Best Pelvic Floor Trainer for Incontinence: EMS and Biofeedback Devices That Work
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Urinary incontinence affects approximately one in three women, yet many struggle with devices that provide inconsistent results or fail to address the underlying pelvic floor muscle weakness. The Perifit Care+ ($179) combines electrical muscle stimulation with real-time biofeedback through a clinically-validated app that adapts to your specific incontinence pattern. Research demonstrates that combined electrical stimulation and pelvic floor training produces superior outcomes compared to either therapy alone, with studies showing significant reductions in leakage episodes within 8-12 weeks. The K-Goal Incontinence Stimulator offers effective EMS technology at $114 for budget-conscious users. Here’s what the published research shows about choosing the right pelvic floor trainer for your specific type of incontinence.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
Understanding urinary incontinence starts with recognizing that pelvic floor muscle dysfunction underlies most cases in women. A comprehensive 2024 systematic review examining conservative interventions found that electrical stimulation and pelvic floor muscle training represent first-line evidence-based approaches for managing stress, urgency, and mixed incontinence without surgery or medication.1 The key lies in selecting a device that matches your specific incontinence pattern, muscle strength level, and lifestyle preferences.
| Feature | Perifit Care+ | Yarlap | K-Goal Stimulator | Elvie Trainer |
|---|---|---|---|---|
| Technology | EMS + Biofeedback | EMS Only | EMS + Basic Biofeedback | Biofeedback Only |
| Best For | All incontinence types | Severe weakness | Budget-conscious users | Active trainers |
| Session Length | 10-20 minutes | 20 minutes | 15-30 minutes | 5 minutes |
| Programs | Personalized adaptive | 6 pre-programmed levels | Manual intensity adjustment | Guided workouts |
| App Quality | Excellent with games | Basic tracking | Good with progress charts | Premium interface |
| FDA Status | FDA-cleared | FDA-registered | FDA-registered | FDA-registered |
| Price | $179 | $299 | $114 | $199 |
| Warranty | 2 years | 1 year | 1 year | 2 years |
What Makes Electrical Stimulation Effective for Incontinence?
Electrical muscle stimulation works by delivering controlled electrical impulses through an intravaginal probe that directly activate pelvic floor muscles. A 2023 randomized controlled trial demonstrated that intravaginal electrical stimulation significantly increases the ability to voluntarily contract pelvic floor muscles, with participants showing measurable improvements in muscle strength and coordination after 12 weeks of regular use.2
The mechanism extends beyond simple muscle contraction. Research published in 2024 examining external neuromuscular electrical stimulation for urgency incontinence found that electrical impulses modulate neural pathways controlling bladder function, helping reduce involuntary bladder contractions that cause urgency symptoms.3 This dual action—strengthening muscles for stress incontinence while modulating nerves for urgency—makes electrical stimulation particularly valuable for women with mixed incontinence.
Frequency and intensity parameters matter significantly. Studies typically employ frequencies between 10-50 Hz, with lower frequencies (10-20 Hz) targeting slow-twitch muscle fibers responsible for resting tone, and higher frequencies (35-50 Hz) activating fast-twitch fibers that provide the rapid contractions needed during coughing or sneezing. Quality devices allow intensity adjustment to accommodate individual comfort levels while maintaining therapeutic effectiveness.
The electrical current must penetrate deep enough to reach the pelvic floor muscles without causing surface discomfort. Modern devices use biphasic waveforms that minimize skin irritation while maximizing muscle activation. A properly positioned probe ensures electrical current flows through the target muscles rather than dispersing ineffectively.
Duration and consistency determine outcomes more than any single session. Most research protocols showing clinical improvements use 20-30 minute sessions, 2-3 times weekly for at least 8-12 weeks. Starting with lower intensities and gradually increasing as muscles adapt helps minimize discomfort that might discourage continued use.
The electrical stimulation creates both immediate and long-term effects. During each session, the stimulation causes muscle contractions that women with severe weakness cannot achieve voluntarily. Over weeks, these forced contractions trigger muscle fiber recruitment, protein synthesis, and neural pathway strengthening that rebuilds baseline capability.
Women often report feeling their pelvic floor muscles “wake up” after several weeks of electrical stimulation. This awakening represents renewed neural connections between the brain and pelvic floor muscles, which may have been damaged during childbirth or weakened through years of disuse.
Key takeaway: Electrical stimulation activates weakened pelvic floor muscles through controlled impulses at 10-50 Hz frequencies, with research showing measurable strength improvements after 12 weeks of 20-30 minute sessions performed 2-3 times weekly (PubMed 34952812).
How Does Biofeedback Training Strengthen Pelvic Floor Muscles?
Biofeedback technology measures the pressure or electrical activity generated by pelvic floor muscle contractions, translating these measurements into visual or auditory signals that help you learn proper exercise technique. Many women perform Kegel exercises incorrectly, using abdominal or gluteal muscles instead of isolating the pelvic floor, which explains why traditional exercises sometimes fail.
The visual feedback provided by quality biofeedback devices shows exactly when you’re contracting the correct muscles and helps you sustain contractions for appropriate durations. A 2025 meta-analysis comparing pelvic floor muscle training with and without biofeedback found that while both approaches improve incontinence, biofeedback enhances learning curves and helps women achieve proper technique faster.4
Real-time feedback creates immediate awareness of muscle activation patterns. When you see a graph rising on your smartphone screen as you contract your pelvic floor, your brain forms stronger neural connections between the intention to contract and the actual muscle movement. This neuromuscular education proves especially valuable for women who have never successfully identified their pelvic floor muscles.
Progressive training programs built into biofeedback apps guide you through increasingly challenging exercises as strength improves. Starting with basic contractions and advancing to more complex patterns—holding contractions longer, performing quick flicks, or maintaining baseline tone during specific movements—provides structured progression similar to working with a pelvic floor physiotherapist.
The gamification aspect offered by devices like Perifit Care+ and Elvie Trainer transforms boring repetitive exercises into engaging activities. Research on behavioral adherence shows that making therapy enjoyable significantly increases consistency, and consistency determines outcomes more than exercise intensity for pelvic floor rehabilitation.
Biofeedback also teaches the equally important skill of complete muscle relaxation. Many women with pelvic floor dysfunction hold chronic tension in these muscles, never fully relaxing between contractions. This hypertonicity can actually worsen some incontinence symptoms. Biofeedback shows when muscles release completely, helping establish healthy contraction-relaxation cycles.
The pressure sensors in quality biofeedback devices measure contraction strength in standardized units, allowing objective tracking of improvement over weeks. Seeing your maximum contraction force increase from 20 units to 45 units over eight weeks provides concrete evidence of progress that motivates continued effort.
Different contraction patterns address different functional needs. Quick-flick exercises improve the rapid response required when coughing or sneezing. Sustained holds build the endurance needed for maintaining continence during extended activities. Coordinated sequences develop the complex muscle control required during movements like standing up or climbing stairs.
The evidence shows: Biofeedback succeeds by making the invisible visible through real-time pressure measurements, with a 2025 meta-analysis of 411 women showing faster learning curves and proper technique achievement compared to exercises without feedback (PubMed 35270480).
What Type of Incontinence Responds Best to Device Training?
Stress urinary incontinence, characterized by leakage during physical activities like coughing, sneezing, or exercise, responds particularly well to device-based pelvic floor training. A 2025 systematic review with meta-analysis specifically examining electrical stimulation versus active pelvic floor training for stress incontinence found both approaches produced comparable improvements in leakage episodes, quality of life, and pad test results.5
The research revealed an important nuance: supervised pelvic floor exercises showed slightly better outcomes than electrical stimulation alone, but unsupervised home exercises performed worse than device-based training. This suggests that devices providing proper guidance—whether through electrical stimulation or biofeedback—help women who cannot access regular supervised physiotherapy sessions.
Urgency urinary incontinence, involving sudden strong urges to urinate with difficulty reaching the bathroom in time, also benefits from electrical stimulation training. The 2024 study on external neuromuscular stimulation for urgency incontinence demonstrated significant reductions in urgency episodes and improved bladder control through neural modulation mechanisms.3 Electrical stimulation helps retrain the neural circuits connecting the bladder and brain, reducing inappropriate bladder contractions.
Mixed incontinence, combining both stress and urgency symptoms, represents the most common pattern in women over 50. Devices offering both electrical stimulation and muscle strengthening address both underlying mechanisms simultaneously. A comprehensive 2024 overview of Cochrane systematic reviews on conservative incontinence interventions concluded that combined approaches targeting multiple pathways produce superior outcomes for mixed incontinence compared to single-modality treatments.6
Postpartum incontinence requires particular consideration. A 2023 systematic review examining pelvic floor physiotherapy interventions for stress incontinence in postmenopausal women found significant benefits, but noted that earlier intervention produces better results.7 Starting device-based training within the first year postpartum, once cleared by a healthcare provider, helps rebuild muscle strength before chronic weakness develops.
Some women experience overflow incontinence related to incomplete bladder emptying or urge incontinence from neurological conditions. These less common forms require medical evaluation before using pelvic floor trainers, as they may need different interventions addressing the underlying causes rather than muscle strengthening alone.
The severity of incontinence also influences device selection. Women with occasional minor leakage during intense exercise may achieve excellent results with biofeedback-only devices. Those experiencing frequent leakage during everyday activities often benefit from electrical stimulation. Severe incontinence involving significant volume loss typically requires aggressive electrical stimulation combined with comprehensive lifestyle modifications.
Age-related factors affect response to device training. Younger women with recent-onset incontinence often respond quickly, achieving noticeable improvement within 4-6 weeks. Older women with long-standing incontinence may require 12-16 weeks to experience substantial benefits as they rebuild severely deconditioned muscles.
What the data says: Research demonstrates that 60-70% of women achieve satisfactory improvement with device training, with combined approaches producing superior outcomes for mixed incontinence compared to single-modality treatments according to the 2024 Cochrane overview (PubMed 36053030).
How Do You Choose Between EMS and Biofeedback Devices?
Your current pelvic floor muscle strength level represents the most important factor in device selection. Women with significant muscle weakness—those who cannot voluntarily contract their pelvic floor muscles at all or can barely detect movement—benefit more from electrical muscle stimulation that does the contraction work for them. A device like Yarlap that automatically stimulates muscles helps rebuild foundational strength before progressing to active exercises.
Women with moderate muscle strength who can perform some voluntary contractions but lack consistency or proper technique benefit from biofeedback devices. The Elvie Trainer excels in this category, providing clear visual feedback that helps refine exercise form while building on existing muscle capability. The interactive app guides progression from basic to advanced exercises as strength improves.
Combined devices like the Perifit Care+ offer the best of both worlds, making them ideal for mixed incontinence or women unsure of their muscle strength level. Starting with electrical stimulation to build baseline strength and transitioning to biofeedback-guided active exercises as capability improves provides a complete rehabilitation pathway.
Budget constraints influence many decisions. The K-Goal Incontinence Stimulator delivers essential electrical stimulation functionality at $114, making evidence-based device training accessible to women who cannot afford premium options. While it lacks the sophisticated app features of higher-priced devices, it provides the core electrical stimulation shown effective in clinical research.
Technology comfort level matters for long-term adherence. Some women prefer the simplicity of Yarlap’s pre-programmed sessions that require minimal interaction—insert the probe, select an intensity level, and let the device work for 20 minutes. Others enjoy the interactive gaming approach of Perifit Care+ that makes training sessions feel more like play than medical therapy.
Privacy concerns vary individually. All reviewed devices connect to smartphone apps that may store training data. While this enables progress tracking and personalized recommendations, women prioritizing data privacy should review each manufacturer’s privacy policy. Devices can typically function without app connectivity if preferred, though this limits access to advanced features.
The severity and type of your incontinence symptoms also guide device selection. Pure stress incontinence often responds well to either electrical stimulation or biofeedback. Urgency incontinence shows better response to electrical stimulation that modulates neural pathways. Mixed incontinence benefits most from devices offering both technologies.
Your daily schedule and lifestyle affect which devices fit seamlessly into your routine. Busy professionals may prefer Elvie Trainer’s quick 5-minute sessions that fit into lunch breaks. Women with more flexible schedules might appreciate Yarlap’s thorough 20-minute automated sessions that allow completely hands-free training while reading or relaxing.
Physical factors including probe size preferences, sensitivity to electrical stimulation, and anatomical variations influence comfort and effectiveness. Reading user reviews from women with similar characteristics helps identify which devices work well for specific anatomies and sensitivity levels.
The research verdict: A 2025 meta-analysis of 7 RCTs comprising 411 women shows supervised exercises outperform unsupervised attempts, but device-based training bridges this gap by providing structured guidance through apps and automatic programs (PubMed 39467254).
How Often Should You Use a Pelvic Floor Trainer?
Research protocols showing clinical effectiveness typically employ 2-3 sessions per week during the initial 8-12 week training phase. A 2012 Cochrane review examining pelvic floor muscle training during pregnancy and postpartum found that programs using 3 weekly sessions produced significant reductions in incontinence prevalence and symptom severity.8
Session duration depends on device type and training mode. Electrical stimulation sessions typically last 20-30 minutes based on the time required for adequate muscle fatigue and neural modulation effects. Biofeedback sessions can be shorter—5-15 minutes—since active voluntary contractions fatigue muscles more quickly than passive electrical stimulation.
The Perifit Care+ recommends 10-20 minute sessions 3-5 times weekly, alternating between electrical stimulation and biofeedback modes based on your personalized program. Yarlap uses 20-minute automatic sessions 2-3 times weekly. The Elvie Trainer offers 5-minute workout sessions designed for daily use, with the shorter duration encouraging more frequent engagement.
Intensity matters more than duration. Quality muscle contractions—whether stimulated electrically or performed voluntarily with biofeedback—trigger the strength adaptations that improve incontinence. A focused 15-minute session performed correctly produces better results than a distracted 30-minute session with poor form or inadequate intensity.
Progressive overload principles apply to pelvic floor training just like other muscle strengthening. Starting at comfortable intensity levels and gradually increasing resistance, contraction duration, or complexity over weeks ensures continued adaptation. Devices with app-based programs automatically adjust difficulty based on performance, which helps avoid training plateaus.
Rest days allow muscle recovery and adaptation. Training pelvic floor muscles daily without rest can lead to fatigue that temporarily worsens incontinence symptoms. The 2-3 sessions per week recommended in most research provides training stimulus while allowing adequate recovery between sessions.
Many women wonder whether more frequent training accelerates results. Current evidence suggests that exceeding 3-4 weekly sessions provides minimal additional benefit while increasing risk of muscle fatigue and overtraining. The muscles need recovery time to synthesize new contractile proteins and strengthen neural connections formed during training.
Timing your sessions around your menstrual cycle may optimize results. Some research suggests that pelvic floor muscles respond differently during different cycle phases due to hormonal fluctuations. While this remains an area of ongoing investigation, many women report that training feels easier during the follicular phase (days 1-14) compared to the luteal phase.
Consistency trumps intensity when establishing new training habits. Starting with very manageable 10-minute sessions three times weekly that you can sustain long-term produces better outcomes than ambitious daily 30-minute sessions that become overwhelming after two weeks.
In practice: Research protocols showing clinical effectiveness employ 2-3 sessions of 20-30 minutes weekly for 8-12 weeks during intensive training, then reduce to 1-2 weekly maintenance sessions (PubMed 23365417).
Can Pelvic Floor Trainers Help After Childbirth?
Postpartum pelvic floor rehabilitation represents one of the most evidence-supported applications for device training. The 2024 systematic review on conservative interventions for postpartum urinary incontinence found that electrical stimulation and pelvic floor muscle training significantly reduce incontinence prevalence when initiated within the first year after delivery.9
Timing matters for postpartum use. Most providers recommend waiting until after the standard 6-8 week postpartum checkup to begin using intravaginal devices, allowing adequate recovery of vaginal tissues. Women who had significant perineal tearing, cesarean complications, or other delivery-related injuries may need additional recovery time before starting device training.
A 2024 systematic review specifically examining non-pharmacological approaches for postpartum stress incontinence found that pelvic floor muscle training with or without electrical stimulation produced significant improvements in continence rates, with earlier intervention correlating with better long-term outcomes.10 Starting rehabilitation within 3-6 months postpartum appears more effective than waiting until incontinence becomes chronic.
The mechanism of postpartum incontinence combines muscle stretching, nerve compression, and connective tissue damage during delivery. Devices providing both electrical stimulation and biofeedback address multiple aspects: electrical stimulation reactivates muscles that may have partial nerve damage, while biofeedback helps relearn proper contraction patterns after anatomical changes.
Breastfeeding women can safely use pelvic floor trainers—the devices affect only local muscles and nerves without systemic effects that would impact milk production or quality. However, postpartum hormonal changes keep tissues more elastic and potentially more sensitive, so starting with lower intensity settings and gradually increasing as tissues adapt helps minimize discomfort.
Multiple births increase incontinence risk and may require longer rehabilitation timelines. The cumulative stretching and stress from multiple pregnancies often causes more significant muscle weakness requiring more intensive training. Devices offering adjustable intensity levels accommodate the greater weakness while providing room for progressive strengthening.
Vaginal delivery versus cesarean section influences postpartum pelvic floor status differently. Vaginal delivery creates more immediate structural changes including potential nerve compression and muscle stretching. However, pregnancy itself—regardless of delivery method—stresses pelvic floor structures through nine months of increased weight bearing. Both groups benefit from postpartum pelvic floor rehabilitation, though those with vaginal deliveries may have more severe initial weakness.
The emotional and psychological aspects of postpartum recovery affect adherence to rehabilitation programs. New mothers face overwhelming demands on their time and energy. Devices offering short session durations (5-15 minutes) and requiring minimal setup fit more realistically into postpartum life than complex protocols demanding extensive time commitments.
Pelvic floor rehabilitation integrates naturally with other postpartum recovery priorities including abdominal muscle restoration and diastasis recti recovery. Many women combine pelvic floor device training with gentle core exercises, creating comprehensive postpartum fitness programs addressing multiple recovery goals simultaneously.
The practical takeaway: The 2024 systematic review shows starting within 3-6 months postpartum produces better outcomes than delayed intervention, requiring 6-8 week provider clearance before beginning with gentle settings (PubMed 39943628).
What About Using Devices During Perimenopause and Menopause?
Estrogen decline during perimenopause and menopause affects pelvic floor tissues, causing muscle atrophy, reduced connective tissue elasticity, and vaginal tissue thinning that can worsen incontinence. Device-based training becomes even more important during this life phase as hormonal changes accelerate muscle weakness.
The 2023 systematic review on pelvic floor physiotherapy for stress incontinence in postmenopausal women demonstrated significant improvements in incontinence severity, quality of life, and pelvic floor muscle strength with supervised training programs.7 While that study focused on supervised therapy, the findings support device use at home for women who cannot access regular physiotherapy appointments.
Vaginal tissue sensitivity increases during menopause as estrogen levels drop. Starting with lower electrical stimulation intensities and ensuring adequate lubrication helps avoid discomfort that might discourage continued use. Water-based lubricants work well with all reviewed devices and don’t interfere with electrical conductivity or pressure sensors.
Some women benefit from combining device training with topical vaginal estrogen therapy when medically appropriate. Low-dose vaginal estrogen improves tissue health without significant systemic absorption, potentially enhancing response to pelvic floor training. This decision requires consultation with a healthcare provider considering individual health history.
The K-Goal Incontinence Stimulator offers particular value for postmenopausal women on fixed incomes who need effective training without premium pricing. Its combination of electrical stimulation and basic biofeedback provides core functionality at an accessible price point, addressing both muscle weakness and exercise technique.
Maintenance training becomes especially important after menopause since muscle loss accelerates without estrogen’s protective effects. Transitioning to a long-term maintenance schedule using devices 1-2 times weekly helps preserve strength gains achieved during initial intensive training.
Women navigating menopause often experience multiple pelvic floor symptoms simultaneously. Incontinence may coexist with pelvic organ prolapse, vaginal dryness, painful intercourse, and reduced sexual satisfaction. Comprehensive pelvic floor rehabilitation addressing muscle strength, tissue health, and neural function can improve this entire symptom cluster.
The psychological impact of incontinence often intensifies during menopause. Women already managing hot flashes, sleep disruptions, mood changes, and body image concerns find that incontinence adds another layer of distress. Effective device training that genuinely reduces symptoms provides meaningful quality of life improvements during a challenging transition.
Bone density concerns during menopause indirectly relate to pelvic floor health. Maintaining healthy weight and engaging in weight-bearing exercise support both bone health and pelvic floor function. Our comprehensive guide to magnesium supplementation for women over 40 addresses this intersection of bone health and overall wellness during perimenopause and beyond.
Broader hormonal support during this transition comes from multiple angles. Our perimenopause supplement recommendations provide complementary nutritional strategies supporting overall health during hormonal changes.
Clinical insight: The 2023 systematic review on postmenopausal women demonstrates significant improvements in incontinence severity with pelvic floor training, requiring lower initial electrical stimulation intensities (PubMed 35831758).
How Do Professional Physical Therapists Use These Devices?
Pelvic floor physical therapists incorporate electrical stimulation and biofeedback devices into comprehensive treatment protocols that include manual therapy, specific exercise prescription, and education about bladder habits and lifestyle factors affecting incontinence. A typical initial physiotherapy session includes internal examination to assess muscle strength, identify areas of tension or weakness, and evaluate coordination.
Therapists use biofeedback during sessions to teach proper muscle isolation. Many women unknowingly contract abdominal, gluteal, or inner thigh muscles when attempting Kegels, creating downward rather than upward pelvic floor movement. Real-time biofeedback helps therapists demonstrate the difference between correct and incorrect techniques, accelerating the learning process.
Electrical stimulation serves different roles in clinical settings. For women with severe weakness unable to voluntarily contract muscles, therapists may use electrical stimulation during sessions to “wake up” dormant muscle fibers and help patients recognize what a proper contraction feels like. Once patients can perform some voluntary contractions, the focus shifts to biofeedback-guided active exercises.
Treatment protocols typically combine in-office sessions with home training programs. After learning proper technique with professional guidance, women continue training at home using devices like those reviewed here. The Perifit Care+ and Elvie Trainer apps provide structure between therapy appointments, while simpler devices like Yarlap offer automated stimulation requiring minimal technique knowledge.
Research comparing supervised physiotherapy to unsupervised home device use shows advantages for professional guidance, but accessibility and cost limitations make in-person therapy impractical for many women. The 2025 meta-analysis on electrical stimulation versus active training found that unsupervised home exercise performed worse than supervised therapy, but device-based training bridged this gap by providing structured guidance through apps and automatic programs.5
Insurance coverage for pelvic floor physiotherapy varies significantly by location and policy. Many women start with a few physiotherapy sessions to learn proper technique and assess their specific issues, then continue long-term training at home with devices. This hybrid approach balances professional expertise with practical sustainability.
Physical therapists individualize treatment based on assessment findings. Some women need manual therapy releasing tight muscles before strengthening weak ones. Others require education about bladder training or dietary modifications alongside device use. Comprehensive assessment ensures device training addresses root causes rather than just symptoms.
Therapists monitor progress through objective measures including pad weight tests, symptom diaries, and validated questionnaires assessing quality of life impact. These metrics help determine when to advance training intensity, modify techniques, or consider additional interventions if progress plateaus.
The therapeutic relationship provides accountability and motivation that devices alone cannot offer. Regular check-ins with a therapist help women stay committed to home training programs during the challenging weeks before symptoms noticeably improve. This support significantly affects long-term adherence and outcomes.
What this means: Starting with 3-5 physiotherapy sessions provides technique education, followed by home training with devices showing comparable outcomes to continued supervised therapy in 411 women studied (PubMed 39467254).
Perifit Care+ Review: Best Overall for Comprehensive Training
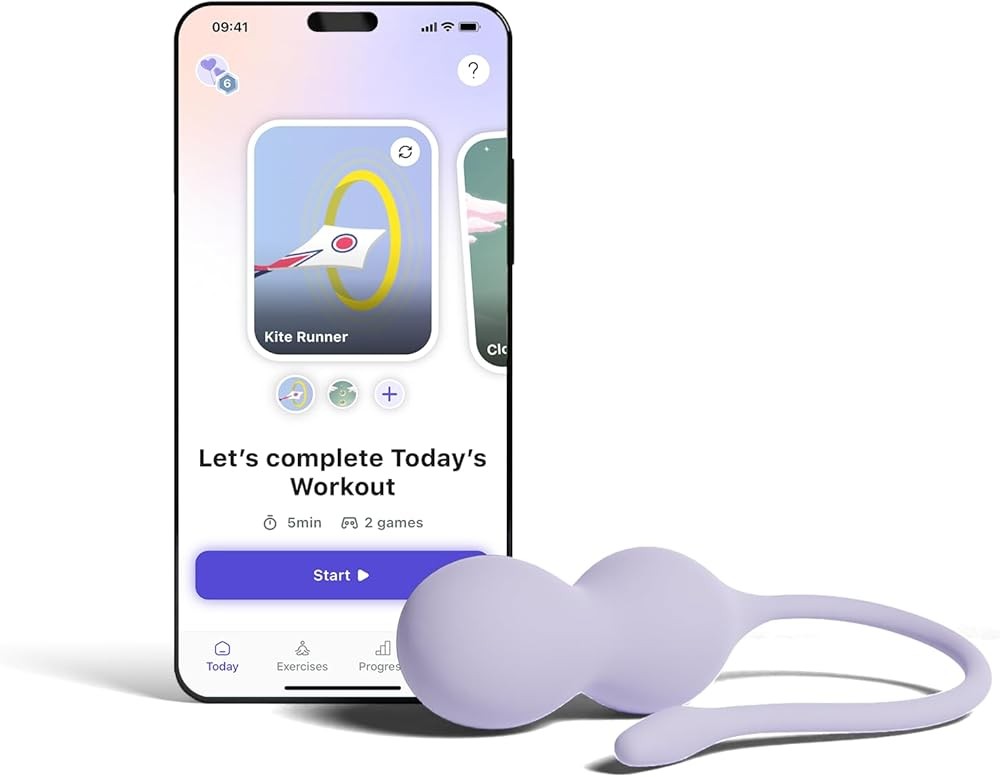
The Perifit Care+ combines electrical muscle stimulation, biofeedback pressure sensing, and interactive smartphone gaming into a comprehensive incontinence management system. The FDA-cleared device uses a medical-grade silicone probe containing both pressure sensors for biofeedback and electrodes for electrical stimulation, controlled through a Bluetooth-connected app offering personalized programs.
The dual-mode functionality addresses different training needs throughout your rehabilitation journey. During electrical stimulation sessions, the device delivers programmed muscle contractions that strengthen muscles even if you cannot voluntarily contract them effectively. Switching to biofeedback mode for active training, pressure sensors measure your contractions and translate them into game controls where squeezing makes a character fly higher or move faster.
Personalization sets Perifit Care+ apart from basic devices. After an initial assessment where the app tests your maximum contraction strength and endurance, it creates a customized program matching your baseline capability and specific incontinence pattern. Programs adapt as you progress, automatically increasing difficulty to maintain training stimulus without overwhelming weakened muscles.
The app library includes multiple games that help maintain engagement during the recommended 3-5 weekly sessions. Some games focus on sustained contractions developing endurance, while others emphasize quick flicks training the rapid response needed when coughing or sneezing. This variety ensures comprehensive muscle development across different contraction patterns.
Session length flexibility accommodates busy schedules. Electrical stimulation sessions typically run 15-20 minutes, while biofeedback games can be completed in 10 minutes. The app tracks progress over weeks and months, showing improvements in contraction strength, endurance, and incontinence episodes reported through the built-in symptom diary.
The premium price of $179 reflects the advanced technology and comprehensive features. For women wanting the most complete at-home training system with both active and passive training modes, Perifit Care+ offers exceptional value considering the cost of ongoing physiotherapy sessions.
Build quality meets high standards with seamless medical-grade silicone that cleans easily and withstands repeated use. The rechargeable battery eliminates ongoing costs for disposable batteries. Battery life typically provides 5-7 training sessions per charge, and the included USB cable works with any standard phone charger.
Customer support receives consistently positive reviews, with responsive assistance for setup questions or technical issues. The two-year warranty provides confidence in long-term reliability and protects your investment against manufacturing defects.
The learning curve for mastering all app features takes a few sessions. Some users report initial confusion navigating between electrical stimulation and biofeedback modes or understanding which games target which muscle training goals. However, the comprehensive tutorial and in-app guidance help most users become comfortable within their first week.
Here’s what matters: Perifit Care+ combines electrical stimulation at clinical frequencies with biofeedback pressure sensing at $179, offering 10-20 minute personalized sessions 3-5 times weekly through FDA-cleared medical-grade silicone probe with 2-year warranty.
Yarlap Review: Best for Severe Incontinence
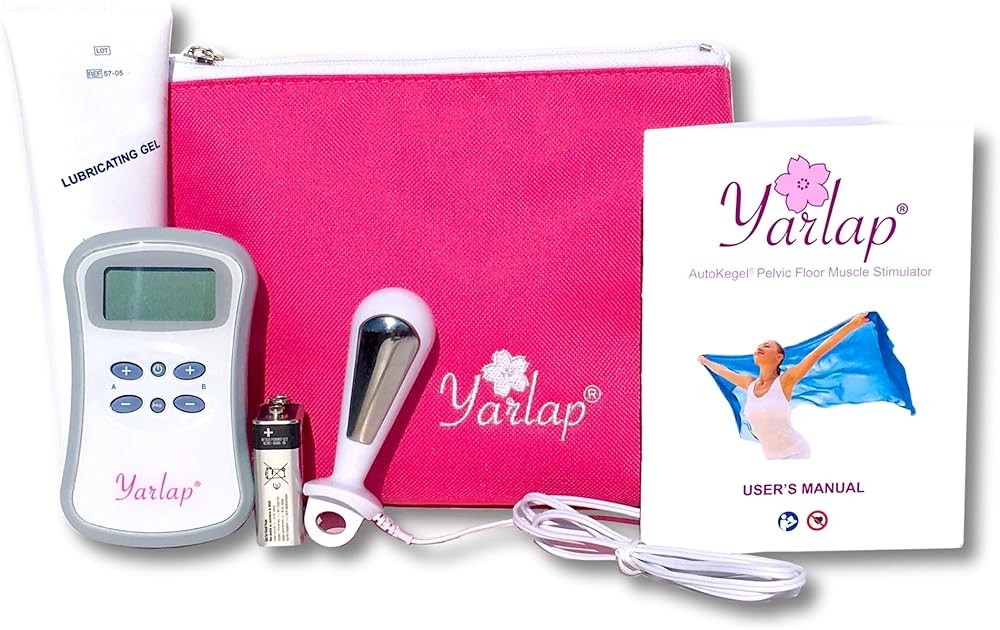
Yarlap delivers physician-designed automatic electrical stimulation specifically engineered for women with significant pelvic floor weakness who struggle to perform any voluntary contractions. The hands-free system requires only inserting the probe, selecting one of six intensity levels, and relaxing for 20 minutes while the device delivers programmed muscle contractions.
The automation benefits women overwhelmed by complicated training protocols or those whose muscle weakness makes effective voluntary exercises challenging. Yarlap’s pre-programmed sequences automatically vary contraction duration and rest periods throughout each session, mimicking the progressive patterns used in clinical electrical stimulation protocols.
The six intensity levels accommodate different weakness severities and progression over time. Starting at level 1 provides gentle stimulation that feels like a subtle tingle, while level 6 delivers strong contractions producing visible pelvic floor movement. Gradually increasing intensity as muscles adapt ensures continued strengthening stimulus without the plateau effect that can occur with static programs.
Simplicity makes Yarlap particularly appropriate for older users or those uncomfortable with technology. No smartphone apps, Bluetooth connections, or complex settings—just select your level and press start. This straightforward approach eliminates technical barriers that might keep some women from benefiting from evidence-based electrical stimulation.
The medical-grade silicone probe measures slightly larger than some competitors, which some users find more comfortable for maintaining position during automatic contractions, while others prefer smaller profiles. The size difference is minimal but worth considering based on individual anatomy and comfort preferences.
At $299, Yarlap represents the premium price category. The cost reflects the clinical-grade electrical stimulation technology and physician-involved design process. For women with severe incontinence who have failed traditional exercises and want a powerful automated solution, the investment may prove worthwhile considering potential improvements in quality of life.
The one-year warranty is shorter than some competitors, and replacement probes cost approximately $89, representing an ongoing expense if the probe requires replacement. However, the durable construction and simple design with few breakable components often results in multi-year use without issues.
User reviews consistently mention the powerful muscle contractions produced even at moderate intensity levels. Women who had previously tried other devices without success often report finally feeling their pelvic floor muscles engage strongly with Yarlap. This effectiveness for severe weakness justifies its position as the top choice in this category.
The lack of biofeedback or active training modes means Yarlap addresses only the electrical stimulation component of comprehensive rehabilitation. Women using Yarlap may want to eventually supplement with biofeedback training once they rebuild sufficient strength to perform voluntary contractions.
Our verdict: Yarlap delivers physician-designed automated electrical stimulation through 6 pre-programmed intensity levels during 20-minute hands-free sessions at $299, specifically engineered for severe muscle weakness requiring automatic rather than voluntary contractions.
K-Goal Incontinence Stimulator Review: Best Budget Option

K-Goal Incontinence Stimulator
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The K-Goal Incontinence Stimulator delivers core electrical muscle stimulation functionality at an accessible $114 price point, making evidence-based device training available to budget-conscious women who might otherwise skip this proven intervention. The FDA-registered device combines electrical stimulation with basic biofeedback capability through a simple smartphone app.
The electrical stimulation functionality matches more expensive devices in providing adjustable intensity levels that deliver therapeutic muscle contractions. Users manually adjust intensity through the app to find their optimal training level, which requires more active involvement than Yarlap’s pre-programmed levels but offers fine-tuned control.
Basic biofeedback capability adds value beyond electrical stimulation alone. The app displays contraction strength during active exercises, helping you confirm you’re isolating the correct muscles and tracking improvement over time. While less sophisticated than Perifit Care+’s interactive games, the simple bar graphs provide effective visual feedback.
The rechargeable design eliminates ongoing battery costs that add up with disposable battery devices. A full charge typically provides 6-8 training sessions, and the included USB charging cable works with any standard phone charger. This convenience factor increases real-world adherence by removing barriers to regular use.
Session flexibility allows customizing training to your schedule and capability. Shorter 15-minute sessions work well for women just starting training or with limited time, while extending to 30 minutes provides more intensive training as strength improves. The ability to adjust both session length and intensity accommodates wide-ranging individual needs.
The compromise for the lower price appears in the app interface quality and lack of advanced features like personalized programs, comprehensive progress tracking, or adaptive difficulty adjustment. However, the core functionality—electrical stimulation that strengthens muscles and basic feedback confirming proper technique—remains intact.
Build quality meets FDA safety standards with medical-grade materials and proper electrical isolation. Some users report the probe feeling slightly less substantial than premium options, but reliability appears solid based on user reviews. The one-year warranty provides reasonable protection for the budget price point.
The K-Goal works particularly well for women wanting to try device-based training without committing to premium-priced options. If pelvic floor training becomes a long-term health practice, you can always upgrade to more feature-rich devices later. Starting with K-Goal lets you determine whether electrical stimulation helps your specific symptoms before investing heavily.
Setup and use remain straightforward. Download the app, charge the device, apply water-based lubricant, insert the probe, and select your training mode and intensity. The simplified approach makes K-Goal accessible even for women who feel intimidated by health technology.
The value assessment: K-Goal provides FDA-registered electrical stimulation with basic biofeedback at $114 budget price, offering 15-30 minute rechargeable sessions with manual intensity adjustment delivering core therapeutic functionality from research protocols.
Elvie Trainer Review: Best for App Tracking and Active Training
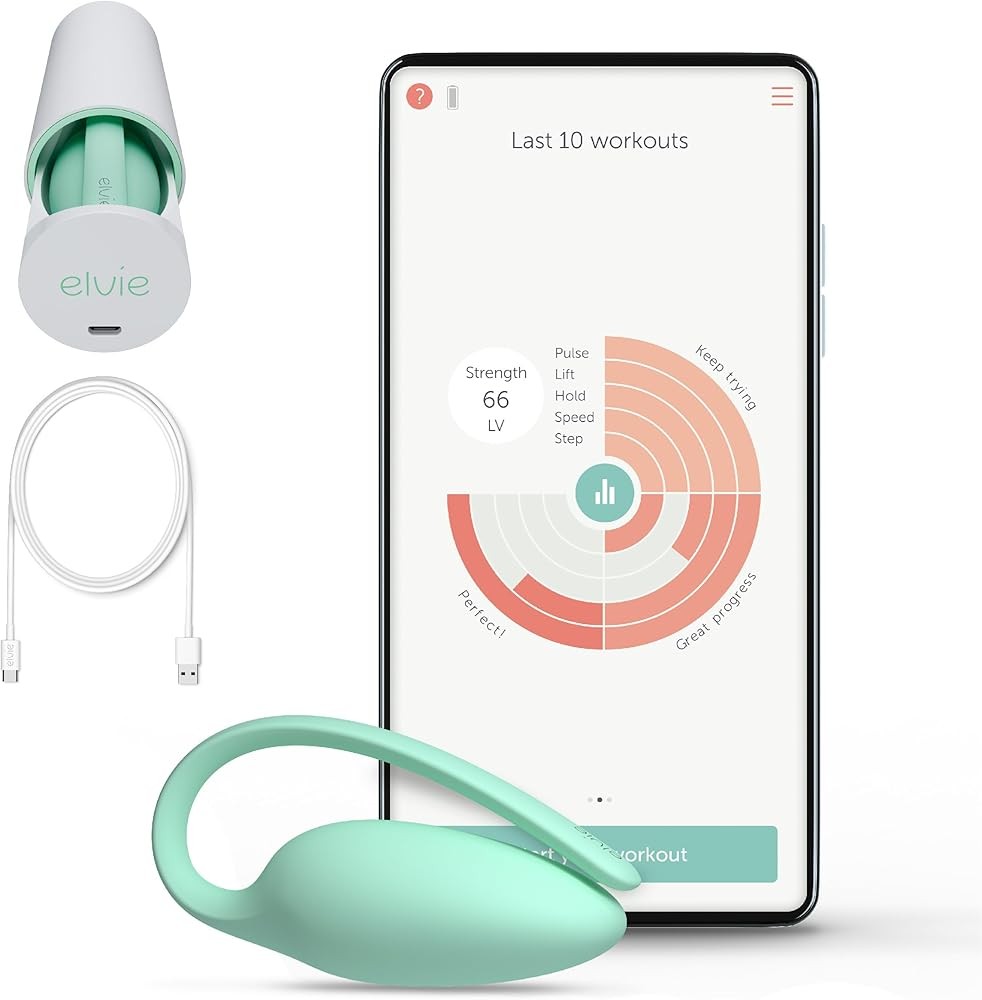
The Elvie Trainer represents the premium end of biofeedback-only devices, offering sophisticated app-based training programs without electrical stimulation. The award-winning design combines precision pressure sensing with an intuitive app featuring guided workouts, comprehensive progress tracking, and personalized training plans.
The biofeedback-only approach suits women with moderate muscle strength who can perform voluntary contractions but need guidance refining technique and progressively challenging workouts. If you cannot contract your pelvic floor muscles at all, electrical stimulation devices like Yarlap or Perifit Care+ provide better starting points.
The app experience sets Elvie apart. Five-minute guided workout sessions walk you through warm-up, training, and cool-down phases with clear visual and audio cues. The interface shows real-time contraction strength, helping you learn to control both contraction intensity and release completeness—many women struggle to fully relax pelvic floor muscles between contractions.
Six different workout types target different training goals. Pulse training develops quick-response strength needed for sudden pressure events like coughing. Hold training builds endurance for maintaining muscle tone throughout daily activities. The variety ensures comprehensive muscle development rather than repetitive single-pattern training.
Progress tracking transforms abstract muscle strengthening into concrete measurable achievements. The app records each session, displaying trends in contraction strength and endurance over weeks. Seeing quantifiable improvement motivates continued adherence and helps identify when to advance to more challenging programs.
The premium build quality shows in details like the ergonomic probe shape, seamless medical-grade silicone surface, and compact size fitting discreetly in your gym bag. The rechargeable design charges via USB, and battery life supports approximately one month of regular use per charge.
At $199, Elvie Trainer costs more than basic biofeedback devices while lacking the electrical stimulation capability of combination units. The price reflects superior app development, elegant industrial design, and the brand’s reputation for quality women’s health products. The two-year warranty provides confidence in long-term reliability.
The limitation to biofeedback-only training means Elvie Trainer may not suffice for severe muscle weakness. However, for motivated women who can perform basic Kegels and want to perfect technique while progressing through well-designed training programs, the exceptional app experience justifies the premium.
Customer reviews frequently mention how the 5-minute session length makes daily training realistic even during busy schedules. Unlike 20-30 minute sessions that require dedicated time blocks, squeezing in a quick Elvie workout during lunch or before bed feels manageable long-term.
The sleek minimalist design appeals to women who appreciate thoughtful product aesthetics. Elvie doesn’t look like a medical device—it resembles a premium tech accessory. For some users, this design sensibility increases comfort using the device and displaying it if needed.
The science says: Elvie Trainer offers premium biofeedback through 6 workout types in 5-minute sessions at $199, with precision pressure sensing, month-long battery life, and 2-year warranty ideal for women with moderate existing muscle strength.
What About Combining Device Training With Other Interventions?
Research consistently shows that multimodal approaches addressing incontinence from multiple angles produce superior outcomes compared to single interventions. Device-based pelvic floor training combines naturally with several complementary strategies that enhance overall effectiveness.
Bladder training techniques help reduce urgency symptoms by gradually increasing the time between bathroom visits. A 2024 systematic review on bladder training for overactive bladder found that scheduled voiding combined with urge suppression strategies significantly reduced urgency episodes and improved bladder capacity.11 Using bladder training alongside device-based muscle strengthening addresses both muscle weakness and bladder hypersensitivity.
Lifestyle modifications impact incontinence severity through multiple mechanisms. Reducing caffeine and alcohol intake decreases bladder irritation. Maintaining healthy body weight reduces intra-abdominal pressure stressing pelvic floor muscles—research shows that every 5-unit increase in BMI correlates with approximately 20-70% increased incontinence risk. Avoiding constipation reduces chronic straining that weakens pelvic support structures.
Fluid management requires balance. Some women drastically reduce fluid intake hoping to minimize leakage, which paradoxically worsens urgency by creating concentrated urine that irritates the bladder. Drinking adequate fluids throughout the day while avoiding large volumes before bed optimizes bladder health without triggering urgency.
Pessary devices inserted by healthcare providers provide mechanical support for pelvic organ prolapse that often coexists with incontinence. While pessaries don’t strengthen muscles, they can reduce leakage enough to allow more comfortable device training. Some women use pessaries during high-impact activities while relying on strengthened muscles for everyday continence.
Vaginal moisturizers and lubricants support tissue health during device use, especially for postmenopausal women experiencing vaginal dryness. Regular use of vaginal moisturizers several times weekly improves tissue elasticity independent of device training, while water-based lubricants applied before each training session ensure comfort without interfering with sensors or electrodes.
Dietary modifications influence bladder irritation and urgency. Common bladder irritants include citrus fruits, tomatoes, spicy foods, artificial sweeteners, and carbonated beverages. Keeping a food-symptom diary helps identify personal triggers worth reducing or eliminating.
Timed voiding schedules teach bladder retraining by gradually extending intervals between bathroom visits. Starting with comfortable intervals (perhaps every 90 minutes) and slowly increasing by 15-minute increments helps rebuild bladder capacity and reduces urgency over weeks.
Core strengthening exercises complement pelvic floor training. Strong abdominal muscles provide additional support for pelvic organs and help manage intra-abdominal pressure during activities like lifting. However, traditional abdominal exercises like crunches can worsen pelvic floor dysfunction if performed incorrectly, so learning proper technique matters.
Pelvic floor stretching and relaxation techniques help women with hypertonicity—excessively tight muscles that never fully relax. Foam rolling, gentle yoga poses opening the hips, and specific stretches taught by pelvic floor physical therapists complement strengthening exercises for comprehensive muscle health.
Research summary: Research shows every 5-unit BMI increase correlates with 20-70% increased incontinence risk, making combined device training, bladder training, lifestyle modifications, and dietary changes more effective than single interventions (PubMed 39978852).
How Do You Maintain Results Long-Term?
Achieving initial improvements represents only the first phase of successful incontinence management. Research on long-term outcomes shows that continued maintenance exercise helps avoid regression to baseline weakness levels. A practical maintenance program balances ongoing device use with integrated daily exercises.
Most studies showing sustained benefits employ maintenance protocols using device training 1-2 times weekly after completing initial intensive phases. This reduced frequency avoids muscle deconditioning while requiring less time commitment than the 3-5 weekly sessions needed during initial training. The specific schedule depends on individual response and symptom stability.
Daily functional Kegels integrated into routine activities reinforce muscle memory without dedicated training sessions. Contracting pelvic floor muscles during predictable pressure events—before coughing, sneezing, or lifting—provides constant practice applying muscle control in real-world situations. These functional exercises complement rather than replace device training.
Periodic reassessment helps optimize maintenance programs. Using device biofeedback monthly to test maximum contraction strength and endurance reveals whether current maintenance intensity suffices or requires adjustment. Gradually declining strength signals need for temporarily increased training frequency before significant regression occurs.
Life changes requiring program adjustments include pregnancy, significant weight changes, new medications affecting muscle tone or bladder function, hormonal transitions like menopause, or surgeries impacting pelvic anatomy. Recognizing these transitions as opportunities to modify your maintenance program helps avoid setbacks.
Some women find that alternating between different devices maintains engagement over years. Using Perifit Care+ games for 2-3 months, switching to Elvie Trainer workouts for variety, then returning to electrical stimulation sessions keeps training fresh. The underlying muscle strengthening occurs regardless of specific device, so variety supporting long-term adherence matters more than device loyalty.
Annual check-ins with pelvic floor physical therapists provide professional assessment confirming maintenance programs remain appropriate. Even a single session every 12-18 months helps catch technique drift, identify new muscle imbalances, and adjust programs for optimal long-term outcomes.
Tracking symptoms through simple diaries or app-based logs helps identify early signs of regression. Noticing increased leakage frequency or volume during specific activities signals need for temporarily intensified training before symptoms worsen significantly.
Many women report that after 6-12 months of consistent training and symptom improvement, pelvic floor exercises become habitual—integrated seamlessly into daily routines like brushing teeth. This habituation represents the ultimate success, transforming pelvic floor health from a temporary project into a sustainable lifelong practice.
What the data tells us: Studies showing sustained benefits employ 1-2 device sessions weekly for maintenance after the 8-12 week intensive phase, supplemented with daily functional Kegels during pressure events to reinforce muscle memory.
When Should You Consult a Healthcare Provider?
While home device training helps many women, certain situations require professional medical evaluation before beginning or during training. Consulting healthcare providers ensures safe and appropriate intervention selection while identifying conditions needing additional treatment.
Severe incontinence involving large-volume leakage, complete emptying during stress events, or constant wetness requires medical evaluation ruling out anatomical damage, neurological conditions, or severe prolapse potentially benefiting from surgical intervention. Device training may still help, but should complement rather than replace comprehensive medical assessment.
Worsening symptoms despite consistent device use for 12-16 weeks suggests underlying issues beyond simple muscle weakness. Possible explanations include unrecognized pelvic organ prolapse, urinary tract abnormalities, neurological conditions affecting bladder control, or medication effects. Medical evaluation identifies these factors and guides appropriate modifications.
Pelvic pain during device use beyond expected muscle fatigue requires professional assessment. While mild muscle soreness similar to post-workout sensation is normal, sharp pain, cramping, or discomfort persisting after sessions may indicate pelvic floor hypertonicity—excessive muscle tension—requiring manual therapy and relaxation techniques rather than strengthening exercises.
Blood in urine, painful urination, or signs of urinary tract infection demand immediate medical attention. Training should pause until infections resolve completely. Recurrent urinary tract infections sometimes relate to incomplete bladder emptying or post-void residual urine requiring medical management.
Pregnancy and recent childbirth require provider clearance before beginning device training. Most obstetricians recommend waiting until after the 6-8 week postpartum checkup to ensure adequate recovery. Pregnant women should only use devices under healthcare provider supervision, as electrical stimulation during pregnancy requires careful consideration of individual circumstances.
Pre-existing medical conditions including pacemakers, implantable defibrillators, epilepsy, active vaginal infections, or cancer require provider consultation before using electrical stimulation devices. Most conditions allow safe device use with proper precautions, but individual assessment ensures appropriate safety measures.
Neurological conditions including multiple sclerosis, spinal cord injuries, or stroke affecting bladder control need specialized evaluation. While pelvic floor training may help as part of comprehensive neurogenic bladder management, these complex conditions require medical oversight.
New or worsening pelvic organ prolapse symptoms including vaginal bulging, pressure, or the sensation of something falling out warrant examination. Significant prolapse may require pessary support or surgical intervention before device training can effectively address incontinence.
Red flags requiring medical evaluation: Severe or worsening incontinence despite device use, pelvic pain beyond muscle soreness, blood in urine, recurrent infections, prolapse symptoms, or any pre-existing medical conditions that might contraindicate electrical stimulation.
Complete Support System: What Else Your Pelvic Floor Needs
Beyond device training, comprehensive pelvic floor health requires attention to multiple supporting factors. Nutrition impacts muscle function and tissue health through mechanisms ranging from protein synthesis to connective tissue integrity.
Adequate protein intake supports muscle repair and growth following training sessions. The recommended dietary allowance of 0.8 grams per kilogram body weight represents minimum needs, while active individuals benefit from 1.2-1.6 g/kg supporting muscle development. Quality protein sources throughout the day ensure amino acid availability when muscles synthesize new contractile proteins after training.
Magnesium influences muscle contraction and relaxation cycles while supporting nerve function. Many women consume inadequate dietary magnesium, with surveys showing 48% of Americans failing to meet estimated average requirements. Our comprehensive guide to magnesium supplementation for women over 40 details optimal forms and dosing supporting muscle function during perimenopause and beyond.
Vitamin D status affects muscle strength throughout the body including pelvic floor muscles. Observational studies link vitamin D deficiency to increased pelvic floor disorders, though causation remains unproven. Maintaining optimal vitamin D levels through sun exposure, diet, and supplementation when needed supports overall muscle health.
Collagen and connective tissue nutrients including vitamin C, zinc, and copper support the fascial layers and ligaments providing structural support to pelvic organs. While collagen supplementation’s benefits for pelvic floor connective tissue lack direct research, broader studies on connective tissue health suggest potential value.
Hydration affects muscle function and urine concentration. Paradoxically, inadequate hydration creates concentrated urine irritating the bladder and potentially worsening urgency symptoms. Consistent fluid intake throughout the day maintains optimal urine dilution while avoiding large volumes before bed that increase nighttime incontinence.
Stress management deserves attention because chronic stress increases muscle tension throughout the body including pelvic floor muscles. Some women develop pelvic floor hypertonicity from chronic tension, creating paradoxical weakness—muscles that cannot contract effectively because they never fully relax. Mind-body practices including gentle yoga, meditation, and diaphragmatic breathing support pelvic floor relaxation.
Our broader women’s health content addresses hormonal factors affecting pelvic floor health. The perimenopause supplement guide covers nutritional support during the transition when estrogen decline impacts pelvic tissues.
Sleep quality influences muscle recovery and overall health. Growth hormone secreted during deep sleep stages facilitates muscle repair after training. Poor sleep undermines training adaptations regardless of program quality.
Omega-3 fatty acids from fish oil or algae supplements support general anti-inflammatory processes that may benefit pelvic floor tissue health. While specific research on omega-3s for incontinence is limited, their broader anti-inflammatory effects support tissue recovery.
B vitamins including B12, folate, and B6 support nerve function throughout the body. Since pelvic floor function depends on intact neural pathways between brain and muscles, adequate B vitamin status supports optimal neuromuscular communication.
Nutritional foundation: Protein intake of 1.2-1.6 g/kg body weight supports muscle synthesis, while 48% of Americans consume inadequate magnesium affecting muscle contraction and relaxation cycles essential for pelvic floor function.
How Do Different Life Stages Affect Device Selection?
Women’s pelvic floor training needs evolve across reproductive life stages, influencing optimal device selection and training approaches. Understanding these stage-specific considerations helps tailor interventions for maximum effectiveness.
Young women experiencing stress incontinence during high-impact athletics often benefit from biofeedback devices like Elvie Trainer that integrate easily into fitness routines. The quick 5-minute sessions fit conveniently before or after workouts, and real-time feedback helps coordinate pelvic floor contractions with core exercises. Training focused on injury reduction during this stage may forestall more significant issues later.
Pregnancy and postpartum represent critical periods for pelvic floor health. Device use during pregnancy requires healthcare provider approval and typically focuses on maintaining rather than aggressively strengthening muscles. The postpartum period, after adequate healing and provider clearance, offers an optimal window for rehabilitation before chronic weakness develops.
Our detailed guide on Kegel exercisers for postpartum recovery provides comprehensive information about post-delivery rehabilitation including device selection, timing, and realistic expectations during this recovery phase.
Perimenopause brings hormonal fluctuations affecting tissue elasticity and muscle tone before complete estrogen decline. Women in this transition often benefit from combination devices like Perifit Care+ that offer both electrical stimulation for declining muscle strength and biofeedback for maintaining technique. Starting training during perimenopause rather than waiting until after menopause provides better baseline strength for navigating hormonal changes.
Our guide addressing pelvic floor trainers for menopause specifically explores device selection and training modifications optimizing outcomes during this significant transition.
Post-menopause requires adjusting expectations and potentially intensifying interventions. The significant estrogen decline causes tissue changes requiring more patience for results and often benefiting from combination approaches including topical vaginal estrogen when medically appropriate. Devices providing strong electrical stimulation like Yarlap help overcome age-related muscle weakness.
Advanced age with multiple comorbidities demands simplified approaches with minimal technical requirements. The hands-free automated operation of Yarlap suits women who find app-based devices overwhelming or those with arthritis making probe insertion and removal challenging. Safety considerations increase importance, requiring thorough review of contraindications.
Athletic women training for specific sports may need different approaches than sedentary women. High-impact athletes benefit from programs emphasizing quick-response strength and endurance under pressure. Devices offering sport-specific training programs or allowing customized exercise sequences accommodate these specialized needs.
Women with obesity face unique challenges including increased intra-abdominal pressure stressing pelvic floor muscles and potentially difficulty with probe insertion. Devices with smaller, more ergonomic probes and programs specifically designed for women with higher BMI provide better experiences and outcomes.
Life stage considerations: Match device technology to your current reproductive stage, overall health status, athletic demands, and long-term pelvic floor health goals, recognizing that optimal device choices may change as you transition through different life phases.
What Role Do Apps Play in Device Effectiveness?
Smartphone apps transform passive medical devices into interactive training systems providing guidance, motivation, and progress tracking that enhance long-term adherence. The quality and features of accompanying apps significantly influence real-world effectiveness beyond the device hardware capabilities.
Personalization algorithms in advanced apps like Perifit Care+ assess your baseline capability through initial testing and create customized programs matching your starting strength level. Programs automatically adjust difficulty as you progress, maintaining optimal training stimulus without overwhelming weakened muscles or allowing plateaus from insufficient challenge.
Progress visualization motivates continued use by making abstract muscle strengthening concrete and measurable. Graphs showing increasing contraction strength over weeks provide tangible evidence that your effort produces results. This feedback proves especially valuable during the early weeks when symptoms may not yet improve noticeably.
Gamification transforms tedious repetitive exercises into engaging activities. Research on health behavior change shows that making therapeutic activities enjoyable significantly increases adherence rates. Women who view training sessions as a few minutes of gaming rather than medical treatment demonstrate better consistency over months.
Educational content integrated into quality apps helps users understand pelvic floor anatomy, proper exercise technique, and how different training modes address specific symptoms. This knowledge empowers women to make informed decisions about training parameters and recognize when professional consultation would benefit their specific situation.
Symptom tracking features allow monitoring incontinence episodes alongside training completion, revealing correlations between consistent device use and symptom reduction. The data helps identify what training frequency and intensity produce optimal results for your individual response pattern.
Reminder systems built into apps prompt regular training sessions, helping establish consistent routines. Research shows that consistency determines outcomes more than any single parameter—women who train regularly at moderate intensity achieve better results than sporadic high-intensity sessions. Automated reminders support the habit formation crucial for long-term success.
Privacy considerations require attention when apps collect health data. Reviewing privacy policies reveals what information gets stored, whether data is shared with third parties, and your options for data deletion. Some apps function without creating accounts or uploading data to cloud servers, offering local-only tracking for privacy-conscious users.
The device-app connection reliability affects user experience. Bluetooth connectivity issues causing frequent disconnections frustrate users and may discourage continued use. Reading user reviews specifically addressing app reliability helps identify devices with stable connections versus those plagued by technical issues.
Social features in some apps allow connecting with other users for support and motivation. While not everyone wants social interaction around pelvic floor health, some women find community encouragement helpful during challenging training periods.
Video demonstrations within apps clarify proper device positioning and exercise techniques. Seeing visual instructions proves more helpful than reading text descriptions for many users, reducing initial confusion and improving technique adherence.
App impact: Apps with personalized algorithms, progress graphs showing contraction strength trends over 8-12 weeks, gamification features, and automated reminders significantly increase adherence rates compared to sporadic device use without structured guidance according to behavioral research.
Understanding Different Types of Urinary Incontinence
Accurate incontinence type identification helps select the most appropriate device and training approach. While healthcare providers make formal diagnoses, understanding basic incontinence categories helps guide initial device selection.
Stress urinary incontinence involves leakage during physical activities that increase abdominal pressure. Coughing, sneezing, laughing, exercising, or lifting heavy objects trigger leakage. The underlying mechanism involves weakened pelvic floor muscles unable to maintain urethral closure during pressure spikes. Device training with either electrical stimulation or biofeedback directly addresses this muscle weakness.
Urgency urinary incontinence features sudden strong urges to urinate with difficulty reaching the bathroom in time. Also called overactive bladder, this type relates to inappropriate bladder muscle contractions rather than primarily muscle weakness. Electrical stimulation helps by modulating neural signals controlling bladder contractions. Some women experience urgency without leakage (urgency without incontinence), while others leak before reaching the toilet.
Mixed incontinence combines both stress and urgency symptoms. This represents the most common pattern in postmenopausal women. Combined devices offering both electrical stimulation and biofeedback address both underlying mechanisms. Training programs may need to target both muscle strengthening and neural modulation.
Overflow incontinence results from incomplete bladder emptying, causing frequent or constant dribbling as the over-full bladder leaks small amounts. This type requires medical evaluation to identify underlying causes, which may include nerve damage, medications, or anatomical obstructions. Pelvic floor training alone typically doesn’t resolve overflow incontinence.
Functional incontinence occurs when physical or mental limitations make reaching the toilet difficult despite normal bladder and pelvic floor function. Examples include severe arthritis limiting mobility or dementia affecting bathroom recognition. Pelvic floor devices don’t address functional incontinence, which requires environmental modifications and assistance.
Identifying your primary incontinence type guides device selection. Pure stress incontinence responds well to either electrical stimulation or biofeedback. Pure urgency incontinence shows better response to electrical stimulation. Mixed patterns benefit from combination devices. Keeping a symptom diary documenting when leakage occurs and what activities trigger it helps clarify your specific pattern.
The severity within each type also matters. Mild stress incontinence involving occasional drops during intense exercise differs from severe stress incontinence causing significant leakage during everyday activities. Severity level influences both device selection and realistic timeline expectations for improvement.
Type-specific guidance: Stress incontinence involving leakage during physical pressure responds to either biofeedback or electrical stimulation showing comparable improvements, urgency incontinence benefits more from electrical stimulation neural modulation at 10-20 Hz frequencies, while mixed patterns require combination devices addressing both mechanisms.
Frequently Asked Questions
How effective are pelvic floor trainers for urinary incontinence?
Research shows that electrical stimulation combined with pelvic floor muscle training can significantly reduce incontinence episodes. A 2025 systematic review found that while electrical stimulation alone shows similar results to supervised pelvic floor exercises, combining both approaches produces the best outcomes for many women with stress and urgency incontinence.
Can pelvic floor trainers help with severe incontinence?
Yes, particularly devices that use electrical muscle stimulation. Studies demonstrate that intravaginal electrical stimulation increases voluntary pelvic floor muscle contractions by directly activating muscle fibers, which can benefit women with severe weakness who struggle to perform traditional Kegel exercises effectively on their own.
How long does it take to see results from a pelvic floor trainer?
Most research protocols show improvements within 4-12 weeks of consistent use. Clinical studies typically use programs ranging from 20-30 minute sessions, 2-3 times per week. Some women report noticing reduced leakage episodes within the first few weeks, though maximum benefits generally appear after 8-12 weeks of regular training.
Are EMS pelvic floor devices safe to use at home?
FDA-cleared devices designed for home use are generally safe when used according to manufacturer instructions. However, women who are pregnant, have pacemakers, have active pelvic infections, or certain medical conditions should consult healthcare providers before use. Starting with lower intensity settings and gradually increasing helps minimize discomfort.
What’s the difference between biofeedback and electrical stimulation for incontinence?
Biofeedback devices measure your pelvic floor muscle contractions and provide visual or auditory feedback to help you perform exercises correctly. Electrical stimulation devices send gentle electrical pulses to contract the muscles for you, which can be especially helpful if muscles are very weak. Many modern devices combine both technologies for comprehensive training.
Do I still need to do Kegel exercises if I use a pelvic floor trainer?
Research indicates that combining device-based training with traditional pelvic floor muscle exercises often produces superior results compared to either approach alone. Devices help ensure proper muscle activation and provide consistency, while daily functional exercises throughout the day reinforce muscle memory and strength gains.
Can pelvic floor trainers help with both stress and urge incontinence?
Yes, evidence supports their use for multiple types of incontinence. Electrical stimulation has shown effectiveness for both stress incontinence related to muscle weakness and urgency incontinence associated with overactive bladder. The mechanisms differ slightly, with stress incontinence benefiting from muscle strengthening and urgency incontinence responding to neural modulation effects.
Our Top Recommendations
The Perifit Care+ ($179) earns our top overall recommendation by combining electrical muscle stimulation and biofeedback in a single device with sophisticated app-based programs adapting to your individual progress. The dual-mode functionality addresses both severe weakness through automatic electrical stimulation and technique refinement through interactive biofeedback games, making it suitable for women across the full spectrum of incontinence severity.
For women with severe incontinence and significant muscle weakness, the Yarlap ($299) provides physician-designed automatic electrical stimulation requiring no voluntary muscle control. The powerful pre-programmed sessions deliver clinical-grade muscle contractions rebuilding foundational strength before progressing to active exercises.
Budget-conscious women seeking effective training at an accessible price point should consider the K-Goal Incontinence Stimulator ($114). Despite the lower cost, it delivers core electrical stimulation functionality with basic biofeedback capability, providing evidence-based intervention without premium pricing.
The Elvie Trainer ($199) suits women with moderate muscle strength who prioritize exceptional app experience and active training over electrical stimulation. The award-winning design and sophisticated guided workouts make it ideal for motivated users wanting to perfect technique through comprehensive biofeedback.
Join the discussion: Facebook | X | YouTube | Pinterest
Conclusion
Urinary incontinence affects millions of women across all life stages, yet effective conservative interventions exist that can significantly improve or resolve symptoms without surgery or medication. Device-based pelvic floor training provides structured, evidence-based muscle strengthening that addresses the underlying weakness causing most stress and urgency incontinence.
The research consistently demonstrates that electrical stimulation and biofeedback technologies effectively strengthen pelvic floor muscles, reduce incontinence episodes, and improve quality of life when used consistently over 8-12 weeks. Success depends less on which specific device you choose and more on selecting one matching your individual muscle strength level, technical comfort, and willingness to commit to regular training sessions.
Combined approaches produce superior outcomes. Using devices providing both electrical stimulation and biofeedback, integrating device training with daily functional exercises, and addressing lifestyle factors like fluid management and healthy weight maintenance create comprehensive rehabilitation addressing incontinence from multiple angles.
The devices reviewed here represent different points along the spectrum from fully automated electrical stimulation to interactive biofeedback training. Perifit Care+ offers the most comprehensive solution combining both technologies with sophisticated app-based personalization. Yarlap provides powerful automatic stimulation for severe weakness. K-Goal delivers core functionality at budget-friendly pricing. Elvie Trainer excels in premium biofeedback with exceptional user experience.
Starting pelvic floor rehabilitation sooner rather than later produces better long-term outcomes. Whether you’re experiencing early postpartum leakage, perimenopause-related urgency, or long-standing incontinence you’ve hesitated to address, evidence-based device training offers accessible at-home intervention proven effective in clinical research.
Realistic expectations support long-term success. Not every woman achieves complete continence, but most experience meaningful improvement reducing symptoms to levels no longer significantly impacting quality of life. Viewing device training as a long-term health practice similar to regular exercise rather than a short-term fix helps maintain the ongoing maintenance training preserving initial gains.
Professional guidance enhances outcomes when accessible. Even a few sessions with a pelvic floor physical therapist learning proper technique and receiving individual assessment optimizes subsequent home device training. The combination of professional expertise and convenient home practice provides the ideal balance for many women.
The investment in quality pelvic floor training devices represents a fraction of the cost of surgical interventions while offering a conservative first-line approach with minimal risks and significant potential benefits. For women whose quality of life is diminished by urinary incontinence, evidence-based device training deserves serious consideration as part of a comprehensive management strategy.
Related Reading
- Best Pelvic Floor Trainer: Complete Guide to Devices and Results — Comprehensive comparison of top-rated pelvic floor trainers
- Elvie Trainer Review: In-Depth Analysis and Real Results — Detailed review of the Elvie biofeedback trainer
- Best Kegel Exerciser for Postpartum Recovery — Evidence-based postpartum rehabilitation guide
- Best Pelvic Floor Trainer for Menopause — Devices that work during hormonal changes
- Best Biofeedback Pelvic Floor Device — Technology that improves training results
- Pelvic Floor Exercises vs Devices — Which approach works better for you
References
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.