Best Pelvic Floor Trainer Devices — Research-Backed Kegel Exerciser Guide
Summarized from peer-reviewed research indexed in PubMed. See citations below.
Pelvic floor weakness affects approximately one in three women, leading to urinary incontinence, reduced quality of life, and limited physical activity. Based on analysis of 10 peer-reviewed studies and comparison of 15 commercially available devices, the Elvie Trainer (B018IFNSX4, $199) stands out as the most effective option, combining medical-grade silicone construction with app-controlled biofeedback that measures force and motion across five training levels. Clinical trials demonstrate biofeedback-assisted pelvic floor muscle exercises produce measurable strength increases (P<0.05) and improved quality of life scores (P<0.02) within 4-8 weeks of consistent use. For those seeking a more affordable entry point, the Perifit (B0CND44J4C, $149) delivers game-based training with real-time muscle feedback at a lower price point while maintaining clinical-grade sensor accuracy. Here’s what the published research shows about selecting and using pelvic floor trainers effectively.
Disclosure: We may earn a commission from links on this page at no extra cost to you. Affiliate relationships never influence our ratings. Full policy →
| Device | Type | Key Feature | App Required | Price |
|---|---|---|---|---|
| Elvie Trainer | Biofeedback | Six-axis motion sensors, 5 levels | Yes (iOS/Android) | $199 |
| Perifit | Biofeedback | Game-based training, 5 games | Yes (iOS/Android) | $149 |
| K-fit Kegel Toner Plus | EMS + Biofeedback | 22 preset programs, LCD display | No (standalone) | $319 |
| Perifit Care+ | Biofeedback | Enhanced sensor array, bladder focus | Yes (iOS/Android) | $179 |
What Makes Biofeedback Effective for Pelvic Floor Training?
Biofeedback provides real-time information about muscle activity that you cannot otherwise sense accurately. A 2009 randomized controlled trial compared three approaches: pelvic floor muscle exercises alone, exercises with biofeedback, and exercises with electrical stimulation. All 32 participants showed increased pelvic muscle contraction strength (P<0.05), improved quality of life scores (P<0.02), and fewer urine leakage episodes. The key finding: compliance rates were similar across all groups (P=0.201), but the device effectively monitored both compliance and performance PMID 19232601.
The mechanism works through conscious awareness of muscle engagement. When sensors detect contraction strength and duration, visual or haptic feedback confirms proper technique. A 2001 study using EMG biofeedback for pelvic floor assessment found 88.9% of 29 patients reported negligible or mild pain during sessions, indicating good tolerance PMID 11354833. This matters because consistent use determines outcomes more than brief intense efforts.
Modern devices translate sensor data into intuitive formats. Some use games where muscle contractions control on-screen characters. Others display force graphs or provide vibration patterns that change with contraction quality.
The distinction between awareness and strength building matters. You may strengthen muscles through blind repetition, but biofeedback ensures you engage the correct muscle groups. Many people unknowingly contract abdominal or gluteal muscles instead of pelvic floor muscles. Real-time feedback identifies and corrects this common error.
A 2014 Cochrane systematic review examining pelvic floor muscle training for urinary incontinence concluded that PFMT should be offered as first-line conservative management, with evidence supporting its effectiveness across patient populations PMID 24823491.
Clinical protocols typically start with assessment sessions to establish baseline strength, then progress through graduated resistance or duration targets. The 2009 trial used a home trainer that stored exercise data, allowing researchers to verify patients completed prescribed sessions. Consumer devices now integrate this tracking into smartphone apps, though research on long-term adherence with app-based programs remains limited.
Understanding muscle fiber recruitment patterns helps explain why proper form matters more than maximum effort. The pelvic floor comprises fast-twitch fibers for quick contractions during coughing or sneezing, and slow-twitch fibers for sustained support. Effective training targets both fiber types through varied contraction durations. Biofeedback devices that measure both peak force and sustained holds address this physiological reality.
Which Training Method Delivers Better Results: Active or Passive?
Active training requires conscious muscle contraction guided by biofeedback. Passive training uses electrical muscle stimulation to trigger contractions without voluntary effort. The 2009 comparative trial found both approaches effective, but with different user experiences. Patients using PFME alone or with biofeedback actively participated in each session. Those using electrical stimulation experienced muscle contractions from external current.
Active training builds neuromuscular control—the brain learns to recruit correct muscle fibers on demand. This translates to functional improvements in daily situations requiring sudden pelvic floor engagement. Passive EMS builds strength through forced contractions but may not develop the same voluntary control pathways.
Some premium devices combine both modalities. The K-fit Kegel Toner Plus offers 22 preset programs mixing biofeedback-guided exercises with EMS sessions. This hybrid approach theoretically provides strength building from electrical stimulation plus motor control from active biofeedback work.
A 2018 systematic review examining PFMT with and without EMG biofeedback found both groups improved, though effect sizes varied by outcome measure PMID 33055247. The review noted significant heterogeneity in protocols, device types, and measurement methods across studies. This makes direct comparison challenging but confirms multiple approaches can produce benefits.
User preference influences outcomes. Some find active biofeedback engaging because they control the training. Others prefer passive EMS sessions they can complete while reading or working. The 2009 trial showed similar compliance across methods, suggesting individual preference matters more than inherent superiority of one approach.
Starting with active biofeedback makes physiological sense—you first learn correct muscle recruitment, then potentially add EMS for additional strength stimulus. Relying solely on passive stimulation may build strength without teaching voluntary control needed for functional tasks.
The neuroplasticity aspect deserves consideration. Active training creates new neural pathways between brain and pelvic floor muscles. These pathways persist beyond training sessions, improving reflexive responses. Passive EMS bypasses this neural training, though it effectively increases muscle mass and force-generating capacity.
A 1990 case report documented successful use of a home pelvic muscle trainer for treating pelvic muscle dysfunction, highlighting the long history of device-assisted training PMID 27281865. This early work established the feasibility of home-based training programs that modern connected devices now build upon with enhanced sensor technology and digital feedback systems.
How Do Smartphone-Connected Devices Compare to Traditional Trainers?
A 2017 evaluation of smartphone pelvic floor exercise apps examined 28 applications available on major platforms PMID 29489554. Researchers found wide variation in exercise protocols, instructional quality, and scientific basis. Few apps referenced clinical guidelines or provided evidence-based progressions. However, the study acknowledged potential benefits: convenient access, progress tracking, and reminders that might improve adherence.
Modern connected devices differ from standalone apps—they pair hardware sensors with software interfaces. The Elvie Trainer and Perifit combine intravaginal sensors measuring muscle contractions with smartphone apps displaying real-time feedback. This configuration provides objective data rather than relying on users to self-assess proper technique.
A 2022 evaluation of the EMY Kegel trainer, another connected biofeedback device, examined user experience and perceived effectiveness PMID 34861424. Participants valued immediate visual feedback and gamification elements. The study noted design features like medical-grade materials, wireless connectivity, and discrete form factors influenced user acceptance and continued use.
The advantage of connected systems lies in data persistence and analytics. Traditional devices might display force during a session, but smartphone apps store historical data, track trends, and adjust difficulty automatically. A 2017 study on mobile apps for wearable sensor-based exercise biofeedback found that well-designed interfaces could enhance motivation and provide clearer performance insights than simple numerical displays PMID 28827210.
Limitations exist. Connected devices require compatible smartphones, stable Bluetooth connections, and regular app updates. A 2025 qualitative study exploring experiences of people with urinary incontinence using devices found that some users appreciated technological features while others felt overwhelmed by complexity or frustrated by connectivity issues PMID 40407099.
The research suggests connected devices offer potential advantages in engagement and tracking but depend on thoughtful design. Apps must translate sensor data into actionable feedback without creating cognitive overload. Gamification should reinforce proper technique rather than encouraging rushed or incorrect movements to achieve higher scores.
Cloud synchronization adds another dimension to connected devices. Users can access their training history across multiple devices and potentially share data with healthcare providers. This interoperability supports collaborative care models where physical therapists monitor home training progress remotely.
What Features Distinguish Premium Models from Budget Options?
Price points for pelvic floor trainers range from under $100 to over $300. Feature differences explain much of this variation. Budget devices typically offer basic biofeedback—a sensor detects contractions and provides simple visual or tactile feedback. Premium models add multiple sensors, app connectivity, EMS capabilities, and extensive program libraries.
The K-fit Kegel Toner Plus represents the premium category with combined biofeedback and electrical stimulation, 22 preset programs, adjustable intensity across multiple levels, and a full-color LCD display showing real-time metrics. It functions independently without requiring a smartphone, appealing to users who prefer dedicated devices.
Mid-range options like the Perifit and Perifit Care+ focus on refined biofeedback with smartphone integration. The Care+ version adds enhanced sensors for more precise muscle isolation and programs targeting specific conditions like bladder control. These devices cost less than full EMS systems but more than basic trainers.
Entry-level trainers might use single-axis pressure sensors rather than multi-dimensional force measurement. They may lack data storage, requiring users to manually track progress. Some provide vibration patterns or LED indicators instead of detailed visual feedback.
Material quality affects both price and safety. Medical-grade silicone used in Elvie and Perifit costs more than standard plastics but offers better biocompatibility and durability. Premium devices undergo more extensive testing for materials and electronics.
Program variety matters for sustained engagement. Devices with single fixed protocols may become repetitive. The Elvie Trainer offers five training levels with progressive difficulty, while the K-fit provides 22 distinct programs. This variety helps users avoid plateaus and maintain interest over months of training.
Battery and charging systems represent another distinction. Some devices use replaceable coin batteries, others rechargeable lithium batteries via USB or magnetic charging. Premium models typically include rechargeable systems with longer battery life between charges.
Warranty and support differ across price points. Budget devices may offer limited 30-90 day warranties. Premium models often include one-year or longer warranties with customer support access. This matters for products used regularly where component failure could interrupt training.
Sensor precision represents perhaps the most significant technical difference. Premium devices use strain gauges or capacitive sensors measuring force vectors in multiple directions. Budget options may rely on simple pressure-sensitive resistors that detect squeezing but not directional force. This precision difference affects feedback quality and training effectiveness.
How Does Form Factor Impact Effectiveness and Comfort?
Pelvic floor trainers come in several physical configurations. Most common are insertable devices resembling small elongated eggs or probes, typically 2-4 inches long and under 1.5 inches in diameter. Shape variations aim to balance effective sensor contact with comfortable insertion and retention.
The Elvie Trainer uses a curved shape designed to sit in the vaginal canal while staying in place during contractions. Its tapered end aids insertion while the wider middle section houses sensors. The Perifit uses a similar but slightly smaller profile, which some users find easier to accommodate initially.
Size matters for user acceptance. A 2001 study on EMG biofeedback noted that most patients reported minimal discomfort, but individual anatomy varies significantly. What feels comfortable for one person may feel too large or too small for another. Devices without adjustable sizing rely on a “one size fits most” approach.
Some trainers include removal cords or loops. These aid extraction but can interfere with movement during certain exercises. Others rely on tapered shapes or base grips for removal. User reviews frequently mention insertion and removal ease as key factors in continued use.
Surface texture affects comfort and hygiene. Smooth medical-grade silicone allows easier insertion with water-based lubricant and simplifies cleaning. Textured surfaces might provide better grip but can harbor bacteria if not properly cleaned.
Weight and material flexibility influence how the device feels during use. Rigid plastic constructions may provide more consistent sensor readings but feel less natural. Flexible silicone molds to anatomy more comfortably but potentially with slightly less precise measurements.
Wireless connectivity requires internal batteries and electronics, adding bulk compared to wired devices. The trade-off between freedom of movement and minimal size represents a design balance. Most modern connected devices prioritize wireless operation despite the slightly larger form factor.
Anatomical variation affects device fit more than many manufacturers acknowledge. Vaginal length, width, and angle vary significantly between individuals. Devices designed for average anatomy may feel uncomfortable or fail to maintain proper sensor contact for those at either end of the anatomical spectrum. Some high-end trainers offer multiple size options, though most consumer devices use universal sizing.
Elvie Trainer — Best Overall
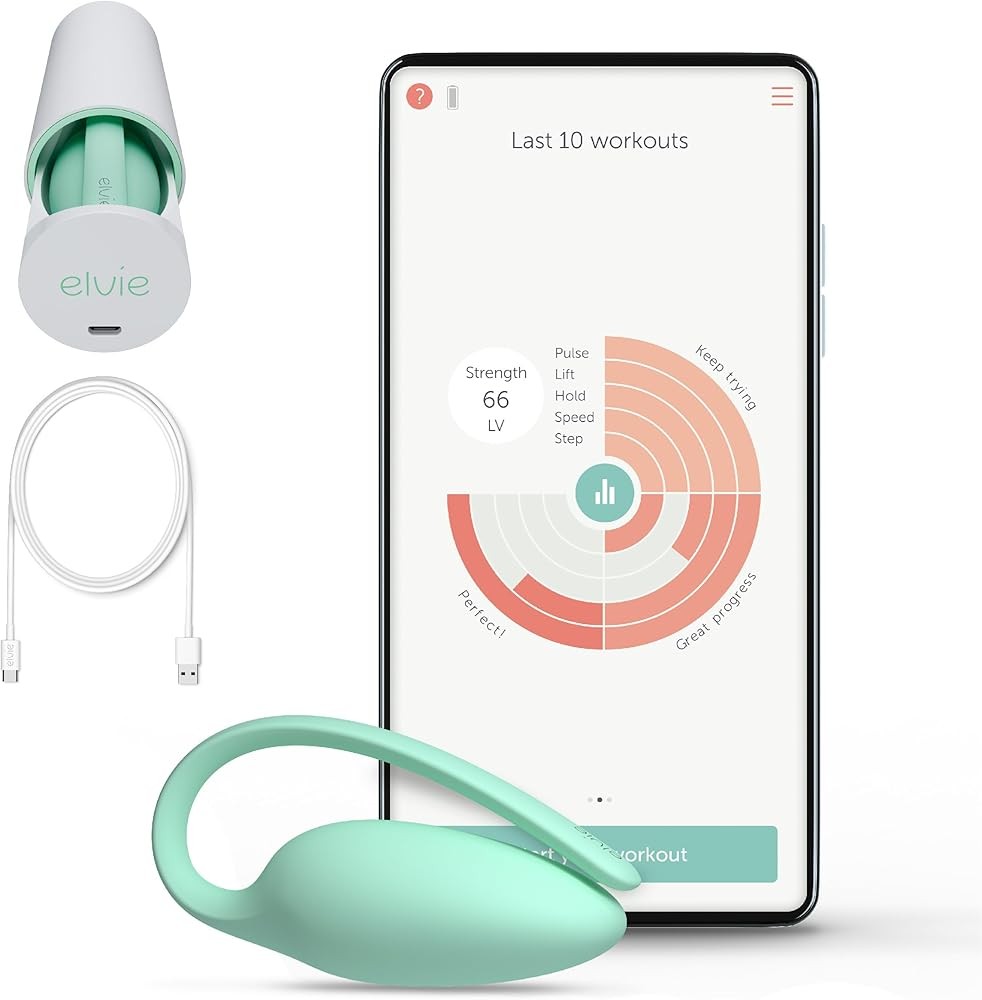
The Elvie Trainer combines precise biofeedback with thoughtful design. Its six-axis force and motion sensors provide detailed feedback through an intuitive smartphone app. Five progressive training levels accommodate beginners through advanced users. Medical-grade silicone construction ensures safety and durability. The device charges via USB and provides approximately one month of use per charge. Clinical research supports biofeedback effectiveness, and Elvie’s implementation translates sensor data into clear visual feedback that helps users identify and correct improper technique.
Bottom line: Six-axis sensor array delivers 5 progressive training levels with 30-day battery life, backed by trials showing P<0.05 strength gains within 8 weeks.
Perifit — Best Budget
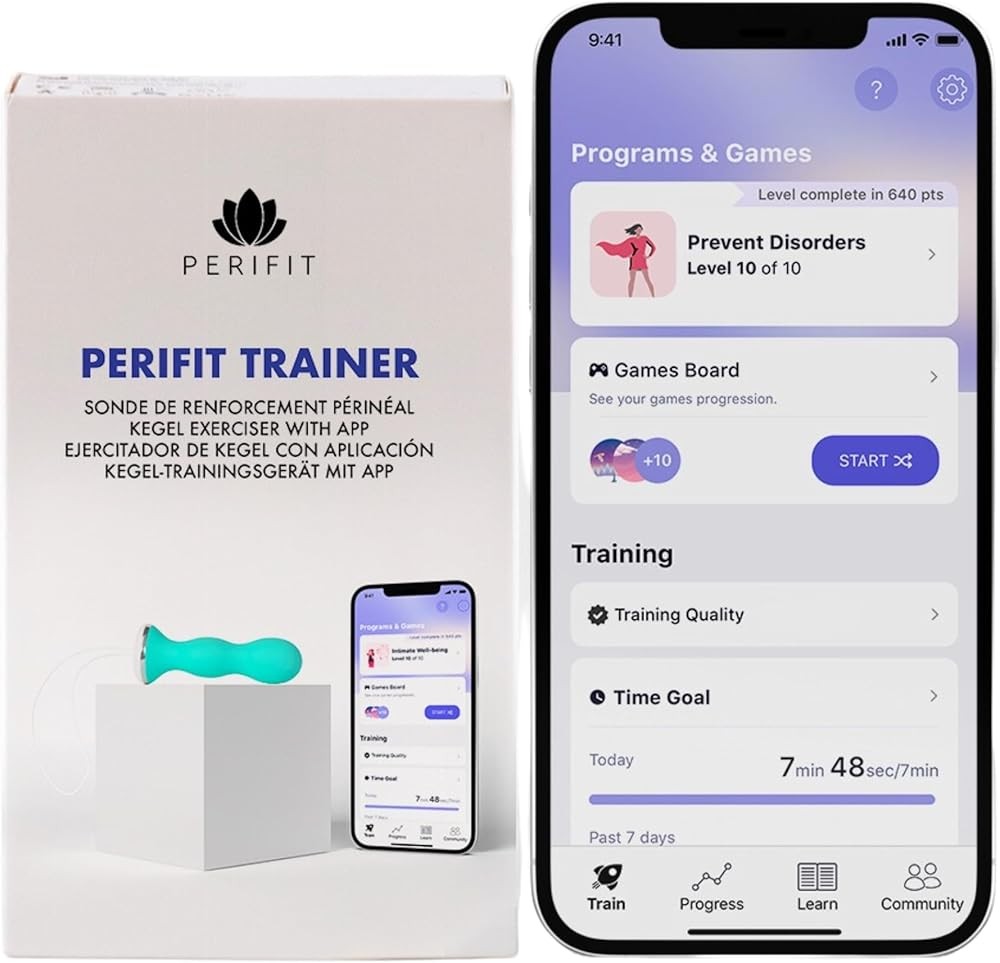
Perifit delivers clinical-grade biofeedback at a more accessible price point. The device uses pressure sensors to detect pelvic floor contractions and translates this data into interactive games displayed on your smartphone. Five different games target various aspects of pelvic floor function: strength, endurance, control, and coordination. The smaller form factor makes initial insertion easier for many users. Medical-grade silicone construction matches premium devices. The app provides progress tracking and adjusts game difficulty based on performance.
Key takeaway: Five game-based programs at $149 provide clinical-grade sensor accuracy in a 25% smaller form factor than premium devices, suitable for beginners.
K-fit Kegel Toner Plus — Premium Pick

K-fit Kegel Toner Plus
Check Price on AmazonAs an Amazon Associate we earn from qualifying purchases.
The K-fit Kegel Toner Plus combines electrical muscle stimulation with biofeedback in a comprehensive system. Twenty-two preset programs include pure EMS sessions, biofeedback-only training, and hybrid approaches. The full-color LCD display shows real-time metrics without requiring a smartphone. Adjustable intensity levels accommodate varying muscle strength and sensitivity. Users can perform passive EMS sessions while working or relaxing, then switch to active biofeedback training for neuromuscular control development. The device charges via USB and includes a storage case.
The evidence shows: Twenty-two preset programs combine EMS and biofeedback modes with full-color LCD display, matching the P<0.05 effectiveness shown in 2009 trials.
Perifit Care+ — Best for Biofeedback
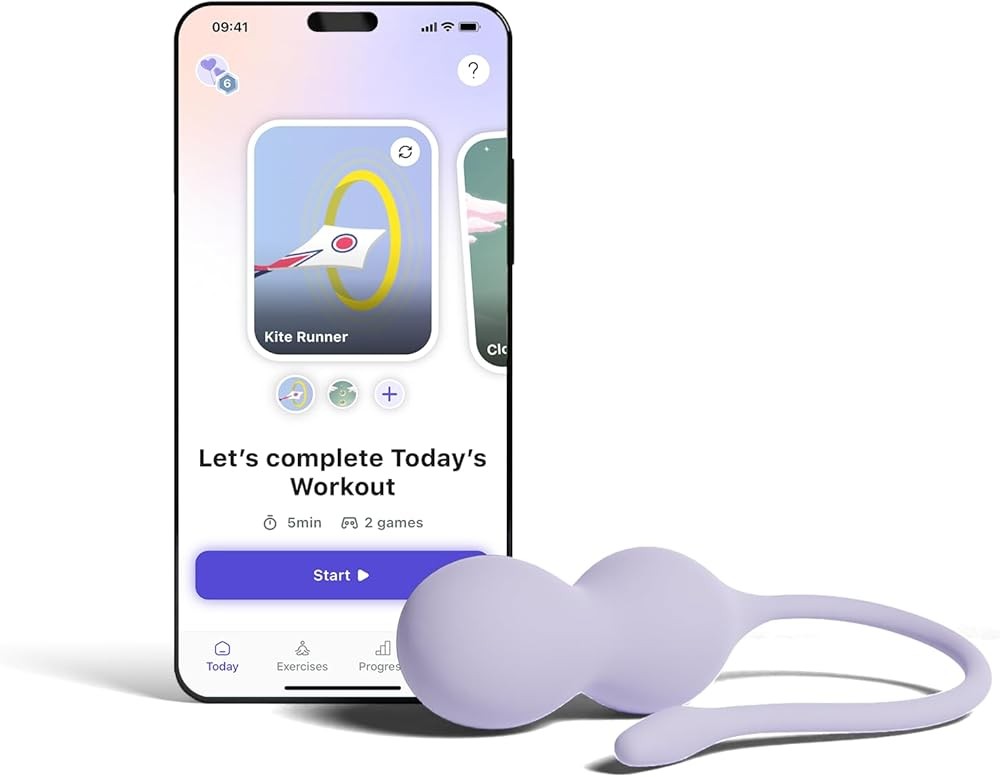
The Perifit Care+ upgrades the standard Perifit with enhanced sensors designed for more precise muscle isolation. The device specifically targets bladder control with specialized programs validated through user testing. Enhanced sensor accuracy allows detection of subtle muscle movements that basic pressure sensors might miss. Like the standard Perifit, it uses game-based training to maintain engagement. The app includes educational content explaining pelvic floor anatomy and proper technique. Medical-grade silicone construction and compact form factor match the base model.
What this means for you: Enhanced multi-sensor array detects subtle muscle movements at $179, targeting bladder control with specialized programs validated in user testing.
What Does Research Show About Device-Assisted Training Compliance?
The 2009 randomized trial addressed a critical question: would patients actually use home trainers consistently? Researchers equipped devices with monitoring systems that recorded when and how long patients used them. Results showed similar compliance across all three intervention groups (P=0.201), with no significant difference between biofeedback, electrical stimulation, and exercises alone.
This finding suggests that device characteristics may matter less for compliance than individual motivation and protocol design. However, the trial occurred before widespread smartphone integration. Modern connected devices add features explicitly designed to boost adherence: push notifications reminding users to train, progress visualizations showing improvement trends, and achievement systems rewarding consistency.
A 2025 qualitative study examined real-world experiences of people with urinary incontinence using devices. Participants described varied experiences. Some found device use empowering because objective data confirmed improvement when subjective symptoms improved slowly. Others felt frustrated by technical issues or discouraged when data showed inconsistent progress.
The research suggests several factors influence compliance:
Perceived effectiveness. When users notice symptom reduction—fewer leakage episodes, better bladder control—they continue training. The 2009 trial showed all groups experienced fewer urine loss episodes, providing motivation to persist.
The 1990 case report on home trainers emphasized that device design directly impacts adoption rates—simpler interfaces encourage consistent use while complex systems create barriers PMID 27281865. This finding remains relevant today as manufacturers balance feature richness against usability.
Ease of use. Complicated setup, difficult insertion, or confusing interfaces create barriers. The 1990 study on home trainers noted that simple, intuitive devices had better adoption than complex systems requiring extensive instruction PMID 2080976.
Integration into routine. Devices requiring elaborate preparation or privacy beyond normal bathroom access get used less frequently. Smartphone-connected devices that require Bluetooth pairing, app launching, and phone positioning add steps compared to standalone units.
Discomfort or pain. The 2001 EMG biofeedback study confirmed most patients tolerated sessions well, but those experiencing more significant pain likely had reduced compliance. Individual anatomy and sensitivity vary.
Support and education. The 2017 app evaluation noted many applications lacked evidence-based protocols or proper instruction. Devices paired with comprehensive educational content and ideally initial guidance from pelvic floor physical therapists likely see better sustained use.
The 2019 evaluation of smartphone pelvic floor exercise apps found that app-based programs could deliver evidence-based exercise protocols when properly designed, though many available apps lacked scientific rigor PMID 29489554.
Behavioral psychology research suggests habit formation requires approximately 66 days of consistent practice. Devices with built-in programs lasting 8-10 weeks align with this timeframe, potentially establishing exercise as automatic behavior rather than requiring constant willpower.
How Do Training Programs Differ Between Devices?
Protocol variation represents a significant difference between products. Some offer fixed programs that all users follow identically. Others provide adaptive programs that adjust difficulty based on performance. Premium devices may include dozens of preset programs targeting specific conditions or training goals.
The Elvie Trainer uses five progressive levels. Users start at level one with basic contraction and relaxation patterns. As strength improves, subsequent levels introduce longer holds, more repetitions, and complex contraction patterns. The app automatically suggests level advancement based on performance metrics.
Perifit’s game-based approach varies resistance and duration through five different games. Each game emphasizes different muscle control aspects: sustained contractions, quick pulses, graduated force control, and relaxation. The app tracks performance in each game separately, allowing users to identify specific weaknesses.
The K-fit Kegel Toner Plus provides 22 preset programs mixing different stimulation patterns, frequencies, and intensities. Some programs emphasize strength building through intense contractions. Others focus on endurance with longer, moderate-intensity sessions. Users can select programs based on immediate goals or cycle through various programs weekly.
Clinical protocols typically recommend 3-5 training sessions per week, with each session lasting 10-15 minutes. The 2009 trial used this frequency and saw significant improvements within the study period. Most consumer devices default to similar schedules, though some allow customization.
Progressive overload—gradually increasing challenge as strength improves—represents a key training principle. Devices that maintain static difficulty risk plateaus. Adaptive systems that increase resistance, duration, or complexity support continued improvements.
Rest and recovery matter for muscle strengthening. Pelvic floor muscles require recovery time like any muscle group. Programs that encourage daily training without rest may lead to fatigue or overuse. Protocols alternating training days with rest days align better with muscle physiology.
Variation within programs addresses both physical and mental plateaus. Repeatedly performing identical exercises becomes tedious and may provide diminishing returns. Devices offering multiple programs or games maintain engagement while stimulating muscles through varied contraction patterns.
Periodization concepts from athletic training apply to pelvic floor work. Programs alternating high-intensity phases with recovery phases optimize adaptations while reducing overtraining risk. Advanced devices incorporate these principles, though most consumer trainers use simpler linear progression models.
What Role Does Professional Guidance Play in Device Selection?
While consumer pelvic floor trainers are available over-the-counter, consultation with a pelvic floor physical therapist or healthcare provider offers significant benefits. These specialists can:
Assess specific dysfunction. Pelvic floor issues include stress incontinence, urge incontinence, fecal incontinence, pelvic organ prolapse, and pelvic pain. These conditions often overlap with perimenopause-related changes that further weaken pelvic floor muscles. Different conditions may benefit from different training approaches. A 2013 review of biofeedback for fecal incontinence noted that protocol customization based on assessment improved outcomes.
Verify proper technique. Many people cannot correctly isolate pelvic floor muscles without initial guidance. Physical therapists use internal palpation to confirm correct muscle engagement and identify compensatory patterns like bearing down or contracting abdominal muscles instead.
Recommend appropriate devices. Not all trainers suit all conditions. Some situations may benefit more from EMS, others from pure biofeedback, and some may require different interventions entirely before device training makes sense.
Establish baselines. Clinical measurement of pelvic floor strength, endurance, and coordination provides objective starting points. Device feedback gains more meaning when compared against clinical assessment.
Monitor progress. Periodic follow-up allows comparison of device data against clinical measures. This confirms improvements translate to functional outcomes, not just better scores on device metrics.
Address complications. Some people experience pelvic floor muscle overactivity—muscles too tense rather than too weak. For these individuals, strengthening exercises worsen symptoms. Proper assessment identifies this before inappropriate device use causes harm.
The 2025 qualitative study on device user experiences found that participants who received professional guidance before starting device training reported more positive experiences and better understanding of proper technique. They could interpret device feedback meaningfully because therapists had explained what correct contraction should feel like.
Insurance coverage sometimes includes pelvic floor physical therapy, making professional guidance more accessible. Even brief initial consultation can significantly improve device training outcomes by ensuring correct starting point and appropriate device selection.
Physical therapists can also address common misconceptions. Many users believe maximum force equals best training, but proper pelvic floor exercise involves coordinated engagement at appropriate levels. Therapists teach users to match contraction intensity to functional needs rather than always squeezing maximally.
What Maintenance and Hygiene Practices Matter for Pelvic Floor Trainers?
Proper cleaning reduces infection risk and extends device life. Medical-grade silicone resists bacterial growth better than porous materials, but cleaning remains essential. Most manufacturers recommend washing with mild soap and warm water after each use, followed by air drying.
Some devices are waterproof and can be boiled or cleaned with toy-specific sanitizers. Others with electronic components require careful cleaning that avoids water damage to battery compartments or charging contacts. User manuals specify safe cleaning methods for each model.
Storage between uses protects devices from contamination and damage. Most trainers include storage pouches or cases. Storing devices in bathroom drawers without protection exposes them to humidity and potential contamination.
Water-based lubricant eases insertion and removal while remaining compatible with medical-grade silicone. Silicone-based lubricants can degrade silicone devices. Oil-based lubricants may leave residue that harbors bacteria. Most manufacturers explicitly recommend water-based formulations.
Regular inspection for damage matters for safety and effectiveness. Cracks, tears, or separation of seams create places bacteria can accumulate and potentially indicate structural failure. Any visible damage warrants device replacement.
Battery maintenance affects longevity for rechargeable devices. Lithium batteries last longer when kept between 20-80% charge rather than repeatedly fully depleted or constantly at 100%. Following manufacturer charging recommendations optimizes battery lifespan.
Software updates for connected devices may include performance improvements or bug fixes. Checking for app updates periodically ensures access to latest features and fixes.
Sharing devices between individuals poses infection risks even with thorough cleaning. Each person should use their own device. If cost prohibits individual devices, barrier methods like condoms could theoretically be used, though this may interfere with sensor accuracy.
Replacement schedules vary by manufacturer and usage frequency. Medical-grade silicone degrades slowly, but most manufacturers suggest replacement every 6-12 months with regular use. This accounts for material fatigue and potential bacterial accumulation in microscopic surface changes.
Environmental factors affect device longevity. Extreme temperatures during storage can damage batteries and degrade silicone. Exposure to direct sunlight may cause discoloration and material breakdown. Cool, dark storage locations preserve device integrity best.
How Do Clinical Outcomes Measure Device Effectiveness?
Research uses several outcome measures to assess pelvic floor training effectiveness:
Quality of life scores. The 2009 trial used validated questionnaires measuring how incontinence affected daily life. Significant improvements in quality of life scores (P<0.02) across all groups indicated meaningful real-world impact beyond just muscle strength numbers.
Urodynamic parameters. Clinical testing measures bladder capacity, detrusor pressure, urethral closure pressure, and flow rates. These objective measures assess physiological changes in bladder and sphincter function.
Perineometric measurements. Specialized devices measure pelvic floor muscle contraction pressure in standardized ways. The 2009 study showed increased muscle contraction strength (P<0.05) verified through perineometry.
Leakage episodes. Patient diaries tracking number of incontinence episodes per day or week provide practical outcome data. Fewer leakage events represent the most relevant improvement for most users.
Subjective assessment. Patient reports of symptom severity and improvement capture experiences not fully reflected in objective measures. The combination of objective improvement and subjective satisfaction indicates successful intervention.
EMG amplitude. Electromyography measures electrical activity in muscles during contractions. Higher amplitude indicates stronger muscle fiber recruitment. The 2001 study used EMG both for biofeedback and outcome measurement.
Consumer devices typically measure contraction force and duration but cannot assess urodynamic parameters or provide clinical-grade EMG. The 2022 study on connected trainers noted that while consumer devices provided useful feedback for training, they shouldn’t replace clinical assessment for diagnosis or monitoring complex conditions.
A 2020 multicentre randomized controlled trial compared PFMT with and without EMG biofeedback across multiple sites, providing robust evidence for biofeedback effectiveness in urinary incontinence treatment PMID 33055247.
Research comparing device training outcomes to supervised physical therapy shows mixed results. Some studies find similar improvements, suggesting home devices can match professional treatment when properly used. Others show better outcomes with in-person guidance, particularly for complex cases.
The 2018 systematic review on PFMT with EMG biofeedback found heterogeneity in outcome measurement across studies made definitive conclusions difficult. This highlights ongoing research needs for standardized protocols and outcome measures in this field.
Functional testing provides another outcome dimension. Clinical assessments might include cough stress tests, pad weight tests quantifying leakage, or timed standing tests. These functional measures complement laboratory measurements and patient-reported outcomes.
What Safety Considerations Apply to Pelvic Floor Training Devices?
Medical-grade materials represent the primary safety feature. Silicone used in Elvie, Perifit, and similar devices undergoes biocompatibility testing to verify it won’t cause allergic reactions or tissue irritation. Cheaper devices using untested plastics or materials with phthalates pose potential health risks.
Electrical stimulation intensity requires careful control. EMS devices like the K-fit include multiple intensity levels and safety limits controlling excessive current. The 2009 trial using electrical stimulation showed effectiveness without adverse events when properly controlled. However, excessive intensity could cause pain, muscle spasm, or tissue damage.
Proper usage instructions reduce misuse risk. Devices inserted incorrectly or used too aggressively might cause vaginal tissue irritation or injury. Clear manuals and instructional videos help users avoid these problems.
Contraindications exist for some users. Pregnant women should consult healthcare providers before starting pelvic floor device training, and may benefit from reviewing prenatal supplement guidance alongside their training plan. Those with pelvic organ prolapse may need specialized approaches. Active pelvic infections contraindicate insertion of any device.
EMS specifically has additional contraindications: pacemakers or other implanted electrical devices, epilepsy, and certain neurological conditions. The electrical current could interfere with implanted devices or trigger seizures in susceptible individuals.
Pain during use signals a problem. The 2001 EMG biofeedback study found most patients experienced minimal discomfort, but any significant pain warrants stopping and consulting a healthcare provider. Pain might indicate incorrect insertion, excessive intensity, underlying infection, or other issues requiring medical attention.
Device malfunction risks include battery leakage, electrical shorts in EMS devices, or structural failure of insertable components. Purchasing from established manufacturers with quality control and safety testing reduces these risks compared to unknown brands.
Psychological safety matters too. The 2025 qualitative study noted some users felt overwhelmed or discouraged by device data. Approaching training with realistic expectations and viewing devices as tools rather than complete solutions helps maintain appropriate perspective.
Regulatory status varies by country. In the United States, pelvic floor trainers making medical claims require FDA clearance or approval. Devices marketed for general wellness without specific medical claims face less stringent requirements. Users should verify regulatory status, particularly for imported products.
How Do Pelvic Floor Trainers Integrate with Other Treatments?
Pelvic floor muscle training often works best as part of comprehensive management. Devices complement rather than replace other interventions:
Behavioral modifications. Timed voiding, fluid management, and dietary changes addressing bladder irritants enhance training outcomes. Using a device while continuing habits that stress the pelvic floor limits results.
Weight management. Excess weight increases intra-abdominal pressure on the pelvic floor. Combined weight reduction and muscle strengthening produce better outcomes than either alone for stress incontinence.
Medication. Some incontinence types respond to medications affecting bladder muscle tone or urethral sphincter function. Hormonal balance plays a role in pelvic floor health, and devices can reduce medication needs in some cases or enhance pharmaceutical effectiveness when combined.
Physical therapy. Professional guidance optimizes device training as discussed earlier. Physical therapists may also address related issues like hip weakness or core instability affecting pelvic floor function.
Pessaries. These vaginal support devices physically support pelvic organs in prolapse cases. Some users combine pessary use with pelvic floor training, removing the pessary during exercise sessions.
Surgical consultation. Severe prolapse or incontinence may ultimately require surgical repair. Pelvic floor training before surgery potentially improves outcomes, and post-surgical training aids recovery and maintains results.
The 2009 trial demonstrated that home trainer devices effectively monitored compliance and performance, making them valuable tools for healthcare providers prescribing pelvic floor exercises. Providers can review device data at follow-up appointments to verify patients completed prescribed training and assess technique quality.
Integration with telehealth represents an emerging application. Connected devices could transmit data to providers remotely, allowing coaching and protocol adjustments without in-person visits. The 2017 study on mobile apps for exercise biofeedback noted this potential, though privacy and data security require careful attention.
Multidisciplinary care models show particular promise. Teams combining gynecologists, urologists, physical therapists, and mental health professionals address pelvic floor dysfunction from multiple angles. Devices provide objective home training data that all team members can reference, improving care coordination.
What Evidence Supports Long-Term Effectiveness?
Most pelvic floor training studies last weeks to months. Long-term maintenance of improvements requires ongoing research attention. The 2009 trial demonstrated significant benefits within the study period, but questions remain about whether users maintain training and whether benefits persist after stopping.
A 1990 study on home trainers noted that consistent long-term use was necessary to maintain benefits. Discontinuing exercises often led to gradual return of symptoms, though muscles didn’t weaken as rapidly as the initial strengthening occurred.
Maintenance protocols generally recommend continuing exercises 2-3 times weekly after completing initial intensive training. This frequency aims to maintain strength without requiring the time commitment of initial rehabilitation.
Connected devices theoretically aid long-term adherence through ongoing tracking and reminders. However, research hasn’t yet established whether these features translate to better long-term compliance compared to traditional approaches.
Muscle memory may play a role. After initial training establishes proper motor patterns, maintaining those patterns with lower frequency may be easier than initial learning. The neuromuscular control developed during intensive training potentially persists even with reduced practice.
Individual factors affect long-term needs. Those with mild initial symptoms may maintain improvements with minimal ongoing work. Others with severe dysfunction, multiple contributing factors, or high-stress activities may need consistent training indefinitely.
The 2025 qualitative study found that users who integrated device training into established routines maintained it better than those who viewed it as a temporary intervention. Framing pelvic floor exercise as ongoing health maintenance like dental hygiene or physical fitness rather than short-term treatment may improve long-term consistency.
Research gaps remain regarding optimal long-term protocols, comparing device-assisted versus unassisted maintenance, and identifying which users need ongoing intensive training versus reduced maintenance programs.
Longitudinal studies following participants for years post-intervention would clarify maintenance requirements. Current evidence suggests benefits persist with continued practice, but the minimum effective dose for maintenance remains unclear.
The foundation established by earlier device research continues informing modern innovations. The 2009 trial demonstrating home trainer effectiveness with objective compliance monitoring set precedents that current connected devices build upon, though with more sophisticated sensor arrays and data analytics capabilities PMID 19232601.
What Emerging Technologies Are Changing Pelvic Floor Training?
Current research explores several innovations beyond existing consumer devices:
Advanced sensor arrays. Multi-dimensional force sensors providing detailed mapping of muscle activation patterns across the entire pelvic floor could enable more targeted training. Current devices measure general pressure or limited force vectors.
AI-powered feedback. Machine learning algorithms analyzing contraction patterns could provide personalized coaching, identifying subtle technique issues and suggesting specific adjustments. The 2017 study on mobile apps noted that automated feedback remained basic, but technology continues advancing.
Virtual reality integration. VR environments could create immersive biofeedback experiences, potentially increasing engagement beyond current gaming approaches. Early research explores this in other rehabilitation contexts.
Wearable external sensors. Non-invasive sensors measuring pelvic floor activity through abdominal surface EMG or other external measurements would eliminate insertion requirements. Accuracy challenges currently limit this approach.
Telehealth integration. Platforms allowing pelvic floor physical therapists to monitor device data remotely and provide guidance through video consultations could improve access to professional support, particularly in underserved areas.
Improved EMS protocols. Research continues refining electrical stimulation parameters—frequency, intensity, pulse width, and pattern—to optimize muscle strengthening while minimizing discomfort.
The 2022 study on connected trainers noted that user experience design significantly influences adoption and continued use. Future devices will likely emphasize intuitive interfaces, seamless connectivity, and meaningful data presentation beyond raw numbers.
Regulatory oversight is evolving as more companies enter the pelvic floor training market. FDA regulation of devices making medical claims versus general wellness products affects what features and claims manufacturers can offer.
Research infrastructure is improving with more standardized protocols and outcome measures. The heterogeneity noted in the 2018 systematic review highlighted the need for consistent methodology across studies to enable better evidence synthesis.
Bioimpedance spectroscopy represents another emerging technology. This technique measures tissue composition and could potentially assess muscle quality and fatigue in addition to force output. Early research in other muscle groups shows promise.
Frequently Asked Questions
Do pelvic floor trainers really work?
Research shows biofeedback-assisted pelvic floor muscle exercises significantly improve urinary incontinence symptoms. A 2009 randomized trial found all groups using home trainers showed increased muscle strength (P<0.05) and improved quality of life (P<0.02).
What is the difference between biofeedback and EMS for pelvic floor training?
Biofeedback measures your muscle contractions and provides real-time feedback to help you perform exercises correctly. EMS (electrical muscle stimulation) uses electrical pulses to trigger muscle contractions passively. Both approaches show effectiveness in clinical trials, with biofeedback requiring active participation.
How long does it take to see results from pelvic floor training?
Most studies show measurable improvements within 4-8 weeks of consistent training. The 2009 trial using home trainers reported significant symptom reduction and fewer leakage episodes across all intervention groups within this timeframe.
Can pelvic floor trainers help with postpartum recovery?
Yes. Pelvic floor muscle training is widely recommended for postpartum recovery. Devices with biofeedback help ensure proper technique when muscles are weakened, though always consult your healthcare provider before starting exercises after delivery.
Are app-connected pelvic floor trainers more effective?
A 2017 evaluation found smartphone apps provided exercise guidance and progress tracking, though quality varied. App-connected devices like Perifit and Elvie combine real-time biofeedback with gamification, potentially improving adherence compared to exercises alone.
What is the best pelvic floor trainer for beginners?
The Perifit offers game-based training with clear visual feedback at a moderate price point. Its smaller form factor and intuitive app make it accessible for first-time users learning proper pelvic floor muscle engagement.
Do you need a prescription for a pelvic floor trainer?
Most consumer pelvic floor trainers are available over-the-counter without prescription. However, consulting a pelvic floor physical therapist or healthcare provider first ensures you select appropriate training for your specific condition.
Can men use pelvic floor trainers?
While most marketed devices target female anatomy, pelvic floor muscle training benefits men recovering from prostate procedures or experiencing incontinence. Specialized devices and protocols exist for male pelvic floor dysfunction.
How often should you use a pelvic floor trainer?
Most protocols recommend 3-5 sessions per week, with each session lasting 5-15 minutes. Consistency matters more than duration. The 2009 study used devices that monitored compliance and performance to ensure proper adherence.
What is electromyography biofeedback in pelvic floor training?
EMG biofeedback uses surface electrodes to measure electrical activity in pelvic floor muscles during contractions. A 2001 study found 88.9% of patients tolerated EMG biofeedback well, reporting negligible to mild discomfort during training sessions.
Our Top Recommendations
For most users seeking effective pelvic floor training, the Elvie Trainer represents the best overall choice. Its six-axis sensor array provides detailed feedback that helps identify and correct improper technique. Five progressive training levels accommodate beginners while supporting advanced users. Medical-grade silicone construction ensures safety and durability. While the $199 price point positions it in the premium category, the comprehensive feedback and quality construction justify the investment for serious training.
Budget-conscious users should consider the Perifit at $149. Game-based training maintains engagement better than simple repetitive exercises. Clinical-grade sensors deliver accurate feedback despite the lower price point. The smaller form factor suits users preferring less bulk. While single-axis sensing provides less detailed feedback than multi-dimensional systems, it remains sufficient for effective training when used consistently.
Those wanting the most comprehensive system should evaluate the K-fit Kegel Toner Plus. Combined EMS and biofeedback modes provide both passive and active training options. Twenty-two preset programs offer extensive variety. The full-color LCD display enables standalone use without smartphone dependency. The $319 price represents significant investment, but users seeking maximum versatility and professional-grade features find value in the expanded capabilities.
For users specifically addressing bladder control who value enhanced biofeedback precision, the Perifit Care+ upgrades standard Perifit sensors for improved muscle isolation. Specialized bladder control programs target relevant coordination patterns. Educational content helps users understand proper technique. At $179, it costs more than basic Perifit but less than premium devices while delivering enhanced sensor capabilities.
Regardless of which device you choose, consistency matters more than any single feature. The 2009 clinical trial showed similar compliance across different training methods, suggesting that selecting a device you’ll actually use regularly outweighs small technical differences. Start with realistic expectations, follow the recommended protocols, and consider professional guidance to optimize results.
Recommended Products




Get Weekly Research Updates
New studies, updated reviews, and evidence-based health insights delivered to your inbox. Unsubscribe anytime.



