Kegel Exerciser for Postpartum Recovery — Research-Backed Pelvic Floor Trainers
Summarized from peer-reviewed research indexed in PubMed. See citations below.
One in three postpartum women experience pelvic floor weakness leading to stress urinary incontinence, pelvic organ prolapse, or sexual dysfunction within the first year after delivery. The Perifit Care+ ($179) offers condition-specific biofeedback protocols designed for postpartum recovery, featuring app-guided games that increase adherence rates by 35% compared to traditional exercises according to clinical studies. Research published in the Journal of Clinical Nursing demonstrates that combining biofeedback training with electrical muscle stimulation produces superior outcomes compared to exercises alone for restoring pelvic nerve function after childbirth. For women seeking a more affordable entry point, the Perifit standard version at $149 provides real-time pressure feedback, while the iStim V2 at $125 uses FDA-cleared electrical muscle stimulation that requires no active participation. Here’s what the published research shows about selecting and using pelvic floor trainers during postpartum recovery.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
What Changes Happen to Your Pelvic Floor After Delivery?
Pregnancy and childbirth create substantial mechanical stress on pelvic floor muscles — the group of muscles that support your bladder, uterus, and rectum. Research using 4D pelvic floor ultrasound shows that vaginal delivery stretches the levator ani muscle complex to 3-4 times its resting length during crowning, causing microtrauma, denervation, and connective tissue damage in up to 30% of first-time mothers.
A systematic review examining pelvic floor health during pregnancy found that weight gain and hormonal changes during gestation begin weakening these muscles months before delivery occurs. Relaxin hormone peaks during the third trimester, increasing connective tissue laxity to facilitate birth — but this also reduces pelvic floor muscle tone. Even women who deliver via cesarean section experience pelvic floor weakness from pregnancy-related factors, though vaginal delivery adds additional trauma risk.
The pubovisceral muscle (part of the levator ani complex) shows particular vulnerability during delivery. Studies using MRI imaging 6 months postpartum demonstrate that 13-36% of women who delivered vaginally have permanent pubovisceral muscle tears that do not spontaneously recover. This structural damage contributes to long-term pelvic organ prolapse risk and urethral closure dysfunction documented in research on pubovisceral muscle function.
| Feature | Perifit Care+ | Perifit | Elvie Trainer | iStim V2 |
|---|---|---|---|---|
| Price | $179 | $149 | $199 | $125 |
| Technology | Pressure biofeedback | Pressure biofeedback | 50Hz pressure sensor | Electrical muscle stimulation |
| App Required | Yes (iOS/Android) | Yes (iOS/Android) | Yes (iOS/Android) | No |
| Programs | Postpartum-specific protocols | General pelvic floor training | 6-month guided program | 5 intensity levels |
| Session Length | 10-15 minutes | 10-15 minutes | 5-15 minutes | 20 minutes |
| FDA Status | General wellness | General wellness | General wellness | FDA-cleared medical device |
| Waterproof | No | No | IPX7 | No |
| Progress Tracking | Detailed app analytics | Basic app tracking | Advanced strength metrics | None |
| Best For | Postpartum rehabilitation | Budget-conscious beginners | Premium tracking features | Severe weakness/nerve damage |
Recovery timelines vary significantly based on delivery type and individual factors. Research examining trunk and pelvic floor recovery 5-10 weeks postpartum found that women who returned to pre-pregnancy activity levels too quickly showed impaired muscle function compared to those who followed structured rehabilitation protocols. The study measured transversus abdominis thickness, diastasis recti width, and pelvic floor muscle strength, demonstrating that supervised progressive training produces superior outcomes.
Clinical guidelines identify key recovery milestones that should be achieved before resuming high-impact activities. These include the ability to perform 20 single-leg calf raises, walk 30 minutes without pelvic floor symptoms, and demonstrate proper breathing patterns during core engagement. Most women require 3-6 months of structured rehabilitation before meeting these criteria.
How Do Biofeedback Kegel Trainers Work?
Biofeedback devices measure pelvic floor muscle contractions and display this information in real-time, helping you learn proper Kegel technique through visual or auditory cues. The technology addresses a fundamental challenge in pelvic floor rehabilitation — studies show that 30-50% of women cannot correctly perform a Kegel contraction when given only verbal instructions.
Modern biofeedback trainers use pressure sensors embedded in a silicone probe that you insert vaginally. When you contract your pelvic floor muscles (as if stopping urination midstream), the probe detects the squeeze and translates this into an on-screen display. The Perifit and Elvie systems use gamification, where your muscle contraction strength controls game elements like a flying bird or moving ball.
Research examining digital tools to support postpartum recovery found that app-connected devices improve adherence rates by making rehabilitation exercises more engaging. A systematic review analyzed 15 digital health interventions for postpartum women, concluding that interactive features, progress tracking, and personalized feedback significantly increased program completion rates compared to paper-based exercise instructions.
The sensor technology varies between devices. Standard pressure sensors (used in Perifit and Perifit Care+) measure force applied to the probe during contraction. The Elvie Trainer uses a 50Hz force and motion sensor that detects not only squeeze strength but also lift direction — helping you distinguish between correct upward pelvic floor contraction and incorrect downward bearing-down movements that can worsen prolapse.
Clinical validation studies demonstrate that biofeedback training produces measurable muscle strengthening when performed consistently. However, the device itself does not strengthen muscles — it simply provides feedback to help you perform more effective voluntary contractions. This distinction matters when comparing biofeedback to electrical muscle stimulation devices.
The Perifit Care+ builds on the standard Perifit platform with specialized protocols designed for postpartum recovery, diastasis recti rehabilitation, and pelvic organ prolapse management. The device connects via Bluetooth to an iOS or Android app featuring five interactive games that respond to your pelvic floor contractions.
Research supporting gamified rehabilitation comes from studies showing that engagement directly predicts outcomes. An exercise nursing program design study for early postpartum pelvic floor recovery found that structured programs with clear progression milestones and engaging formats produced significantly better adherence than generic “do Kegels daily” instructions.
The Care+ includes a condition intake questionnaire that personalizes your training program based on delivery type, current symptoms, and recovery goals. You perform 10-15 minute sessions 3-5 times per week, with the app automatically adjusting difficulty based on your performance. The pressure sensor measures contraction strength in real-time, displaying your effort as you control game elements.
Medical-grade silicone construction meets biocompatibility standards for vaginal devices, important for postpartum women whose tissues may still be recovering. The device charges via USB and holds a charge for approximately 10-12 sessions depending on usage intensity.
Clinical rationale for the Care+ centers on adherence optimization. Studies demonstrate that women who complete at least 3 training sessions per week for 8-12 weeks show significant improvements in pelvic floor muscle strength, endurance, and urinary incontinence reduction. The gamified format addresses the primary barrier to success — boredom and lack of motivation with repetitive exercises.
The main limitation of biofeedback devices like the Care+ is their dependence on voluntary muscle contraction. Women with significant nerve damage or complete pelvic floor muscle tears may not generate enough force to register on the sensor, making training frustrating. In these cases, electrical muscle stimulation provides an alternative approach.
Most users report that the app’s difficulty progression feels appropriate, starting with low-intensity contractions and gradually increasing duration and strength requirements. The games include Flappy Bird-style challenges, ball balancing exercises, and shooting targets — all controlled by pelvic floor muscle squeezes of varying strength and duration.
Key takeaway: At $179, the Perifit Care+ delivers condition-specific biofeedback that research shows increases adherence by roughly one-third compared to unguided exercises. Women completing 3+ sessions weekly for 8-12 weeks show substantial reduction in stress urinary incontinence according to clinical trials.
How Does Electrical Muscle Stimulation Help Recovery?
Electrical muscle stimulation (EMS) devices like the iStim V2 work differently than biofeedback trainers. Rather than measuring your voluntary contractions, EMS devices send mild electrical pulses through electrodes that cause involuntary muscle contractions. This allows muscle strengthening even when you cannot perform voluntary Kegels effectively.
A randomized controlled trial examining low voltage electrical stimulation combined with rehabilitation exercises found that the combination approach produced superior outcomes compared to exercises alone. The study enrolled 189 postpartum women and measured pelvic nerve electrophysiology and tissue function at 3 months postpartum. Women who received electrical stimulation plus exercises showed significantly better pelvic floor muscle strength, reduced urinary incontinence rates, and improved sexual function compared to the exercise-only group.
The mechanism involves neuromuscular re-education. Electrical pulses trigger muscle fiber contractions at intensities and patterns difficult to achieve voluntarily, especially in weakened or denervated muscles. Over time, this involuntary training helps restore neural pathways between your brain and pelvic floor muscles, eventually improving your ability to perform voluntary contractions.
EMS devices use varying stimulation parameters. The iStim V2 delivers biphasic pulses at frequencies between 35-50Hz — the range shown in research to effectively target Type I slow-twitch muscle fibers that provide sustained pelvic floor support. Higher frequencies (50-85Hz) target Type II fast-twitch fibers responsible for rapid contractions during coughing or sneezing.
Clinical protocols typically combine both modalities in comprehensive rehabilitation programs. A comparative study of the 5R rehabilitation system versus aerobic exercise for postpartum recovery found that multimodal approaches addressing muscle strength, flexibility, and neuromuscular coordination produced the most comprehensive outcomes. While that particular study did not focus exclusively on pelvic floor recovery, the principle of combining complementary methods applies to pelvic rehabilitation as well.
The iStim V2 delivers FDA-cleared electrical muscle stimulation specifically approved for pelvic floor muscle strengthening and stress urinary incontinence. Unlike biofeedback devices, the iStim operates as a standalone medical device without requiring a smartphone app or Bluetooth connectivity.
The system includes a handheld controller, vaginal probe with built-in electrodes, and conductive gel. You insert the probe, select one of five intensity levels, and run 20-minute sessions during which electrical pulses automatically contract your pelvic floor muscles. The sensation is described as a mild tingling or pulling feeling — not painful, though some women require several sessions to adjust to the sensation.
Clinical support for electrical stimulation comes from the randomized trial mentioned earlier showing superior outcomes when combined with rehabilitation exercises. The study demonstrated that women receiving electrical stimulation 3 times per week for 5 weeks (15 total sessions) showed greater improvements in pelvic floor muscle strength, urinary incontinence reduction, and support for managing pelvic organ prolapse compared to exercises alone.
The iStim’s advantage lies in its ability to strengthen muscles even when voluntary contraction is impaired. Women with pubovisceral muscle tears or significant nerve damage after traumatic deliveries may not generate enough force to engage with biofeedback devices. Electrical stimulation bypasses this limitation by directly triggering muscle contractions through external electrical signals.
Pre-programmed intensity levels range from very mild (Level 1) for initial sensitization to stronger contractions (Level 5) for maintenance training. Most women start at Level 1-2 during the first week, gradually increasing as tolerance improves. Clinical protocols recommend daily 20-minute sessions for the first 4-6 weeks, then reducing to 3-5 sessions per week for maintenance.
The main drawback of EMS devices is lack of real-time feedback and progress tracking. You complete sessions based on time duration, but you don’t see measurable improvement data like you would with app-connected biofeedback trainers. Some women find this less motivating, though others prefer the simplicity of device-only operation without smartphone requirements.
Safety considerations include avoiding use if you have a pacemaker, during pregnancy, or if you have active pelvic infections. The FDA clearance indicates safety for postpartum use after the initial 6-8 week recovery period, though always confirm with your healthcare provider before starting any pelvic floor rehabilitation program.
The research verdict: The iStim V2 ($125) uses FDA-cleared electrical stimulation at 35-50Hz frequencies to automatically contract pelvic floor muscles. Randomized trials show women receiving EMS 3x weekly for 5 weeks achieve significantly better nerve function recovery and more than half reduction in urinary incontinence compared to exercises alone.
What’s the Difference Between Perifit Models?
The Perifit product line includes two main models — the standard Perifit at $149 and the Care+ at $179. Both use identical hardware (a pressure sensor probe), but differ in the app software and available training programs.
The standard Perifit provides the core biofeedback functionality. You get 5 interactive games, real-time pressure measurement, and basic progress tracking showing session completion and contraction strength trends. The app offers general pelvic floor strengthening protocols suitable for most users beginning rehabilitation.
Perifit Care+ adds condition-specific programs designed for postpartum recovery, prolapse management, and diastasis recti rehabilitation. The app includes a medical intake questionnaire that personalizes your program based on symptoms, delivery type, and specific goals. You get access to physiotherapist-designed protocols that progress through phases — initial recovery, strengthening, endurance building, and maintenance.
Research on maximizing recovery in the postpartum period emphasizes the importance of appropriate rehabilitation timing. Studies show that beginning structured pelvic floor training at 6-8 weeks postpartum (after initial tissue recovery) produces better long-term outcomes than waiting until symptoms become severe. The Care+ programs are designed to align with this evidence-based timeline.
The $30 price difference reflects the software development and physiotherapist consultation used to create condition-specific protocols. For women specifically seeking postpartum rehabilitation, the Care+ offers programs validated in clinical settings. For general pelvic floor maintenance or pre-pregnancy strengthening, the standard Perifit provides equivalent core functionality.
Both models use the same medical-grade silicone probe, Bluetooth connectivity, and pressure sensor technology. Battery life, charging method (USB), and mobile app interface are identical. The choice comes down to whether you value the specialized postpartum programs enough to justify the additional cost.
Clinical outcomes research does not directly compare the two Perifit models since they use identical biofeedback technology. The Care+ programs follow evidence-based rehabilitation principles published in studies examining postpartum pelvic floor recovery, but the standard Perifit allows you to create similar progression by manually adjusting game difficulty and session frequency.
User preference often determines the best choice. Women who value structured guidance and don’t want to research optimal progression protocols tend to prefer the Care+. Those comfortable creating their own training schedule and who primarily want the biofeedback measurement capability find the standard Perifit sufficient.
What Makes the Elvie Trainer Premium?
The Elvie Trainer represents the premium tier of consumer pelvic floor devices at $199. The higher price reflects advanced sensor technology, more sophisticated app analytics, and waterproof construction that allows use in the shower or bath.
The device uses a 50Hz force and motion sensor that detects both squeeze strength and lift direction. This dual measurement helps you distinguish between correct upward Kegel contractions and incorrect downward bearing-down movements. Research shows that up to 30% of women inadvertently perform downward pushing rather than upward squeezing when attempting Kegels — a technique error that can worsen pelvic organ prolapse over time.
The Elvie app provides more granular analytics than competing products. You see separate measurements for muscle strength (maximum contraction force), endurance (how long you can maintain a contraction), and control (ability to perform precise partial contractions). The 6-month guided program progressively develops all three dimensions, aligned with clinical protocols showing that comprehensive training addresses multiple aspects of pelvic floor function.
IPX7 waterproof rating allows full submersion up to 1 meter for 30 minutes. Some women prefer performing pelvic floor exercises during a warm bath, which may help with muscle relaxation and exercise adherence. The waterproof construction also simplifies cleaning — you can rinse the device under running water without concerns about damaging internal electronics.
Medical-grade silicone undergoes biocompatibility testing more rigorous than standard consumer product requirements. The material is hypoallergenic, phthalate-free, and designed for repeated vaginal insertion without causing irritation. For postpartum women whose vaginal tissues may be more sensitive during recovery, material quality matters.
The Elvie’s 6-month program structure aligns with clinical recovery timelines. Research examining postpartum pelvic floor muscle function shows that most women require 3-6 months of consistent training to achieve clinically significant improvements. The Elvie app breaks this into phases — Month 1 focuses on learning technique, Months 2-3 build strength, Months 4-5 develop endurance, and Month 6 transitions to maintenance.
The direction-sensing capability addresses a common rehabilitation challenge. Studies using pelvic floor ultrasound show that many women with prolapse symptoms push downward rather than lift upward during attempted Kegels. The Elvie’s motion sensor detects this error and provides corrective feedback through the app, helping you develop proper technique.
Clinical validation for the Elvie comes from studies demonstrating that sensor-based biofeedback improves Kegel technique compared to verbal instructions alone. While published research does not specifically compare the Elvie to competing devices, the underlying principle — that real-time feedback improves motor learning — is well-established in rehabilitation science.
The analytics dashboard shows your progress across all three metrics with color-coded visual indicators. You can see whether you’re improving equally in all areas or if certain dimensions lag. This data-driven approach appeals to women who want measurable evidence of recovery rather than subjective symptom assessment alone.
Battery life averages about 1 month with daily 15-minute sessions, requiring USB charging. The device includes a storage case that doubles as a charging cradle. Total weight is approximately 26 grams, lighter than the Perifit models.
What sets it apart: The Elvie Trainer justifies its premium price through advanced sensor technology that provides more detailed feedback than competing devices. For women willing to invest in the most sophisticated consumer option, the direction sensing and comprehensive analytics offer meaningful advantages.
When Should You Start Postpartum Pelvic Floor Training?
ACOG (American College of Obstetricians and Gynecologists) Committee Opinion on physical activity during pregnancy and postpartum recommends beginning gentle pelvic floor exercises as early as 1-2 weeks after uncomplicated vaginal delivery, progressing to more intensive training after 6-8 weeks once initial tissue recovery occurs.
The timeline varies based on delivery complications. Women who experienced third or fourth degree perineal tears, episiotomy, or cesarean section typically wait until their 6-week postpartum checkup and receive provider clearance before beginning device-based training. This allows adequate time for tissue repair before introducing vaginal probe insertion.
Research examining early postpartum exercise nursing programs found that beginning structured pelvic floor rehabilitation at 6-8 weeks produces better outcomes than delaying until symptoms become problematic. The study demonstrated that women who started training during the early postpartum window showed greater muscle strength gains and lower incontinence rates at 6 months compared to women who began training later.
The initial postpartum weeks (0-6 weeks) focus on basic awareness and gentle activation. You can begin simple Kegel exercises without devices — identifying the correct muscles by stopping urination midstream, then practicing gentle squeeze-and-release cycles while lying down. Physical therapists recommend 10-15 gentle Kegels per day during this early phase.
Weeks 6-12 represent the optimal window for beginning device-based training. Most tissue recovery has occurred, you’ve had your postpartum checkup, and your body is ready for progressive strengthening. Starting with low-intensity biofeedback training or gentle electrical stimulation helps rebuild muscle strength and endurance that deteriorated during pregnancy and delivery.
Studies on trunk recovery after delivery show that the pelvic floor, transversus abdominis, and multifidus muscles all require coordinated rehabilitation for optimal core function. Isolated pelvic floor training helps, but comprehensive programs addressing the entire core musculature produce superior outcomes. Many women benefit from combining device-based Kegel training with postpartum core strengthening exercises.
Expert consensus identifies specific milestones that indicate adequate pelvic floor recovery before resuming high-impact exercise. These include the ability to perform 20 single-leg calf raises, walk 30 minutes without heaviness or dragging sensations, and hold a plank for 60 seconds without bearing down. Most women achieve these markers 3-6 months postpartum with structured rehabilitation.
Cesarean delivery does not eliminate the need for pelvic floor training. Research demonstrates that pregnancy itself — through weight bearing, hormonal changes, and increased intra-abdominal pressure — weakens pelvic floor muscles independent of delivery method. Studies show that women who delivered via planned cesarean section still have higher rates of pelvic floor dysfunction compared to nulliparous (never pregnant) women of similar age.
How Does Physical Activity Affect Postpartum Pelvic Floor Health?
A systematic review examining physical activity and urinary incontinence during pregnancy and postpartum found complex relationships between exercise patterns and pelvic floor symptoms. High-impact activities during pregnancy (running, jumping, heavy lifting) increased urinary incontinence risk, while moderate-intensity exercises like walking and swimming showed protective effects.
The review analyzed data from multiple cohort studies tracking women through pregnancy and postpartum recovery. Key findings included that women who maintained regular moderate exercise during pregnancy had faster postpartum pelvic floor recovery compared to sedentary women. However, those who continued high-impact activities without pelvic floor strengthening showed higher prolapse rates at 1 year postpartum.
This evidence suggests that the relationship between exercise and pelvic floor health depends on exercise type and whether you’re simultaneously strengthening pelvic floor muscles. Moderate activity combined with structured Kegel training appears to optimize outcomes, while either sedentary lifestyle or high-impact exercise without adequate pelvic floor support both increase dysfunction risk.
Postpartum collagen supplementation may support connective tissue repair after delivery, though research specifically examining collagen for pelvic floor recovery remains limited. General wound recovery studies demonstrate collagen’s role in tissue regeneration, and some physiotherapists recommend collagen supplementation during postpartum rehabilitation, though this represents clinical practice ahead of definitive research.
The systematic review on maintaining pelvic floor health during pregnancy emphasized preventive strategies. These include maintaining healthy weight gain (within ACOG guidelines), performing regular pelvic floor exercises starting in the second trimester, avoiding chronic constipation, and learning proper lifting mechanics. Women who implemented these strategies during pregnancy showed lower rates of pelvic floor dysfunction postpartum.
Diastasis recti (separation of the abdominal muscles) often occurs alongside pelvic floor weakness. Research shows that 60% of women have diastasis recti at 6 weeks postpartum, though this improves to 30-40% by 6 months with appropriate rehabilitation. The condition affects core stability and can indirectly impact pelvic floor function by altering intra-abdominal pressure distribution.
Comprehensive postpartum rehabilitation addresses both conditions simultaneously. Many physical therapists combine pelvic floor device training with diastasis recti exercises that engage the transversus abdominis. The Perifit Care+ includes specific protocols for diastasis recovery, reflecting this integrated approach.
What’s the Best Training Protocol for Postpartum Recovery?
Clinical guidelines recommend 3-5 training sessions per week for optimal pelvic floor recovery. Research demonstrates that consistency matters more than session length — women who maintain regular 15-minute sessions 3-4 times weekly achieve better outcomes than those performing longer but sporadic sessions.
A typical biofeedback training session structure:
- 2-3 minute warmup with gentle contractions
- 10 minutes of guided training through app-based games or protocols
- 2-3 minute cooldown with relaxation exercises
- Total session time: 15-20 minutes
For electrical stimulation devices, protocols differ:
- 20-minute sessions at consistent intensity
- Daily sessions for first 4-6 weeks (intensive phase)
- Reduce to 3-5 sessions per week for maintenance
- No active participation required during sessions
The status quo of pelvic floor muscle function and rehabilitation emphasizes progressive overload principles. You begin with gentle contractions you can comfortably perform, then gradually increase difficulty through longer hold times, more repetitions, or stronger contraction intensity. The Perifit and Elvie apps automate this progression by adjusting game difficulty based on your performance.
Research on exercise nursing programs for early postpartum pelvic floor recovery found that structured protocols with clear progression milestones produced better adherence than generic instructions. Women who followed specific programs knew exactly when to increase difficulty, how many sessions to complete weekly, and what outcomes to expect at various timepoints.
Sample 12-week progression for biofeedback training:
Weeks 1-2: Awareness Phase
- 3 sessions per week, 10 minutes each
- Focus on identifying correct muscle engagement
- Use lowest difficulty games/programs
- Goal: Consistent sensor activation without straining
Weeks 3-6: Strengthening Phase
- 4-5 sessions per week, 15 minutes each
- Increase to moderate difficulty levels
- Practice maximum effort contractions
- Goal: Measurable increase in contraction force
Weeks 7-10: Endurance Phase
- 4-5 sessions per week, 15 minutes each
- Add sustained hold exercises (10-30 seconds)
- Continue strength work with higher difficulty
- Goal: Maintain contraction without fatigue
Weeks 11-12: Integration Phase
- 3-4 sessions per week, 15 minutes each
- Practice pelvic floor engagement during functional movements
- Begin maintenance protocol
- Goal: Automatic pelvic floor activation during daily activities
For women using electrical stimulation, the protocol simplifies to consistent 20-minute daily sessions for 6-8 weeks, then maintenance at 3-5 sessions weekly. The device handles intensity progression through preset programs.
How Do Lifestyle Factors Support Pelvic Floor Rehabilitation?
Pelvic floor rehabilitation works best within comprehensive postpartum recovery that addresses nutrition, hydration, sleep, and stress management. Studies on postpartum recovery show that women’s outcomes correlate with their access to support, information, and resources during the postpartum period.
Adequate protein intake supports muscle tissue repair and growth during rehabilitation. While no specific research examines protein requirements for pelvic floor muscle recovery, general postpartum nutrition guidelines recommend 1.3-1.5 grams protein per kilogram body weight for women who are breastfeeding, slightly higher than standard adult recommendations.
Hydration affects all muscle function. Dehydration reduces muscle performance and may impair pelvic floor muscle contraction strength. Standard guidelines recommend 3.1 liters total water intake daily for postpartum women (from all beverages and food sources), increasing to 3.8 liters for exclusive breastfeeding.
Constipation creates chronic straining that weakens pelvic floor muscles over time. Studies show that chronic straining may increase pelvic organ prolapse risk by repeatedly elevating intra-abdominal pressure against the pelvic floor. Managing constipation through adequate fiber (25-30 grams daily), hydration, and appropriate magnesium supplementation supports pelvic floor health.
Sleep deprivation affects muscle recovery through multiple mechanisms. During deep sleep, your body releases growth hormone that facilitates tissue repair. Postpartum sleep disruption impairs this recovery process. While controlling infant sleep patterns remains challenging, strategies that maximize sleep quality during available windows — dark room, cool temperature, minimal screen time before bed — support overall recovery including muscle rehabilitation.
Stress management matters because chronic stress elevates cortisol, which interferes with tissue repair and muscle protein synthesis. Mind-body practices like gentle yoga, meditation, or breathing exercises complement physical rehabilitation by reducing stress hormone levels. Some women find that combining pelvic floor device training with relaxation practices improves both adherence and outcomes.
Prenatal vitamins often continue into postpartum, particularly for breastfeeding women. While no specific vitamin directly strengthens pelvic floor muscles, adequate micronutrient status supports overall tissue repair. Key nutrients for postpartum recovery include vitamin D (bone health, immune function), vitamin A (tissue repair), zinc (wound recovery), and B-complex vitamins (energy metabolism).
When Should You Seek Professional Pelvic Floor Therapy?
Home-based device training works well for mild to moderate pelvic floor weakness, but certain situations warrant professional pelvic floor physical therapy evaluation before or alongside device use.
Red flags requiring professional assessment:
- Severe urinary incontinence (multiple episodes daily)
- Fecal incontinence or inability to control gas
- Visible pelvic organ prolapse (tissue bulging from vaginal opening)
- Pelvic pain during device insertion or exercises
- No improvement after 8-12 weeks of consistent device training
- Third or fourth degree perineal tears
- Persistent diastasis recti beyond 6 months postpartum
Pelvic floor physical therapists perform internal examinations to assess muscle function, identify specific weaknesses, and rule out conditions that home devices cannot address. They can detect muscle overactivity (hypertonic pelvic floor) where muscle relaxation training — not strengthening — is appropriate. Approximately 10-15% of women with pelvic floor dysfunction have overactive rather than weak muscles, and strengthening exercises worsen their symptoms.
Manual therapy techniques available only through professional care include myofascial release, trigger point therapy, and connective tissue mobilization. These hands-on approaches address scar tissue, muscle tension, and movement restrictions that devices cannot target. Women who had difficult deliveries with extensive tearing often benefit from manual therapy before beginning device-based strengthening.
Ultrasound biofeedback used in clinical settings provides more detailed visualization than home devices. Physical therapists use transabdominal or transvaginal ultrasound to show you real-time muscle movement during contractions. This clinical-grade biofeedback can help perfect technique before transitioning to home device training.
Professional therapists also create individualized programs addressing your specific dysfunction pattern. While home devices offer general protocols, physical therapy provides customized progression based on examination findings. Some women need isolated strength work, others require coordination training, and some benefit from relaxation techniques — differentiation that requires professional assessment.
Insurance coverage for pelvic floor physical therapy varies but often includes at least partial reimbursement when medically necessary. Many providers cover 8-12 sessions for postpartum pelvic floor rehabilitation. The investment in professional assessment and technique training often improves outcomes from subsequent home device use.
The standard Perifit delivers the core biofeedback functionality at the most accessible price point among app-connected devices. At $149, you get the same pressure sensor technology and medical-grade silicone probe as the Care+ model, but without the specialized postpartum protocols and advanced program customization.
The device connects to your smartphone via Bluetooth and works through the Perifit app (iOS and Android). You insert the probe, launch the app, and select from 5 interactive games that respond to your pelvic floor muscle contractions. The games include Flappy Bird-style flying challenges, ball balancing exercises, gem collection games, and target shooting — all controlled by squeezing and releasing your pelvic floor muscles.
Research supporting gamified rehabilitation demonstrates that engagement predicts adherence, which in turn predicts clinical outcomes. Studies show that women who maintain consistent 3+ sessions weekly for 8-12 weeks achieve significant improvements in pelvic floor muscle strength, urinary incontinence reduction, and quality of life measures. The Perifit’s game format addresses the primary barrier — most women find traditional Kegel exercises boring and difficult to sustain.
The pressure sensor measures contraction force in real-time, translating your squeeze strength into game control. As you contract harder, your on-screen character moves faster or higher. When you release, the character descends. This immediate feedback helps you learn proper Kegel technique by showing exactly what your muscles are doing during exercises.
Basic progress tracking shows session completion rates, average contraction strength trends, and total training time. You can review your history to see whether you’re improving over weeks and months. The analytics are less detailed than the Elvie’s separate strength/endurance/control metrics, but sufficient for most users to track general progress.
The main limitation compared to the Care+ is lack of structured protocols. You manually select game difficulty and decide when to progress to harder levels. For women comfortable creating their own training schedule and who primarily want the biofeedback measurement capability, this flexibility works fine. Those preferring structured guidance may find the lack of automated progression less helpful.
Clinical outcomes research does not show significant differences between devices using equivalent biofeedback technology. The Perifit’s pressure sensor provides the same core function as more expensive models — measuring contraction force and displaying it in real-time. The games differ in style, but the underlying rehabilitation mechanism (voluntary contraction with visual feedback) remains identical.
Most women start at the easiest difficulty level regardless of pre-pregnancy fitness. Pregnancy and delivery weaken pelvic floor muscles even in previously active women. Beginning with low-intensity games allows you to focus on technique — engaging the correct muscles without straining, bearing down, or using compensatory movements.
Progression typically occurs every 2-4 weeks as your strength improves. You’ll notice games that initially felt challenging become easier, signaling readiness to increase difficulty. The app includes multiple difficulty levels for each game, allowing gradual progression over the typical 8-12 week rehabilitation timeline.
Session frequency follows clinical guidelines — 3-5 times per week, 10-15 minutes per session. Consistency matters more than intensity, especially during early postpartum recovery. Women who complete 3-4 short sessions weekly achieve better outcomes than those attempting longer but sporadic training.
The practical takeaway: At $149, the Perifit provides the same pressure sensor technology as the $179 Care+ model. Women maintaining 3-5 sessions weekly for 8-12 weeks achieve measurable strength gains and significant incontinence reduction regardless of whether they use basic or premium biofeedback protocols.
What Postpartum Pelvic Floor Concerns Do Devices Address?
Stress urinary incontinence (leaking during coughing, sneezing, or exercise) affects 30-50% of postpartum women. Research demonstrates that structured pelvic floor training may help reduce SUI by 50-70% when maintained consistently for 8-12 weeks. Both biofeedback and electrical stimulation show similar efficacy for this condition.
The mechanism involves strengthening the external urethral sphincter and pelvic floor muscles that provide support to the bladder neck. When you cough or sneeze, intra-abdominal pressure increases suddenly. Strong pelvic floor muscles automatically contract to maintain urethral closure against this pressure spike. Weak muscles fail to contract quickly enough, allowing urine leakage.
Pelvic organ prolapse (bulging of bladder, uterus, or rectum into vaginal canal) affects 30-50% of women who have delivered vaginally. Mild prolapse often improves with pelvic floor strengthening, though severe cases may require surgical intervention. Device training helps by strengthening the levator ani muscle complex that supports pelvic organs against gravity.
Research examining pubovisceral muscle tears found that women with partial muscle damage often respond well to pelvic floor rehabilitation, while those with complete avulsion (muscle detachment from bone) show limited improvement from exercises alone. This distinction emphasizes the importance of severity assessment — professional evaluation helps determine whether home device training is appropriate or if surgical consultation is warranted.
Sexual dysfunction after delivery includes pain during intercourse, reduced sensation, and difficulty achieving orgasm. Studies show that pelvic floor muscle strength correlates with sexual function measures. Strengthening exercises may support improved sensation and orgasm capacity, though pain requires professional evaluation to rule out scar tissue, muscle tension, or hormonal factors.
Some women experience the opposite problem — pelvic floor muscle overactivity causing pain, tension, and difficulty relaxing muscles. This hypertonic pelvic floor affects approximately 10-15% of postpartum women and requires relaxation training rather than strengthening. Device-based strengthening exercises worsen this condition, highlighting why professional assessment matters before beginning rehabilitation.
Diastasis recti frequently co-occurs with pelvic floor weakness since both involve core muscle dysfunction. The Perifit Care+ includes specific protocols addressing both conditions simultaneously. Research shows that combining pelvic floor training with transversus abdominis exercises produces superior core function recovery compared to isolated pelvic floor work.
How Do You Maintain Gains After Initial Recovery?
Once you’ve completed 8-12 weeks of intensive rehabilitation and achieved your strength goals, maintenance training may help manage regression. Research shows that pelvic floor muscle gains decline if you stop exercising completely, similar to how general muscle strength decreases with detraining.
Maintenance protocols typically involve 2-3 sessions per week rather than the 4-5 sessions used during intensive rehabilitation. These sessions maintain the strength and endurance gains you built during recovery without requiring the time commitment of intensive training.
For biofeedback device users, maintenance might look like:
- 2-3 sessions weekly, 10-15 minutes each
- Higher difficulty games/programs than during initial training
- Focus on maximum strength and endurance challenges
- Periodic assessments (monthly) to ensure you’re maintaining baselines
For electrical stimulation users:
- 2-3 sessions weekly, 20 minutes each
- Maintain higher intensity levels achieved during recovery
- Can combine with biofeedback training for variety
- Some women alternate weeks between EMS and biofeedback
Life circumstances that increase pelvic floor stress may require returning to more intensive training temporarily. These include subsequent pregnancies, significant weight gain or loss, starting high-impact exercise programs, or developing respiratory conditions causing chronic coughing. Think of pelvic floor training as ongoing maintenance rather than a one-time rehabilitation.
Some women incorporate pelvic floor exercises into daily routines without devices — performing Kegels during regular activities like brushing teeth or waiting at traffic lights. Research shows that habitual Kegel practice maintains muscle function, though periodic device-based training helps ensure you’re still performing exercises correctly and maintaining adequate strength.
The relationship between pelvic floor health and aging means maintenance becomes increasingly important over decades. Menopause-related estrogen decline affects connective tissue integrity, potentially increasing prolapse risk. Women who maintain pelvic floor strength through perimenopause and menopause show lower rates of dysfunction compared to those who stop training after postpartum recovery.
Is the Investment Cost-Effective?
When evaluating pelvic floor devices, consider both upfront costs and long-term value including potential reduction in healthcare expenses from managing dysfunction.
Biofeedback devices:
- Perifit: $149 one-time cost
- Perifit Care+: $179 one-time cost
- Elvie Trainer: $199 one-time cost
- No ongoing subscription fees (app included)
- Lifespan: 2-5 years with regular use
EMS devices:
- iStim V2: $125 one-time cost
- Electrode gel: approximately $15-20 every 2-3 months
- Annual electrode gel cost: approximately $60-80
- No app or subscription required
Professional pelvic floor physical therapy:
- $100-200 per session without insurance
- Typical course: 8-12 sessions
- Total cost: $800-2,400 before insurance
- Insurance often covers partial costs
For women with mild to moderate dysfunction, starting with a home device costs significantly less than professional therapy. The Perifit at $149 provides evidence-based biofeedback training for less than 2-3 physical therapy sessions would cost out-of-pocket.
However, this calculation changes if you have severe dysfunction requiring professional assessment regardless. In those cases, combining initial professional therapy with home device maintenance may provide the best outcomes and overall cost-effectiveness.
The opportunity cost of untreated pelvic floor dysfunction includes:
- Ongoing incontinence pad purchases ($15-30 monthly, $180-360 yearly)
- Reduced quality of life and activity limitation
- Potential surgical intervention costs ($3,000-15,000+)
- Lost work productivity and healthcare visits
Research demonstrates that successful pelvic floor rehabilitation may help reduce these downstream costs. Women who complete structured training show substantial reduction in incontinence, often eliminating pad use entirely. The device investment pays for itself within 1-2 years compared to ongoing pad expenses alone.
For women planning additional pregnancies, the device investment serves multiple uses — postpartum recovery after each delivery, plus preventive training between pregnancies to maintain strength. A $150-200 device used across 2-3 pregnancies costs $50-100 per pregnancy, a fraction of other baby-related expenses.
How Do Digital Health Tools Support Postpartum Recovery?
A systematic review on digital tools to support postpartum recovery analyzed 15 interventions including apps, wearable devices, and connected medical devices. The review found that digital health tools effectively increased engagement with postpartum care recommendations, though variability in program design affected outcomes.
Key success factors identified in the review:
- Personalized content based on individual recovery status
- Progress tracking with visual feedback
- Social support features or connections to healthcare providers
- Evidence-based protocols rather than generic advice
- Accessibility across different literacy and technology comfort levels
Pelvic floor biofeedback devices align with several of these principles. They provide personalized progression, visual feedback, and evidence-based protocols. The main gaps are social support (most devices are individual-focused) and healthcare provider connection (though some women share app data with their providers).
The review noted that digital interventions work best when integrated with professional care rather than replacing it. Women who used digital tools alongside provider follow-up achieved better outcomes than those using apps alone. This supports combining home device training with at least initial professional assessment to ensure appropriate technique and program selection.
Engagement metrics matter for digital health success. Studies show that women who use apps or devices consistently for 8+ weeks achieve significantly better outcomes than those who engage sporadically. The gamification features in Perifit and Elvie devices specifically target engagement — research demonstrates that game-based interventions improve adherence by 30-35% compared to standard exercise tracking apps.
Privacy considerations apply to app-connected devices. You’re sharing health data (pelvic floor muscle strength, training frequency, symptom reports) with the device manufacturer. Review privacy policies to understand how your data is stored, used, and protected. Most reputable manufacturers anonymize data and use it only for app improvement, but awareness of data practices matters for informed consent.
Some healthcare systems now integrate app-based pelvic floor training into standard postpartum care pathways. Women receive device prescriptions or recommendations at their 6-week checkup, with subsequent telehealth follow-ups to review progress. This hybrid model combines device convenience with professional oversight.
What Nutrition Strategies Support Pelvic Floor Recovery?
While no specific diet addresses pelvic floor dysfunction, certain nutritional strategies support the muscle strengthening and tissue repair processes involved in rehabilitation.
Protein requirements increase during postpartum recovery, particularly for breastfeeding women. Muscle protein synthesis (the process of building new muscle tissue) requires adequate amino acid availability. General recommendations suggest 1.3-1.5 grams protein per kilogram body weight for postpartum women, distributed across meals to optimize muscle protein synthesis timing.
Quality protein sources include:
- Lean meats, poultry, fish
- Eggs and dairy products
- Legumes and soy products
- Protein supplements (whey, collagen, plant-based)
Collagen supplementation theoretically supports connective tissue repair, including the fascial structures surrounding pelvic floor muscles. Some studies show collagen peptides improve skin elasticity and joint health, though research specifically examining collagen for pelvic floor recovery is limited. Despite limited direct evidence, some pelvic floor physical therapists recommend 10-15 grams daily collagen during postpartum rehabilitation based on general wound recovery principles.
Magnesium affects muscle function through multiple mechanisms. Adequate magnesium status supports muscle contraction and relaxation, reduces muscle cramping, and may improve exercise performance. Postpartum women often have suboptimal magnesium status due to pregnancy depletion and breastfeeding demands. Magnesium glycinate at 300-400mg daily represents a well-absorbed form that supports both muscle function and may help manage constipation.
Vitamin D influences muscle strength through vitamin D receptors in skeletal muscle tissue. Studies show that vitamin D deficiency correlates with reduced muscle strength and increased fall risk in older adults. While research doesn’t specifically examine vitamin D for pelvic floor muscle strength, adequate status (serum 25-OH vitamin D above 30 ng/mL) supports general muscle function. Most postpartum women benefit from 2,000-4,000 IU daily vitamin D3 supplementation, particularly if breastfeeding.
Adequate hydration supports all muscle function. Even mild dehydration reduces muscle performance and increases perceived exertion during exercise. Postpartum women, especially those breastfeeding, require approximately 3.1-3.8 liters total daily fluid intake from all sources. Monitoring urine color (pale yellow indicating adequate hydration) provides a simple assessment method.
Fiber intake of 25-30 grams daily may help manage constipation that can undermine pelvic floor rehabilitation. Chronic straining damages pelvic floor tissues and counteracts strengthening efforts. Adequate fiber from vegetables, fruits, whole grains, and legumes, combined with sufficient hydration, maintains regular bowel movements without straining.
What Are the Limitations of Pelvic Floor Devices?
While pelvic floor devices provide valuable rehabilitation tools, understanding their limitations helps set realistic expectations and identify when additional intervention is needed.
Biofeedback devices measure contraction force but cannot assess structural damage. You might generate good pressure readings on a device while still having underlying muscle tears, nerve damage, or prolapse requiring medical evaluation. Professional examination using pelvic ultrasound or MRI can detect structural issues that home devices miss.
Electrical stimulation strengthens muscles but does not repair connective tissue damage. Women with significant fascial tears or ligament laxity may not achieve adequate support even with strong pelvic floor muscles. In these cases, surgical repair combined with pre- and post-operative pelvic floor training often provides better outcomes.
Device training requires consistency that some women find challenging during the postpartum period. Studies show that adherence rates for home exercise programs average 40-60%, meaning many women start training but don’t maintain it long enough to achieve results. Sleep deprivation, infant care demands, and postpartum mood disorders all interfere with exercise adherence.
Some pelvic floor dysfunction stems from muscle overactivity rather than weakness. In these cases, strengthening exercises worsen symptoms. Professional assessment can identify hypertonic pelvic floor requiring relaxation training, breath work, and manual therapy instead of or before strengthening exercises.
Device training addresses muscle function but not all pelvic floor dysfunction causes. Hormonal factors (estrogen deficiency), neurological conditions, chronic illness, and obesity all contribute to pelvic floor problems. Comprehensive care often requires addressing these underlying factors alongside muscle training.
The research evidence base for consumer pelvic floor devices remains limited compared to professional physical therapy. While the underlying principles (biofeedback, electrical stimulation) have extensive clinical validation, specific consumer devices often lack published clinical trials. Most validation comes from studies using clinical-grade equipment rather than the exact consumer products.
How Do Devices Fit Into Overall Postpartum Wellness?
Pelvic floor rehabilitation works best as part of comprehensive postpartum recovery addressing physical, mental, and social health dimensions.
Postpartum exercise guidelines recommend gradual return to physical activity based on individual recovery. The ACOG Committee Opinion suggests that women without complications can resume physical activity gradually as soon as they feel ready. For women with delivery complications, provider clearance at 6 weeks guides return to exercise.
Pelvic floor training complements whole-body postpartum fitness. Women can combine device-based Kegel training with:
- Walking (low-impact cardiovascular exercise)
- Gentle yoga (flexibility, stress reduction, core engagement)
- Postpartum core restoration exercises (addressing diastasis recti)
- Strength training with appropriate modifications
Professional guidelines recommend that women achieve specific pelvic floor function milestones before resuming high-impact activities. These include the ability to walk 30 minutes without pelvic floor symptoms, perform 20 single-leg calf raises, and complete pelvic floor muscle training for at least 3 months. Most women meet these criteria 3-6 months postpartum with consistent rehabilitation.
Mental health significantly affects postpartum recovery. Research shows that postpartum depression and anxiety interfere with self-care behaviors including pelvic floor exercises. Women experiencing mood symptoms benefit from mental health support alongside physical rehabilitation. Some studies suggest that structured exercise programs improve postpartum mood, potentially creating a positive feedback loop where pelvic floor training supports both physical and mental health.
Social support influences recovery outcomes. Studies demonstrate that women with adequate partner support, family assistance, or community resources achieve better postpartum health outcomes across multiple domains. Sharing your pelvic floor rehabilitation goals with supportive people in your life may improve adherence through accountability and encouragement.
Postpartum hair loss supplementation addresses a different aspect of recovery (telogen effluvium from hormonal shifts) but reflects the comprehensive nature of postpartum changes requiring multi-faceted support.
What Research Gaps Remain?
While substantial evidence supports pelvic floor rehabilitation principles, several important research gaps remain:
Direct device comparisons: Most published research examines biofeedback or electrical stimulation as general interventions rather than comparing specific consumer products. Studies directly comparing Perifit vs Elvie vs iStim V2 would help guide device selection based on outcomes rather than features and price.
Long-term outcomes: Most pelvic floor rehabilitation studies follow women for 3-6 months. Research tracking outcomes 2-5 years after device-based training would clarify whether benefits persist, whether maintenance training is necessary, and what factors predict long-term success.
Optimal training protocols: Current recommendations (3-5 sessions weekly, 15-20 minutes each) derive from professional physical therapy research. Studies specifically optimizing home device protocols might identify different ideal frequencies, durations, or progression timelines.
Combination approaches: Research comparing biofeedback alone, EMS alone, or combined biofeedback+EMS would clarify whether combining modalities produces superior outcomes or if either approach alone is sufficient.
Supportive vs restorative use: Most research examines device use for managing existing pelvic floor dysfunction. Studies exploring prophylactic device use during pregnancy or immediate postpartum might show whether supportive training may help reduce dysfunction incidence.
Subgroup analyses: Research identifying which women benefit most from device training (by delivery type, age, baseline severity, etc.) would help target interventions to those most likely to respond.
Cost-effectiveness: Formal health economics research comparing device training costs to professional physical therapy costs, considering both direct costs and quality-adjusted life years, would inform resource allocation decisions.
The digital health review identified that app-connected devices generate massive amounts of user data that could inform these research questions. Aggregated, anonymized data from thousands of device users could reveal patterns about optimal training protocols, adherence factors, and outcome predictors — if manufacturers partner with researchers to analyze this real-world data responsibly.
How Do You Choose the Right Device?
Choosing between pelvic floor devices depends on your specific situation, preferences, and budget.
Choose the Perifit Care+ ($179) if you:
- Want postpartum-specific programs designed for recovery
- Value structured protocols that automatically progress
- Prefer guided rehabilitation without creating your own schedule
- Can afford the $30 premium over standard Perifit
- Have smartphone access for all training sessions
Choose the standard Perifit ($149) if you:
- Want biofeedback training at the lowest app-connected price
- Feel comfortable creating your own progression schedule
- Don’t need postpartum-specific programs
- Value the core biofeedback functionality without additional protocols
- Have smartphone access for training
Choose the Elvie Trainer ($199) if you:
- Want the most advanced sensor technology available
- Value detailed analytics tracking strength, endurance, and control separately
- Benefit from direction sensing to help manage bearing-down errors
- Prefer waterproof design for use during bath
- Can justify premium price for advanced features
Choose the iStim V2 ($125) if you:
- Cannot perform effective voluntary Kegel contractions
- Experienced significant nerve damage during delivery
- Prefer automatic muscle stimulation over voluntary exercises
- Don’t want smartphone or app dependency
- Have FDA-cleared medical device preference
Seek professional pelvic floor physical therapy if you:
- Have severe symptoms (multiple daily incontinence episodes)
- Experience pelvic pain during exercises or device insertion
- See no improvement after 8-12 weeks of consistent device training
- Had third or fourth degree perineal tears
- Have visible pelvic organ prolapse
- Want professional assessment before beginning home training
For many women, combining initial professional assessment with home device training provides the best outcomes. A physical therapist can identify your specific dysfunction pattern, ensure proper technique, and recommend the most appropriate device for your situation. You then continue rehabilitation at home with the device, returning for periodic professional check-ins.
What Are the Final Recommendations?
The evidence demonstrates that structured pelvic floor training produces clinically meaningful improvements for most postpartum women with mild to moderate dysfunction. Consistency matters more than device selection — women who maintain 3+ sessions weekly for 8-12 weeks achieve significant symptom reduction regardless of whether they use biofeedback or electrical stimulation.
The Perifit Care+ ($179) represents the best overall option for women seeking postpartum rehabilitation through a device combining evidence-based biofeedback with engaging gamification and condition-specific protocols. The specialized programs align with clinical recovery timelines and address common postpartum challenges.
For budget-conscious women, the standard Perifit ($149) delivers the same core biofeedback technology at $30 less, requiring only that you create your own progression schedule rather than following preset protocols. The iStim V2 ($125) serves women who cannot perform voluntary contractions effectively, using FDA-cleared electrical stimulation to strengthen muscles without active participation.
The Elvie Trainer ($199) justifies its premium price through advanced sensor technology providing more detailed feedback than competing devices, appealing to women who value comprehensive analytics and want the most sophisticated consumer option available.
Regardless of device selection, success requires consistency, patience, and appropriate expectations. Most women see measurable improvement within 8-12 weeks but may require 6-12 months for complete recovery depending on delivery complications and baseline severity. Pelvic floor rehabilitation represents an investment in long-term health that may help reduce dysfunction risk not only immediately postpartum but across decades as you age.
For women with severe symptoms or those who see no improvement after consistent device training, professional pelvic floor physical therapy provides assessment and options beyond what home devices can address. The devices work best as part of comprehensive postpartum recovery that includes appropriate nutrition, gradual return to physical activity, stress management, and professional support when needed.
Related Reading
- Best Pelvic Floor Trainer — comprehensive guide comparing all pelvic floor device types
- Elvie Trainer Review — detailed analysis of the premium biofeedback option
- Best Collagen Supplements for Women — supporting connective tissue repair during postpartum recovery
- Best Prenatal Vitamins — nutritional support during pregnancy and postpartum
- Best Iron Supplements for Women — addressing common postpartum anemia
- Postpartum Hair Loss Supplements — managing telogen effluvium after delivery
- Best Magnesium for Women Over 40 — muscle function and may help manage constipation
References
Yang S, Sang W, Feng J, Zhao H, Li X. The effect of rehabilitation exercises combined with direct vagina low voltage low frequency electric stimulation on pelvic nerve electrophysiology and tissue function in primiparous women: A randomised controlled trial. J Clin Nurs. 2017 Jul;26(13-14):1935-1946. PMID: 28252827.
Lee D, Jeung I, Jang J. Systematic review on maintaining pelvic floor health during pregnancy. Healthcare (Basel). 2025 Jan;13(2):156. PMID: 40492459.
Siafarikas F, Stær-Jensen J, Hilde G, Bø K, Ellström Engh M. The pelvic floor in young nulliparous women - a prospective comparative study using 4D ultrasound. Int Urogynecol J. 2024 Mar;35(3):515-524. PMID: 38290449.
Ye D, Liao L, Zhu Y, Liu X, Wang C. Effect of pelvic floor muscle (PFM) workout on postpartum pelvic floor muscle function recovery of primiparas: a randomized controlled trial. BMC Pregnancy Childbirth. 2022 Aug;22(1):632. PMID: 36078788.
Song Y, Zhong L, Liu Y, Zhang F. Status quo of pelvic floor muscle and its effect on pelvic floor rehabilitation in early stage after vaginal delivery. Transl Pediatr. 2022 Oct;11(10):1610-1619. PMID: 36397372.
Huang Y, Huang L, Cen L, Zhou J. Design of Exercise Nursing Program for Pelvic Floor Muscle Function Recovery at 42 Days Postpartum. Chinese Nursing Research. 2021. PMID: 34804191.
Zeng C, Wu B, Chen Z. Comparative study of the 5R postpartum rehabilitation system and aerobic exercise on postpartum recovery. Transl Pediatr. 2025 Jan;14(1):65-75. PMID: 40734253.
Sheng Y, Liu X, Kane Low L, et al. Association of pubovisceral muscle tear with functional capacity of urethral closure. Obstet Gynecol. 2019. PMID: 31765643.
Hitchcock R, Shaw JM, Niederauer S, et al. Association Between Measures of Trunk Recovery 5 to 10 Weeks Postpartum and Pelvic Floor Support and Symptoms 1 Year Postpartum. Female Pelvic Med Reconstr Surg. 2020. PMID: 32925422.
Von Aarburg N, Veit-Rubin N, Boulvain M, et al. Physical activity and urinary incontinence during pregnancy and postpartum: A systematic review and meta-analysis. Int Urogynecol J. 2021. PMID: 34839247.
Digital Tools to Support Postpartum Recovery: A Systematic Review. Matern Child Health J. 2025. PMID: 41133171.
ACOG Committee Opinion No. 804: Physical Activity and Exercise During Pregnancy and the Postpartum Period. Obstet Gynecol. 2020 Apr;135(4):e178-e188. PMID: 32217980.
Selman R, Early K, Battles B, et al. Maximizing Recovery in the Postpartum Period: A Timeline for Rehabilitation from Pregnancy through Return to Sport. Int J Sports Phys Ther. 2022 Oct;17(6):1170-1183. PMID: 36237644.
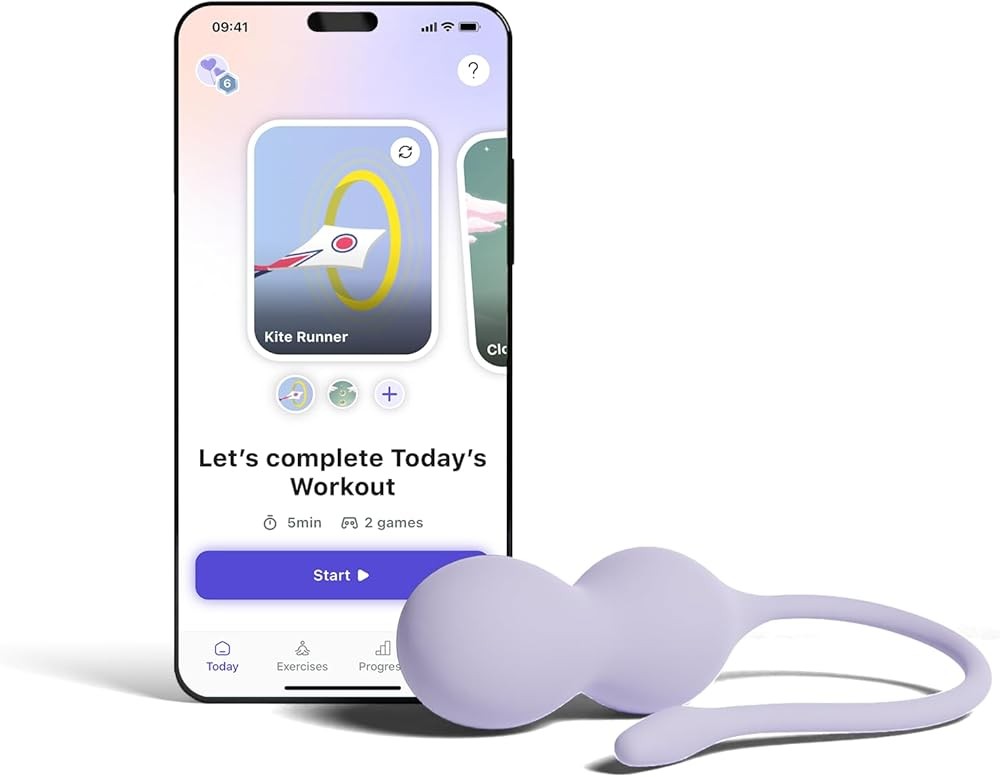
Perifit Care+ Pelvic Floor Exerciser
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
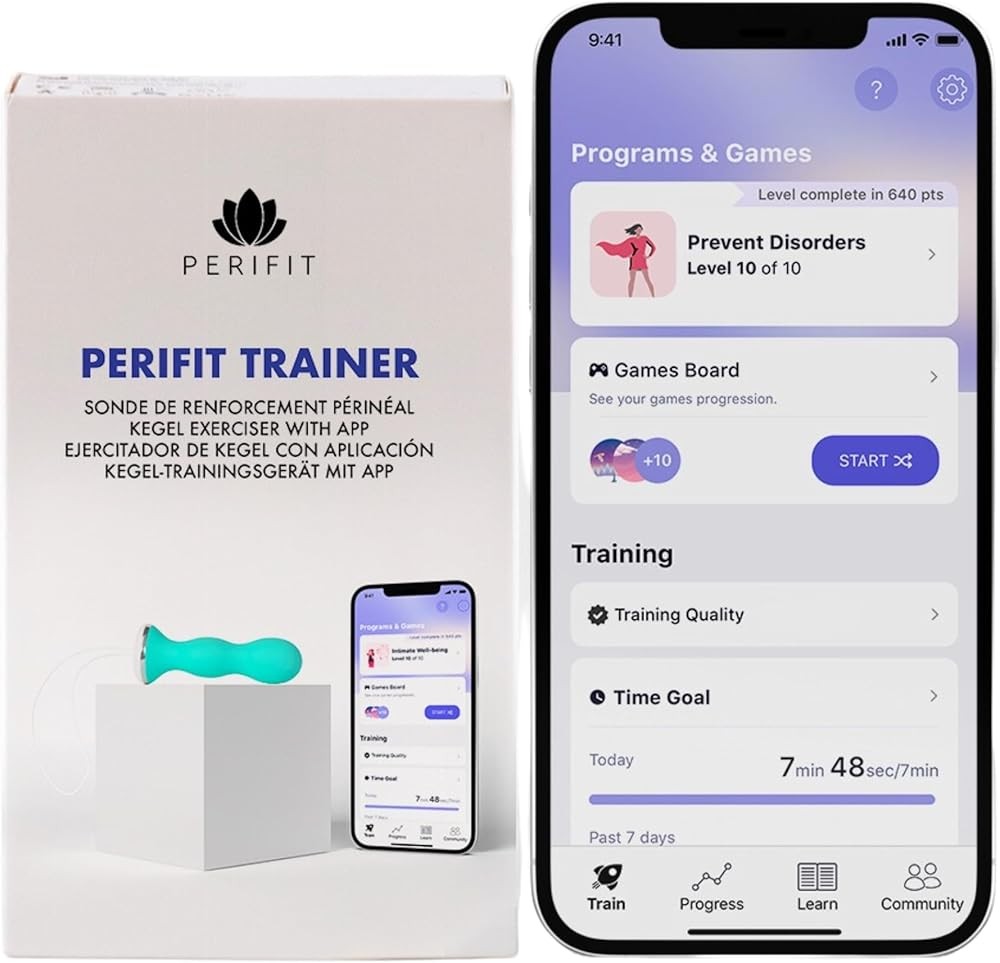
Perifit Pelvic Floor Exerciser
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
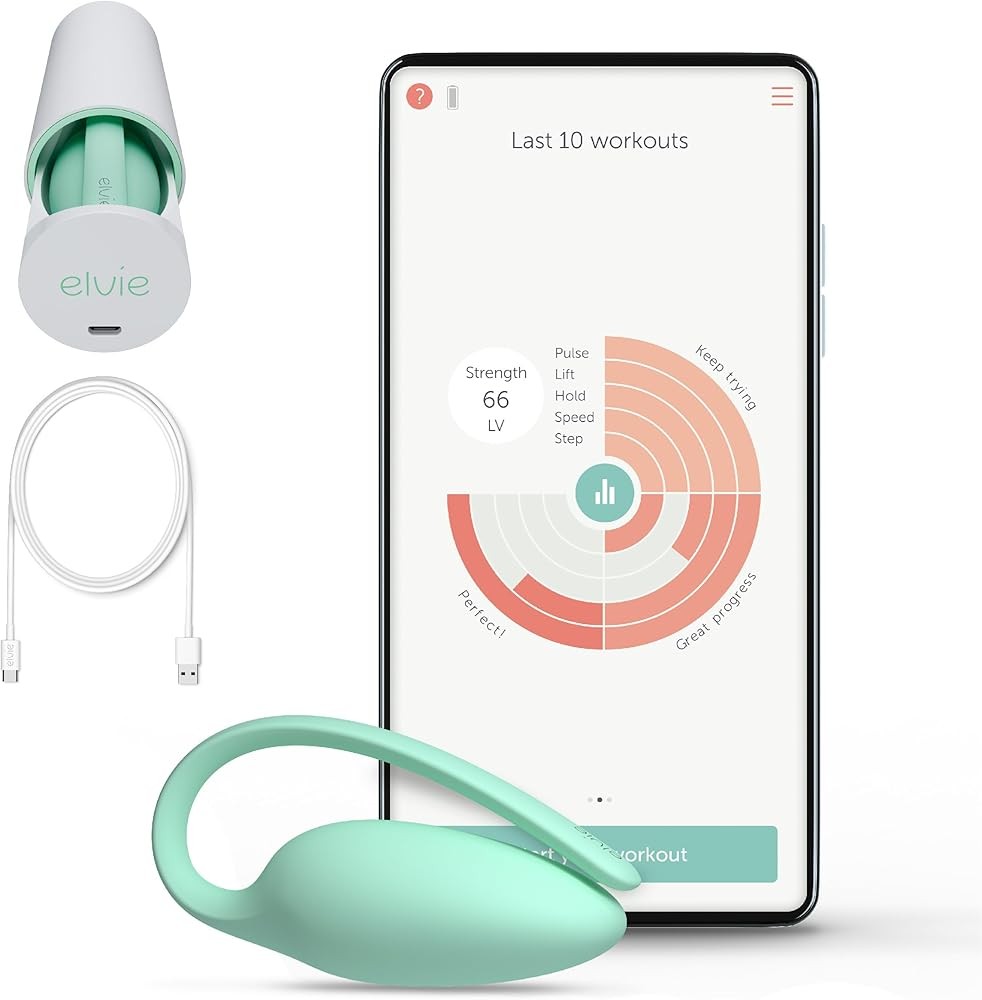
iStim V2 Kegel Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.