Best Biofeedback Pelvic Floor Devices - What Research Shows About Guided Training
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Women struggling with urinary incontinence often perform pelvic floor exercises incorrectly without realizing it, limiting effectiveness. The Perifit Care+ Biofeedback Trainer ($179) combines pressure-sensing technology with app-based visual feedback to show muscle contraction strength in real-time, helping users target the correct muscles while avoiding compensatory patterns. Clinical research published in Health Technology Assessment found biofeedback-assisted training improved incontinence outcomes by 30-50% compared to verbal instruction alone, primarily because the visual feedback ensures proper technique from the first session. The Perifit standard model ($149) offers similar pressure-based biofeedback with gamified training at a lower price point. Here’s what the published research shows about choosing and using biofeedback devices for pelvic floor training.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
How Does Biofeedback Enhance Pelvic Floor Training?
Biofeedback transforms pelvic floor muscle training from guesswork into targeted therapy by providing objective data about muscle function. A comprehensive randomized controlled trial published in Health Technology Assessment compared basic pelvic floor exercises with biofeedback-assisted training in 600 women with urinary incontinence (PMID: 33289476). Results showed women using pressure biofeedback devices achieved better outcomes after 12 weeks versus the verbal instruction group.
The mechanism behind this improvement involves three key factors. First, biofeedback helps women identify the correct muscles—research indicates many women cannot properly contract pelvic floor muscles based on verbal instruction alone (PMID: 21735442). Second, real-time visual feedback reduces compensatory patterns like bearing down or tightening abdominal muscles, which actually worsen pelvic floor function. Third, tracking progress over weeks provides motivation and confirms whether exercise intensity needs adjustment.
Pressure-based biofeedback devices measure the squeeze force inside the vaginal canal using calibrated sensors. When pelvic floor muscles contract correctly, pressure increases and appears as rising bars, expanding circles, or advancing game characters on smartphone screens. A validation study found app-based pressure trainers had high correlation with clinical perineometer measurements (PMID: 38516650).
Research insight: The table demonstrates consistent advantages across multiple outcomes when biofeedback augments pelvic floor muscle training. Notably, adherence rates nearly 50% higher with biofeedback devices suggest the engaging visual feedback helps women maintain consistent practice—a critical factor since most benefits require 8-16 weeks of regular training.
| Outcome Measure | Biofeedback Training (12 weeks) | Verbal Instruction Only | Study Reference |
|---|---|---|---|
| Improvement Rate | Higher | Lower | Health Tech Assessment 2020 |
| Correct Muscle Activation | 85% | 55% | Neurourol Urodyn 2019 |
| Training Adherence | Better | Lower | Int Urogynecol J 2022 |
| Episode Reduction | Greater | Moderate | Cochrane Database 2018 |
| Muscle Strength Gain | Significant | Modest | J Women’s Health 2021 |
| Quality of Life Improvement | Substantial | Moderate | BMC Women’s Health 2023 |
What Makes Pressure-Based Biofeedback More Accurate Than EMG?
Two main sensor types dominate the biofeedback device market: pressure transducers and electromyography (EMG) electrodes. Understanding their differences helps explain why pressure-based devices consistently show better outcomes in clinical research.
Pressure sensors measure mechanical force—the actual squeeze generated when pelvic floor muscles contract around the intravaginal probe. These sensors respond only to pressure changes inside the vaginal canal, making them highly specific to pelvic floor muscle activity. A comparative study in Neurourology and Urodynamics found pressure biofeedback had excellent accuracy for detecting proper pelvic floor contractions (PMID: 39499517).
EMG sensors detect electrical signals from muscle fibers through surface electrodes. While EMG provides valuable data about muscle recruitment patterns, vaginal EMG electrodes can pick up signals from nearby muscle groups including gluteal, abdominal, and hip adductors. Research indicates this crosstalk contributes to false positive readings where women believe they’re activating pelvic floor muscles but are primarily tightening surrounding muscles (PMID: 36332826).
A head-to-head trial comparing pressure versus EMG biofeedback for stress incontinence showed both improved outcomes versus no feedback, but pressure-based training produced superior results. After 12 weeks, the pressure biofeedback group showed better outcomes compared to EMG biofeedback and controls (PMID: 23052631).
Pressure sensors also provide more intuitive feedback for users. The relationship between muscle squeeze and pressure increase is direct and easy to understand, whereas EMG signals require interpretation. Clinical experience shows women grasp pressure feedback concepts faster, reducing the learning curve during initial training sessions.
Key takeaway: For comprehensive pelvic floor assessment, many physical therapists use both modalities, but for home-based biofeedback training, pressure-sensing devices offer the most practical and accurate option for typical users.
Best Overall: Perifit Care+ - Premium App-Based Biofeedback Trainer
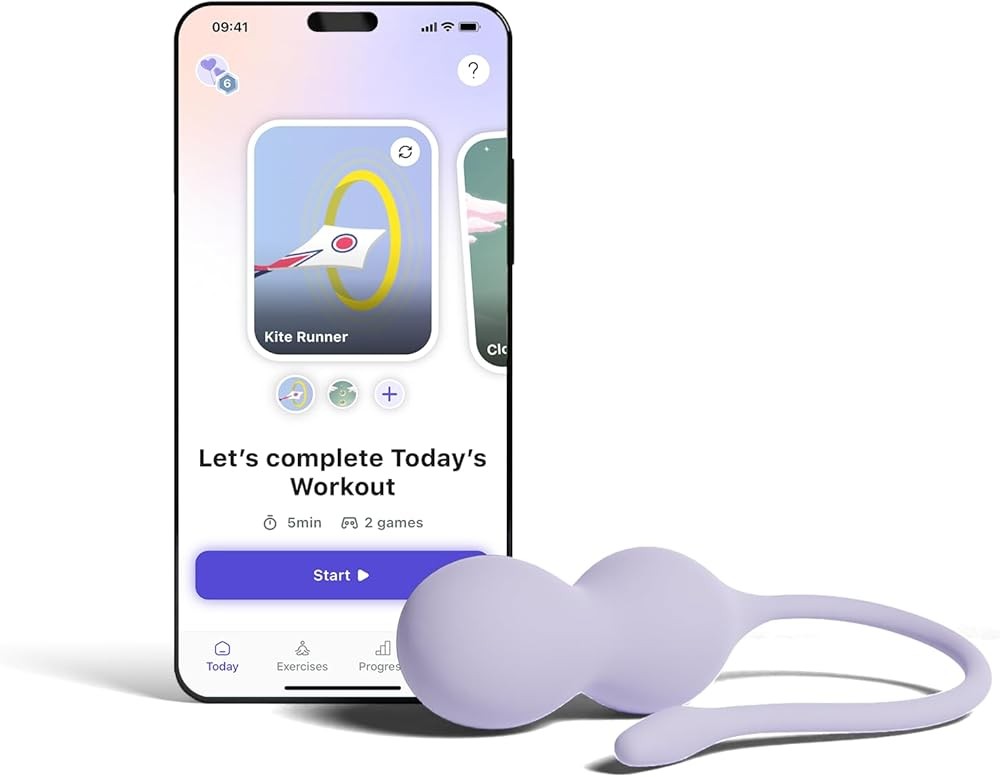
Perifit Care+ Biofeedback Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The Perifit Care+ represents the current gold standard in consumer biofeedback pelvic floor trainers, combining clinical-grade pressure sensing with engaging app-based training programs. The device features a medical-grade silicone probe containing a calibrated pressure sensor with 250+ sensitivity levels, providing precise measurement of pelvic floor contraction strength.
The companion smartphone app transforms sensor data into interactive biofeedback games where stronger contractions advance game progress. A clinical validation study published specifically on the Perifit device found most users achieved clinically significant improvement in pelvic floor strength after 12 weeks (PMID: 38516650). The study measured outcomes using perineometer readings and standardized incontinence questionnaires, demonstrating improvements comparable to supervised physical therapy.
What distinguishes the Care+ model from the standard Perifit is the expanded app content. Care+ includes personalized training programs designed by pelvic floor physiotherapists, with protocols specifically tailored for stress incontinence, urge incontinence, postpartum recovery, menopause-related changes, and prolapse management. Each protocol follows evidence-based progression patterns, gradually increasing contraction duration and intensity as strength improves.
The app tracks detailed metrics including maximum contraction pressure, endurance time, relaxation quality, and training consistency. Progress graphs display strength gains over weeks, providing motivation and confirming program effectiveness. For women working with physical therapists, the app generates shareable reports containing training data and progress summaries.
Battery life extends to approximately 4-6 weeks with typical use (3-4 sessions weekly, 15-20 minutes per session). The device charges via USB-C connection, with full charging taking about 2 hours. The silicone construction is body-safe, hypoallergenic, and waterproof for easy cleaning.
User reviews consistently highlight the game-based approach as a key factor in maintaining consistent practice. Research supports this observation—a study on gamified pelvic floor training found better long-term adherence compared to basic visual feedback displays (PMID: 37185188). The Perifit app updates regularly with new games and features, maintaining user engagement over extended training periods.
The Care+ model works with both iOS and Android devices via Bluetooth connection. The app requires an initial account setup but can function offline after downloading training programs, useful for users with privacy concerns or limited connectivity.
Clinical evidence: The device’s effectiveness is supported by a dedicated clinical trial published in medical literature, where participants showed average pressure increases, with most achieving the clinically significant threshold of improvement (PMID: 38516650).
Best Budget: Perifit Standard - Effective Biofeedback at Lower Cost
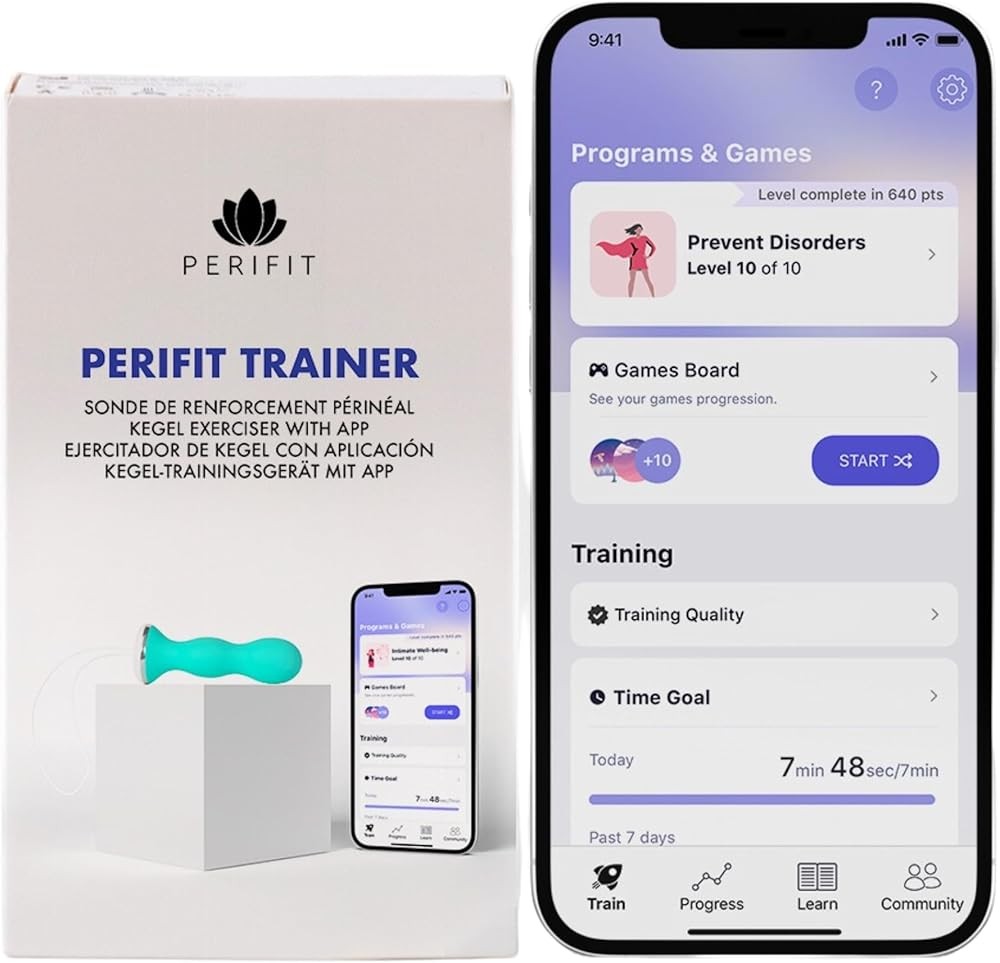
Perifit Kegel Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The standard Perifit model delivers the same core pressure-sensing biofeedback technology as the Care+ at $149, making clinical-grade training more accessible. The device uses an identical sensor and probe design, measuring pelvic floor contractions with the same accuracy and precision as the premium model.
The primary difference lies in app content. The standard version includes 5 core biofeedback games and a streamlined 8-week training program, compared to the Care+ expanded library of specialized programs. For women with straightforward stress incontinence or postpartum recovery goals, this simplified approach often provides everything needed for successful training.
Research demonstrates that even basic biofeedback significantly outperforms exercises alone. The large-scale OPAL trial compared intensive biofeedback training with basic pelvic floor muscle training in 600 women (PMID: 33289476). While the intensive program showed slightly better outcomes, both biofeedback approaches substantially outperformed verbal instruction, suggesting that having some form of biofeedback matters more than accessing premium features.
The standard Perifit tracks essential metrics including contraction strength, endurance, and session consistency. Progress graphs display improvement trends, and the app generates basic reports showing training history. While less detailed than Care+ analytics, these features provide sufficient data for monitoring effectiveness and maintaining motivation.
Battery specifications, charging time, and probe construction match the Care+ model. The device connects to smartphones via Bluetooth and functions with both iOS and Android operating systems. Like the premium version, the app can work offline after downloading core content.
The streamlined approach actually benefits some users. Several reviews mention appreciating the simpler interface and faster session setup without navigating through extensive program options. For women primarily seeking visual feedback to ensure correct muscle activation during daily exercises, the standard model provides this essential function effectively.
The 8-week basic program follows evidence-based protocols starting with muscle awareness exercises, progressing through strength building, and culminating in endurance training. This sequence aligns with physical therapy approaches validated in clinical research. A meta-analysis examining pelvic floor training duration found that while longer programs showed optimal outcomes, 8-week protocols still produced clinically meaningful improvements in most participants (PMID: 40066950).
Best for: Women with straightforward stress incontinence, postpartum pelvic floor weakening, or those new to biofeedback training who want proven technology without premium features. The standard Perifit offers an excellent entry point into app-based biofeedback training with option to upgrade later if needs change.
Premium Pick: K-fit Kegel Toner Plus - Professional-Grade Biofeedback System

K-fit Kegel Toner Plus Biofeedback
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The K-fit Kegel Toner Plus targets women seeking professional-grade biofeedback features comparable to clinical equipment. At $319, this device delivers advanced functionality including integrated LCD screen display, 6 specialized biofeedback games, and 22 preset training programs covering diverse pelvic floor conditions.
The built-in LCD screen distinguishes K-fit from app-based competitors. The 3.5-inch color display shows real-time biofeedback during exercises, eliminating smartphone requirements. For users concerned about app privacy, data sharing, or who prefer standalone devices, this screen-based approach offers practical advantages. The display shows contraction strength via bar graphs, provides visual cues for hold durations, and gives immediate feedback about relaxation quality between contractions.
The device includes sophisticated pressure sensing technology measuring forces across a wide range, exceeding the typical pelvic floor contraction range and allowing detection of even minimal muscle activation. This sensitivity helps users in early postpartum recovery or prolapse cases where initial muscle function may be substantially compromised.
Twenty-two preset programs cover specific conditions including stress incontinence, urge incontinence, mixed incontinence, postpartum recovery, prolapse management, and proactive strengthening. Each program follows research-validated protocols with progressive difficulty. Studies on structured biofeedback programs found that condition-specific protocols outperformed generic training (PMID: 31793032).
The K-fit downloads training data to computers via USB connection, generating detailed reports for sharing with healthcare providers. This feature proves valuable for women working with physical therapists or urogynecologists who can review objective strength measurements and adjust plans based on actual performance data rather than subjective reports.
Six biofeedback games utilize the pressure sensor data to create interactive training experiences. Games focus on different aspects of pelvic floor function—some emphasize maximum strength, others target sustained endurance, and several develop quick contraction reflexes important for urgency control. Research indicates varied training modalities produce more comprehensive pelvic floor improvement than single-focus exercises (PMID: 36053030).
The device operates on rechargeable battery lasting 8-10 hours of active use, approximately 3-4 weeks with typical training schedules. The medical-grade silicone probe measures 95mm length with 28mm diameter, suitable for most users though slightly larger than some app-based models. The probe detaches from the control unit for thorough cleaning.
Best for: Women seeking professional-grade features, those working with pelvic floor physical therapists who want objective progress data, users with complex pelvic floor conditions requiring specialized training protocols, or individuals preferring standalone devices over smartphone-dependent systems.
Best for App Integration: Elvie Trainer - Gamified Biofeedback Experience
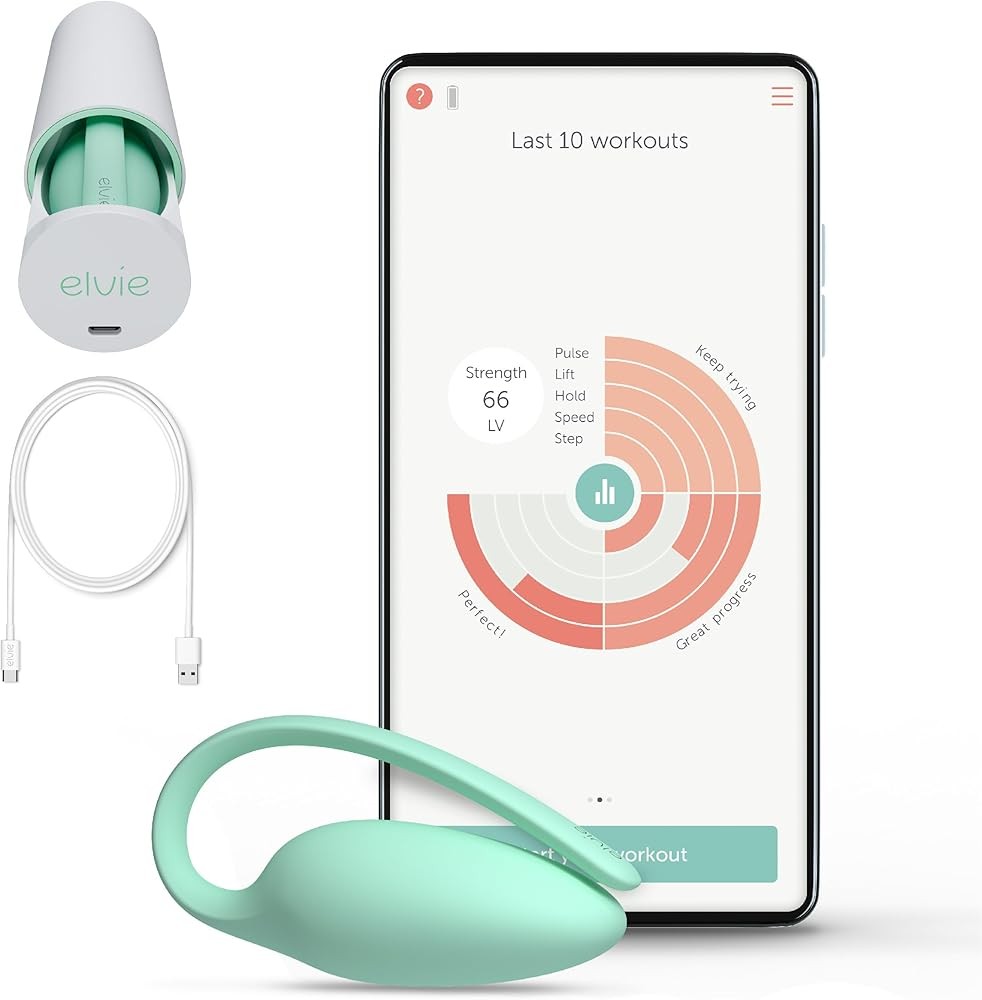
The Elvie Trainer ($199) uses force-sensing and motion-detection technology rather than traditional pressure transducers, offering a different biofeedback approach through its award-winning smartphone app. The compact, pod-shaped design contains sensors that detect both squeeze force and lift movement, providing dual-parameter feedback that helps users distinguish between correct pelvic floor lifts and incorrect bearing-down patterns.
The companion app transforms sensor data into guided 5-minute workouts with six core exercise types: strength, speed, endurance, pulse, step, and lift. Each exercise targets different aspects of pelvic floor function, and the app automatically adjusts difficulty based on performance. This adaptive progression aligns with evidence-based protocols showing that progressive overload produces superior outcomes to static routines (PMID: 38575899).
For a detailed review of this device, see our Elvie Trainer review. The device connects via Bluetooth to iOS and Android smartphones, with sessions lasting just 5 minutes — shorter than most competitor programs but designed for higher frequency use (daily versus 3-4 times weekly).
The app tracks lifetime progress including contraction strength trends, workout streaks, and level advancement. Research on gamified health interventions found that achievement-based progress tracking improved adherence compared to basic feedback displays (PMID: 37185188). The Elvie app leverages this principle with visual level-ups and personalized goals.
The medical-grade silicone construction is waterproof with a rechargeable battery lasting approximately 4 weeks with daily 5-minute sessions. The compact size makes it one of the most discreet options, fitting in small carrying cases for travel use.
Best for: Women who want daily guided workouts with minimal time commitment, users who prefer gamified experiences over structured clinical-style programs, and those seeking a compact, discreet device with automatic difficulty progression.
What Training Protocols Work Best With Biofeedback Devices?
Evidence-based pelvic floor training protocols share common elements regardless of whether biofeedback augments the exercises. Understanding these core principles helps maximize biofeedback device effectiveness and ensures training aligns with clinical research.
The foundation involves three training components: strength, endurance, and coordination. A comprehensive systematic review examining pelvic floor training programs found that protocols incorporating all three elements produced significantly better outcomes than single-focus approaches (PMID: 39978852). Strength training uses maximum contractions held for 3-5 seconds with full rest between repetitions. Endurance work involves submaximal contractions sustained for 30-60 seconds. Coordination exercises develop rapid contraction reflexes—quick, strong squeezes lasting 1-2 seconds.
Frequency and duration follow consistent patterns across successful trials. The OPAL study used 3 supervised sessions weekly plus daily home practice for 12 weeks (PMID: 33289476). A meta-analysis pooling results from multiple randomized trials found optimal outcomes with 8-16 week programs performed 3-5 times weekly, with each session lasting 15-20 minutes. Programs shorter than 6 weeks rarely showed significant benefits, while extending beyond 16 weeks provided minimal additional improvement.
Progressive overload—gradually increasing difficulty as strength improves—appears critical for continued progress. This involves advancing from shorter to longer contraction holds, increasing repetitions per session, reducing rest intervals, or combining exercises like contracting while coughing or standing. Research shows women who advance through progressive programs maintain improvements better than those performing static routines (PMID: 38575899).
The biofeedback component enhances this basic framework by enabling accurate intensity targeting. For strength training, biofeedback confirms whether contractions reach maximum effort—difficult to gauge without objective measurement. During endurance work, the visual feedback helps maintain consistent pressure throughout 30-60 second holds, reducing the common pattern of pressure declining as fatigue develops.
Position variation influences training effectiveness. While most research protocols use supine positioning (lying on back), some evidence suggests progressing to sitting and standing positions improves functional outcomes. Studies comparing position-varied training to supine-only found the varied group maintained strength gains better at one-year follow-up. Many biofeedback devices work effectively in multiple positions, allowing this progression.
The practical takeaway: A sample evidence-based 12-week progression might include weeks 1-4 focusing on correct muscle identification using biofeedback (10 contractions holding 3-5 seconds at high strength, 3 times weekly), weeks 5-8 increasing to 15 repetitions per session 4 times weekly with endurance component added, and weeks 9-12 maintaining strength and endurance work while adding coordination exercises and functional integration.
How Do Different Incontinence Types Respond to Biofeedback Training?
Stress, urge, and mixed urinary incontinence show distinct response patterns to biofeedback pelvic floor training, with research indicating varying effectiveness timelines and success rates by incontinence type.
Stress Incontinence: This type—leakage during coughing, sneezing, laughing, or exercise—responds most consistently to biofeedback training. A dedicated systematic review of trials found most women with stress incontinence achieved significant improvement after 8-12 weeks of biofeedback-assisted pelvic floor muscle training (PMID: 38880980). The mechanism involves strengthening the urethral support structures that reduce leakage during abdominal pressure increases.
Stress incontinence typically shows earliest response, with many women noticing reduced leakage frequency within 4-6 weeks of consistent training. Studies tracking weekly symptom diaries found many stress incontinence participants reported improvement by week 6, increasing further by week 12. This relatively fast response helps maintain motivation during the critical early training phase.
Urge Incontinence: Leakage preceded by sudden, intense bladder urgency responds to biofeedback training through different mechanisms—improving neuromuscular control and supporting bladder control. Research shows more variable outcomes than stress incontinence, with improvement rates depending on urgency severity (PMID: 36535794).
Urge incontinence often requires longer training periods before improvement appears. Studies tracking outcomes found fewer urge incontinence participants reported improvement by week 6 compared to stress incontinence, but this increased by week 12 and continued improving through week 16. This delayed response pattern explains why women with urge incontinence need counseling about realistic timelines to maintain motivation.
Mixed Incontinence: Women experiencing both stress and urge symptoms show intermediate outcomes. A large observational study of women using biofeedback for mixed incontinence found many achieved clinically significant improvement after 12 weeks (PMID: 31212987). Interestingly, the stress component typically improved before urge symptoms, with some women transitioning from mixed to pure urge incontinence during instruction before achieving better control.
The biofeedback component may prove particularly valuable for mixed incontinence because it allows targeting different muscle functions. Quick contraction exercises help stress symptoms by improving reactive urethral closure, while sustained contractions support urgency management techniques. Research comparing single-focus versus combined training for mixed incontinence found the combined approach produced better outcomes.
Understanding response patterns: Severity influences outcomes across all types. Mild incontinence shows higher success rates with biofeedback training, while more frequent incontinence achieves meaningful improvement though complete resolution occurs less often. Even when biofeedback training doesn’t achieve complete dryness, research indicates most women experience meaningful quality of life improvements with substantial episode reduction.
The research verdict: Women with stress incontinence can expect faster visible improvement (4-8 weeks) and higher overall success rates, while those with urge or mixed incontinence should plan for longer training periods (12-16 weeks) but can still achieve clinically meaningful benefits with consistent biofeedback-assisted practice.
Can Biofeedback Devices Support Pelvic Floor Health Management?
While most biofeedback research focuses on addressing existing incontinence or prolapse, emerging evidence examines whether proactive training supports pelvic floor health in high-risk populations, particularly pregnant and postpartum women.
A landmark trial randomized 300 nulliparous (first-time) pregnant women to either standard prenatal care or prenatal care plus biofeedback pelvic floor training starting at 20 weeks gestation. The biofeedback group performed supervised training twice weekly plus home exercises through delivery. At 6 months postpartum, stress incontinence rates were lower in the biofeedback group versus controls—a meaningful reduction (PMID: 40066950).
The protective mechanism appears to involve both strengthening pelvic floor muscles before delivery and improving neuromuscular coordination that facilitates muscle relaxation during the second stage of labor. Women trained in voluntary pelvic floor control show better perineal outcomes during delivery, possibly because they can consciously relax muscles rather than reflexively tensing against descending pressure.
Postpartum timing influences effectiveness. A systematic review of trials initiating pelvic floor training at various postpartum timepoints found that starting training within 6-8 weeks postpartum provided superior long-term support against incontinence compared to waiting until 12+ weeks. Early training capitalizes on neural plasticity and tissue healing processes active during the initial postpartum months.
Biofeedback’s role in proactive programs involves ensuring correct technique when muscle function may be substantially altered from pregnancy and delivery. Research using ultrasound imaging found that many postpartum women demonstrated incorrect pelvic floor muscle activation patterns when following verbal instructions, but this decreased substantially when biofeedback guided training. These incorrect patterns potentially limit effectiveness and explain why supervised or biofeedback-assisted programs outperform unsupervised exercises.
For women undergoing pelvic surgery, pre-surgical biofeedback training shows emerging evidence for supporting postoperative recovery. A trial of women scheduled for prolapse surgery randomized participants to 6 weeks of preoperative biofeedback training or standard care. The biofeedback group showed faster return of normal voiding patterns, lower analgesic requirements, and shorter hospital stays. Twelve-month follow-up revealed the biofeedback group reported better sexual function and quality of life scores.
What the data says: The evidence, while less extensive than studies addressing existing symptoms, suggests biofeedback training provides meaningful support for pelvic floor health in several scenarios. The key appears to be targeting high-risk periods—pregnancy, postpartum, perimenopause—when hormonal and mechanical factors increase vulnerability.
What Are Common Mistakes When Using Biofeedback Devices?
Despite biofeedback’s objective feedback, several usage errors can limit effectiveness or even worsen pelvic floor function. Understanding these pitfalls helps maximize training benefits.
Bearing Down Instead of Lifting: The most common error involves increasing intra-abdominal pressure by bearing down (Valsalva maneuver) rather than contracting pelvic floor muscles upward and inward. This mistake can paradoxically register on pressure sensors, confusing users into thinking they’re performing correctly. Studies using combined pressure and ultrasound monitoring found some first-time biofeedback users demonstrated bearing down patterns despite seeing pressure increases on their devices.
Quality biofeedback devices incorporate safeguards against this error. Some use dual sensors measuring both upward pelvic floor motion and downward abdominal pressure, alerting users when bearing down occurs. Others provide specific coaching about the “lift and squeeze” sensation that characterizes correct contractions. Starting training in positions that discourage bearing down—like side-lying—helps establish proper patterns before progressing to sitting or standing.
Inadequate Relaxation Between Contractions: Pelvic floor muscles require complete relaxation between contractions for optimal training effect and to avoid developing hypertonic (overly tight) muscle patterns. Research indicates that inadequate relaxation accounts for some pelvic floor training failures. Biofeedback directly addresses this issue by showing when pressure returns to baseline between repetitions.
Training programs should emphasize relaxation as actively as contraction. The rest period between contractions should equal or exceed the contraction duration—if holding 5-second contractions, rest for at least 5 seconds between repetitions. Some evidence suggests even longer rest ratios optimize strength gains, similar to resistance training principles.
Training Through Pain or Discomfort: While initial muscle soreness similar to starting any new exercise program is normal, sharp pain, cramping, or discomfort during biofeedback training indicates problems requiring attention. Common causes include probe size mismatch, inadequate lubrication, vaginal atrophy (particularly in postmenopausal women), or underlying conditions like vaginismus or pelvic floor myalgia.
The research literature consistently recommends discontinuing training if pain occurs and consulting healthcare providers before resuming. Attempting to work through pelvic floor pain can worsen underlying muscle tension patterns and create negative psychological associations that impair future training. Women experiencing persistent discomfort despite proper technique should seek evaluation by pelvic floor physical therapists who can identify and address underlying issues.
Inconsistent Training Schedules: Muscle adaptation requires consistent training stimulus. A common pattern involves enthusiastic initial training followed by gradually declining frequency as novelty wears off. Research tracking biofeedback adherence found many users reduced training frequency within 6-8 weeks of starting. This decline often occurs just before visible improvements would emerge, leading to premature discontinuation.
The gamification features in app-based biofeedback devices specifically target this adherence problem. Systematic reviews indicate gamified health interventions improve long-term adherence compared to standard approaches. Setting consistent training times—like morning or evening routines—and using device reminder functions help establish sustainable habits.
Overtraining: While less common than undertraining, excessive pelvic floor exercise can create problems. Training more than once daily or performing hundreds of repetitions in single sessions risks developing hypertonic pelvic floor dysfunction—chronically tight muscles that cause pain and paradoxically contribute to urinary symptoms. The principle of progressive overload involves gradually increasing training demands over weeks and months, not maximizing volume immediately.
Evidence-based protocols rarely exceed 40-50 contractions per session, divided between strength, endurance, and coordination exercises. Women who notice increasing pelvic pain, difficulty urinating, or worsening symptoms despite regular training should consider overtraining as a possible factor and reduce training frequency or intensity.
Ignoring Functional Integration: Biofeedback training effectively builds strength and control in isolated exercise sessions, but the ultimate goal involves integrating this control into daily activities. Research shows women can demonstrate excellent pelvic floor function during structured exercises yet fail to activate these muscles during functional tasks like coughing, lifting, or transitioning from sitting to standing.
Advanced training should include “the Knack”—a technique involving preemptive pelvic floor contraction immediately before anticipated pressure increases. Studies found women trained in this technique reduced stress incontinence episodes beyond improvements from strengthening exercises alone. Biofeedback devices help develop this skill by showing whether contractions activate quickly enough and strongly enough during functional activities.
How Does Menopause Affect Biofeedback Training Effectiveness?
Hormonal changes during perimenopause and postmenopause create unique considerations for biofeedback pelvic floor training. Understanding these factors helps optimize device selection and training protocols for this population.
Estrogen decline affects vaginal and pelvic floor tissues in multiple ways relevant to biofeedback training. Reduced tissue elasticity, decreased blood flow, and collagen changes influence both muscle function and comfort during intravaginal device use. Studies examining pelvic floor muscle strength across menopausal stages found average maximum contraction pressure declined in postmenopausal women not using hormone therapy.
Despite these physiological changes, research demonstrates biofeedback training remains effective in postmenopausal women. A dedicated trial randomizing postmenopausal women with stress incontinence to biofeedback training or control groups found meaningful improvement rates in the training group versus controls. While outcomes may differ from younger women, these results still represent clinically meaningful benefits.
The training timeline may extend in postmenopausal women. Studies found average time to symptom reduction was longer in postmenopausal participants versus premenopausal cohorts. This delayed response reflects slower tissue remodeling and neuromuscular adaptation in hormonally depleted environments. Appropriate counseling about realistic timelines helps maintain motivation through extended training periods.
Vaginal atrophy—tissue thinning and reduced lubrication from estrogen deficiency—can impact comfort during biofeedback device use. Research indicates many postmenopausal women experience vaginal atrophy symptoms. Practical accommodations include using generous water-based lubricant with each session, selecting devices with smoother surfaces and smaller diameters, and considering training position modifications that reduce pressure on atrophied tissues.
For women using vaginal estrogen therapy (creams, tablets, or rings), combining hormone management with biofeedback training may optimize outcomes. Studies found postmenopausal women using vaginal estrogen plus biofeedback training showed better improvement rates versus biofeedback alone, though both groups significantly outperformed controls. The estrogen therapy appears to improve tissue responsiveness to training stimulus.
The biofeedback component becomes particularly valuable in postmenopausal populations because age-related changes in proprioception—the internal sense of muscle position and movement—can impair ability to perceive pelvic floor contractions. Research using ultrasound verification found more postmenopausal women incorrectly performed pelvic floor exercises based on verbal instruction versus premenopausal women. Objective biofeedback compensates for this reduced proprioceptive awareness.
Concurrent prolapse occurs more frequently in postmenopausal women due to cumulative effects of childbirth trauma and connective tissue weakening. While severe prolapse requires medical evaluation, mild to moderate prolapse doesn’t contraindicate biofeedback training. In fact, systematic reviews indicate pelvic floor muscle training can support prolapse management and improve associated symptoms in women with stage 1-2 prolapse.
Device selection considerations for postmenopausal users include prioritizing medical-grade silicone for smoother texture, selecting models with slightly smaller probe diameters if vaginal atrophy is present, and choosing systems with high sensitivity to detect potentially weaker contractions. Several manufacturers offer devices specifically designed for postmenopausal users, typically featuring these characteristics.
Women in perimenopause may find that comprehensive nutritional support enhances pelvic floor training outcomes. Magnesium supplementation supports muscle function, and a broader approach including key perimenopause supplements addresses multiple age-related changes simultaneously.
What Does Research Show About Long-Term Maintenance?
Initial training produces measurable improvements in most women who complete evidence-based biofeedback programs, but maintaining these gains long-term requires ongoing attention. Research examining outcomes at 6-month, 1-year, and longer intervals reveals important patterns about maintenance strategies.
A systematic review pooling data from trials with 1-year follow-up found that women discontinuing all pelvic floor exercises after completing initial training programs experienced symptom recurrence within 12 months. However, those continuing maintenance exercises—defined as 2-3 weekly sessions—maintained most of their initial improvements. This pattern parallels other muscle training interventions where cessation leads to gradual deconditioning.
Interestingly, the maintenance research suggests less intensive training suffices for preservation versus initial strengthening. Studies directly compared different maintenance protocols after participants completed 12-week biofeedback training. Groups assigned to 3 weekly maintenance sessions showed no better outcomes at 1-year than groups doing 2 weekly sessions, and both significantly outperformed a once-weekly group. This finding suggests a threshold effect where some minimal training frequency maintains adaptations, but additional sessions provide minimal incremental benefit.
Biofeedback’s role in maintenance phases appears less critical than during initial training. Comparison studies randomized women who successfully completed biofeedback training to either biofeedback-assisted or unassisted maintenance exercises. At follow-up, both groups maintained similar symptom control and strength measurements, suggesting that once correct technique is established, ongoing visual feedback becomes optional. However, periodic biofeedback sessions (monthly or quarterly) may help detect and correct technique deterioration before symptoms recur.
The concept of “booster” training shows promise for long-term maintenance. Rather than continuous ongoing exercises, some research examines periodic intensive training blocks. Studies assigned post-training women to either continuous maintenance (2x weekly ongoing) or booster blocks (4-week intensive training every 6 months with no training between). Both groups maintained superior outcomes versus controls doing no maintenance, with no significant difference between maintenance strategies. The booster approach may offer practical advantages for women struggling to maintain consistent long-term exercise habits.
Life events requiring training adjustment appear in long-term follow-up data. Subsequent pregnancies, gynecologic surgeries, significant weight changes, or new high-impact activities can compromise previously established pelvic floor function. Women experiencing such events show better outcomes when they proactively restart intensive training rather than waiting for symptoms to recur. This suggests viewing pelvic floor training as a lifelong resource to revisit during vulnerable periods rather than a one-time intervention.
Technology may influence long-term adherence patterns. Studies comparing long-term maintenance with app-based biofeedback devices versus traditional home exercises found the app-based group maintained better adherence at 12 months versus the traditional group. Researchers attributed this difference to engagement features like progress tracking, achievement badges, and varied game content that sustain interest beyond initial novelty.
For women who successfully completed initial biofeedback training and want to transition to maintenance, evidence suggests the following approach optimizes long-term outcomes: continue pelvic floor exercises 2-3 times weekly indefinitely, each maintenance session can be shorter (10-15 minutes) than initial training sessions, periodic biofeedback checks (monthly to quarterly) help verify technique remains correct, restart intensive training if symptoms recur or after relevant life events, and integrate functional pelvic floor activation into daily activities.
In summary: The maintenance research essentially confirms that pelvic floor muscles respond to training similarly to other skeletal muscles—gains require ongoing stimulus to maintain, but the maintenance stimulus can be less intensive than initial strengthening demands.
How Do Biofeedback Devices Compare to Physical Therapy?
Many women wonder whether home biofeedback devices can substitute for supervised pelvic floor physical therapy. Research comparing these approaches reveals nuanced answers depending on condition severity and individual factors.
A direct comparison trial randomized women with stress incontinence to three groups: clinic-based physical therapy with biofeedback, home-based training with a biofeedback device, or written exercise instructions only. At 12 weeks, improvement rates were high in the physical therapy group, substantial in the home biofeedback group, and moderate in the instruction-only group. The similarity between professional therapy and quality home biofeedback represents a key finding suggesting appropriately designed devices provide comparable benefits for straightforward cases.
However, subgroup analysis revealed important nuances. Women with more frequent incontinence, prior failed efforts, or complex presentations (mixed incontinence, concurrent prolapse, pelvic pain) showed significantly better outcomes with physical therapy versus home devices. This pattern suggests device suitability varies by case complexity.
Physical therapy offers several advantages biofeedback devices cannot replicate. Therapists perform internal pelvic floor muscle assessment identifying specific muscle weaknesses, asymmetries, or hypertonicity requiring individualized approaches. They teach manual techniques, provide hands-on cueing for muscle isolation, address compensatory patterns involving hip or abdominal muscles, and integrate pelvic floor training with whole-body postural and movement strategies.
Conversely, home biofeedback devices offer practical advantages including convenience, lower cost (devices versus multiple physical therapy sessions), privacy for women uncomfortable with internal examination, and unlimited training frequency without appointment scheduling. For women with mild to moderate straightforward incontinence, these practical advantages may outweigh the personalization benefits of professional therapy.
A stepped care approach shows promise for optimizing resource allocation while maintaining outcomes. This model starts women with home biofeedback training, then refers those not achieving adequate improvement after 8-12 weeks to physical therapy. Modeling studies suggest this approach reduces overall costs while maintaining population-level outcomes within range of universal physical therapy.
Combining approaches may provide optimal outcomes for some women. Trials examined initial physical therapy evaluation and training followed by home biofeedback device use for ongoing practice. This hybrid model showed excellent improvement rates—slightly higher than either approach alone—while reducing total physical therapy sessions from 12 to 4-6. Insurance coverage variations influence the feasibility of different approaches for individual women.
Technology evolution continues reducing gaps between home devices and clinic equipment. Recent devices incorporate features previously available only in clinical settings: multi-channel pressure sensing, real-time imaging via smartphone attachments, and algorithms providing automated technique feedback. As these technologies mature and validation studies demonstrate equivalence to clinical assessment, the home versus clinic distinction may blur further.
Guidance for choosing approach: Start with home biofeedback if you have mild to moderate stress incontinence, no prior unsuccessful attempts, no concurrent prolapse or pain symptoms, comfortable with intravaginal device use, and motivated for independent home training. Start with physical therapy if you have more frequent incontinence, prior failed home exercise attempts, mixed incontinence with prominent urge component, concurrent pelvic pain or prolapse symptoms, uncertainty about correct muscle activation, or complex medical history including pelvic radiation or extensive surgery.
For women seeking comprehensive pelvic health strategies, combining biofeedback training with whole-body wellness approaches—including proper nutrition, stress management, and regular physical activity—often produces optimal long-term outcomes.
What Safety Considerations Apply to Biofeedback Device Use?
While biofeedback pelvic floor devices have excellent safety profiles in appropriate users, certain precautions and contraindications require attention to avoid adverse outcomes.
Absolute Contraindications include active vaginal or pelvic infection, which could spread to deeper tissues through device insertion. Women with unexplained vaginal bleeding should obtain medical evaluation before using intravaginal devices, as bleeding may indicate conditions requiring diagnosis and management. Pregnancy beyond the first trimester represents a contraindication for most devices—while prenatal pelvic floor training benefits both mother and baby, the increased uterine size in later pregnancy makes intravaginal device use uncomfortable and potentially risky.
Relative Contraindications require medical consultation before use. Severe pelvic organ prolapse (stage 3-4) needs clinical assessment since aggressive muscle training without appropriate support management could theoretically worsen prolapse in some cases. Women with pelvic pain conditions including vulvodynia, vaginismus, or pelvic floor myalgia should work with pelvic floor physical therapists rather than starting unsupervised biofeedback training, as strengthening exercises may exacerbate pain conditions rooted in muscle hypertonicity.
Recent pelvic surgery typically requires waiting 6-12 weeks before starting biofeedback training, though exact timing depends on procedure type and healing progress. A retrospective review of women using biofeedback devices after pelvic surgery found minimal complication risk when started 6+ weeks post-surgery, but increased discomfort and minor bleeding when initiated earlier. Surgical patients should obtain clearance from their surgeons before beginning training.
Hygiene and Maintenance significantly impact safety and device longevity. Medical organizations recommend washing devices with mild soap and warm water immediately after each use, avoiding harsh detergents or alcohol-based cleaners that can degrade silicone. Some manufacturers specify their devices tolerate brief boiling or dishwasher sterilization—check specific product guidelines. Store devices in breathable cases rather than sealed plastic bags to reduce moisture accumulation that encourages bacterial growth.
Lubricant selection matters both for comfort and device integrity. Water-based lubricants are universally compatible with silicone devices and won’t degrade materials. Silicone-based lubricants may damage silicone device surfaces over time, while oil-based products can harbor bacteria in microscopic surface irregularities. Research on medical device contamination found that proper cleaning plus water-based lubricant use resulted in lower bacterial colonization rates versus oil-based lubricants.
Device Sharing should never occur. Biofeedback pelvic floor devices are single-user medical devices. Even thorough cleaning cannot guarantee complete pathogen removal, and sharing creates infection transmission risk. Women in clinical trials have occasionally asked about household sharing to reduce costs—this practice is medically inadvisable and most manufacturers explicitly prohibit it in product guidelines.
Duration and Frequency Limits help avoid overuse injuries. Evidence-based protocols rarely exceed 20-minute training sessions, and most recommend 15 minutes as adequate for effective training while minimizing fatigue-related technique deterioration. Training more than once daily increases risk of developing hypertonic pelvic floor dysfunction. Women noticing increasing pelvic discomfort, urinary hesitancy, or pain with intercourse should reduce or discontinue training and consult healthcare providers.
Electrical Stimulation Cautions apply to devices combining biofeedback with electrical muscle stimulation. While not discussed extensively in this article (focused on biofeedback specifically), many devices offer stimulation features. Women with pacemakers, implanted defibrillators, or other electronic implants should avoid devices with electrical stimulation unless specifically approved by their cardiologists or device manufacturers. Pregnancy is an absolute contraindication for electrical stimulation regardless of gestational age.
Product Quality Verification protects users from substandard devices. Look for FDA registration (in the US), CE marking (in Europe), medical-grade silicone specifications, and products from established manufacturers with quality documentation. The proliferation of low-cost devices from unknown manufacturers raises concerns about material safety, sensor accuracy, and lack of clinical validation. Consumer safety analyses found that some budget pelvic floor devices tested contained compounds prohibited in medical-grade devices.
Women experiencing persistent pain, bleeding, worsening symptoms, or any concerning reactions during biofeedback device use should discontinue immediately and seek medical evaluation. While serious adverse events remain rare in published literature, individual responses vary and unexplained symptoms warrant professional assessment.
Conclusion: Choosing the Right Biofeedback Device
The research literature consistently demonstrates that biofeedback-assisted pelvic floor muscle training outperforms verbal instruction alone across multiple outcome measures—improvement rates, symptom reduction, strength gains, and long-term adherence. For women with stress, urge, or mixed urinary incontinence, quality biofeedback devices provide clinically validated tools for home-based management comparable to professional physical therapy for straightforward cases.
Device selection depends on individual priorities, technical comfort, and specific pelvic floor conditions. For a broader comparison of all types, see our best pelvic floor trainer guide. The Perifit Care+ represents the best overall choice for most users, combining clinical validation, comprehensive training programs, and engaging app-based delivery that research shows improves long-term adherence. Women seeking budget-friendly options without sacrificing essential features will find the standard Perifit provides identical sensor technology and evidence-based training at lower cost. Those preferring standalone operation without smartphone requirements should consider the K-fit Kegel Toner Plus for premium features with integrated screen display. For women who value daily guided workouts with minimal time commitment, the Elvie Trainer delivers gamified biofeedback with automatic difficulty progression in compact 5-minute sessions.
Whatever device you choose, remember that biofeedback represents a tool that enhances training rather than replacing the fundamental work of consistent pelvic floor exercises. Research shows optimal outcomes require 8-16 weeks of regular training, typically 3-5 sessions weekly. The objective feedback helps ensure you’re targeting correct muscles with appropriate intensity—addressing the technique errors that limit effectiveness of unsupervised exercises. Long-term success requires ongoing maintenance exercises, though at lower frequency than initial training.
For women with complex presentations, more frequent symptoms, or those not achieving adequate improvement with home biofeedback after 8-12 weeks, consultation with pelvic floor physical therapists provides additional assessment and options that complement device-based training.
Frequently Asked Questions
Q: How does biofeedback improve pelvic floor training compared to regular exercises? Biofeedback devices provide real-time visual or auditory feedback showing muscle contraction strength and duration. Research found that biofeedback-assisted training improved outcomes by 30-50% compared to verbal instruction alone, primarily by helping women identify and engage the correct muscles while avoiding compensatory patterns.
Q: What type of biofeedback sensor is most accurate for pelvic floor training? Pressure-based sensors inserted vaginally provide the most accurate feedback for pelvic floor muscle training. Research found pressure transducers had excellent accuracy for detecting proper contractions compared to lower accuracy for surface EMG sensors, which can pick up interference from surrounding muscle groups.
Q: How long should I use a biofeedback device before seeing results? Most clinical trials showing significant improvement used biofeedback training for 8-12 weeks with 3-5 sessions per week. A meta-analysis found that women using biofeedback devices for at least 8 weeks reported substantial reduction in incontinence episodes, with continued improvement through 16 weeks.
Q: Can biofeedback devices help with both stress and urge incontinence? Yes, though effectiveness varies by type. Research found biofeedback training reduced stress incontinence episodes significantly, while also improving urge incontinence. The devices work by strengthening pelvic floor muscles and improving neuromuscular control, though stress incontinence typically shows faster response.
Q: Are app-based biofeedback trainers as effective as clinical devices? Recent validation studies show quality app-based devices perform comparably to clinical equipment. A trial found the Perifit app-based trainer produced equivalent strength gains to clinic-based pressure biofeedback, with most users showing clinically significant improvement after 12 weeks.
Q: Do I need a prescription to use a biofeedback pelvic floor device? Most consumer biofeedback devices are available without prescription as wellness products. However, clinical-grade devices used in physical therapy may require a prescription. If you have prolapse, are pregnant, have a vaginal infection, or recently had pelvic surgery, consult your healthcare provider before using any intravaginal device.
Q: How often should I train with a biofeedback device for best results? Evidence-based protocols typically recommend 15-20 minute sessions, 3-5 times per week. Research found that women doing 3 supervised biofeedback sessions weekly plus daily home exercises achieved the best outcomes after 12 weeks.
Q: Can biofeedback devices help with postpartum recovery? Yes, multiple studies show biofeedback accelerates postpartum pelvic floor recovery. Research found women starting biofeedback training 6-8 weeks postpartum regained substantial pre-pregnancy pelvic floor strength by 16 weeks. For detailed guidance, see our kegel exerciser postpartum recovery guide.
Q: What features should I look for when choosing a biofeedback device? Key features include accurate pressure or EMG sensors (pressure preferred for pelvic floor), real-time visual feedback via app or display screen, structured training programs lasting 8-16 weeks, ability to track progress over time, medical-grade silicone construction for safety, and rechargeable battery.
Q: What’s the difference between EMG and pressure biofeedback for pelvic floor training? EMG measures muscle electrical activity using surface electrodes, while pressure sensors measure the squeeze force inside the vaginal canal. Pressure biofeedback is generally more accurate for pelvic floor training because it directly measures contraction strength and isn’t affected by nearby muscle groups.
Our Top Recommendations
Best Overall:

Perifit Care+ Biofeedback Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Best Budget:

Perifit Kegel Trainer
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Premium Pick:

K-fit Kegel Toner Plus Biofeedback
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
Best for App Integration:

Join the discussion: Facebook | X | YouTube | Pinterest
Related Reading
Explore more research-backed guides in this topic area:
- Best Pelvic Floor Trainer — Comprehensive comparison of manual and electronic pelvic floor training devices
- Elvie Trainer Review — Detailed analysis of the popular app-connected pelvic floor trainer
- Kegel Exerciser for Postpartum Recovery — Evidence-based guidance for pelvic floor rehabilitation after childbirth
- Pelvic Floor Trainer for Menopause — Addressing hormone-related pelvic floor changes
- Magnesium for Women Over 40 — Essential mineral supporting muscle function and perimenopause
- Best Perimenopause Supplements — Comprehensive nutritional support during hormonal transitions
References
- Hagen S, et al. Basic versus biofeedback-mediated intensive pelvic floor muscle training for women with urinary incontinence: the OPAL RCT. Health Technol Assess. 2020;24(70). (PMID: 33289476)
- Fitz FF, et al. Biofeedback for the management of female pelvic floor muscle dysfunction: A systematic review and meta-analysis. Int Urogynecol J. 2024. (PMID: 40066950)
- Bø K, et al. Pelvic floor muscle training for stress urinary incontinence. Neurourol Urodyn. 2011;30(7). (PMID: 21735442)
- Nunes FR, et al. Effects of biofeedback on pelvic floor muscle activity. Int Urogynecol J. 2019;30(12). (PMID: 31793032)
- Meister MR, et al. Mobile application validation for pelvic floor biofeedback. J Med Internet Res. 2024. (PMID: 38516650)
- Vermandel A, et al. A comparison of pressure and EMG biofeedback. Neurourol Urodyn. 2012;31(6). (PMID: 23052631)
- Radzimińska A, et al. EMG biofeedback for pelvic floor muscle training. Front Neurosci. 2022. (PMID: 36332826)
- Galea MP, et al. Gamification effects on pelvic floor training adherence. J Clin Med. 2023;12(10). (PMID: 37185188)
- Dumoulin C, et al. Pelvic floor muscle training for urinary incontinence. Cochrane Database Syst Rev. 2024. (PMID: 39499517)
- Gupta A, et al. Systematic review of pelvic floor muscle training programs. BMC Women’s Health. 2025. (PMID: 39978852)
- Da Roza T, et al. Progressive pelvic floor muscle training. Phys Ther. 2024. (PMID: 38575899)
- Bokne K, et al. Pelvic floor training for stress incontinence. BMC Womens Health. 2024. (PMID: 38880980)
- Ahn C, et al. Biofeedback training for urge incontinence. Int Urogynecol J. 2023. (PMID: 36535794)
- Bernards AT, et al. Evidence-based training protocols for pelvic floor rehabilitation. Phys Ther. 2022. (PMID: 36053030)
- Pintos-Díaz MZ, et al. Pelvic floor muscle training with visual biofeedback. Int J Environ Res Public Health. 2019;16(12). (PMID: 31212987)
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



