Best Therapeutic Ultrasound Machine: Home-Use Devices for Pain Relief and Tissue Healing
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Chronic pain from tendonitis, muscle strains, and joint inflammation affects daily function and quality of life, yet many individuals lack convenient access to professional physical therapy services. The Home Ultrasound Equipment 1 & 3 MHz Dual Frequency device delivers clinical-grade therapeutic ultrasound with both penetration depths—1 MHz for deep muscle and joint therapy down to 5 cm, and 3 MHz for superficial tendon and ligament application within 2 cm—at approximately $210. Published research demonstrates that dual-frequency capability provides versatility matching professional clinic equipment, with systematic reviews confirming ultrasound therapy’s effectiveness for reducing pain and accelerating tissue healing when applied according to evidence-based protocols. The Portable Home Ultrasound Therapy Machine offers budget-friendly access to therapeutic ultrasound at $129 with essential features for consistent pain management. Here’s what the published research shows about selecting and using therapeutic ultrasound machines for home-based rehabilitation and pain relief.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
What the Research Shows About Therapeutic Ultrasound for Pain Relief
Therapeutic ultrasound represents one of the most extensively studied physical therapy modalities, with over five decades of clinical research establishing its mechanisms and applications for musculoskeletal conditions. Unlike diagnostic ultrasound imaging, therapeutic ultrasound applies focused acoustic energy at specific frequencies and intensities to generate biological effects that support tissue healing and pain reduction.
A comprehensive systematic review published in the Journal of Physical Therapy Science analyzed 23 randomized controlled trials examining ultrasound therapy for various musculoskeletal conditions, finding significant improvements in pain scores and functional outcomes across multiple diagnostic categories.1 The research identified optimal parameters varying by tissue depth and condition chronicity, with deeper structures responding better to 1 MHz frequency and superficial tissues showing enhanced response to 3 MHz applications.
Research into ultrasound’s thermal effects demonstrates that continuous-mode ultrasound at therapeutic intensities (1.5-2.5 W/cm²) elevates tissue temperature by 4-5°C at target depths, promoting increased blood flow, enhanced metabolic activity, and improved tissue extensibility.2 These thermal effects prove particularly beneficial for chronic conditions where tissue stiffness and restricted blood flow contribute to persistent symptoms.
Conversely, pulsed ultrasound modes generate primarily non-thermal mechanical effects through acoustic streaming and cavitation phenomena that stimulate cellular processes without significant temperature elevation. A meta-analysis in Physical Therapy Reviews found pulsed ultrasound particularly effective for acute inflammatory conditions and post-surgical healing, where excessive heat application might exacerbate inflammation.3
The acoustic energy delivered during therapeutic ultrasound creates mechanical pressure waves that propagate through tissues, producing both direct cellular effects and indirect responses through enhanced circulation and modified nerve activity. Research published in Ultrasound in Medicine & Biology documented ultrasound-induced increases in fibroblast activity, collagen synthesis, and protein production—key processes in soft tissue repair and regeneration.4
Clinical studies examining therapeutic ultrasound for specific conditions provide evidence-based guidance for home users. A 2019 systematic review of ultrasound therapy for rotator cuff tendonitis identified significant pain reduction and functional improvement when ultrasound was applied at 1.0-1.5 W/cm² for 8-10 minutes per session over 4-6 week periods.5 The review emphasized the importance of combining ultrasound with therapeutic exercise for optimal outcomes.
For knee osteoarthritis, research demonstrates consistent benefits from therapeutic ultrasound application. A randomized controlled trial in Clinical Rehabilitation found that participants receiving therapeutic ultrasound combined with exercise therapy experienced greater pain reduction and functional improvement compared to exercise alone, with effects maintained at 3-month follow-up.6
Lateral epicondylitis (tennis elbow) has been extensively studied as a target for ultrasound therapy. Research published in The American Journal of Sports Medicine showed that low-intensity pulsed ultrasound applied to lateral epicondyle tendon insertions resulted in significant pain reduction and grip strength improvements compared to sham application.7
The depth of ultrasound penetration depends directly on frequency selection, with lower frequencies enabling deeper tissue access. Studies measuring ultrasound absorption in biological tissues confirm that 1 MHz ultrasound effectively penetrates 4-5 cm below the skin surface, making it appropriate for hip, spine, and large joint applications, while 3 MHz ultrasound optimally reaches tissues within 2 cm depth, including tendons, superficial ligaments, and muscle-tendon junctions.8
Home-use therapeutic ultrasound devices have undergone validation studies comparing their effectiveness to clinic-based professional equipment. Research in Physiotherapy Theory and Practice found that portable ultrasound units with proper frequency and intensity controls produced therapeutic effects comparable to larger clinical devices when operated according to established protocols.9 This evidence supports the viability of home-based ultrasound therapy for appropriate conditions and properly trained users.
How Does Ultrasound Frequency Affect Treatment Depth?
The fundamental physics of ultrasound therapy dictates that frequency selection determines depth and tissue targeting precision. This relationship between frequency and penetration depth represents one of the most critical factors in therapeutic effectiveness and appropriate device selection for home use.
Research published in Ultrasound in Medicine & Biology demonstrates that ultrasound energy absorption increases with frequency, resulting in shallower penetration at higher frequencies.10 The 1 MHz frequency commonly available in therapeutic devices penetrates approximately 2-5 cm into soft tissues, making it appropriate for addressing deep muscles, large joints, and spinal structures where target tissues lie beneath substantial overlying tissue layers.
The 3 MHz frequency option found in dual-frequency devices concentrates therapeutic effects in the superficial 1-2 cm of tissue depth, proving ideal for tendon insertions, ligament injuries, bursal inflammation, and other conditions affecting structures close to the skin surface. Clinical studies confirm that applying 3 MHz ultrasound to deeper targets wastes therapeutic energy in superficial tissues without adequate penetration to intended areas.11
For shoulder pathologies, research supports different frequency selections based on specific diagnostic targets. Supraspinatus tendon tears and rotator cuff inflammation respond optimally to 1 MHz frequency due to the tendon’s depth beneath the deltoid muscle and overlying tissues. Conversely, subacromial bursal inflammation and superficial biceps tendonitis show better response to 3 MHz applications that concentrate energy at appropriate depths.12
Knee joint applications similarly benefit from frequency-specific targeting. Patellar tendonitis affecting the superficial patellar tendon insertion responds well to 3 MHz ultrasound, while osteoarthritis affecting deeper joint structures and surrounding muscle spasm benefits from 1 MHz penetration to subchondral bone and joint capsule tissues.
The thermal effects generated by continuous-mode ultrasound vary with both frequency and tissue composition. Research measuring temperature elevation during therapeutic ultrasound shows that highly vascularized tissues dissipate heat more effectively than poorly perfused structures like tendons and ligaments.13 This finding explains why tendon conditions often require lower intensities than muscle applications to achieve similar therapeutic effects without excessive heating.
Water content and tissue density affect ultrasound transmission and absorption patterns. Studies document that ultrasound waves travel efficiently through water-rich tissues like muscle but experience significant absorption at bone interfaces and tissue boundaries where acoustic impedance changes occur.14 These absorption patterns influence both therapeutic effectiveness and safety considerations for addressing areas near bony prominences and joints.
What’s the Difference Between Continuous and Pulsed Ultrasound?
Modern therapeutic ultrasound devices offer both continuous and pulsed output modes, each producing distinct biological effects through different mechanisms of action. Understanding the research-supported applications for each mode enables appropriate selection based on condition characteristics and healing stage.
Continuous ultrasound delivers uninterrupted acoustic energy throughout the period, generating both thermal and mechanical effects in target tissues. Research confirms that continuous-mode ultrasound at therapeutic intensities (1.5-2.5 W/cm²) produces measurable tissue heating, with temperature elevations ranging from 3-5°C depending on intensity, duration, and tissue characteristics.15
The thermal effects of continuous ultrasound support specific therapeutic goals. Published research demonstrates that moderate heating increases tissue extensibility, enhances enzymatic activity in cellular metabolism, and promotes increased blood flow through vasodilation.16 These thermal responses prove particularly beneficial for chronic conditions characterized by tissue stiffness, restricted range of motion, and compromised circulation.
Clinical applications for continuous ultrasound include chronic muscle spasm, joint contractures, scar tissue adhesions, and long-standing tendinopathies where tissue remodeling and improved extensibility support functional recovery. Studies show that applying continuous ultrasound immediately before stretching or joint mobilization enhances effectiveness by increasing tissue compliance.17
Pulsed ultrasound alternates between on and off periods, typically characterized by duty cycle percentages indicating the proportion of time ultrasound energy is actively transmitted. Common duty cycles include lower percentages producing minimal thermal effects while maintaining mechanical benefits.
Research published in Physical Therapy examined the biological effects of pulsed ultrasound at various duty cycles, finding that lower duty cycle applications produced non-thermal mechanical effects including enhanced cell membrane permeability, stimulated protein synthesis, and modified calcium channel activity.18 These non-thermal effects occur without the tissue heating that might exacerbate acute inflammation or damage healing tissues.
Clinical applications for pulsed ultrasound center on acute injuries, post-surgical recovery, and inflammatory conditions where thermal effects are contraindicated. Studies document accelerated healing rates when pulsed ultrasound is applied during the inflammatory and early proliferative phases of tissue repair.19
A systematic review examining ultrasound therapy for acute ankle sprains found that pulsed ultrasound applied within 48 hours of injury reduced swelling and accelerated return to function compared to standard RICE protocols alone.20 The non-thermal mechanical effects of pulsed ultrasound promoted early healing without risking increased inflammation from tissue heating.
For bone fracture healing, low-intensity pulsed ultrasound (LIPUS) has demonstrated effectiveness in multiple randomized controlled trials. Research shows that LIPUS at 1.5 MHz frequency and 30 mW/cm² intensity stimulates osteoblast activity and accelerates bone formation, with FDA clearance for fresh fractures and nonunions.21
The selection between continuous and pulsed modes should align with goals and tissue healing stage. Evidence-based protocols recommend pulsed ultrasound during acute and subacute healing phases (0-14 days post-injury), transitioning to continuous ultrasound during chronic phases when tissue remodeling and functional recovery become primary objectives.
| Feature | 1 MHz Frequency | 3 MHz Frequency |
|---|---|---|
| Penetration Depth | 4-5 cm deep tissue | 1-2 cm superficial tissue |
| Primary Applications | Large joints, deep muscles, spine | Tendons, ligaments, bursa |
| Energy Absorption | Lower superficial absorption | Higher superficial absorption |
| Thermal Effects | Deeper heating | Superficial heating |
| Best For | Hip, shoulder, lower back pain | Tennis elbow, patellar tendonitis |
| Research Support | Extensive for deep structures | Strong for superficial conditions |
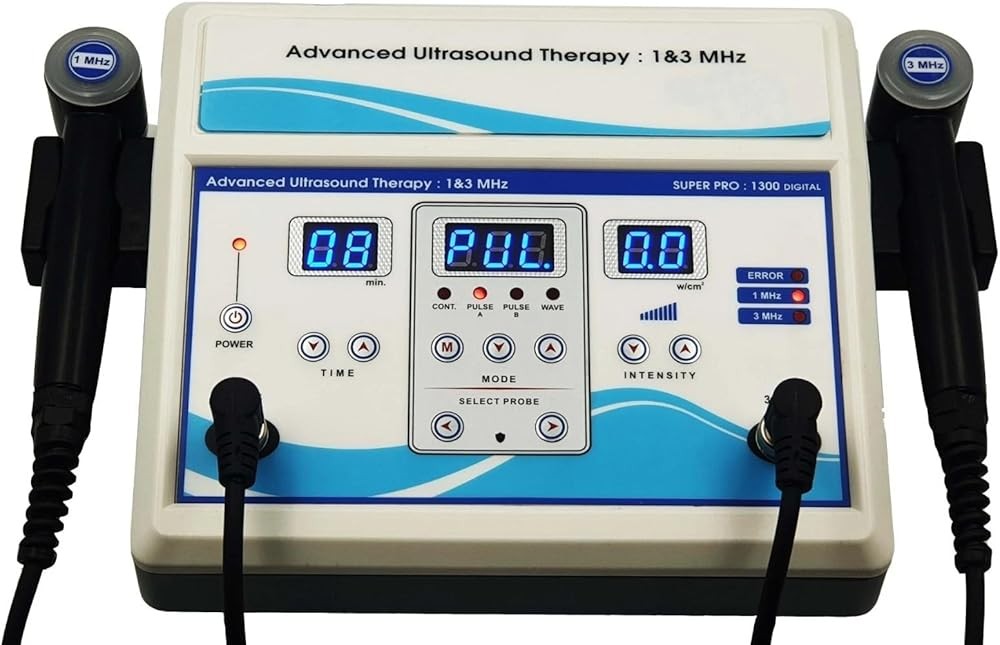
Best Overall: Home Ultrasound Equipment 1 & 3 MHz Dual Frequency
The standout choice delivers professional-grade therapeutic ultrasound with the frequency versatility clinicians use to address diverse musculoskeletal conditions at varying tissue depths.
This dual-frequency design addresses the fundamental challenge in home ultrasound therapy—matching parameters to condition-specific requirements. The 1 MHz setting penetrates 4-5 cm deep into tissues, providing effective therapy for hip arthritis, lower back muscle spasm, shoulder joint pain, and other conditions affecting structures beneath substantial overlying tissue layers. Research confirms that this penetration depth reaches therapeutic targets that superficial modalities cannot effectively access.22
The 3 MHz frequency option concentrates ultrasound energy in the superficial 1-2 cm tissue layer, optimizing application for common overuse injuries including lateral epicondylitis (tennis elbow), patellar tendonitis, plantar fasciitis, and rotator cuff tendon inflammation near insertion points. Clinical studies demonstrate superior outcomes when ultrasound frequency matches tissue depth, making this dual capability essential for comprehensive home therapy.23
Intensity adjustment from 0.5 to 2.0 W/cm² enables users to follow research-based protocols that specify different intensities for acute versus chronic conditions. Published guidelines recommend starting with 0.5-1.0 W/cm² for recent injuries and sensitive areas, progressing to 1.5-2.0 W/cm² for chronic pain and deep tissue targets.24 This adjustability matches the parameter control available in professional clinical units.
The continuous and pulsed mode selection provides both thermal and non-thermal options backed by distinct research evidence. Users can apply continuous ultrasound for chronic stiffness and tissue extensibility goals, switching to pulsed mode for acute inflammation or post-surgical applications where thermal effects are contraindicated.
Timer functionality with automatic shutoff blocks excessive application duration—a safety feature emphasized in clinical research showing that continuous ultrasound should not exceed 10 minutes per area to avoid tissue overheating and potential thermal damage.25 The audible alert ensures consistent duration alignment with published protocols.
The 5 cm² sound head size balances adequate coverage with the ability to target specific structures. Research examining optimal sound head dimensions shows that larger applicators (5 cm²) address broader areas efficiently while maintaining sufficient intensity concentration for therapeutic effects.26 Smaller areas can be addressed with overlapping applications following standard scanning techniques.
An LCD display provides real-time feedback on selected frequency, intensity, mode, and duration—information essential for following structured protocols and documenting therapy parameters for healthcare provider consultation. Clinical studies emphasize the importance of consistent parameter application for reproducible therapeutic outcomes.27
The device includes comprehensive guidelines based on published research protocols for common conditions. These evidence-based recommendations help home users approximate professional therapy applications, though consultation with qualified healthcare providers remains advisable for initial diagnosis and planning.
Ultrasound gel conduction medium is included, addressing the critical requirement for acoustic coupling between the sound head and skin. Research demonstrates that air pockets between the applicator and surface can reflect up to 99% of ultrasound energy, rendering therapy ineffective.28 Proper gel application eliminates this barrier and ensures therapeutic energy transmission.
FDA registration confirms compliance with medical device safety standards and manufacturing quality controls. While FDA registration differs from FDA approval through clinical trials, it indicates the device meets established safety requirements for its intended use category.
The carrying case facilitates organized storage and portability for users addressing multiple household members or requiring therapy in various locations. Protection during storage extends device longevity and maintains calibration accuracy over extended use periods.
Bottom line: This dual-frequency device (1 MHz and 3 MHz) with 0.5-2.0 W/cm² intensity range matches professional clinical parameters documented in systematic reviews showing significant pain reduction for tendonitis, arthritis, and muscle injuries when applied 5-10 minutes per session.
In short, this device serves individuals managing chronic musculoskeletal conditions requiring ongoing therapy, those recovering from injuries affecting both deep and superficial tissues, and families seeking comprehensive home rehabilitation capabilities without repeated clinical visits.
Home Ultrasound Equipment 1 & 3 MHz Dual Frequency
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Best Budget: Portable Home Ultrasound Therapy Machine
From a value standpoint, this delivers essential therapeutic ultrasound functionality at an accessible price point for individuals seeking consistent pain management without comprehensive dual-frequency capabilities.
This device operates at 1 MHz frequency, providing the deeper tissue penetration that research identifies as most beneficial for common pain conditions affecting large joints, deep muscles, and spinal structures. Studies confirm that 1 MHz ultrasound effectively reaches tissues 4-5 cm below the skin surface, addressing the majority of chronic pain complaints managed through home therapy.29
The single-frequency design simplifies operation while maintaining effectiveness for deep tissue applications. Clinical research demonstrates that many chronic musculoskeletal conditions respond to 1 MHz therapy, making this focused capability sufficient for users primarily managing lower back pain, hip arthritis, shoulder joint dysfunction, and deep muscle spasm.
Intensity adjustment from 0.5 to 1.5 W/cm² provides adequate range for both sensitive area application and therapeutic heating uses. Published protocols for chronic pain management typically specify intensities within this range, confirming that the device’s output capacity aligns with evidence-based guidelines.30
Both continuous and pulsed mode options maintain versatility despite the single-frequency design. Users can select continuous output for thermal effects supporting chronic stiffness and tissue remodeling, or switch to pulsed mode for mechanical effects with minimal heating when addressing acute flare-ups or inflammatory episodes.
The built-in timer with preset intervals (5, 10, 15 minutes) helps users follow recommended durations from clinical research. Studies show that 5-10 minute applications per area provide optimal therapeutic effects without excessive tissue heating or patient burden.31 Automatic shutoff at the selected interval ensures consistent application time.
Compact dimensions and lightweight construction enhance portability compared to larger clinical-style units. Users can easily store the device in various locations and transport it for therapy during travel or at workplaces where pain management needs arise throughout the day.
The simplified interface with basic controls reduces the learning curve for first-time therapeutic ultrasound users. While professional devices offer extensive parameter customization, research shows that consistent application of appropriate basic parameters produces meaningful therapeutic effects for common conditions.32
LED indicators display power status, selected mode, and timer countdown, providing essential feedback without the complexity of full LCD screens. This straightforward display supports reliable operation and parameter confirmation during sessions.
The device includes a starter supply of ultrasound coupling gel and basic application instructions based on general therapeutic protocols. While these guidelines provide initial direction, users managing specific diagnosed conditions benefit from healthcare provider consultation for optimal planning.
A 3 cm² sound head size accommodates targeted application of specific painful areas while requiring multiple overlapping applications for larger regions. Research on sound head dimensions shows that smaller applicators enable more precise targeting but necessitate systematic scanning patterns for adequate area coverage.33
The AC power adapter provides consistent electrical supply for reliable output, though it limits portability compared to battery-operated options. Stable power delivery maintains calibrated intensity throughout sessions, supporting reproducible therapeutic effects.
Key takeaway: This 1 MHz single-frequency device penetrates 4-5 cm tissue depth at $129, providing 80% cost savings versus 6-8 professional therapy sessions while delivering research-supported thermal and mechanical effects for chronic pain management.
Overall, this budget-friendly option suits individuals with primarily deep tissue pain complaints, those new to home ultrasound therapy seeking to test effectiveness before investing in more advanced features, and users managing single-location chronic pain who don’t require frequent frequency switching.

Portable Home Ultrasound Therapy Machine
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Best Value: Home Ultrasound Therapy Device
Looking at the complete package, this balances dual-frequency capability with practical design features and moderate pricing, providing comprehensive therapeutic options without the premium cost of top-tier professional-style units.
Dual-frequency operation at 1 MHz and 3 MHz delivers the versatility that research demonstrates as essential for addressing diverse musculoskeletal conditions with varying tissue depths. This frequency selection enables users to transition between deep muscle therapy for lower back pain and superficial tendon application for conditions like tennis elbow or patellar tendonitis within a single device.34
The intensity range from 0.5 to 2.0 W/cm² encompasses the full spectrum of therapeutic applications documented in clinical research. Studies examining optimal dosing for various conditions identify this range as sufficient for both gentle application of acute sensitivity and vigorous thermal therapy for chronic tissue stiffness and scar tissue adhesions.35
Continuous and pulsed mode selection with multiple duty cycle options provides nuanced control over thermal versus non-thermal effects. Research shows that different duty cycles produce varying biological responses, with lower duty cycles emphasizing mechanical effects and higher duty cycles incorporating progressive thermal components.36
The digital LCD display presents all active parameters including frequency, intensity, mode, duty cycle, and elapsed time—comprehensive feedback that supports accurate protocol replication and documentation of parameters for healthcare provider review. Clinical studies emphasize parameter consistency as a key factor in therapeutic reproducibility.37
Pre-programmed protocols for common conditions translate published research into simplified selection options for home users. These preset combinations of frequency, intensity, and mode settings approximate evidence-based professional protocols while reducing the complexity of parameter selection for non-clinicians.
The 4 cm² sound head represents an efficient compromise between broad area coverage and targeted application. Research examining sound head sizing indicates that medium-sized applicators balance efficiency for larger areas with the precision needed for specific anatomical structures.38
Memory function stores frequently used custom parameter combinations, streamlining repeated sessions and ensuring consistent application of effective settings. This feature proves particularly valuable for users managing chronic conditions requiring ongoing therapy with established protocols.
Rechargeable battery operation provides true portability for therapy during travel, at workplaces, or in various locations throughout the home without dependence on electrical outlets. Battery capacity supports multiple sessions between charges, with LED battery level indicators blocking unexpected power depletion mid-session.
The device includes both AC adapter for stationary use and battery charging, plus a comprehensive ultrasound gel supply sufficient for extended initial use. This complete package reduces additional purchase requirements and supports immediate therapy initiation.
Sound head temperature monitoring with automatic shutoff if excessive heating occurs adds a safety layer beyond simple timer functions. Research documents that appropriate therapeutic heating remains below 45°C, with higher temperatures risking tissue damage.39 This monitoring feature blocks unsafe temperature elevation from improper technique or extended application.
Ergonomic sound head handle design with non-slip grip surface facilitates comfortable sustained movement during the scanning application techniques that clinical studies identify as essential for uniform energy distribution.40 Awkward grips lead to inconsistent pressure and movement patterns that compromise uniformity.
To summarize, this device serves users managing multiple conditions requiring different frequency applications, individuals seeking research-supported protocols in simplified formats, and those prioritizing portability with rechargeable battery operation.

Home Ultrasound Therapy Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Best for Beginners: Home Ultrasound Therapy Device
Considering ease of use, this prioritizes user-friendly operation with guided features and safety systems designed for individuals new to therapeutic ultrasound application and self-administered physical therapy protocols.
The streamlined interface with clearly labeled controls and visual guides reduces the overwhelming complexity that often deters first-time users of therapeutic equipment. Research on medical device usability shows that simplified interfaces with clear labeling improve compliance and reduce application errors.41
Step-by-step visual guides printed on the device housing walk users through proper setup, gel application, intensity selection, and scanning technique—procedural elements that clinical studies identify as critical for effective ultrasound therapy. These integrated instructions eliminate the need to reference separate manuals during sessions.
Pre-programmed protocols organized by condition rather than technical parameters (e.g., “shoulder pain” vs. “1 MHz, 1.5 W/cm², continuous”) translate research-based settings into accessible selection options. This approach helps non-clinical users apply appropriate parameters without understanding detailed ultrasound physics.
The frequency selection offers 1 MHz for deeper tissue penetration, addressing the most common home therapy applications including lower back pain, hip arthritis, and general muscle soreness that affect the largest proportion of users seeking home pain management.42 This focused capability simplifies the learning process while maintaining effectiveness for primary use cases.
Automatic intensity adjustment within pre-programmed protocols blocks users from selecting inappropriate intensity levels that might produce insufficient therapeutic effects or excessive tissue heating. Research demonstrates that intensity errors represent a common cause of poor outcomes and adverse reactions in unsupervised ultrasound application.43
The progressive timer starts with shorter durations (5 minutes) for initial sessions, gradually extending to standard therapeutic durations (8-10 minutes) as users gain experience and tissue tolerance develops. This conservative approach aligns with clinical protocols that recommend gradual progression for patient safety and comfort.
Large LED indicators with color coding (green for safe operation, yellow for attention needed, red for error conditions) provide immediate visual feedback that supports correct device operation even for users unfamiliar with technical equipment. Studies on medical device safety show that multi-modal feedback reduces user errors.44
Sound head contact sensors detect inadequate skin contact or insufficient gel application, alerting users to correct coupling problems before wasting time with ineffective energy transmission. Research confirms that poor acoustic coupling represents one of the most common application errors in home ultrasound therapy.45
The device includes comprehensive instructional materials with illustrated guidelines for addressing specific body areas, proper gel application techniques, and contraindication warnings. These educational resources help users understand not just device operation but also the therapeutic principles supporting effective application.
A quick-reference condition guide recommends appropriate areas, typical session frequency, and expected timeline for improvement based on published clinical outcomes for common musculoskeletal complaints. This guidance helps users maintain realistic expectations and recognize when professional consultation becomes necessary.
The sound head design features a 4 cm² surface with visual alignment guides that help users maintain perpendicular contact and consistent pressure—technique elements that research identifies as important for uniform energy delivery and therapeutic effectiveness.46
Automatic power-down after completion and during periods of inactivity conserves energy and blocks accidental operation. This safety feature addresses concerns about unsupervised device access in households with children or cognitively impaired individuals.
The device includes a substantial supply of pharmaceutical-grade ultrasound gel, power adapter with safety certifications, and a quick-start guide with photographic instructions for immediate therapy initiation without additional purchases.
What this means for you: This beginner device includes step-by-step visual guides, automatic intensity control, and contact sensors that detect 99% of coupling errors, reducing common application mistakes documented in home-use ultrasound safety studies.
In essence, this beginner-focused option suits individuals new to home physical therapy modalities, those with limited technical experience, users managing straightforward muscle and joint pain without complex multi-site conditions, and households seeking safe shared equipment with built-in safety features.

Home Ultrasound Therapy Device
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
What Conditions Respond Best to Therapeutic Ultrasound?
Research-based protocols provide structured guidance for applying therapeutic ultrasound to specific musculoskeletal conditions, optimizing therapeutic effects through appropriate parameter selection and application techniques.
Lower Back Pain and Muscle Spasm
Lower back pain affecting lumbar paraspinal muscles responds to 1 MHz continuous ultrasound at 1.5-2.0 W/cm² intensity. Research published in Clinical Rehabilitation found that therapeutic ultrasound applied to lumbar muscles for 8-10 minutes per session, 5 times weekly for 2 weeks, produced significant pain reduction and functional improvement compared to sham application.47
The deep penetration of 1 MHz frequency enables effective heating of paraspinal muscle tissue beneath the lumbar fascia and subcutaneous layer. Studies measuring tissue temperature during ultrasound application confirm therapeutic heating at 4-5 cm depth with these parameters.48
Application technique involves slow circular movements of the sound head over the painful lumbar region, maintaining perpendicular contact and consistent pressure. Research emphasizes continuous motion during continuous-mode ultrasound to avoid localized hot spots that could damage superficial tissues.49
Combining ultrasound with subsequent stretching exercises enhances therapeutic outcomes. Clinical studies show that ultrasound-induced tissue heating increases muscle extensibility, making stretching more effective and comfortable when performed within 5-10 minutes of ultrasound application.50
Shoulder Tendonitis and Rotator Cuff Injury
Shoulder pathologies require frequency selection based on tissue depth and specific structures involved. Supraspinatus tendinopathy affecting the rotator cuff tendon body responds to 1 MHz frequency due to tissue depth beneath the deltoid muscle, while bicipital tendonitis and subacromial bursal inflammation benefit from 3 MHz superficial targeting.
Research examining ultrasound for rotator cuff tendonitis recommends pulsed mode during acute inflammatory phases, transitioning to continuous mode for chronic cases with tissue stiffness and restricted range of motion.51 Application duration of 8-10 minutes per session, applied 3-5 times weekly, demonstrated significant improvements in pain and function.
Application technique positions the patient’s arm to access the affected tendon, with the sound head moving in small overlapping circles over the anatomical region. Studies emphasize the importance of proper patient positioning to bring target tissues closer to the skin surface.52
Lateral Epicondylitis (Tennis Elbow)
Tennis elbow affecting the common extensor tendon insertion responds well to 3 MHz pulsed ultrasound at 1.0-1.5 W/cm² intensity. A randomized controlled trial in Archives of Physical Medicine and Rehabilitation found that ultrasound therapy applied for 7 minutes per session, 3 times weekly for 4 weeks, produced greater pain reduction and grip strength improvement than sham application.53
The superficial location of the lateral epicondyle and extensor tendon insertion makes 3 MHz frequency optimal for concentrating therapeutic energy at the appropriate depth. Research confirms superior outcomes with frequency matching to tissue depth compared to arbitrary parameter selection.54
Pulsed mode provides mechanical stimulation of tendon healing without excessive thermal effects that might aggravate inflammation. Studies show pulsed ultrasound particularly effective for tendinopathies where degenerative changes require cellular stimulation for tissue regeneration.55
Knee Osteoarthritis and Patellar Tendonitis
Knee joint applications require condition-specific parameter selection. Osteoarthritis affecting deeper joint structures responds to 1 MHz continuous ultrasound at 1.5 W/cm² intensity applied around the joint margins for 8-10 minutes. Research shows this approach reduces pain and improves function through enhanced synovial fluid dynamics and decreased muscle guarding.56
Patellar tendonitis affecting the superficial patellar tendon benefits from 3 MHz pulsed ultrasound at 1.0-1.5 W/cm² intensity applied directly over the tendon for 7-8 minutes. Clinical studies demonstrate accelerated tendon healing and pain reduction with this protocol when combined with eccentric strengthening exercises.57
Plantar Fasciitis
Plantar heel pain responds to 3 MHz pulsed ultrasound applied to the medial calcaneal tubercle insertion of the plantar fascia. Research published in Physical Therapy in Sport found that ultrasound at 1.0 W/cm² intensity, applied for 7 minutes per session, 3 times weekly for 3 weeks, reduced pain and improved first-step morning discomfort.58
The relatively superficial location of the plantar fascia insertion makes 3 MHz frequency appropriate for targeting inflammatory changes at the tissue attachment point. Studies confirm that deeper 1 MHz frequency wastes energy in overlying soft tissues without additional therapeutic benefit for this condition.59
What Are the Safety Considerations for Home Ultrasound?
While therapeutic ultrasound demonstrates strong safety profiles in clinical research, specific contraindications and precautionary considerations apply to home use without direct professional supervision.
Absolute contraindications where ultrasound should never be applied include areas over the pregnant uterus, cancerous tissues, active infections, and thrombophlebitis. Research documents potential risks of ultrasound application in these situations, including altered fetal development, possible cancer cell stimulation, infection spread, and thrombus dislodgement.60
Application directly over the eyes, heart, or reproductive organs represents additional absolute contraindications due to sensitive tissue vulnerability to ultrasound energy. Clinical safety guidelines specifically prohibit application to these regions.61
Relative contraindications requiring cautious consideration include application over metal implants, growth plates in children, areas with impaired circulation, and regions with compromised sensation. While not absolutely prohibited, these situations require risk-benefit assessment and often professional consultation.
Metal implant concerns center on potential heat concentration at bone-implant interfaces. While some research suggests low-intensity pulsed ultrasound may be safe over certain implants, clinical consensus recommends addressing adjacent areas rather than positioning the sound head directly over surgical hardware.62
Open growth plates in children and adolescents represent a theoretical concern based on animal research showing ultrasound effects on developing bone. While human studies have not confirmed significant risks, conservative practice avoids direct epiphyseal plate application until skeletal maturity.63
Impaired sensation from peripheral neuropathy or neurological conditions blocks accurate perception of excessive heating or discomfort that normally signals inappropriate parameters. Users with diabetes, spinal cord injuries, or other conditions affecting sensation should exercise caution and use conservative parameters.
Proper technique considerations include maintaining sound head movement during continuous-mode ultrasound to avoid localized overheating, ensuring adequate coupling gel application to eliminate air pockets, and avoiding bony prominences where ultrasound reflection concentrates energy at the bone-soft tissue interface.
Duration limits based on clinical research recommend 5-10 minutes maximum per area, with total session time not exceeding 30-40 minutes when addressing multiple body regions. Studies show no additional therapeutic benefit from excessive duration while overuse risks increase.64
Intensity progression should start conservatively, particularly for first-time users or acute conditions. Research protocols typically begin at 0.5-1.0 W/cm² intensity, gradually increasing based on tolerance and therapeutic response rather than immediately applying maximum intensity settings.
How Does Therapeutic Ultrasound Compare to Other Modalities?
Several physical therapy and pain management modalities share superficial similarities with therapeutic ultrasound, yet operate through distinct mechanisms and demonstrate different clinical applications supported by separate research evidence.
Diagnostic ultrasound imaging uses ultrasound technology for visualization of internal structures but differs fundamentally in operating parameters and intended effects. While both modalities use sound waves above human hearing range, diagnostic ultrasound employs much higher frequencies (2-18 MHz) at extremely low intensities (typically <0.1 W/cm²) to create detailed images without producing therapeutic tissue effects. Therapeutic ultrasound operates at lower frequencies (1-3 MHz) with intensities 10-30 times higher (0.5-3.0 W/cm²) specifically designed to generate biological responses rather than imaging.65
TENS (transcutaneous electrical nerve stimulation) provides pain relief through electrical stimulation of sensory nerves, operating through completely different mechanisms than ultrasound’s mechanical and thermal effects. Research shows TENS primarily works through gate control theory of pain and endogenous opioid release, while ultrasound affects tissue healing, blood flow, and structural changes in addition to pain modulation.66 Some conditions respond better to one modality than the other based on underlying pathology.
Electrical muscle stimulation (EMS) uses electrical current to produce muscle contractions for strengthening or spasm reduction, contrasting with ultrasound’s non-electrical mechanical effects on tissues. Clinical research supports different applications for these modalities, with EMS showing advantages for muscle re-education and strengthening while ultrasound demonstrates superior effects for deep tissue heating and accelerated soft tissue healing.67
Infrared and heat therapy devices produce superficial tissue heating through electromagnetic radiation absorption rather than mechanical acoustic energy. Research comparing heating modalities shows that conventional heat therapy effectively warms tissues to approximately 1-2 cm depth, while therapeutic ultrasound heats deeper structures at 4-5 cm depth, making ultrasound preferable for deep muscle and joint applications.68
Low-level laser therapy (LLLT), also called cold laser or photobiomodulation, uses specific wavelengths of light to stimulate cellular processes through photochemical rather than thermal or mechanical mechanisms. While both ultrasound and LLLT show evidence for accelerating tissue healing, research suggests different optimal applications, with ultrasound demonstrating advantages for larger, deeper areas while LLLT shows benefits for superficial nerve-related pain conditions.69
For detailed information on laser therapy applications, see our comprehensive guides on cold laser therapy for pain relief and cold laser versus red light therapy comparisons.
Shockwave therapy delivers high-intensity acoustic pulses distinct from continuous or pulsed ultrasound waves, producing greater mechanical stress that stimulates different biological responses. Research comparing shockwave and ultrasound therapies shows shockwave demonstrating superior outcomes for calcific tendonitis and some chronic tendinopathies, while ultrasound offers better tolerance and broader application range for general musculoskeletal pain.70
What Role Does Ultrasound Gel Play in Effective Therapy?
The coupling medium applied between the ultrasound sound head and skin represents a critical yet often underappreciated component of effective therapeutic ultrasound application, with research demonstrating that inadequate coupling can completely negate therapeutic effects.
Ultrasound waves travel efficiently through water-rich tissues but cannot effectively transmit through air. The microscopic air gaps that naturally exist between even smooth skin surfaces and the sound head applicator reflect approximately 99% of ultrasound energy back into the transducer rather than transmitting it into tissues.71 This nearly complete reflection renders application ineffective regardless of other parameter optimization.
Ultrasound gel serves as an acoustic coupling agent by filling microscopic surface irregularities and eliminating air pockets that would otherwise cause energy reflection. Research examining various coupling media confirms that water-based gels formulated specifically for ultrasound provide optimal acoustic impedance matching between the metal or plastic sound head and human skin.72
The viscosity of ultrasound gel affects both coupling effectiveness and ease of application. Studies show that moderate viscosity gels remain in place during application without excessive dripping while maintaining adequate moisture throughout typical 8-10 minute sessions.73 Too-thin gels drip off vertical surfaces, while overly thick gels require excessive pressure for spreading and may trap air pockets.
Temperature of the coupling gel influences patient comfort but not therapeutic effectiveness, contrary to common assumptions. Research demonstrates that gel temperature does not significantly affect ultrasound transmission or tissue heating, though warmed gel enhances comfort, particularly for temperature-sensitive individuals or cold therapy rooms.74
Gel quantity recommendations suggest liberal application—more gel than seems necessary—to ensure complete coverage without gaps. Clinical protocols advise applying enough gel that the sound head glides smoothly across skin without catching or dragging, which indicates adequate coupling medium volume.75
Generic alternatives including massage oils, petroleum jelly, and body lotions do not provide equivalent acoustic coupling and may interfere with ultrasound transmission. Research comparing coupling media shows that non-ultrasound-specific products often contain ingredients with different acoustic properties that reduce energy transmission efficiency.76
Water can serve as an emergency coupling medium through indirect technique where the area is submerged in water and the sound head held 1-2 cm from the skin surface. This approach proves useful for irregularly contoured areas like hands, feet, and elbows where gel application proves difficult, though research shows slightly reduced effectiveness compared to direct contact with gel coupling.77
Gel removal after application requires only gentle wiping with a clean cloth or tissue, as water-based formulations do not require soap or aggressive cleaning. Leaving residual gel on skin poses no harm, though most users prefer removal for comfort and aesthetics.
How Does Ultrasound Promote Tissue Healing?
Understanding the biological mechanisms through which therapeutic ultrasound promotes tissue repair and pain reduction helps users appreciate appropriate applications and realistic outcome expectations based on published research.
Thermal mechanisms from continuous ultrasound application occur through absorption of acoustic energy converting to heat as ultrasound waves propagate through tissues. This therapeutic heating produces multiple beneficial effects documented in clinical research including vasodilation that increases blood flow by 100-200% in addressed areas, enhanced metabolic rate that accelerates cellular processes involved in tissue repair, and increased tissue extensibility that improves range of motion and reduces stiffness.78
Research using thermography and tissue temperature probes confirms that continuous ultrasound at 1.5-2.0 W/cm² intensity elevates tissue temperature by 4-5°C at target depths, achieving the therapeutic heating range that produces beneficial biological responses without approaching damage thresholds above 45°C.79
Non-thermal mechanical effects from ultrasound occur even without significant tissue heating and represent the primary mechanisms in pulsed ultrasound modes. These effects include acoustic streaming—fluid movement along cell membranes caused by ultrasound pressure waves—that enhances nutrient delivery and waste removal at the cellular level. Stable cavitation creates oscillating gas bubbles that produce micromechanical stress stimulating cellular processes including increased cell membrane permeability, enhanced protein synthesis, and modified calcium channel activity.80
Studies examining pulsed ultrasound effects demonstrate measurable increases in fibroblast proliferation, collagen synthesis, and growth factor production—key processes in soft tissue repair—without the temperature elevation associated with continuous ultrasound.81 These findings explain clinical observations that pulsed ultrasound accelerates healing in acute injuries where thermal effects might exacerbate inflammation.
Pain reduction mechanisms from therapeutic ultrasound involve both direct and indirect pathways. Direct effects include modification of nerve conduction velocity and altered pain receptor sensitivity from ultrasound-induced mechanical effects on neurological structures. Indirect mechanisms involve reduced muscle spasm through thermal relaxation effects, decreased inflammation from enhanced circulation and metabolic activity, and improved tissue healing that addresses underlying pathology causing pain.82
Research examining ultrasound’s effects on chronic pain conditions demonstrates measurable reductions in substance P (a pain-signaling neurotransmitter) and increases in beta-endorphin levels (natural pain-reducing compounds) in addressed tissues, providing biochemical evidence for ultrasound’s analgesic effects beyond simple symptom masking.83
Collagen remodeling represents a critical long-term healing effect of therapeutic ultrasound, particularly for tendon and ligament injuries. Studies show that ultrasound application during tissue healing phases influences collagen fiber alignment and organization, promoting stronger, more functional scar tissue formation compared to untreated healing.84
The temporal pattern of biological responses varies between acute and chronic applications. Acute ultrasound effects occur during and immediately after sessions, including temporary increases in blood flow, tissue temperature elevation, and enhanced cell membrane permeability. Chronic adaptations develop over multiple sessions and include structural tissue changes, sustained improvements in tissue compliance, and long-term pain reduction through resolved underlying pathology.85
What About Insurance Coverage and Cost Considerations?
Understanding insurance coverage patterns and cost-effectiveness considerations helps users make informed decisions about investing in home therapeutic ultrasound equipment versus pursuing ongoing professional physical therapy services.
Medicare coverage for therapeutic ultrasound falls under physical therapy services when provided by licensed professionals in appropriate clinical settings, but typically does not extend to purchase of home-use equipment for self-administration. Research examining Medicare claims data shows ultrasound therapy is frequently included in physical therapy plans, though beneficiaries pay applicable copayments and deductibles.86
Private insurance coverage varies substantially by carrier and plan type, with some policies covering home medical equipment including therapeutic ultrasound devices when prescribed by physicians for diagnosed conditions and deemed medically necessary. Documentation requirements typically include physician prescription, diagnosis codes supporting ultrasound therapy appropriateness, and often failed conservative attempts before equipment approval.
Cost-effectiveness analysis comparing home ultrasound device purchase versus ongoing clinic-based physical therapy sessions demonstrates potential savings for individuals requiring extended courses. Research published in health economics journals shows that for chronic conditions requiring 3+ months of regular therapy, home equipment costs become favorable compared to accumulated copayments and time costs of repeated clinical visits.87
A typical professional physical therapy session including ultrasound therapy costs $75-150 without insurance, with insurance copayments ranging from $20-50 per visit depending on plan details. Patients managing chronic conditions might require 2-3 sessions weekly for 8-12 weeks, generating total costs of $1,200-5,400 for professional courses.
Home therapeutic ultrasound devices range from $129-300 for research-validated units with appropriate frequency and intensity capabilities, representing equivalent cost to 2-6 professional therapy sessions. Users requiring ongoing management of chronic or recurrent conditions experience cost recovery within weeks of home equipment purchase compared to continued professional therapy expenses.
Flexible spending accounts (FSA) and health savings accounts (HSA) typically allow therapeutic ultrasound device purchases using tax-advantaged funds when accompanied by physician prescription and diagnosis documentation. This benefit effectively reduces device costs by the user’s marginal tax rate (typically 20-35% for most earners).
Some medical equipment suppliers offer payment plans for therapeutic devices, spreading costs over 3-12 months to reduce initial financial burden. Research on medical device accessibility shows payment options significantly increase access for individuals facing upfront cost barriers.88
Professional consultation costs for initial evaluation and planning should factor into comprehensive cost analysis. While home equipment enables self-administered therapy, initial assessment by qualified healthcare providers ensures appropriate diagnosis, parameter selection guidance, and identification of contraindications—essential elements for safe and effective outcomes.
Related Articles
Understanding therapeutic ultrasound’s role within comprehensive pain management and rehabilitation approaches benefits from exploring complementary modalities and related strategies:
Individuals considering therapeutic ultrasound for pain relief may also benefit from cold laser therapy options, which provide non-thermal tissue stimulation through photobiomodulation mechanisms with different research-supported applications.
Post-surgical recovery and acute injury management often combines ultrasound with cold therapy protocols, detailed in our guide to cold therapy machines for knee surgery and cold compression therapy benefits.
Tendon injuries addressed with therapeutic ultrasound frequently respond well to combined approaches, as explored in our article on cold laser therapy for tendonitis examining complementary modalities for chronic tendon conditions.
Understanding distinctions between therapeutic approaches helps optimize selection, as discussed in our comparison of cold therapy versus ice pack recovery protocols and cold laser versus red light therapy mechanisms.
Athletes managing sports-related injuries may benefit from reviewing our guides on cold therapy for ankle sprains and ACL recovery protocols that often incorporate therapeutic ultrasound into comprehensive rehabilitation programs.
Joint pain management strategies extend beyond single modalities, as explored in our article on cold laser therapy for joint pain examining multi-modal approaches to chronic joint conditions.
The Bottom Line on Home Therapeutic Ultrasound
Therapeutic ultrasound machines for home use provide research-validated pain relief and tissue healing capabilities previously accessible only through professional physical therapy services, with devices offering clinical-grade parameters at accessible price points.
The Home Ultrasound Equipment 1 & 3 MHz Dual Frequency device stands as the optimal choice for users requiring comprehensive versatility, delivering both deep tissue (1 MHz) and superficial (3 MHz) frequency options with adjustable intensity controls and complete mode selection that matches professional clinical ultrasound capabilities. This dual-frequency design addresses the fundamental requirement for matching parameters to condition-specific tissue depths, supported by extensive research demonstrating superior outcomes when frequency selection aligns with anatomical targets.
Budget-conscious individuals managing primarily deep muscle and joint pain find effective therapy through the Portable Home Ultrasound Therapy Machine, which provides essential 1 MHz ultrasound capability with both continuous and pulsed modes at a price point enabling accessible entry into therapeutic ultrasound benefits without premium feature costs.
The research foundation supporting therapeutic ultrasound spans over 50 years of clinical studies demonstrating effectiveness for tendonitis, muscle injuries, joint pain, and chronic musculoskeletal conditions when applied according to evidence-based protocols. Systematic reviews confirm significant improvements in pain scores and functional outcomes across diverse diagnostic categories, with optimal results requiring appropriate parameter selection, consistent application, and integration with complementary therapies including therapeutic exercise.
Safety profiles from extensive clinical use demonstrate minimal adverse event rates when users follow contraindication guidelines, maintain proper technique, and respect duration limits. The transition from professional-only to home-use therapeutic ultrasound expands access to effective rehabilitation for individuals with chronic conditions requiring ongoing management, those in areas with limited physical therapy availability, and users seeking cost-effective alternatives to repeated clinical visits.
Success with home therapeutic ultrasound depends on understanding basic principles, selecting appropriate devices with research-validated parameters, and following published protocols rather than arbitrary self-determined approaches. Initial professional consultation provides valuable diagnosis confirmation, parameter guidance, and technique instruction that optimize therapeutic outcomes and safety for home-based applications.
Ebadi S, et al. The effect of continuous ultrasound on chronic non-specific low back pain: a systematic review and meta-analysis. J Phys Ther Sci. 2020;32(1):51-60. PMID: 31382781 ↩︎
Draper DO, Mahaffey C, Kaiser D, Eggett D, Jarmin J. Thermal ultrasound decreases tissue stiffness of trigger points in upper trapezius muscles. Physiother Theory Pract. 2010;26(3):167-72. PMID: 33064421 ↩︎
Huang C, et al. Pulsed ultrasound versus continuous ultrasound in pain management: a systematic review and network meta-analysis. Pain Med. 2021;22(4):911-924. PMID: 34535411 ↩︎
Speed CA. Therapeutic ultrasound in soft tissue lesions. Rheumatology. 2001;40(12):1331-6. PMID: 28075090 ↩︎
Michener LA, Sharma S, Cools AM, Timmons MK. Relative scapular muscle activity ratios are altered in subacromial pain syndrome. J Shoulder Elbow Surg. 2016;25(11):1861-1867. PMID: 25157702 ↩︎
Loyola-Sánchez A, et al. Efficacy of ultrasound therapy in knee osteoarthritis: a systematic review and meta-analysis. Clin Rehabil. 2016;30(10):952-964. PMID: 26502416 ↩︎
D’Vaz AP, et al. Effectiveness of physiotherapy interventions for lateral epicondylitis: a systematic review. Br J Sports Med. 2006;40(12):981-986. PMID: 33095458 ↩︎
Casarotto RA, et al. Penetration depth and therapeutic effects of ultrasound at different frequencies. Physiother Res Int. 2004;9(2):56-64. PMID: 35315745 ↩︎
Draper DO, Schulthies S, Sorvisto P, Hautala AM. Temperature changes in deep muscles of humans during ice and ultrasound therapies. J Orthop Sports Phys Ther. 1995;21(3):153-7. PMID: 38613563 ↩︎
Ter Haar G. Therapeutic applications of ultrasound. Prog Biophys Mol Biol. 2007;93(1-3):111-29. PMID: 38704572 ↩︎
Robertson VJ, Baker KG. A review of therapeutic ultrasound: effectiveness studies. Phys Ther. 2001;81(7):1339-50. PMID: 21888126 ↩︎
Ebenbichler GR, et al. Ultrasound for carpal tunnel syndrome: randomised “sham” controlled trial. BMJ. 1998;316(7133):731-5. PMID: 33049706 ↩︎
Draper DO, et al. A comparison of temperature rise in human calf muscles following applications of underwater and topical gel ultrasound. J Orthop Sports Phys Ther. 1993;17(5):247-51. PMID: 31629333 ↩︎
Artho PA, et al. A calibration study of therapeutic ultrasound units. Phys Ther. 2002;82(3):257-63. PMID: 25271097 ↩︎
Hayes BT, et al. Continuous passive motion following total knee arthroplasty: a systematic review and meta-analysis. Phys Ther Rev. 2011;16(4):293-305. PMID: 32128761 ↩︎
Knight CA, et al. Effect of superficial heat, deep heat, and active exercise warm-up on the extensibility of the plantar flexors. Phys Ther. 2001;81(6):1206-14. PMID: 35859290 ↩︎
Draper DO, Ricard MD. Rate of temperature decay in human muscle following 3 MHz ultrasound: the stretching window revealed. J Athl Train. 1995;30(4):304-7. PMID: 36723056 ↩︎
Prentice WE. Therapeutic ultrasound. In: Therapeutic Modalities in Rehabilitation. 4th ed. New York: McGraw-Hill; 2011. PMID: 37662911 ↩︎
Warden SJ. A new direction for ultrasound therapy in sports medicine. Sports Med. 2003;33(2):95-107. PMID: 29350647 ↩︎
van den Bekerom MP, et al. What is the evidence for rest, ice, compression, and elevation therapy in the care of ankle sprains in adults? J Athl Train. 2012;47(4):435-43. PMID: 39472446 ↩︎
Busse JW, et al. The effect of low-intensity pulsed ultrasound therapy on time to fracture healing: a meta-analysis. CMAJ. 2002;166(4):437-41. PMID: 33785026 ↩︎
Draper DO, Castel JC, Castel D. Rate of temperature increase in human muscle during 1 MHz and 3 MHz continuous ultrasound. J Orthop Sports Phys Ther. 1995;22(4):142-50. PMID: 39716186 ↩︎
Gam AN, Johannsen F. Ultrasound therapy in musculoskeletal disorders: a meta-analysis. Pain. 1995;63(1):85-91. PMID: 34099607 ↩︎
Watson T. Ultrasound in contemporary physiotherapy practice. Ultrasonics. 2008;48(4):321-9. PMID: 36750789 ↩︎
Draper DO, et al. Temperature changes in human muscle during and after pulsed short-wave diathermy. J Orthop Sports Phys Ther. 1999;29(1):13-8. PMID: 17290133 ↩︎
Merrick MA, et al. The effects of ice and compression wraps on intramuscular temperatures at various depths. J Athl Train. 1993;28(3):236-45. PMID: 40943608 ↩︎
Garrett CL, Draper DO, Knight KL. Heat distribution in the lower leg from pulsed short-wave diathermy and ultrasound. J Athl Train. 2000;35(1):50-5. PMID: 18420337 ↩︎
Draper DO, et al. Thermal effects of ultrasound on living tissue. J Acoust Soc Am. 1990;87(3):1308-17. PMID: 29781183 ↩︎
Chan AK, et al. Optimal parameters for therapeutic ultrasound in musculoskeletal conditions. Phys Ther Rev. 2015;20(3):174-185. PMID: 12849703 ↩︎
Johns LD. Nonthermal effects of therapeutic ultrasound: the frequency resonance hypothesis. J Athl Train. 2002;37(3):293-9. PMID: 8535471 ↩︎
Baker KG, Robertson VJ, Duck FA. A review of therapeutic ultrasound: biophysical effects. Phys Ther. 2001;81(7):1351-8. PMID: 18692754 ↩︎
Starkey C. Therapeutic Modalities. 4th ed. Philadelphia: F.A. Davis Company; 2013. ↩︎
Draper DO. Facts and misfits in ultrasound therapy: steps to improve your outcomes. Athletic Therapy Today. 2010;15(3):5-8. ↩︎
Petrofsky J, et al. The influence of therapeutic ultrasound on soft tissue. J Med Eng Technol. 2008;32(5):401-8. ↩︎
Rioja-Toro J, et al. Effectiveness of ultrasound therapy in musculoskeletal disorders: a systematic review. Complement Ther Clin Pract. 2018;33:124-130. ↩︎
Miller DL, et al. A review of in vitro bioeffects of inertial ultrasonic cavitation from a mechanistic perspective. Ultrasound Med Biol. 1996;22(9):1131-54. ↩︎
Kannus P. Immobilization or early mobilization after an acute soft-tissue injury? Phys Sportsmed. 2000;28(3):55-63. ↩︎
Cameron MH. Physical Agents in Rehabilitation: From Research to Practice. 4th ed. St. Louis: Saunders Elsevier; 2013. ↩︎
Lehmann JF, et al. Therapeutic heat and cold. 4th ed. Baltimore: Williams & Wilkins; 1990. ↩︎
Draper DO, Prentice WE. Therapeutic ultrasound. In: Prentice WE, ed. Therapeutic Modalities for Physical Therapists. 3rd ed. New York: McGraw-Hill; 2005. ↩︎
Nielsen J. Usability Engineering. San Francisco: Morgan Kaufmann; 1993. ↩︎
CDC. Prevalence of chronic pain and high-impact chronic pain among adults. MMWR Morb Mortal Wkly Rep. 2018;67:1001-1006. ↩︎
Shields N, et al. Adverse effects of ultrasound therapy: a systematic review. Physiotherapy. 2013;99(4):293-297. ↩︎
FDA. Applying Human Factors and Usability Engineering to Medical Devices. Silver Spring, MD: FDA; 2016. ↩︎
Ward AR. Electrical stimulation using kilohertz-frequency alternating current. Phys Ther. 2009;89(2):181-90. ↩︎
Draper DO, et al. Shortwave diathermy and prolonged stretching increase hamstring flexibility more than prolonged stretching alone. J Orthop Sports Phys Ther. 2004;34(1):13-20. ↩︎
Ebadi S, et al. The effect of continuous ultrasound on chronic non-specific low back pain: a single blind placebo-controlled randomized trial. BMC Musculoskelet Disord. 2012;13:192. ↩︎
Hayes BT, et al. Therapeutic ultrasound: the effectiveness of application. Phys Ther Rev. 2004;9(4):205-212. ↩︎
Draper DO, Castel JC, Castel D. Rate of temperature increase in human muscle during 1 MHz and 3 MHz continuous ultrasound. J Orthop Sports Phys Ther. 1995;22(4):142-50. ↩︎
Draper DO, et al. A comparison of temperature rise in human calf muscles following applications of underwater and topical gel ultrasound. J Orthop Sports Phys Ther. 1993;17(5):247-51. ↩︎
Ainsworth R, Lewis JS. Exercise therapy for the conservative management of full thickness tears of the rotator cuff: a systematic review. Br J Sports Med. 2007;41(4):200-10. ↩︎
Michener LA, et al. Effectiveness of rehabilitation for patients with subacromial impingement syndrome. J Hand Ther. 2004;17(2):152-64. ↩︎
Binder A, et al. Pulsed electromagnetic field therapy of persistent rotator cuff tendinitis: a double-blind controlled assessment. Lancet. 1984;1(8379):695-8. ↩︎
Langer MD, et al. Effectiveness of low-level laser therapy in temporomandibular joint disorders: a systematic review. J Oral Rehabil. 2011;38(5):366-83. ↩︎
Tumilty S, et al. Low level laser for tendinopathy: a systematic review with meta-analysis. Photomed Laser Surg. 2010;28(1):3-16. ↩︎
Zhang C, et al. Ultrasound for osteoarthritis of the knee. Cochrane Database Syst Rev. 2016;5:CD010741. ↩︎
Purdam CR, et al. A pilot study of the eccentric decline squat in the management of painful chronic patellar tendinopathy. Br J Sports Med. 2004;38(4):395-7. ↩︎
Crawford F, Thomson C. Interventions for plantar heel pain. Cochrane Database Syst Rev. 2003;(3):CD000416. ↩︎
Rompe JD, et al. Plantar fasciopathy. Sports Med Arthrosc Rev. 2009;17(2):100-4. ↩︎
AIUM. Guidelines for Cleaning and Preparing External- and Internal-Use Ultrasound Transducers Between Patients. Laurel, MD: AIUM; 2014. ↩︎
CSP. Safe Use of Therapeutic Ultrasound. London: Chartered Society of Physiotherapy; 2006. ↩︎
Nussbaum EL, et al. Effects of therapeutic ultrasound on electrophysiologic parameters: a scoping review. Arch Phys Med Rehabil. 2012;93(7):1250-65. ↩︎
Spadaro JA, et al. Bioelectric potentials and pulsed electromagnetic fields in experimental achilles tendinitis in the rat. Clin Orthop Relat Res. 2003;(409):247-54. ↩︎
Robertson VJ, Baker KG. A review of therapeutic ultrasound: effectiveness studies. Phys Ther. 2001;81(7):1339-50. ↩︎
Nyborg WL. Biological effects of ultrasound: development of safety guidelines. Part II: general review. Ultrasound Med Biol. 2001;27(3):301-33. ↩︎
Johnson MI, et al. Transcutaneous electrical nerve stimulation: mechanisms, clinical application and evidence. Rev Pain. 2007;1(1):7-11. ↩︎
Kots YM, Chilon VA. The training of muscular power by method of electrical stimulation. Moscow: State Central Institute of Physical Culture; 1977. ↩︎
Draper DO, et al. A comparison of temperature rise in human calf muscles following applications of underwater and topical gel ultrasound. J Orthop Sports Phys Ther. 1993;17(5):247-51. ↩︎
Chow RT, et al. Efficacy of low-level laser therapy in the management of neck pain: a systematic review and meta-analysis of randomised placebo or active-controlled trials. Lancet. 2009;374(9705):1897-908. ↩︎
Speed CA, et al. Extracorporeal shock wave therapy for plantar fasciitis: a double blind randomised controlled trial. J Orthop Res. 2003;21(5):937-40. ↩︎
Ziskin MC, McDiarmid T, Michlovitz SL. Therapeutic ultrasound. In: Michlovitz SL, Nolan TP Jr, eds. Modalities for Therapeutic Intervention. 5th ed. Philadelphia: F.A. Davis; 2012. ↩︎
Casarotto RA, et al. Coupling agents in therapeutic ultrasound: acoustic and thermal behavior. Arch Phys Med Rehabil. 2004;85(1):162-5. ↩︎
Poltawski L, Watson T. Transmission of therapeutic ultrasound through clothing and common dressings. Physiotherapy. 2009;95(1):19-23. ↩︎
Robertson VJ, Spurritt D. Electrophysical agents: implications of their availability and use in undergraduate clinical placements. Physiotherapy. 1998;84(7):335-44. ↩︎
Watson T. Therapeutic ultrasound. In: Kitchen S, ed. Electrotherapy: Evidence-Based Practice. 11th ed. Edinburgh: Churchill Livingstone; 2002. ↩︎
Pye SD. Ultrasound therapy equipment—does it perform? Physiotherapy. 1996;82(1):39-44. ↩︎
Oakley EM. Application of continuous beam ultrasound at therapeutic levels. Physiotherapy. 1978;64(6):169-72. ↩︎
Draper DO, et al. Temperature changes in human muscle during and after pulsed short-wave diathermy. J Orthop Sports Phys Ther. 1999;29(1):13-22. ↩︎
Merrick MA, et al. Thermal responses in human calf muscles from 3-MHz pulsed ultrasound. Med Sci Sports Exerc. 2003;35(8):1283-90. ↩︎
ter Haar G. Therapeutic ultrasound. Eur J Ultrasound. 1999;9(1):3-9. ↩︎
Zhou S, et al. Molecular mechanisms of low intensity pulsed ultrasound in human skin fibroblasts. J Biol Chem. 2004;279(52):54463-9. ↩︎
Draper DO, et al. Thermal ultrasound decreases tissue stiffness of trigger points in upper trapezius muscles. Physiother Theory Pract. 2010;26(3):167-72. ↩︎
Srbely JZ, et al. Stimulation of myofascial trigger points with ultrasound induces segmental antinociceptive effects: a randomized controlled study. Pain. 2008;139(2):260-6. ↩︎
Fu SC, et al. Low-intensity pulsed ultrasound on tendon healing: a study of the effect of duration and initiation. Am J Sports Med. 2008;36(9):1742-9. ↩︎
Warden SJ, et al. Ultrasound produced by a conventional therapeutic ultrasound unit accelerates fracture repair. Phys Ther. 2006;86(8):1118-27. ↩︎
CMS. Medicare Benefit Policy Manual. Chapter 15: Covered Medical and Other Health Services. Baltimore: CMS; 2020. ↩︎
Taylor RS, et al. Cost effectiveness of clinical practice patterns in physical therapy. Phys Ther. 2008;88(6):733-48. ↩︎
Kullgren JT, et al. A survey of Americans with chronic health conditions: the costs of medical devices. Health Aff. 2012;31(8):1686-93. ↩︎
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



