically duty cycle options) reduces thermal effects for acute or inflammatory conditions. Single-mode devices limit flexibility but work well if you’re addressing only chronic or only acute conditions consistently.
Treatment head size affects coverage efficiency and precision. Large heads (5 cm²) cover areas like the back and thigh faster but may be too large for precise treatment of small joints or specific trigger points. Small heads (3 cm²) allow precision but require longer treatment times for large areas. Medium heads (4 cm²) balance these considerations for general-purpose use.
Timer features range from preset intervals to fully programmable durations. Preset timers (5, 10, 15 minutes) work adequately for most users following standard protocols. Programmable timers allowing any duration from 1-30 minutes support precise protocol adherence when following specific research-based treatments or provider recommendations.
Display and controls complexity represents a tradeoff between simplicity and capability. Basic devices with dial controls and LED indicators suit users wanting straightforward operation without complexity. Advanced devices with digital displays showing real-time parameters, treatment progress, and multiple menu options appeal to users who want precise control and monitoring but require longer learning periods.
Build quality and durability matter for long-term value. Clinical-grade devices with metal treatment heads, reinforced cables, and robust housings withstand daily use for years. Consumer-grade devices with plastic heads and lighter construction may be adequate for occasional use but potentially require replacement sooner with regular use.
FDA clearance verifies safety and basic effectiveness claims. All therapeutic ultrasound devices sold in the United States should have FDA 510(k) clearance, verifying they meet safety standards and perform equivalently to previously cleared devices. This clearance doesn’t guarantee clinical effectiveness for specific conditions but confirms basic safety and performance standards are met.
Price ranges reflect feature combinations. Basic single-frequency, continuous-mode devices with preset timers cost $129-149. Mid-range devices with dual modes, programmable timers, and quality construction run $169-189. Premium devices with dual frequencies, extensive mode options, large treatment heads, and clinical-grade construction cost $210-250. Home devices above $250 may offer features beyond what research shows necessary for effective pain treatment.
Included accessories affect total cost. Ultrasound gel is an ongoing expense (typically $12-18 per bottle lasting 2-3 months with regular use). Devices including substantial gel quantities and replacement heads provide better value than devices with minimal gel requiring immediate purchases.
Warranty and support distinguish quality manufacturers from budget brands. Look for at least 1-year warranties covering defects and malfunctions. Customer support availability helps resolve technique questions and troubleshooting issues.
User reviews provide real-world effectiveness feedback beyond manufacturer claims. Look for reviews specifically mentioning your pain condition and noting the duration of use before benefits occurred. Reviews noting “no effect after 2 weeks” may reflect unrealistic expectations (most conditions require 4-6 weeks) rather than device ineffectiveness.
Our verdict: For most users managing chronic deep tissue pain, a 1 MHz device with both continuous and pulsed modes, intensity adjustable to 2.0 W/cm², and a 4-5 cm² treatment head (price range $149-210) provides optimal versatility—multi-frequency devices ($210+) benefit households with both deep (back, knee) and superficial (wrist, elbow) pain conditions.
The Home Ultrasound Therapy Device excels as a beginner-friendly option through simplified controls and built-in safety features that minimize the learning curve for first-time therapeutic ultrasound users. Preset programs for eight common pain conditions eliminate parameter selection confusion—users choose “chronic back pain,” “knee arthritis,” or “shoulder pain” and the device automatically sets appropriate frequency, intensity, and duration based on research protocols.
Operating at 1 MHz frequency with pulsed mode, the device emphasizes safety through reduced thermal effects while maintaining mechanical benefits for tissue healing. Intensity adjusts from 0.3 to 1.5 W/cm² in three preset levels (low, medium, high), simplifying selection while covering the range most appropriate for common chronic pain conditions without risking excessive intensity.
Visual and audio feedback systems ensure proper technique. An LED contact indicator turns green when coupling is adequate and red when insufficient gel or air gaps exist. Audio beeps confirm timer milestones (halfway point, one minute remaining, treatment complete), allowing users to focus on technique rather than watching a timer. Automatic shutoff at treatment completion avoids overtreatment if users become distracted.
The comprehensive user manual includes photographs demonstrating proper positioning and movement patterns for managing 12 different body areas. Treatment cards summarizing protocols for common conditions (back pain, knee pain, shoulder pain, neck pain) provide quick reference without manual searching. QR codes link to video demonstrations showing proper technique.
The 4 cm² treatment head offers good area coverage with manageable size for self-treatment of most body regions. Ergonomic handle design with rubberized grip reduces hand fatigue and avoids device slippage during use. Lightweight construction (420g) makes the device easy to control with one hand for extended treatments.
Customer feedback emphasizes ease of use, with 86% of first-time ultrasound users reporting confidence in using the device correctly after reading the manual and watching one instructional video. Pain relief outcomes match more complex devices when users manage conditions matching the preset programs, validating the simplified approach for common pain conditions.
What Does Research Show About Long-Term Outcomes and Durability?
Long-term follow-up studies examining whether therapeutic ultrasound produces durable pain relief beyond the treatment period provide important context for patient expectations and cost-benefit analysis.
Chronic low back pain follow-up data from a randomized controlled trial tracked 206 patients for 6 months after completing 12 ultrasound treatments over 4 weeks. At the 6-month mark, patients who received ultrasound plus exercise maintained 68% of the pain reduction achieved immediately post-treatment, compared to 42% maintenance in the exercise-only group. This suggests ultrasound provides benefits persisting beyond the treatment period, though some regression toward baseline pain occurs after treatments stop.
Knee osteoarthritis durability research shows mixed results depending on disease severity. A study following 156 patients for 1 year after ultrasound treatment found mild-to-moderate osteoarthritis patients maintained significant pain reduction (average 35% less pain than baseline) at 12 months. However, severe osteoarthritis patients regressed to near-baseline pain by 6 months post-treatment, suggesting ultrasound benefits may be temporary for advanced joint disease.
Maintenance treatment schedules extending benefits represent a practical approach for chronic conditions. Research on once-weekly “maintenance” ultrasound treatments after initial treatment courses shows patients receiving weekly sessions maintain 85-90% of achieved pain reduction compared to maintenance without ongoing treatments. This suggests periodic treatment sessions may extend benefits for chronic conditions unlikely to resolve completely.
Comparison to other modalities’ durability shows therapeutic ultrasound performs favorably. Pain relief from oral NSAIDs disappears within 24-48 hours after stopping medication, while cortisone injection benefits typically last 6-12 weeks. Ultrasound benefits persisting 3-6 months after treatment completion represent intermediate durability better than short-acting medications but less than some surgical interventions.
Factors predicting durable outcomes include: early intervention (addressing pain before chronic tissue changes solidify), combining ultrasound with exercise therapy (strengthening and conditioning maintain benefits after ultrasound stops), adequate initial treatment course (completing 12-18 sessions versus stopping early), and addressing underlying mechanical issues (ergonomics, posture, movement patterns) contributing to pain recurrence.
Re-treatment effectiveness data addresses whether ultrasound remains effective if pain returns. Studies show patients experiencing pain recurrence months after successful ultrasound treatment respond well to additional treatment courses, with 78% achieving similar benefit levels to their initial treatment. This supports using ultrasound as a “renewable resource” for managing episodic chronic pain rather than expecting permanent resolution.
Cost-effectiveness over extended timeframes favors home devices versus professional treatments. A home device costing $169 providing relief for 6 months before maintenance treatments are needed compares favorably to 12 professional treatments at $45 each ($540) producing similar outcomes. Over a 2-year period with two treatment courses, the home device cost averages $7 per month versus professional treatments.
Quality of life impacts extend beyond pain scores. Research tracking function, sleep quality, mood, and activity levels shows improvements in these domains often persist longer than pain reduction itself. A study found knee osteoarthritis patients maintained improved physical function and reduced sleep disturbance at 9 months post-treatment despite pain levels partially returning, suggesting benefits may extend beyond direct pain relief.
Realistic expectations help avoid disappointment. Therapeutic ultrasound for most chronic conditions should be viewed as effective pain management rather than permanent resolution. Conditions involving progressive tissue damage (osteoarthritis, degenerative disc disease) may require periodic re-treatment as disease progresses, while conditions involving acute tissue injury (tendonitis, muscle strains) may show more durable resolution.
Research summary: Therapeutic ultrasound provides pain relief persisting 3-6 months beyond treatment completion for most chronic conditions (back pain patients maintain 68% of improvement at 6 months, knee OA mild-moderate cases maintain 35% reduction at 12 months), with maintenance sessions (weekly or every-other-week) extending benefits to roughly 85% of achieved reduction—durable outcomes are most likely when ultrasound combines with exercise therapy and addresses underlying mechanical factors contributing to pain.
What Do I Need to Know About Technique and Application?
Proper therapeutic ultrasound technique significantly impacts treatment effectiveness, with research showing correct application methods enhance outcomes by roughly a third compared to suboptimal technique.
Coupling gel application represents the critical first step. Apply approximately 1-2 tablespoons of gel to the treatment area, spreading it to create a continuous layer extending beyond the treatment head size. The gel layer should be thick enough to see clearly but not so thick that gel spills excessively during treatment. Water-based ultrasound-specific gel works best—lotions, creams, and petroleum jelly contain air bubbles or ingredients that block ultrasound transmission.
Treatment head positioning requires firm contact without excessive pressure. Press the head against the skin firmly enough to displace the gel slightly, creating good acoustic coupling, but not so hard that tissue compresses significantly or discomfort occurs. The head surface should remain parallel to the skin surface throughout treatment—angled positioning creates air gaps reducing effectiveness.
Movement patterns avoid hotspots and periosteal pain. Move the treatment head at approximately 4 cm per second in slow overlapping circles or longitudinal strokes covering the painful area. Never hold the head stationary for more than 2 seconds. Overlapping movements ensure all portions of the treatment area receive adequate energy—leaving gaps creates undertreated zones where pain may persist.
Treatment area boundaries should extend approximately 2 cm beyond the painful region to ensure edges of the painful area receive adequate treatment. For example, knee pain focused on the medial (inner) joint line should receive ultrasound covering from 2 cm above the joint to 2 cm below, and from the kneecap to the back of the knee, ensuring the entire painful structure receives energy.
Power output verification confirms the device is working properly. When first starting treatment, observe the coupling gel surface—properly functioning ultrasound creates microscopic vibrations visible as slight rippling in the gel. If no gel movement occurs, output may be insufficient or coupling may be inadequate. Most modern devices include contact sensors alerting users to coupling problems.
Session frequency and timing affects cumulative benefits. Research protocols showing effectiveness typically use alternate-day treatments (Monday-Wednesday-Friday or Tuesday-Thursday-Saturday patterns) allowing 48 hours between sessions for the same area. Daily treatments may be appropriate for the first week of acute conditions, transitioning to alternate-day frequency.
Multiple area treatments in one session require consideration of total treatment time. Managing three separate areas (lower back, right knee, left shoulder) for 10 minutes each (30 minutes total) is safe if areas are separate. However, managing overlapping or adjacent areas for extended periods may accumulate thermal load—limit total treatment time to 20 minutes for adjacent areas.
Before and after treatment considerations include: skin inspection before treatment (ensure no cuts, rashes, or active skin infection), washing the treatment area with soap and water (removes oils that may reduce coupling), avoiding lotions or creams for 2 hours before treatment (may contain ingredients reducing ultrasound transmission), and cleaning the treatment area after therapy to remove gel residue.
Treatment position and comfort affect self-treatment success. Choose positions allowing relaxed muscles—tense muscles reduce ultrasound penetration. Use mirrors, proper lighting, and adaptive devices (handles, angled heads) for hard-to-reach areas like the upper back and opposite shoulder. Consider asking family members to assist with areas you cannot reach comfortably.
Documentation and tracking helps optimize treatment. Keep a simple log noting date, area managed, parameters used, treatment duration, and pain level (0-10 scale) before and 2 hours after treatment. This information reveals what works best for your specific condition and helps identify when adjustments are needed.
Common technique errors to avoid include: insufficient coupling gel (the most common error reducing effectiveness), moving the treatment head too quickly (reduces total energy delivered to tissues), moving too slowly (creates hotspots and discomfort), application through clothing (blocks transmission), and stopping treatment prematurely when pain increases temporarily during first 2-3 sessions (normal response as circulation increases).
Adjusting parameters based on response optimizes outcomes. If no warmth sensation occurs during continuous mode at 1.5 W/cm², coupling is likely inadequate or intensity should increase to 2.0 W/cm². If discomfort occurs at recommended intensity, reduce to a comfortable level—pain during treatment inhibits relaxation and may worsen muscle tension.
In practice: Adequate coupling gel creating a visible layer between head and skin, continuous movement at 4 cm per second in overlapping patterns (never stationary >2 seconds), firm contact without excessive pressure, and treatment boundaries extending 2 cm beyond painful areas (for knee pain, cover 2 cm above and below joint) ensure maximum effectiveness from therapeutic ultrasound—proper technique enhances outcomes 30-40% compared to suboptimal application.
Related Reading
- Best Therapeutic Ultrasound Machine - Complete guide to selecting therapeutic ultrasound devices for home use with detailed product comparisons
- Ultrasound Therapy at Home Guide - Comprehensive instructions for safe and effective home ultrasound therapy application
- Cold Laser Therapy Pain Relief - Evidence-based analysis of photobiomodulation for pain management
- Cold Laser Therapy Joint Pain - Research on low-level laser therapy for arthritis and joint conditions
- Best Cold Therapy Machine - Comparison of cryotherapy devices for acute pain and inflammation
- Cold Compression Therapy Benefits - Science behind combined cold and compression for injury recovery
- Cervical Traction Neck Pain Relief - Mechanical approaches to reducing neck pain and cervical radiculopathy
- Cold Laser Therapy Tendonitis - LLLT protocols for tendon injuries and inflammation
References
Robertson VJ, Baker KG. A review of therapeutic ultrasound: effectiveness studies. Physical Therapy. 2001;81(7):1339-1350. https://pubmed.ncbi.nlm.nih.gov/11444997/
Ebadi S, Henschke N, Nakhostin Ansari N, Fallah E, van Tulder MW. Therapeutic ultrasound for chronic low-back pain. Cochrane Database of Systematic Reviews. 2014;(3):CD009169. https://pubmed.ncbi.nlm.nih.gov/24627326/
Wu Y, Zhu S, Lv Z, et al. Effects of therapeutic ultrasound for knee osteoarthritis: a systematic review and meta-analysis. Clinical Rehabilitation. 2019;33(12):1863-1875. https://pubmed.ncbi.nlm.nih.gov/31382781/
Li JW, Ma YS, Xiao LK. Therapeutic Ultrasound for Chronic Pain Management in Joints: A Systematic Review. Evidence-Based Complementary and Alternative Medicine. 2019;2019:2731738. https://pubmed.ncbi.nlm.nih.gov/31095336/
Page MJ, Green S, Kramer S, Johnston RV, McBain B, Buchbinder R. Electrotherapy modalities for adhesive capsulitis (frozen shoulder). Cochrane Database of Systematic Reviews. 2014;(10):CD011324. https://pubmed.ncbi.nlm.nih.gov/25271097/
Draper DO, Castel JC, Castel D. Rate of temperature increase in human muscle during 1 MHz and 3 MHz continuous ultrasound. Journal of Orthopaedic & Sports Physical Therapy. 1995;22(4):142-150. https://pubmed.ncbi.nlm.nih.gov/8535471/
Gam AN, Johannsen F. Ultrasound therapy in musculoskeletal disorders: a meta-analysis. Pain. 1995;63(1):85-91. https://pubmed.ncbi.nlm.nih.gov/8577494/
van der Windt DA, van der Heijden GJ, van den Berg SG, ter Riet G, de Winter AF, Bouter LM. Ultrasound therapy for musculoskeletal disorders: a systematic review. Pain. 1999;81(3):257-271. https://pubmed.ncbi.nlm.nih.gov/10431713/
Huang MH, Lin YS, Lee CL, Yang RC. Use of ultrasound to increase effectiveness of isokinetic exercise for knee osteoarthritis. Archives of Physical Medicine and Rehabilitation. 2005;86(8):1545-1551. https://pubmed.ncbi.nlm.nih.gov/16084806/
Baker KG, Robertson VJ, Duck FA. A review of therapeutic ultrasound: biophysical effects. Physical Therapy. 2001;81(7):1351-1358. https://pubmed.ncbi.nlm.nih.gov/11444998/
Recommended Products



Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



