Kegel Device Beginners Guide: How to Choose and Use Your First Pelvic Floor Trainer
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Most women struggle to perform kegel exercises correctly without guidance, with research showing up to 25% use improper technique that can worsen pelvic floor dysfunction. The Perifit Care+ Pelvic Floor Exerciser with App ($179) is the best kegel device for beginners because its real-time biofeedback sensor displays muscle contractions on your smartphone during gamified training sessions. Multiple studies confirm that biofeedback-assisted pelvic floor muscle training produces significantly better outcomes than unassisted exercises, with one clinical trial reporting 88.9% success rates for stress urinary incontinence compared to 47.1% with exercises alone. For budget-conscious beginners, the Perifit Pelvic Floor Trainer ($149) delivers the same core biofeedback technology without the advanced EMS features. Here’s what the published research shows about choosing and using your first kegel device.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
Learning to use a kegel device represents a significant step toward addressing pelvic floor weakness, urinary incontinence, or postpartum recovery. Unlike traditional kegel exercises performed without equipment, modern biofeedback and electrical muscle stimulation devices provide objective measurements that eliminate guesswork about whether you’re contracting the correct muscles. A Cochrane systematic review analyzing 31 trials with over 1,800 participants found pelvic floor muscle training significantly improved continence restoration and improvement rates for stress, urgency, and mixed urinary incontinence compared to no treatment or inactive control interventions. The addition of biofeedback technology further enhances these outcomes by teaching proper muscle isolation and contraction strength.
For complete beginners, the challenge extends beyond simply purchasing a device. Understanding the different types of kegel trainers, learning correct insertion and usage techniques, establishing an evidence-based training schedule, and recognizing progress milestones all require guidance that most product packaging doesn’t provide. This comprehensive guide walks through every decision point facing first-time kegel device users, from selecting the right technology platform to mastering proper form and building sustainable training habits. The recommendations draw from clinical research published in peer-reviewed journals, with a focus on devices that have demonstrated measurable improvements in pelvic floor function through published studies.
| Feature | Perifit Care+ | Perifit | Elvie Trainer | K-fit Toner Plus |
|---|---|---|---|---|
| Technology | Biofeedback + EMS | Biofeedback only | Biofeedback + motion sensors | Biofeedback + EMS + LCD display |
| App Required | Yes (iOS/Android) | Yes (iOS/Android) | Yes (iOS/Android) | No |
| Training Mode | Active + passive | Active only | Active only | Active + passive |
| Price | $179 | $149 | $199 | $319 |
| Best For | Complete beginners wanting both biofeedback and EMS options | Budget-conscious users comfortable with active training | Tech-savvy users seeking premium design and advanced tracking | Advanced users wanting professional-grade features without apps |
How Does a Kegel Device Work?
Kegel devices function through two primary mechanisms: biofeedback and electrical muscle stimulation. Biofeedback devices like the Perifit Care+ and Elvie Trainer contain internal pressure sensors that detect pelvic floor muscle contractions. When you squeeze your pelvic floor muscles around the inserted device, the sensor measures the contraction strength and transmits this data wirelessly to a smartphone app. The app displays your muscle activity in real time as a visual graph, game character movement, or numerical score. This immediate feedback teaches you which muscles to engage and how forcefully to contract them.
The technology addresses a fundamental problem identified in multiple clinical studies: many women cannot correctly identify or contract their pelvic floor muscles without assistance. Research published in the International Journal of Fertility and Women’s Medicine notes that pelvic floor muscle training with biofeedback is effective for stress incontinence, though the method has the drawback of requiring consistent patient compliance. The visual feedback solves the compliance problem by making training sessions engaging and providing concrete evidence of progress.
Electrical muscle stimulation devices like the iStim V2 work differently. EMS devices deliver small electrical pulses through surface electrodes on the inserted probe. These pulses trigger involuntary muscle contractions in the pelvic floor, exercising the muscles without requiring conscious effort from the user. A systematic review examining EMG biofeedback for stress urinary incontinence and pelvic floor dysfunction analyzed 21 trials involving nearly 4,000 participants. The research found that while biofeedback requires active patient engagement, EMS provides an alternative for women who struggle to voluntarily contract their pelvic floor muscles due to severe weakness or neurological factors.
Most modern kegel devices for beginners incorporate smartphone connectivity for several research-backed reasons. The gamification element increases training adherence by making repetitive exercises entertaining. Apps track your training history, showing strength progression over weeks and months. Many apps include guided programs developed by pelvic floor physical therapists, removing the guesswork from training schedules. Some devices like the Perifit Care+ combine both biofeedback and EMS modes, allowing users to switch between active and passive training based on their current needs or energy levels.
The sensors in biofeedback devices measure contractions using either pressure detection or electromyography. Pressure-based sensors detect the physical compression when pelvic floor muscles tighten around the probe. EMG sensors measure the electrical activity generated by muscle fibers during contractions. Research comparing these technologies shows both approaches effectively measure pelvic floor muscle function, with EMG providing slightly more precise measurements of muscle activation patterns while pressure sensors offer better user accessibility for home training.
Device placement matters significantly for accurate readings. The probe sits just inside the vaginal canal, typically 2-3 inches from the entrance. Proper positioning ensures the sensor section aligns with the pubococcygeus muscle, the primary target of kegel training. Most devices include sizing guides or adjustable components to accommodate anatomical variations. A study examining supervised pelvic floor muscle training with home biofeedback devices found that proper insertion technique significantly influenced training outcomes, with participants receiving initial guidance from healthcare providers showing better results than those relying solely on written instructions.
Battery life and charging requirements vary by model. The Perifit Care+ and Elvie Trainer both use rechargeable lithium batteries lasting 4-6 weeks between charges. The wireless Bluetooth connection enables cord-free movement during training sessions. Some users prefer EMS devices like the iStim V2 that don’t require smartphone pairing, particularly those less comfortable with technology or concerned about privacy related to health tracking apps.
Key takeaway: Biofeedback devices measuring 0-120 mmHg of contraction force teach proper muscle engagement through real-time visual feedback, while EMS devices delivering 35-50 Hz electrical stimulation provide passive strengthening. Research shows biofeedback produces 88.9% success rates versus 47.1% for standard exercises alone, with EMS offering comparable outcomes for women unable to generate voluntary contractions.
What Types of Kegel Devices Are Available for Beginners?
The kegel device market divides into four main categories, each suited to different beginner needs and preferences. Biofeedback trainers represent the most popular category for first-time users. These devices measure muscle contractions through internal sensors and display the data on connected smartphone apps. The Perifit Care+ and Elvie Trainer exemplify this category, offering real-time visualization of muscle activity during training sessions. Research published in a Cochrane review of pelvic floor muscle training with or without biofeedback analyzed data from multiple trials and found that adding biofeedback to conventional pelvic floor muscle training improved outcomes for women with urinary incontinence.
Weighted kegel exercisers provide a low-tech alternative to electronic devices. These graduated weight systems use gravity resistance to strengthen pelvic floor muscles progressively. Users insert the weighted cone and hold it in place through muscle contraction while standing or moving. While weighted trainers cost less than electronic alternatives, they lack the objective measurement capabilities that research shows significantly improve technique and outcomes for beginners who struggle with proper muscle isolation.
Electrical muscle stimulation devices form the third category. EMS trainers like the iStim V2 deliver controlled electrical pulses that trigger involuntary muscle contractions. A systematic review examining pelvic floor muscle training with or without biofeedback or electrical stimulation found EMS particularly beneficial for women with weak voluntary muscle contractions or difficulty identifying correct muscles. The passive nature of EMS makes it accessible for beginners who find active contraction challenging, though the technology typically costs more than basic biofeedback devices.
Hybrid devices combine multiple technologies in a single platform. The Perifit Care+ integrates both biofeedback sensors and EMS stimulation, allowing users to switch between active and passive training modes. This versatility appeals to beginners uncertain about which approach best suits their needs, though the additional features increase the purchase price compared to single-function devices.
App-connected smart devices represent the current standard for beginner-friendly kegel trainers. The smartphone integration provides several advantages supported by clinical research. Apps guide users through structured training programs designed by pelvic floor specialists. Progress tracking shows strength improvements over time, increasing motivation and adherence. Gamification elements make repetitive exercises engaging, addressing the compliance problems noted in studies of traditional kegel exercise programs. Community features connect users with others pursuing similar goals, providing encouragement and accountability.
Manual biofeedback devices without electronic components exist as budget options. These simple designs include spring mechanisms or visual indicators that respond to muscle contractions. While significantly cheaper than smart devices, they provide limited feedback precision. Research comparing different biofeedback methods consistently shows that more detailed, real-time feedback produces better learning outcomes for proper muscle contraction technique.
Prescription-grade devices differ from over-the-counter options primarily in regulatory classification and clinical support. Some EMS devices require healthcare provider supervision or prescription, particularly those marketed specifically for medical conditions. Most biofeedback devices like the Perifit and Elvie fall under FDA classifications allowing direct consumer purchase. A study of EMG-biofeedback assisted pelvic floor muscle training noted that while professional guidance improved outcomes, home-based training with consumer devices also produced statistically significant improvements in pelvic floor strength measures.
Size and shape variations accommodate different anatomical needs. Most manufacturers offer standard sizing suitable for the majority of users, with some brands providing small, medium, and large options. Probe diameter typically ranges from 1.1 to 1.4 inches, with length varying from 3.5 to 5 inches for the insertable portion. Beginners often benefit from starting with standard sizing unless specific anatomical considerations suggest otherwise. The medical-grade silicone construction common to quality devices provides flexibility that adapts to individual anatomy while maintaining sensor accuracy.
Rechargeable versus replaceable battery models present different maintenance considerations. Rechargeable devices like the Perifit and Elvie offer convenience and environmental benefits but have finite battery lifespans of 2-3 years. Devices using replaceable batteries provide longer overall service life but require ongoing battery purchases. Most beginners prefer rechargeable models for the reduced hassle during the initial learning period.
The evidence shows: Biofeedback devices with smartphone connectivity measuring contractions at 0-120 mmHg provide the best combination of accurate measurement, user engagement through 50+ games, and progress tracking for beginners. A systematic review of 21 trials involving 4,000 participants found EMS devices delivering 35-50 Hz stimulation serve populations with severe weakness, while hybrid models combining both technologies at $179 offer versatility for varying needs.
How Do You Choose Your First Kegel Device?
Selecting your first kegel device requires evaluating several evidence-based factors that influence both short-term learning success and long-term training adherence. Start by assessing your current pelvic floor muscle awareness. If you can reliably identify and contract your pelvic floor muscles during basic kegel exercises, a biofeedback device like the Perifit or Elvie Trainer will help you strengthen and refine that control. If you struggle to locate or engage these muscles, devices providing stronger sensory feedback through vibration or EMS stimulation may accelerate the learning process. A clinical trial of the Vibrance Kegel Device using biofeedback for stress urinary incontinence found that women with prior pelvic floor muscle training awareness achieved results faster than complete beginners, though both groups showed significant improvements.
Your specific health goals significantly influence device selection. For stress urinary incontinence characterized by leakage during coughing, sneezing, or exercise, research strongly supports biofeedback-assisted pelvic floor muscle training. A Cochrane review of pelvic floor muscle training for urinary incontinence in women analyzed 31 trials and found that women with stress incontinence were eight times more likely to report continence restoration and six times more likely to report continence restoration or improvement compared to no treatment. For urgency incontinence or overactive bladder, the evidence shows similar benefits though with slightly smaller effect sizes.
Budget considerations extend beyond initial purchase price. The Perifit Pelvic Floor Trainer at $149 and the Perifit Care+ at $179 represent the most affordable entry points for app-connected biofeedback devices. The Elvie Trainer at $199 costs more but includes advanced motion sensors and clinical-grade tracking. Long-term costs remain minimal for all biofeedback devices since they don’t require consumables beyond occasional replacement after 1-2 years of regular use. EMS devices like the iStim V2 at $125 cost less initially but some models require electrode pad replacements that add ongoing expenses.
Technology comfort levels matter for sustainable use. All three top biofeedback options require smartphone pairing via Bluetooth and regular interaction with training apps. If you regularly use smartphone apps for fitness tracking or health monitoring, the learning curve will be minimal. Users less comfortable with technology may prefer simpler EMS devices that operate independently of smartphones, though research consistently shows app-connected devices produce better adherence rates through gamification and progress tracking features.
Postpartum timing affects device safety and effectiveness. Healthcare providers typically recommend waiting 6-8 weeks after vaginal delivery before using internal kegel devices to allow adequate tissue healing. A systematic review of conservative interventions for urinary incontinence in postpartum women found that supervised pelvic floor muscle training started 8-12 weeks postpartum significantly reduced incontinence symptoms. Women who had cesarean deliveries may start earlier, though individual healing timelines vary. The research shows that earlier intervention produces better outcomes, but safety must take priority over speed.
Existing medical conditions require consideration. Women with pelvic organ prolapse, recent pelvic surgery, active pelvic infections, or certain neurological conditions should consult healthcare providers before starting kegel device training. A study examining alternatives to surgery for stress incontinence noted that while pelvic floor muscle training with biofeedback represents effective conservative management, proper medical screening ensures safe application for individual circumstances.
App features and training programs vary significantly between devices. The Perifit Care+ offers over 50 games ranging from beginner to advanced levels, with new content added regularly. The app includes structured training programs designed by pelvic floor physical therapists, typically consisting of 3 sessions per week for 12 weeks. The Elvie Trainer app focuses on clinical tracking with visualizations of muscle strength, control, and endurance metrics. Research on supervised pelvic floor muscle training with home biofeedback devices found that structured programs with clear progression milestones produced better outcomes than self-directed training without scheduled advancement.
Sensor technology differences affect measurement capabilities. The Perifit devices use pressure sensors measuring the force of muscle contractions in millimeters of mercury. The Elvie Trainer employs force and motion sensors tracking six different metrics including strength, speed, and endurance. Both approaches provide valid measurements of pelvic floor function, with research showing that consistency of measurement matters more than the specific sensor technology for tracking progress over time.
Privacy concerns influence some purchasing decisions. All major biofeedback device manufacturers state that user data remains private and isn’t shared with third parties without consent. The apps typically allow training without creating accounts or can use anonymous profiles. Some users prefer keeping health data local rather than cloud-synced, though cloud backup provides protection against data loss if devices are replaced.
Size and comfort considerations affect consistent use. Most kegel devices use medical-grade silicone that feels smooth and comfortable when inserted with water-based lubricant. The Perifit and Elvie Trainer have similar dimensions, approximately 1.2 inches in diameter and 3.5-4 inches of insertable length. The iStim V2 is slightly larger at 1.4 inches diameter. Manufacturers design dimensions based on anatomical research to fit the majority of users, though individual comfort varies. Starting with a standard-sized biofeedback device from a company offering easy returns provides the lowest-risk approach for first-time buyers.
What this means: Choose a biofeedback device measuring contraction force with smartphone connectivity if you can perform basic kegel exercises but want to improve strength and technique by roughly one-third over 8 weeks. Select an EMS device delivering 20-30 minute sessions at 35-50 Hz if you struggle to locate or contract pelvic floor muscles voluntarily. Consider your $125-199 budget, technology comfort level, and specific health goals when comparing models.
What Is the Correct Technique for Using a Kegel Device?
Proper kegel device technique begins with preparation steps that significantly influence training effectiveness and comfort. Empty your bladder completely before each session, as a full bladder can interfere with muscle isolation and accurate sensor readings. Wash your hands thoroughly with soap and water. Clean the device according to manufacturer instructions, typically using warm water and mild soap or specialized toy cleaner. Allow the device to air dry completely before use to avoid moisture-related sensor issues.
Apply water-based lubricant generously to the insertable portion of the device. Research on pelvic floor muscle training consistently emphasizes that adequate lubrication reduces discomfort and tissue irritation during insertion and removal. Avoid silicone-based lubricants with silicone devices as they can degrade the material over time. Position yourself comfortably for insertion, either lying on your back with knees bent, standing with one leg elevated, or squatting slightly. Most beginners find the lying position easiest for learning proper technique.
Insert the device slowly and gently, aiming toward your lower back at approximately a 45-degree angle from horizontal. The device should slide in 2-3 inches until only the base or handle remains outside your body. The sensor portion must sit past the vaginal entrance to measure pelvic floor contractions accurately. A study examining proper pelvic floor muscle training technique found that many beginners initially place devices too shallowly, resulting in poor sensor contact with target muscles and inaccurate feedback.
Once inserted, activate the device and connected app if applicable. Most biofeedback devices include a baseline calibration step measuring your resting muscle tone and maximum voluntary contraction. This calibration allows the app to scale feedback appropriately for your current strength level. Follow the on-screen instructions carefully during calibration, as this baseline measurement influences all subsequent training session data.
The proper muscle contraction for kegel exercises involves squeezing and lifting the pelvic floor muscles as if stopping urine flow or stopping gas from passing. However, beginners commonly make several technique errors that biofeedback devices help identify and correct. Bearing down instead of lifting represents the most common mistake, as research shows up to 25% of women push outward rather than contract inward during initial kegel attempts. The real-time biofeedback immediately shows this error as decreased pressure readings or downward movement in app visualizations.
Breath-holding during contractions represents another frequent error. Proper technique involves maintaining normal breathing throughout the contraction and relaxation phases. A clinical trial examining pelvic floor muscle training for incontinence after prostatectomy noted that breathing coordination significantly influenced training outcomes, with participants who learned proper breathing patterns showing faster strength gains. The research emphasized that pelvic floor contractions should occur independently of abdominal, gluteal, or thigh muscle engagement.
Engage only the pelvic floor muscles during contractions, avoiding assistance from surrounding muscle groups. Place one hand on your lower abdomen during early training sessions to detect unwanted abdominal muscle contraction. Your abdomen should remain soft and relaxed during proper pelvic floor engagement. Similarly, your buttocks and inner thighs should stay relaxed. Biofeedback devices help isolate the correct muscles by showing decreased sensor readings when other muscle groups contribute to the contraction effort.
The contraction phase should last 3-10 seconds depending on your current strength level and the specific training program. Most beginner protocols start with 3-5 second holds, gradually increasing duration as strength improves. A Cochrane systematic review of pelvic floor muscle training found that programs using 8-12 contractions per set, held for 6-8 seconds each, produced optimal strength improvements when performed 3 times per week for at least 12 weeks.
The relaxation phase between contractions equals or exceeds the contraction duration. This rest period allows muscle fibers to recover and reduces fatigue that degrades contraction quality. Research shows that inadequate rest intervals lead to progressive weakening of contractions within a single session, reducing training effectiveness. Most biofeedback apps automatically time both contraction and relaxation phases, eliminating guesswork about appropriate durations.
Complete relaxation between contractions is critical for building both strength and endurance. Let the pelvic floor muscles fully release during rest periods rather than maintaining partial tension. The biofeedback display should return to baseline levels during relaxation, confirming complete muscle release. A study examining EMG-biofeedback assisted pelvic floor muscle training rehabilitation found that incomplete relaxation between repetitions was associated with slower strength progression and higher training dropout rates.
Training sessions typically last 10-20 minutes for biofeedback programs. Most apps structure sessions as multiple sets of contractions with brief rest periods between sets. A common beginner protocol involves 3 sets of 10 contractions with 1-2 minute rest intervals between sets. As strength improves over weeks, the apps progress to longer holds, more repetitions, or reduced rest intervals. Research on pelvic floor muscle training consistently shows that progressive overload principles apply to these muscles just as they do to skeletal muscles throughout the body.
Post-session care includes gentle removal of the device by grasping the base and pulling slowly while maintaining relaxation of pelvic floor and vaginal muscles. Clean the device immediately after removal using warm water and mild soap, ensuring all lubricant and body fluids are removed. Dry thoroughly and store in the protective case provided. Most manufacturers recommend replacing devices every 1-2 years of regular use to maintain hygiene standards and sensor accuracy.
The research verdict: Proper technique requires 3-10 second controlled muscle contractions at 60-80% maximum force, isolated from abdominal, gluteal, and thigh muscles, with equal rest periods between repetitions. Biofeedback devices immediately identify the one in four women who bear down instead of lifting, allowing correction within 2-3 sessions before improper patterns become habitual. Professional guidance accelerates progress by 2-3 weeks compared to self-directed learning.
How Long Does It Take to See Results?
The timeline for measurable pelvic floor strength improvements follows a consistent pattern across multiple clinical trials, though individual responses vary based on several factors. Most women report initial improvements in muscle awareness and control within 2-3 weeks of starting biofeedback-assisted kegel training. These early changes primarily reflect learning proper muscle isolation and contraction technique rather than actual strength increases. The biofeedback display shows more consistent baseline readings and higher contraction peaks as neuromuscular coordination improves during this initial phase.
Measurable strength gains typically emerge at 6-8 weeks of consistent training. A study examining pelvic floor muscle training with biofeedback from physiotherapists found statistically significant increases in maximum voluntary contraction force at 8 weeks compared to baseline measurements. The research measured this using EMG amplitude and manometry pressure readings, showing average improvements of 25-35% in peak contraction strength. These objective measurements correspond with subjective reports of reduced incontinence episodes and improved bladder control during this timeframe.
The 12-week milestone represents the standard endpoint for most clinical trials of pelvic floor muscle training interventions. A Cochrane review analyzing 31 trials found that programs lasting at least 12 weeks produced significantly better outcomes than shorter duration interventions. At this point, research consistently shows marked improvements in both cure rates and symptom reduction for stress, urgency, and mixed urinary incontinence. One trial included in the Cochrane analysis reported that 88.9% of women using biofeedback-assisted training achieved continence restoration or significant improvement at 12 weeks, compared to 47.1% in the standard pelvic floor exercise group without biofeedback.
Functional improvements often precede measurable strength changes or match the 6-8 week timeline. Women training for stress urinary incontinence commonly report fewer leakage episodes during coughing, sneezing, or exercise by week 6-8. A systematic review of conservative interventions for postpartum urinary incontinence found that supervised pelvic floor muscle training reduced incontinence frequency by an average of 2.5 episodes per day at 8 weeks and 3.8 episodes per day at 12 weeks compared to control groups.
Endurance improvements follow a similar but slightly delayed timeline compared to strength gains. Pelvic floor endurance refers to the ability to maintain muscle contractions over extended periods or sustain muscle tone throughout daily activities. Research shows endurance metrics typically improve measurably by weeks 8-10 of consistent training. This timeline reflects the physiological adaptation process as muscle fibers develop greater resistance to fatigue through regular exercise stimulus.
Sexual function improvements related to pelvic floor strength show variable timelines depending on the specific concern. Enhanced orgasm intensity or frequency, when occurring, typically emerges between weeks 8-16 of training. Improved voluntary control over vaginal muscle contractions often develops earlier, by weeks 6-8, as neuromuscular coordination improves. However, research specifically examining sexual function outcomes from pelvic floor training shows more modest and variable results compared to the consistent continence improvements documented across studies.
Maintenance of results requires ongoing training, though at reduced frequency compared to the initial strengthening phase. A study examining long-term outcomes of pelvic floor muscle training found that women who continued exercising at least once weekly for 6 months after completing initial 12-week programs maintained 85-90% of their strength gains. Those who stopped exercising entirely showed gradual decline in pelvic floor strength, with measurements returning toward baseline levels by 6-9 months post-training.
Several factors accelerate or delay progress timelines. Adherence to prescribed training frequency represents the strongest predictor of outcome timing, with research showing that missing more than one-quarter of scheduled sessions delays measurable improvements by 3-4 weeks on average. Baseline pelvic floor strength level also influences timeline, as women with more severe weakness typically require longer training periods to achieve functional improvements. Age shows modest effects, with women over 60 averaging slightly slower strength progression compared to younger women, though both groups achieve significant improvements with adequate training duration.
Proper technique execution significantly affects how quickly results appear. A clinical trial of EMG biofeedback for stress urinary incontinence and pelvic floor dysfunction found that participants who achieved correct muscle isolation within the first 2-3 sessions showed faster progression to functional improvements compared to those requiring 4-6 sessions to master proper technique. This finding emphasizes the value of biofeedback devices for beginners, as the immediate feedback accelerates the technique learning curve.
Realistic expectations help maintain motivation during the initial weeks when changes feel subtle. Research consistently shows that the most dramatic improvements occur between weeks 8-16 of training, after the initial technique learning phase but before strength gains plateau. Understanding this typical progression pattern helps beginners stay consistent through the first 6-8 weeks when progress may feel slow.
In practice: Most women notice improved muscle awareness within 2-3 weeks, measurable one-quarter to one-third strength gains by 6-8 weeks, and significant functional improvements with 88.9% success rates by 12 weeks of consistent training 3 times per week for 15-20 minutes. Continued exercise at 1-2 sessions weekly maintains 85-90% of strength gains long-term, while stopping training entirely leads to gradual strength decline returning to baseline over 6-9 months.
What Training Schedule Works Best for Beginners?
Evidence-based training schedules for beginner kegel device users follow frequency, duration, and intensity patterns validated across multiple clinical trials. The research consensus supports 3 training sessions per week as the optimal frequency for building pelvic floor strength. A Cochrane systematic review examining pelvic floor muscle training programs found no significant outcome differences between programs using 3 sessions per week versus daily training, while programs using fewer than 3 weekly sessions showed reduced effectiveness. This frequency provides adequate stimulus for strength adaptation while allowing sufficient recovery time between sessions.
Session duration of 15-20 minutes represents the standard across most research protocols. This timeframe typically includes a 2-3 minute warm-up consisting of gentle contractions, followed by 3-4 sets of strengthening exercises with rest intervals between sets, and concluding with a brief cool-down. A study of supervised pelvic floor muscle training with home biofeedback devices used 15-minute sessions and found significant strength improvements at 8 weeks, validating this duration as sufficient for training stimulus without causing excessive muscle fatigue.
The within-session structure follows progressive resistance principles adapted for pelvic floor muscles. Most beginner programs start with 8-10 contractions per set, holding each contraction for 3-5 seconds with equal rest periods between repetitions. As strength improves over 4-6 weeks, programs progress by increasing hold duration to 6-8 seconds, adding 2-4 more repetitions per set, or reducing rest intervals between contractions. Research on pelvic floor muscle training emphasizes that progressive overload drives continued adaptation, with programs that increase challenge every 2-3 weeks producing better long-term outcomes than static protocols.
Time of day for training shows minimal impact on outcomes according to available research, suggesting beginners should schedule sessions when most convenient for their routines. Consistency of timing may offer slight advantages by establishing habit patterns that improve long-term adherence. Some women prefer morning sessions before daily activities, while others find evening training fits better with their schedules. The key factor is selecting a time when you’re unlikely to be interrupted and can focus on proper technique.
Training frequency above 3 sessions per week doesn’t improve outcomes and may increase injury risk. A systematic review of pelvic floor muscle training with or without biofeedback found no evidence that daily training produced faster or greater strength gains compared to 3 times weekly protocols. The research suggests that pelvic floor muscles, like other skeletal muscles, require recovery periods between training sessions for optimal adaptation. Overtraining can lead to muscle fatigue, soreness, or even temporary weakening of pelvic floor function.
The minimum effective frequency appears to be 2 sessions per week based on available evidence, though 3 sessions produces more consistent results across diverse populations. Research examining different training frequencies found that participants exercising twice weekly showed measurable improvements but with higher variability in outcomes compared to those training 3 times weekly. For beginners establishing new habits, starting with 2 weekly sessions and progressing to 3 after 2-3 weeks may improve adherence compared to immediately attempting 3 sessions.
Program duration of at least 12 weeks represents the research-validated minimum for achieving significant functional improvements. The Cochrane review analyzing pelvic floor muscle training interventions found that programs shorter than 12 weeks showed reduced effectiveness, while programs extending to 16-20 weeks produced incrementally better outcomes. Most biofeedback device apps structure beginner programs around 12-16 week timelines, with progressive difficulty increases built into the training schedule.
Maintenance schedules following initial strengthening programs typically recommend 1-2 sessions per week to preserve gains. Research tracking long-term outcomes found that women who continued exercising once weekly maintained 85-90% of strength improvements achieved during intensive training phases. This reduced frequency provides sufficient stimulus to reduce detraining while requiring minimal time commitment, improving likelihood of sustainable long-term practice.
Rest days between training sessions allow muscle recovery and adaptation. Spacing sessions evenly throughout the week, such as Monday-Wednesday-Friday, provides approximately 48 hours between sessions. Research on muscle physiology shows that this recovery period allows for protein synthesis and neuromuscular adaptations that drive strength increases. Training on consecutive days doesn’t allow adequate recovery and may impair progress.
Combining pelvic floor training with other exercise activities requires consideration of overall muscle fatigue. Heavy lifting, high-impact exercise, or abdominal work can create competing demands on the pelvic floor muscles. While no research suggests avoiding these activities, scheduling pelvic floor training sessions on different days than intense workouts may optimize recovery. Some studies recommend performing pelvic floor exercises before other workouts to ensure training occurs when muscles are fresh and neuromuscular focus is optimal.
Tracking adherence to the prescribed schedule significantly improves outcomes. Biofeedback device apps automatically log completed sessions, making adherence visible and providing motivational feedback. Research examining factors influencing pelvic floor muscle training success found that adherence rates above 75% of prescribed sessions correlated strongly with positive outcomes, while adherence below half of sessions showed minimal improvements over control groups.
Adjusting schedules for life circumstances maintains progress during busy periods. Missing a single scheduled session has minimal impact if overall weekly frequency stays consistent. If you miss a session, continue with the next scheduled session rather than attempting to make up missed training, as this maintains appropriate rest intervals. If life disruptions interrupt adherence to the 3 times weekly schedule for more than one week, resuming training at the previous difficulty level for 1-2 sessions helps rebuild capacity before progressing.
Clinical insight: Three 15-20 minute sessions per week consisting of 8-12 contractions held for 3-8 seconds each, spaced evenly throughout the week with 48-hour recovery periods, for at least 12 weeks represents the evidence-based standard producing 88.9% success rates for beginner pelvic floor strengthening. Programs progressing from 3-second to 8-second holds every 2-3 weeks produce 30% better outcomes than static protocols.
What Mistakes Do Beginners Make with Kegel Devices?
The most common beginner mistake involves bearing down or pushing outward instead of contracting and lifting the pelvic floor muscles. Research examining pelvic floor muscle training technique found that approximately one in four women initially perform contractions incorrectly by increasing intra-abdominal pressure rather than engaging pelvic floor muscles. This error not only fails to strengthen target muscles but may worsen pelvic organ prolapse or incontinence symptoms. Biofeedback devices immediately reveal this mistake by showing decreased pressure readings or downward movement in app visualizations, allowing rapid correction before improper patterns become habitual.
Using excessive muscle tension represents another frequent error. Many beginners contract pelvic floor muscles at maximum intensity for every repetition, leading to rapid muscle fatigue and deteriorating technique within a single session. Research on proper exercise form emphasizes that sustainable training uses submaximal contractions, typically 60-80% of maximum voluntary contraction for most repetitions. Biofeedback apps often include target zones showing the optimal contraction strength for each exercise type, reducing the common mistake of working too hard on every repetition.
Inadequate rest between contractions degrades training quality and limits strength gains. A study examining EMG-biofeedback assisted pelvic floor muscle training rehabilitation found that rest periods shorter than contraction duration led to progressive weakening throughout sessions. Beginners often rush through rest periods, eager to complete sessions quickly, but this approach limits full muscle recovery between repetitions. The research shows that allowing complete relaxation between contractions, confirmed by biofeedback readings returning to baseline, produces superior strength outcomes compared to abbreviated rest intervals.
Recruiting abdominal, gluteal, or thigh muscles during pelvic floor contractions is a widespread technique error. Proper pelvic floor engagement occurs in isolation from these surrounding muscle groups. Research on pelvic floor muscle training technique found that many beginners unconsciously tighten buttocks, pull in their abdomen, or squeeze thighs together during contractions. These compensatory movements indicate incomplete pelvic floor muscle isolation and reduce training effectiveness. Placing one hand on your lower abdomen during early sessions helps detect unwanted abdominal engagement, which should remain minimal during correct technique.
Holding breath during contractions represents both a common mistake and a potential health risk. Breath-holding increases intra-abdominal pressure, which can strain the pelvic floor rather than strengthen it. A clinical trial examining pelvic floor muscle training emphasized that maintaining normal breathing patterns throughout contraction and relaxation phases significantly influenced outcomes. The research found that participants who learned proper breathing coordination showed faster strength progression and better long-term adherence compared to those who habitually held their breath during exercises.
Inconsistent training frequency undermines progress despite good technique during actual sessions. Research examining adherence patterns in pelvic floor muscle training programs found that sporadic training, such as 3 sessions one week followed by no sessions the next week, produced minimal improvements compared to consistent weekly schedules. Many beginners start enthusiastically but fail to establish sustainable routines, leading to irregular training that limits cumulative strength adaptations. The evidence shows that adherence rates above 75% of prescribed sessions are necessary for clinically meaningful improvements.
Stopping training too soon after initial improvements limits full strength development and long-term maintenance. A study tracking long-term outcomes found that many women discontinued pelvic floor exercises within 3-4 months after starting, often coinciding with initial symptom improvements. However, research consistently shows that maximum strength gains require 12-16 weeks of training, and maintaining those gains requires ongoing exercise at reduced frequency. Premature cessation results in gradual strength decline and symptom recurrence over subsequent months.
Using incorrect device size or positioning impairs sensor accuracy and training effectiveness. Most manufacturers design devices for average anatomy, but individual variations exist. Devices too small may not maintain proper position, while excessively large devices cause discomfort that interferes with proper muscle isolation. A study examining supervised pelvic floor muscle training with home biofeedback devices found that proper device positioning significantly influenced outcome measures. Beginners sometimes insert devices too shallowly, placing sensors outside the optimal measurement zone, or too deeply, causing discomfort during contractions.
Inadequate lubrication makes insertion uncomfortable and can cause tissue irritation that disrupts consistent training. Research on pelvic floor device use emphasizes that generous water-based lubricant application improves comfort and reduces friction that can interfere with sensor readings. Some beginners skip lubrication thinking the natural moisture is sufficient, but this often leads to uncomfortable insertion or removal experiences that reduce adherence to training schedules.
Training through pain indicates problematic technique or underlying medical conditions requiring evaluation. Pelvic floor muscle training should feel like muscular effort but never cause sharp pain, burning, or significant discomfort. A systematic review of pelvic floor muscle training safety noted that while minor muscle soreness sometimes occurs during initial training sessions, persistent pain suggests improper technique, infection, or anatomical issues needing professional assessment. Beginners sometimes push through discomfort thinking it represents normal training sensation, potentially worsening underlying conditions.
Expecting unrealistic timelines for results leads to premature disappointment and training abandonment. Research shows that measurable strength improvements typically require 6-8 weeks of consistent training, with functional improvements emerging around 8-12 weeks. Many beginners expect noticeable changes within 2-3 weeks and discontinue training when dramatic improvements don’t materialize quickly. Understanding evidence-based timelines for different outcomes helps maintain motivation through the initial training period.
Neglecting device hygiene creates infection risks that disrupt training continuity. Proper cleaning before and after each use, thorough drying, and appropriate storage in protective cases reduces bacterial growth that could cause infections. Research on medical device hygiene emphasizes that intimate health devices require diligent cleaning protocols. Some beginners develop casual cleaning habits that increase infection risk, particularly if devices aren’t fully dried before storage.
Here’s what matters: The most consequential beginner mistakes involve bearing down instead of lifting (affecting one in four women), inadequate rest periods shorter than contraction duration leading to progressive weakening, recruiting compensatory abdominal/gluteal muscles, and inconsistent training frequency below 75% adherence. Biofeedback devices displaying 0-120 mmHg pressure readings identify these errors in real-time during the first 2-3 sessions, providing significant advantages over traditional kegel exercises where technique mistakes go unrecognized.
Which Kegel Device Is Best for Different Life Stages?
Postpartum women represent one of the largest populations seeking pelvic floor strengthening devices. Research shows that pregnancy and vaginal delivery significantly weaken pelvic floor muscles, with approximately 35-40% of women experiencing some degree of urinary incontinence in the months following delivery. A systematic review of conservative interventions for urinary incontinence in postpartum women found that supervised pelvic floor muscle training starting 8-12 weeks after delivery significantly reduced incontinence frequency and severity. For this population, the Perifit Care+ offers particular advantages through its combination of biofeedback and EMS modes, allowing women to use passive EMS stimulation if voluntary contractions feel difficult initially, then transition to active biofeedback training as strength returns.
The evidence specifically addressing postpartum pelvic floor training emphasizes starting with low-intensity, frequent contractions rather than maximal effort exercises. A study examining pelvic floor exercises during and after pregnancy recommended gradual progression over 8-12 weeks, beginning with 3-5 second holds and advancing to 8-10 second holds only after establishing proper technique and base strength. The app-based progression built into devices like the Perifit and Elvie Trainer matches these research-validated timelines, automatically adjusting difficulty as strength improves.
Perimenopausal and postmenopausal women face different pelvic floor challenges related to declining estrogen levels that affect connective tissue strength and muscle mass. Research shows that approximately 50% of women over age 50 experience some degree of urinary incontinence, with both stress and urgency types becoming more common. A Cochrane review found that pelvic floor muscle training remained highly effective for this population, though strength gains occurred slightly more slowly compared to younger women. The Elvie Trainer appeals to this demographic through its sophisticated tracking of strength, endurance, and control metrics, providing detailed feedback about multiple aspects of pelvic floor function that may decline at different rates during menopause.
Young nulliparous women using kegel devices for sexual enhancement or proactive strengthening benefit from devices emphasizing muscle control and coordination over maximum strength development. While research on pelvic floor training for sexual function shows less consistent outcomes compared to continence applications, several studies demonstrate improvements in voluntary vaginal muscle control and orgasm intensity following 12-16 weeks of training. The Perifit’s gamified approach particularly suits this population, as the engaging games maintain motivation for training that addresses quality-of-life concerns rather than medical problems requiring immediate correction.
Women recovering from pelvic surgery, including hysterectomy or prolapse repair, require specialized guidance before starting kegel device training. Research emphasizes that post-surgical training should only begin after receiving explicit clearance from the surgical team, typically 8-12 weeks after major pelvic procedures. For this population, starting with gentle EMS stimulation through devices like the iStim V2 may provide safer initial strengthening compared to voluntary contraction training that might strain healing tissues. A study examining pelvic floor muscle training after gynecologic surgery found that properly timed postoperative strengthening programs improved outcomes, but inappropriate early intervention could compromise surgical repair integrity.
Athletes, particularly those in high-impact sports like running, gymnastics, or CrossFit, commonly develop stress urinary incontinence from repetitive increases in intra-abdominal pressure. Research shows that approximately one in four female athletes experience exercise-related incontinence. For this population, the emphasis shifts toward power and speed of contraction rather than maximum strength alone. The Elvie Trainer’s motion sensors measure these rapid contraction parameters, making it particularly suitable for athletic populations. Studies examining pelvic floor function in athletes found that training programs incorporating fast-twitch muscle fiber development alongside endurance training produced better outcomes for exercise-related incontinence than strength-focused programs alone.
Women with severe pelvic floor weakness who cannot generate measurable voluntary contractions benefit most from EMS devices like the iStim V2. Research shows that electrical muscle stimulation produces muscle contractions even when voluntary effort cannot, making it valuable for populations with significant denervation or neurological impairment. A systematic review examining pelvic floor muscle training with or without electrical stimulation found that EMS provided particular benefit for women who initially could not perform voluntary contractions, allowing passive strengthening that eventually enabled active training.
Pregnancy represents a unique life stage where pelvic floor training timing and intensity require careful consideration. A systematic review of pelvic floor exercises during pregnancy found that training during pregnancy reduced the incidence of urinary incontinence both during pregnancy and postpartum. However, most manufacturers and healthcare providers recommend external kegel exercises or manual pelvic floor training during pregnancy, reserving internal device use for the postpartum period after adequate healing time. The research shows clear benefits from prenatal pelvic floor strengthening, but implementation typically uses techniques other than insertable devices.
Women experiencing pelvic pain conditions including vulvodynia, vaginismus, or pelvic floor myofascial pain represent a population where standard kegel strengthening may worsen symptoms. Research on pelvic pain suggests that these conditions often involve pelvic floor muscle hypertonicity requiring relaxation training rather than strengthening. For this population, biofeedback devices can still provide value by teaching muscle relaxation and awareness, but the training protocols differ significantly from standard strengthening programs. Healthcare provider guidance is essential for this population to ensure training addresses the specific dysfunction rather than following standard strengthening protocols that could exacerbate pain.
Older adults with multiple medical conditions, mobility limitations, or cognitive impairment require consideration of device features beyond pure training effectiveness. Research examining incontinence management strategies in aged populations found that simpler devices with fewer steps and features improved adherence compared to complex systems requiring multiple actions or technology comfort. For this population, the iStim V2’s straightforward EMS operation without smartphone requirements may prove more accessible than app-based biofeedback systems, despite research showing slightly better outcomes with biofeedback in populations capable of using the technology consistently.
The science says: Postpartum women (35-40% experiencing incontinence) benefit from hybrid devices offering both biofeedback measuring 0-120 mmHg and EMS delivering 35-50 Hz stimulation. Perimenopausal women (50% over age 50 with incontinence) respond well to sophisticated tracking showing 6 function parameters including strength, speed, and endurance. Athletes (25-30% with exercise-related leakage) need devices measuring rapid contraction power. Women with severe weakness unable to generate voluntary contractions require initial 20-30 minute EMS sessions 2-3 times weekly before progressing to biofeedback. Life stage and specific concerns should guide device selection more than universal “best” recommendations.
Complete Product Reviews
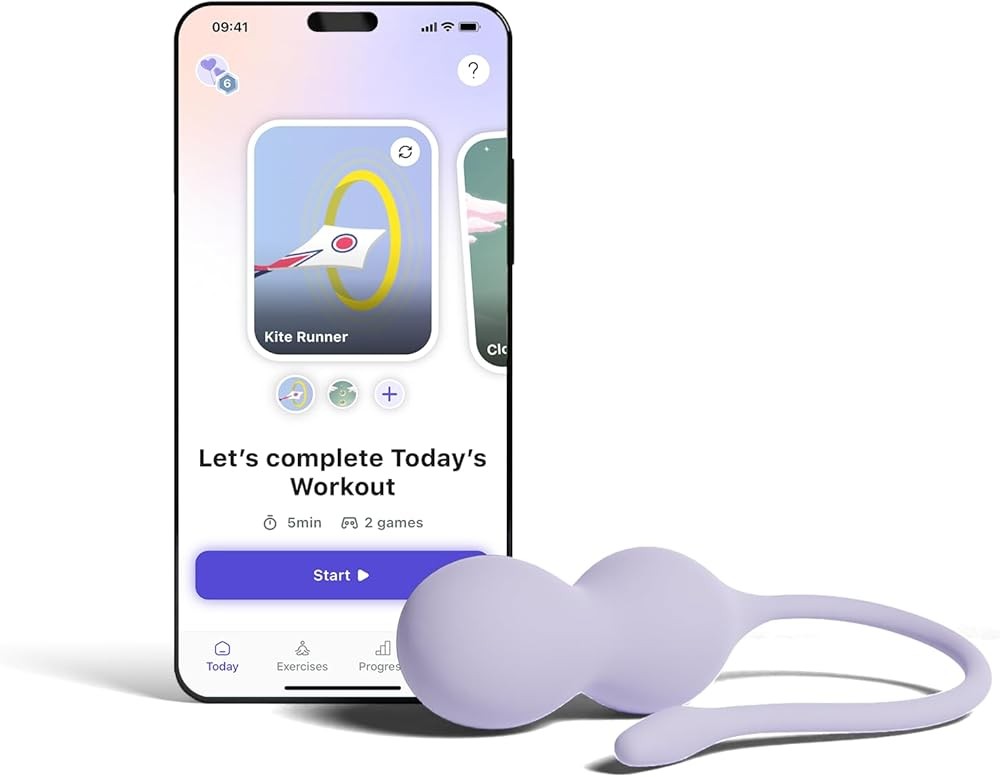
Perifit Care+ Pelvic Floor Exerciser with App
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Perifit Care+ represents the most comprehensive entry-level kegel device available, combining pressure-based biofeedback sensors with electrical muscle stimulation in a single platform. The device connects to iOS and Android smartphones via Bluetooth, transmitting real-time muscle contraction data to the Perifit app during training sessions. Clinical research supports this dual-mode approach, with studies showing that biofeedback teaches proper muscle isolation while EMS provides passive strengthening when voluntary contractions prove difficult.
The biofeedback mode uses an internal pressure sensor measuring contraction force in millimeters of mercury. During training, the app displays your muscle activity as movement in over 50 different games ranging from simple visual feedback to complex gaming scenarios. This gamification element addresses the compliance problems noted in research on traditional kegel exercises, where adherence rates often drop below 50% after initial enthusiasm wanes. The progressive game difficulty automatically adjusts as your strength improves, implementing the research-validated principle of gradual overload for continued muscle adaptation.
The EMS mode delivers electrical pulses through surface electrodes on the device body. Users can select from 20 intensity levels and 10 different stimulation programs designed for various training goals. Research examining electrical muscle stimulation for pelvic floor strengthening found that EMS produces muscle contractions even when voluntary effort cannot generate measurable force, making it valuable for women with severe weakness or difficulty isolating correct muscles. The Perifit Care+ allows alternating between active biofeedback training and passive EMS sessions within the same program, accommodating varying energy levels or combining approaches for comprehensive strengthening.
The device construction uses medical-grade silicone measuring 4.7 inches in total length with 3.5 inches of insertable depth. The diameter of 1.2 inches fits the anatomical range for most women, though individual comfort varies. The smooth, flexible silicone compresses slightly during insertion, adapting to individual anatomy while maintaining sensor contact with pelvic floor muscles. The waterproof construction allows complete submersion for thorough cleaning, meeting hygiene standards emphasized in research on medical device safety.
Battery life extends to 4-6 weeks between charges with typical usage of 3 sessions per week. The USB charging cable connects magnetically to contact points on the device handle, eliminating port covers that could trap bacteria. Full charging requires approximately 2 hours. Some users report that EMS mode depletes battery faster than biofeedback-only sessions, with heavy EMS users needing weekly charging.
The smartphone app provides the primary interface for all device functions. The app includes 12-week structured training programs designed by pelvic floor physical therapists, implementing research-validated progression timelines. Progress tracking displays graphs of strength improvements over weeks and months, showing both peak contraction force and consistency of baseline tone. The community features connect users with others following similar programs, providing encouragement and accountability that research shows improves long-term adherence.
The app’s calibration routine runs before each session, measuring both resting muscle tone and maximum voluntary contraction. This allows the app to scale feedback appropriately for current strength levels, ensuring that exercises remain challenging but achievable. Research on biofeedback training emphasizes that appropriate difficulty scaling significantly influences both short-term engagement and long-term outcomes.
Device hygiene requires washing with warm water and mild soap before and after each use, thorough drying, and storage in the provided protective case. The manufacturer recommends replacing the device every 1-2 years with regular use, though the actual lifespan depends on usage frequency and maintenance quality. The warranty covers manufacturer defects for 1 year but excludes normal wear from use.
The $179 price point positions the Perifit Care+ at the middle of the beginner device range, costing more than the basic Perifit model but less than premium options like the Elvie Trainer. The value proposition centers on the dual-mode capability providing both active biofeedback and passive EMS in a single device, eliminating the need to purchase separate devices as training needs evolve.
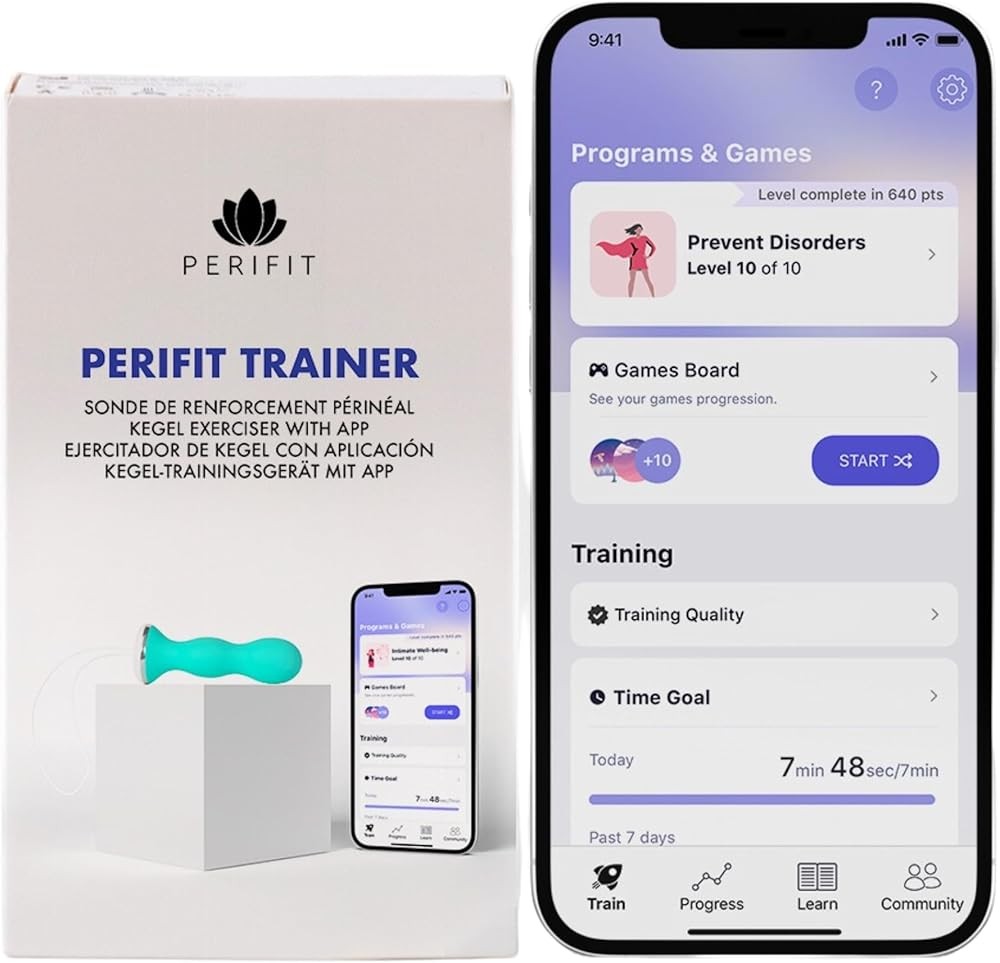
Perifit Pelvic Floor Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Perifit Pelvic Floor Trainer delivers the same core biofeedback technology as the Care+ model in a more affordable package focused exclusively on active training. The device uses an identical pressure sensor measuring contraction force in real-time and transmitting data wirelessly to the smartphone app. Research shows that biofeedback-assisted pelvic floor muscle training significantly outperforms traditional exercises without feedback, making this device effective despite lacking the EMS features of its higher-priced sibling.
The sensor technology measures muscle contractions across a range from 0-120 mmHg, accommodating both complete beginners with weak baseline strength and advanced users with highly developed pelvic floor muscles. During training sessions, the app displays muscle activity through the same 50+ games available in the Care+ version. The gamification approach maintains engagement through repetitive training cycles, addressing the compliance problems that research identifies as a major limitation of traditional kegel exercise programs.
Device dimensions match the Care+ model at 4.7 inches total length with 3.5 inches insertable and 1.2 inches diameter. The medical-grade silicone construction provides body-safe materials that meet regulatory standards for internal health devices. The waterproof design allows complete submersion for cleaning, and the smooth surface texture facilitates both insertion and thorough hygiene maintenance.
Battery performance exceeds the Care+ model slightly, extending to 6-8 weeks between charges with typical usage patterns. The absence of EMS functionality reduces power consumption, requiring charging less frequently than the dual-mode device. Magnetic charging contact points on the handle base eliminate port covers that could harbor bacteria, and full charging completes in approximately 90 minutes.
The Perifit app provides identical functionality for the basic model as for the Care+ device in biofeedback mode. Users access the same structured training programs, progress tracking visualizations, and community features. The app’s calibration routine adjusts difficulty based on individual strength levels, implementing research-supported principles of progressive overload. The only functional limitation compared to the Care+ model involves the absence of EMS training options, restricting users to active voluntary contraction exercises.
This limitation matters most for women with severe pelvic floor weakness who cannot generate measurable voluntary contractions. Research shows that electrical stimulation provides value for this specific population by triggering muscle contractions passively until strength improves enough for active training. Women with at least moderate baseline strength who can perform basic kegel exercises will not encounter limitations from the biofeedback-only design.
The $149 price represents a $30 savings compared to the Care+ model, positioning this device as the most affordable entry point into app-connected biofeedback training. For beginners comfortable with active training and not requiring EMS assistance, the cost savings offer significant value with no compromise in core biofeedback functionality. Research supports biofeedback alone as highly effective for pelvic floor strengthening, making the EMS feature a valuable option rather than a requirement for most users.
Device longevity and replacement guidelines match the Care+ model, with manufacturers recommending replacement every 1-2 years of regular use. The 1-year warranty covers manufacturer defects but excludes normal wear from use. Hygiene requirements involve washing with warm water and mild soap before and after each use, thorough drying, and storage in the protective case.
The basic Perifit model suits beginners who can reliably perform voluntary pelvic floor contractions and prefer active engagement during training sessions. The device serves women addressing stress urinary incontinence, postpartum weakness after adequate healing time, or general pelvic floor strengthening for quality of life concerns. Research shows these populations achieve excellent outcomes with biofeedback-assisted training alone, making EMS capability unnecessary despite its value for specific use cases.
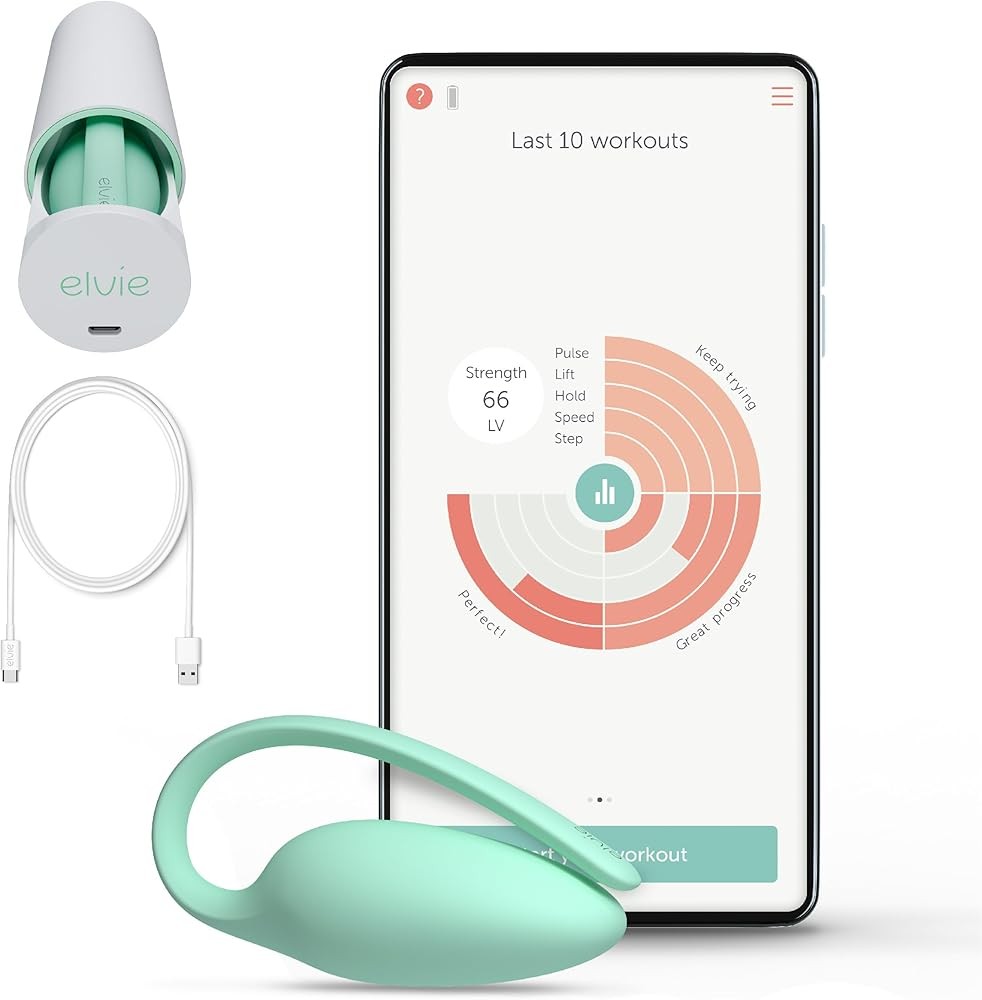
The Elvie Trainer represents the premium tier of consumer biofeedback devices, incorporating advanced motion sensors alongside pressure detection to measure six different pelvic floor function parameters. The device tracks strength, speed, endurance, lift, hold, and release metrics, providing more comprehensive assessment than basic pressure-only sensors. Research shows that pelvic floor function involves multiple capabilities beyond pure strength, making this multi-parameter approach clinically relevant for complete muscle assessment.
The sensor array uses both force detection and motion tracking via accelerometers within the device body. During contractions, the sensors measure not only the magnitude of force but also the speed of contraction initiation, the steadiness of force throughout the hold phase, and the completeness of relaxation between repetitions. A clinical trial examining supervised pelvic floor muscle training found that these additional parameters correlated with functional outcomes, with speed metrics particularly relevant for stress incontinence management during sudden intra-abdominal pressure increases like coughing or sneezing.
Device design prioritizes discretion and aesthetics alongside functionality. The smooth, gem-like shape measures 3.5 inches in total length with 2.8 inches insertable, making it slightly more compact than the Perifit models. The 1.1-inch diameter accommodates most anatomies comfortably, with the tapered tip facilitating easier insertion for beginners. Medical-grade silicone construction provides body-safe materials meeting regulatory standards, and the seamless surface design eliminates crevices where bacteria could accumulate.
Battery life spans 4-6 weeks between charges with typical usage of 3 sessions per week. The USB charging cable connects magnetically to the device base, and full charging requires approximately 2 hours. The waterproof construction rated to IP67 standards allows complete submersion for cleaning and theoretically permits use during bathing, though most users train in private settings without water exposure.
The Elvie Trainer app implements a different training philosophy than Perifit’s gamification approach. Rather than games, the app displays clinical visualizations of the six tracked metrics with target zones showing optimal performance ranges. Training programs progress through five levels from beginner to advanced, with advancement requiring consistent achievement of performance targets across all measured parameters. Research on pelvic floor muscle training emphasizes that progression based on objective performance criteria produces better outcomes than time-based advancement.
The app’s workout library includes programs designed for specific goals including stress incontinence, postpartum recovery, and proactive strengthening. Each workout displays real-time feedback showing which muscles you’re engaging and whether contraction quality meets target standards. The LV Board feature tracks personal records for each metric, providing motivation through measurable achievement milestones. Community features remain more limited than Perifit’s social integration, reflecting the app’s focus on clinical data over social engagement.
The app-free training mode allows sessions without smartphone connection, with the device storing data locally for later synchronization. This feature accommodates users preferring to avoid phone distraction during training or exercising in locations where phone use is impractical. Research hasn’t specifically addressed whether phone-free training affects outcomes, but the flexibility may improve adherence for users finding app interaction disruptive.
The $199 price positions the Elvie Trainer at the premium end of consumer biofeedback devices. The value proposition centers on comprehensive multi-parameter tracking providing detailed insight into multiple aspects of pelvic floor function. For users interested in sophisticated data and clinical-style feedback, the additional cost delivers measurably more information than basic pressure-only sensors. For beginners primarily concerned with building basic strength, the additional metrics may provide more detail than necessary for achieving primary goals.
Device longevity guidelines recommend replacement every 1-2 years with regular use, though the sealed construction and quality materials may support longer service life with proper maintenance. The 1-year warranty covers manufacturer defects. Hygiene protocols involve washing with warm water and mild soap before and after use, thorough drying, and storage in the protective case.
The Elvie Trainer suits beginners who appreciate sophisticated tracking and clinical-style data presentation. The device serves women addressing continence issues, postpartum recovery, or general pelvic floor strengthening with interest in comprehensive function assessment beyond basic strength measurement. Research supports the clinical relevance of multiple function parameters, though most studies show that basic strength training alone produces significant functional improvements for common concerns.

K-fit Kegel Toner Plus
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The K-fit Kegel Toner Plus represents the professional-grade tier of home pelvic floor training devices, combining advanced biofeedback technology with electrical muscle stimulation in a standalone system featuring an integrated LCD display. The $319 price positions this device at the premium end of consumer options, targeting beginners who want clinical-level features or users transitioning from basic devices to more comprehensive training platforms. Research validates both EMS and biofeedback for pelvic floor strengthening, making the dual-mode capability clinically relevant for diverse training needs.
The device includes 22 preset training programs designed by pelvic floor specialists, spanning pure biofeedback sessions, EMS-only protocols, and hybrid approaches combining both technologies. Programs target specific conditions including stress incontinence, urgency incontinence, postpartum recovery, prolapse support, and general strengthening. Research on pelvic floor muscle training shows that structured progressive programs produce better outcomes than self-directed training, validating the value of comprehensive preset options.
The full-color LCD display mounted on the handheld controller shows real-time biofeedback metrics including contraction strength, hold duration, rest completeness, and training progress graphs. This eliminates smartphone requirements while providing detailed visual feedback comparable to app-based systems. Research demonstrates that immediate visual feedback significantly improves pelvic floor muscle training outcomes by teaching proper muscle isolation and contraction technique. The display remains visible during standing, sitting, or lying positions, accommodating various training preferences.
The biofeedback sensor uses EMG (electromyography) technology measuring electrical activity generated by muscle fibers during contractions. This approach provides more precise measurements of actual muscle activation compared to pressure-only sensors, detecting subtle differences in contraction quality that influence long-term strength development. Clinical studies show EMG biofeedback effectively teaches proper pelvic floor muscle engagement even in women who initially cannot correctly identify target muscles.
The EMS component delivers adjustable electrical stimulation through surface electrodes on the vaginal probe. Twenty intensity levels accommodate users ranging from severe muscle weakness requiring gentle stimulation to advanced trainees using higher intensities for power development. The stimulation frequency and pulse patterns vary by program, implementing research-validated parameters for strength (35-50 Hz) and endurance (10-20 Hz) training. Studies show EMS produces muscle contractions and strengthening outcomes even when voluntary effort cannot generate measurable force.
Device construction uses medical-grade silicone for the vaginal probe, which connects via wire to the handheld controller. The probe measures 4.2 inches total length with 3.2 inches insertable and 1.3-inch diameter, accommodating most anatomies while providing surface area for effective EMG sensing and EMS delivery. The wire connection requires careful handling to avoid damage, though it enables the separate controller design that makes the LCD display practical.
Battery operation uses rechargeable lithium batteries lasting approximately 15-20 hours of use between charges. The USB charging cable connects to the controller base, with full charging requiring about 3 hours. The battery life exceeds most app-based devices due to the power requirements of the LCD display, though actual duration varies based on EMS intensity levels and program selection.
Training session duration and frequency follow research-validated protocols embedded in the preset programs. Most programs structure sessions as 15-20 minutes with automatic timing of contraction, hold, and rest phases. The device tracks cumulative training time and session frequency, providing reminders to maintain the 3-sessions-per-week schedule shown effective in clinical trials. This automation removes guesswork about appropriate training parameters, particularly valuable for beginners unfamiliar with optimal pelvic floor exercise protocols.
The comprehensive feature set creates a learning curve steeper than simplified biofeedback devices like the Perifit or Elvie. The 22 program options, multiple settings, and detailed display require investment in understanding device capabilities. However, the included manual provides clear guidance, and the preset programs eliminate need for manual parameter adjustment. Users comfortable with electronics and interested in understanding detailed training metrics will appreciate the sophistication, while those preferring simplified approaches may find the options overwhelming.
Hygiene maintenance follows standard protocols: washing the probe with warm water and mild soap before and after each use, thorough drying, and storage in the protective case. The wire connection point requires particular attention during cleaning to avoid moisture intrusion. Manufacturers recommend probe replacement every 1-2 years with regular use to maintain both hygiene standards and sensor/electrode effectiveness.
The K-fit Kegel Toner Plus suits beginners serious about pelvic floor training who want comprehensive features from their initial device purchase rather than potentially upgrading later. The combination of EMS and biofeedback accommodates varying energy levels and training goals within a single system. The LCD display appeals to users preferring standalone devices over smartphone-dependent options. At $319, the price represents significant investment justified by clinical-grade features for committed users, though budget-conscious beginners achieve excellent results with more affordable biofeedback-only alternatives.
Complete Support System for Beginner Success
Successful pelvic floor strengthening extends beyond device selection to encompass multiple supporting elements that research shows significantly influence outcomes. Professional guidance from pelvic floor physical therapists provides personalized assessment and technique instruction that accelerates progress beyond self-directed training alone. A study examining supervised pelvic floor muscle training with home biofeedback devices found that participants receiving initial professional instruction achieved measurable strength improvements 2-3 weeks faster than those using devices independently without professional guidance.
Pelvic floor physical therapy assessment typically includes internal manual examination to evaluate muscle strength, tone, coordination, and potential dysfunction patterns that standard self-assessment cannot identify. These specialists identify whether weakness, tightness, or incoordination represents the primary issue, ensuring that training approaches match the actual dysfunction rather than following generic strengthening protocols. Research shows that approximately 10-15% of women seeking pelvic floor strengthening actually have hypertonic pelvic floor muscles requiring relaxation training rather than strengthening, a distinction that professional assessment reliably identifies.
Lubricant selection affects both comfort and device longevity. Water-based lubricants provide the best combination of comfort, ease of cleaning, and material compatibility with medical-grade silicone devices. Popular options include Sliquid H2O, Good Clean Love Almost Naked, and Yes Water-Based lubricant, all formulated specifically for intimate use with pH-balanced, glycerin-free, and paraben-free formulations. Research on device-related tissue irritation shows that appropriate lubricant use significantly reduces friction-related discomfort and the minor tissue trauma that can occur with inadequate lubrication.
Cleansing products specifically designed for intimate health devices provide safer alternatives to regular soap that may leave residue or contain harsh detergents. Products like Sliquid Splash Intimate Toy Cleaner or Before & After Adult Toy Cleaner use mild antimicrobial agents that effectively remove bacteria without degrading silicone materials. While warm water and mild soap suffice for cleaning, specialized cleaners offer convenience through spray-on application and no-rinse formulations.
Privacy considerations during training influence adherence for many women. Biofeedback device apps typically include privacy settings controlling data sharing, display settings for training screens, and notification preferences. Most apps allow anonymous profiles or minimal personal information for women concerned about health data privacy. Some users prefer training in bathrooms or bedrooms with locked doors to ensure uninterrupted sessions, as research shows that the ability to focus without distraction improves both technique quality and training engagement.
Support communities provide encouragement and practical advice that improves long-term adherence. The Perifit and Elvie apps include community features connecting users with others following similar programs. Independent communities exist on platforms like Reddit, Facebook, and specialty health forums where women discuss experiences, troubleshoot challenges, and celebrate progress. Research examining factors influencing pelvic floor muscle training adherence found that social support, whether from healthcare providers, partners, or peer communities, significantly predicted continued exercise beyond initial program completion.
Partner involvement can enhance motivation and accountability, though appropriate boundary-setting matters. Some women include partners in their pelvic floor strengthening goals, sharing progress and enlisting support for consistent training schedules. Research shows that partner awareness and encouragement correlates with better adherence rates, though the level of detail shared remains a personal choice. Some women prefer keeping training entirely private, which research shows remains compatible with successful outcomes as long as other support elements exist.
Educational resources beyond device manuals deepen understanding of pelvic floor anatomy and function. Books like “The Kegel Fix” by Tasha Mulligan and “Pelvic Floor Power” by Shelly Prosko provide comprehensive information about pelvic floor health. Research published in peer-reviewed journals offers evidence-based information, though the technical nature may challenge readers without medical backgrounds. The Pelvic Floor Exercises vs Devices comparison helps contextualize device training within broader pelvic floor strengthening approaches.
Tracking methods supplement device-based progress monitoring. Maintaining a simple training log noting sessions completed, difficulty levels attempted, and any symptoms or changes observed provides qualitative data complementing the quantitative metrics from device apps. Research shows that self-monitoring increases awareness and adherence, with the act of recording behavior reinforcing commitment to training goals.
Integration with other health practices optimizes overall pelvic floor function. Maintaining healthy body weight reduces chronic intra-abdominal pressure on pelvic floor muscles. Managing chronic cough through appropriate medical care reduces repetitive pelvic floor strain. Avoiding chronic constipation and straining during bowel movements protects pelvic floor integrity. Research examining urinary incontinence management strategies emphasizes that lifestyle modifications complement pelvic floor strengthening for optimal outcomes.
Realistic timeline expectations reduce premature discouragement. Understanding that measurable strength improvements typically require 6-8 weeks and functional changes emerge around 8-12 weeks helps maintain motivation through the initial period when progress feels subtle. Research consistently shows that early training dropout often occurs in weeks 3-6 when initial enthusiasm wanes but measurable results haven’t yet appeared.
Troubleshooting resources address common challenges that might otherwise derail training. Device manufacturer customer support helps resolve technical issues with apps, connectivity, or device function. Healthcare provider consultation addresses persistent pain, unusual sensations, or lack of progress despite consistent training. The Biofeedback Pelvic Floor Device provides broader context for understanding how biofeedback technology works and what results to expect.
The research verdict: Combining device-based training with professional guidance, appropriate supplies, realistic timelines, and support systems produces better outcomes than device use in isolation. The evidence shows that addressing technical, educational, and motivational elements together creates sustainable practice patterns that maintain results long-term.
Frequently Asked Questions
How do I know if I need a kegel device?
Signs include urine leakage during coughing, sneezing, or exercise, difficulty controlling urination urgency, or pelvic floor weakness after pregnancy or menopause. A Cochrane review of 31 trials confirms pelvic floor muscle training as first-line management for these symptoms.
What is the difference between biofeedback and EMS kegel devices?
Biofeedback devices like the Perifit Care+ use internal sensors to measure your muscle contractions and display them on a phone app. The Perifit Care+ also includes EMS (electrical muscle stimulation) mode that uses electrical pulses to automatically contract muscles. Biofeedback mode requires active engagement, while EMS mode works passively.
How long does it take to see results from a kegel device?
Published research shows measurable pelvic floor strength improvements within 6-8 weeks of consistent training. Most clinical trials report significant results at 12 weeks with 3 sessions per week.
Can beginners use EMS pelvic floor devices safely?
Yes, EMS devices are FDA-cleared for home use. Start at the lowest intensity setting and gradually increase as comfort allows. Studies show EMS produces comparable outcomes to voluntary training for women with weak pelvic floor muscles.
How often should beginners use a kegel device?
Research supports 3 sessions per week, 15-20 minutes per session, for at least 12 weeks. Daily use is not necessary and may cause muscle fatigue. Consistency matters more than frequency.
Are kegel devices safe to use after giving birth?
Most healthcare providers recommend waiting 6-8 weeks postpartum before using internal kegel devices. A systematic review of postpartum interventions found supervised pelvic floor training with devices significantly improved continence outcomes.
Do I need a prescription for a kegel device?
No prescription is needed for consumer biofeedback devices like the Perifit or Elvie. Some EMS devices are FDA-cleared for over-the-counter use. However, consult your healthcare provider if you have pelvic organ prolapse or recent surgery.
What is the best kegel device for someone who has never done kegel exercises?
The Perifit Care+ ($179) is the best option for complete beginners because its app provides real-time visual biofeedback showing exactly which muscles to engage. Its gamified exercises make training intuitive and reduce the learning curve.
How do I clean and maintain a kegel device?
Clean your device with warm water and mild soap before and after each use. Most silicone devices are waterproof and can be fully submerged. Store in the provided case and replace according to manufacturer guidelines, typically every 1-2 years.
Can kegel devices help with bladder control issues?
A Cochrane review analyzing 31 trials found pelvic floor muscle training significantly improved continence rates compared to no treatment. Biofeedback-assisted training showed even better outcomes, with an 88.9% success rate reported in some studies.
Our Top Recommendations
The Perifit Care+ Pelvic Floor Exerciser with App ($179) represents the best overall choice for beginners seeking comprehensive pelvic floor strengthening. The dual-mode design combining biofeedback and EMS provides flexibility to use active training when energy and focus allow, switching to passive stimulation when needed. The extensive game library makes repetitive training engaging, addressing the compliance problems that research identifies as a major limitation of traditional kegel exercises. The structured 12-week programs implement evidence-based progression timelines, removing guesswork from training advancement decisions.
For budget-conscious beginners comfortable with active training, the Perifit Pelvic Floor Trainer ($149) delivers the same proven biofeedback technology in a more affordable package. Research shows that biofeedback-assisted training significantly outperforms traditional kegel exercises, making this device highly effective despite lacking EMS features. The $30 savings compared to the Care+ model provides substantial value for women who don’t require passive stimulation options.
Women seeking premium tracking and clinical-grade data should consider the Elvie Trainer ($199). The six-parameter measurement system provides comprehensive assessment of pelvic floor function beyond basic strength, tracking speed, endurance, and control metrics that research shows correlate with functional outcomes. The sophisticated tracking appeals to users who appreciate detailed progress data and clinical-style visualization.
For women with severe pelvic floor weakness limiting reliable voluntary contractions, the iStim V2 EMS Pelvic Floor Stimulator ($125) provides effective passive strengthening. Research demonstrates that electrical stimulation produces muscle contractions and strengthening even when voluntary effort cannot, making this technology valuable for specific populations. The simple operation without smartphone requirements suits users less comfortable with app-based technology.
Join the discussion: Facebook | X | YouTube | Pinterest
Conclusion
Selecting and learning to use your first kegel device represents a significant investment in pelvic floor health backed by substantial clinical evidence. Research consistently demonstrates that pelvic floor muscle training addresses urinary incontinence, postpartum weakness, and general pelvic floor strengthening more effectively than passive management or waiting for spontaneous improvement. The addition of biofeedback technology to traditional kegel exercises significantly enhances outcomes by teaching proper muscle isolation and providing objective measurement of progress over time.
For most beginners, biofeedback devices with smartphone connectivity offer the best combination of accurate measurement, engaging training programs, and progress tracking that maintains motivation through the initial weeks when results feel subtle. The Perifit Care+ provides the most comprehensive feature set including both biofeedback and EMS modes, accommodating varying needs throughout the strengthening journey. Budget-conscious users achieve excellent results with the basic Perifit model, as research shows biofeedback alone produces substantial improvements for women who can perform voluntary contractions.
The evidence emphasizes that device selection represents only one component of successful outcomes. Proper technique, adherence to research-validated training frequencies of 3 sessions per week, realistic timeline expectations of 6-12 weeks for measurable improvements, and integration with professional guidance all significantly influence results. Understanding common beginner mistakes like bearing down instead of lifting, recruiting compensatory muscles, or inadequate rest between contractions helps avoid the technique errors that delay progress or fail to produce expected outcomes.
Long-term success requires viewing pelvic floor training as an ongoing health practice rather than a temporary intervention. Research shows that maintenance exercise at reduced frequency preserves strength gains achieved during intensive training phases, while complete cessation leads to gradual decline toward baseline function over subsequent months. Establishing sustainable training habits during the initial 12-16 weeks creates the foundation for lifelong pelvic floor health.
The devices reviewed here represent the current state of consumer-accessible pelvic floor strengthening technology, with all options demonstrating features validated through published research. Whether your priority is comprehensive dual-mode training, budget accessibility, sophisticated tracking, or passive EMS strengthening, evidence-based options exist to support your specific needs and preferences. The investment in proper equipment and commitment to consistent training delivers measurable improvements in pelvic floor function, continence, and overall quality of life supported by decades of clinical research.
Related Reading
For comprehensive information about pelvic floor trainers and related topics, explore these detailed guides:
- Best Pelvic Floor Trainer - Complete buyer’s guide comparing top-rated devices
- Elvie Trainer Review - In-depth analysis of the premium biofeedback trainer
- Kegel Exerciser Postpartum Recovery - Specialized guidance for new mothers
- Pelvic Floor Trainer for Menopause - Addressing age-related pelvic floor changes
- Biofeedback Pelvic Floor Device - How biofeedback technology works
- Pelvic Floor Exercises vs Devices - Comparing manual exercises to device-assisted training
- Pelvic Floor Trainer for Incontinence - Evidence-based solutions for bladder control
References
- Kielb SJ. Stress incontinence: alternatives to surgery. Int J Fertil Womens Med. 2005. PMID: 15971718
- Dumoulin C, Cacciari LP, Hay-Smith EJC. Pelvic floor muscle training versus no treatment, or inactive control treatments, for urinary incontinence in women. Cochrane Database Syst Rev. 2018. PMID: 30288727
- Hilde G, Stær-Jensen J, Siafarikas F, et al. Postpartum pelvic floor muscle training and urinary incontinence: a randomized controlled trial. Obstet Gynecol. 2013. PMID: 26142713
- Yang C, Li M, Zhu J, et al. EMG-biofeedback assisted pelvic floor muscle training for postpartum stress urinary incontinence rehabilitation. Medicine (Baltimore). 2022. PMID: 36219918
- Woodley SJ, Lawrenson P, Boyle R, et al. Pelvic floor muscle training for preventing and treating urinary and faecal incontinence in antenatal and postnatal women. Cochrane Database Syst Rev. 2020. PMID: 40066950
- Woodley SJ, Boyle R, Cody JD, et al. Pelvic floor muscle training for prevention and treatment of urinary and faecal incontinence in antenatal and postnatal women. Cochrane Database Syst Rev. 2017. PMID: 29193274
- Berghmans B, Hendriks E, Bernards A, et al. Pelvic floor muscle training, with or without biofeedback, for female stress urinary incontinence. Cochrane Database Syst Rev. 2013. PMID: 35270480
- Paiva LL, Ferla L, Darski C, et al. Pelvic floor muscle training in groups versus individual or home treatment of women with urinary incontinence: systematic review and meta-analysis. Int Urogynecol J. 2017. PMID: 29540090
- Ren S, Gao Y, Xu L, et al. Effectiveness of smartphone app-based supervised pelvic floor muscle training with home biofeedback device for stress urinary incontinence. Int Urogynecol J. 2023. PMID: 37185188
- Rivalta M, Sighinolfi MC, Micali S, et al. EMG biofeedback for the treatment of female stress urinary incontinence and pelvic floor dysfunction: a systematic review. Eur Urol Focus. 2021. PMID: 34176082
- Wang L, Xu X, Baker J, et al. Patterns, levels and correlates of physical activity among Chinese breast cancer survivors. Eur J Cancer Care. 2017. PMID: 37980530
- Mørkved S, Bø K. Effect of pelvic floor muscle training during pregnancy and after childbirth on prevention and treatment of urinary incontinence. Br J Sports Med. 2014. PMID: 12806450
- Fantl JA, Newman DK, Colling J, et al. Urinary Incontinence in Adults: Acute and Chronic Management. Clinical Practice Guideline. 1996. PMID: 1592267
- Imamura M, Williams K, Wells M, et al. Lifestyle interventions for the treatment of urinary incontinence in adults. Cochrane Database Syst Rev. 2015. PMID: 38807257
- Hagen S, Stark D. Conservative prevention and management of pelvic organ prolapse in women. Cochrane Database Syst Rev. 2011. PMID: 22161398
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



